Stage : Early Localized Disease
Symptoms of Lyme disease usually start 1 to 2 weeks after the tick bite. One of the earliest signs of the disease is a bulls-eye rash.
The rash occurs at the site of the tick bite, usually, but not always, as a central red spot surrounded by a clear spot with an area of redness at the edge. It may be warm to the touch, but it isnt painful and doesnt itch. This rash will gradually fade in most people.
The formal name for this rash is erythema migrans. Erythema migrans is said to be characteristic of Lyme disease. However, many people dont have this symptom.
Some people have a rash thats solid red, while people with dark complexions may have a rash that resembles a bruise.
The rash can occur with or without systemic viral or flu-like symptoms.
Other symptoms commonly seen in this stage of Lyme disease include:
What If A Tick Bites My Dog
The more ticks in your region, the likelier it is that your furry pal will bring them home.
Your dog is much more likely to be bitten by a tick than you are. And where Lyme disease is common, up to 25% of dogs have had it at some point.
About 10% of dogs with Lyme disease will get sick. 7-21 days after a tick bite, your dog might seem like theyâre walking on eggshells. They also might have a fever and enlarged lymph nodes. Plus, they might seem tired. Dogs also get antibiotics for Lyme.
What if my dog brings ticks into my home?
Use a tick control product on your pet to prevent Lyme disease. Also, have your dog vaccinated against Lyme.
Check your dogâs whole body each day for bumps. If you notice a swollen area, see if thereâs a tick there. If you find a tick, wear gloves while you use tweezers to separate it from your dog. Then, put it in soapy water or alcohol, or flush it down the toilet.
Use alcohol to clean the spot on your dog where the tick was attached. Keep an eye on that spot, and also on your dog to make sure theyâre behaving normally. If you notice any changes, check with your vet.
Show Sources
John Aucott, MD, assistant professor of medicine, Johns Hopkins University School of Medicine director, Johns Hopkins Lyme Disease Clinical Research Center.
CDC.
Morbidity and Mortality Weekly Report: âVital Signs: Trends in Reported Vectorborne Disease Cases — United States and Territories, 2004-2016.â
American College of Rheumatology.
Tick Talk On Ixodes Scapularis
Ixodes scapularis require high humidity, so they tend to be associated with habitats that are heavily shaded and covered with leaf litter. Tick habitats also include areas where hosts are frequently observed such as brush piles, stone wall bases, wood piles, wooded areas, edges of fields, and areas with low dense woody vegetation. White-tailed deer and white-footed mice are the primary hosts in the northeast of the United States. The large habitat of these hosts allows for a wide distribution.
Ixodes scapularis require two years to complete their life cycle from egg to larvae to nymph to adult. Adults are typically active from October-May but can be found year-round if the temperature exceeds freezing. Adults prefer larger hosts such as deer and humans. Once females fully engorge on their blood meal, they drop off the host into the leaf litter where they lay an egg mass in late spring, early summer. Larvae emerge from the egg mass in late summer and can attach to any size mammalian host and many bird species. After a blood meal the larvae will molt and re-emerge the following spring as a nymph. Nymphs are most active May-August. The poppy seed sized nymphs are known to be the most responsible in human disease transmission due to their extremely small size, often going unnoticed when attached. The nymphal ticks that have fed, as larvae, on infected hosts during the prior summer are now able to transmit the pathogens to people and their pets
Also Check: Natural Protocol For Lyme Disease
How Is Lyme Disease Diagnosed
Diagnosing Lyme disease can be difficult as symptoms vary from person to person. Symptoms can also be similar to other illnesses.
A diagnosis of Lyme disease is based on:
- the outcome of laboratory testing
Laboratory testing may be recommended for patients with signs, symptoms and history of exposure to tick bite to support a clinical diagnosis.
Seek your health care provider right away if you develop symptoms of Lyme disease after being bitten by a tick or if you visited a known at risk area for Lyme disease. The earlier a diagnosis is made, the greater the chance of a successful treatment.
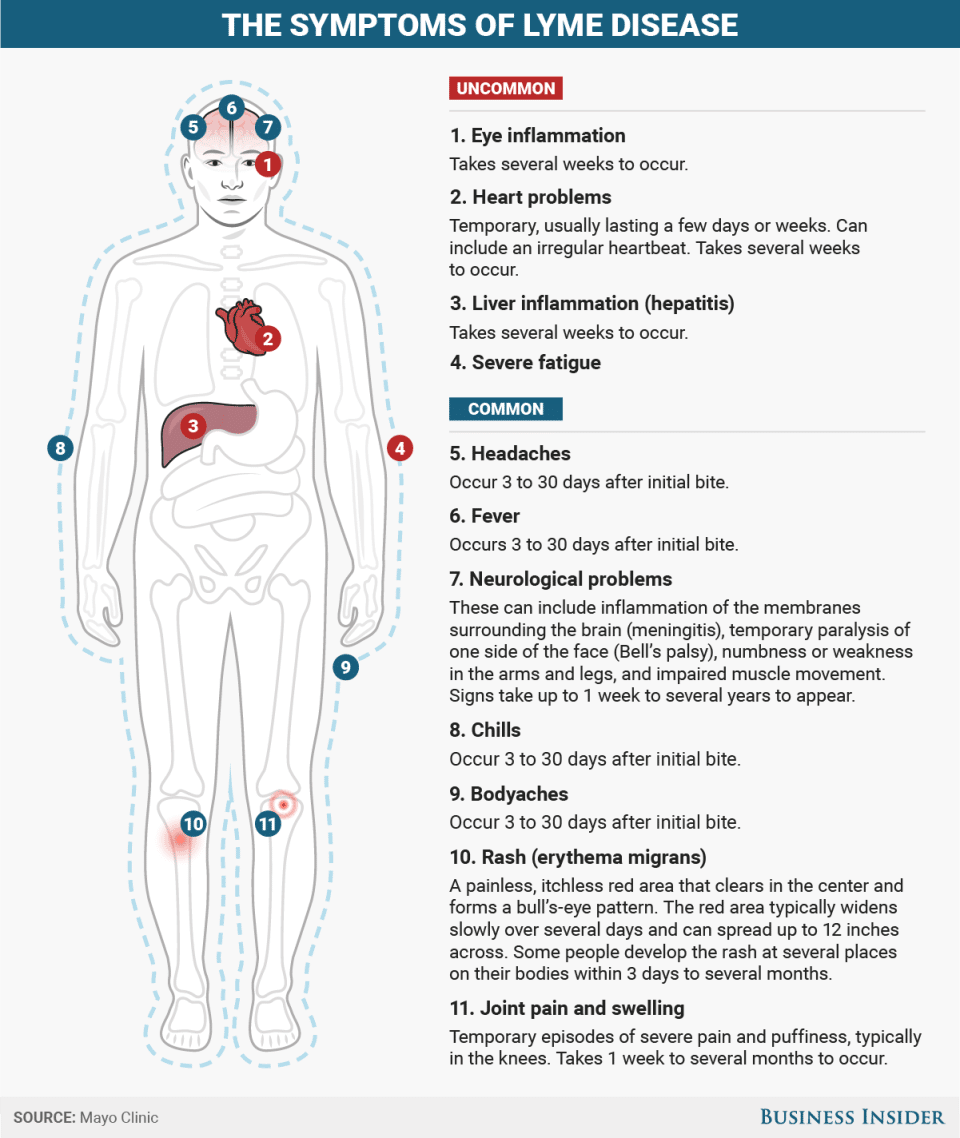
What Are The Symptoms Of Lyme Disease

Early symptoms of Lyme disease start between 3 to 30 days after an infected tick bites you. The symptoms can include:
- A red rash called erythema migrans . Most people with Lyme disease get this rash. It gets bigger over several days and may feel warm. It is usually not painful or itchy. As it starts to get better, parts of it may fade. Sometimes this makes the rash look like a “bull’s-eye.”
- Fever
- Muscle and joint aches
- Swollen lymph nodes
If the infection is not treated, it can spread to your joints, heart, and nervous system. The symptoms may include:
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of your body
- Facial palsy, which is a weakness in your facial muscles. It can cause drooping on one or both sides of your face.
- Arthritis with severe joint pain and swelling, especially in your knees and other large joints
- Pain that comes and goes in your tendons, muscles, joints, and bones
- Heart palpitations, which are feelings that your heart is skipping a beat, fluttering, pounding, or beating too hard or too fast
- Shooting pains, numbness, or tingling in the hands or feet
Also Check: Lyme Disease And Behavior Problems
Keeping Cells Free Of Debris
You depend on your immune system to keep the spaces between cells free of debris so that they get good flow. Specialized immune cells, called macrophages, constantly patrol your tissues searching for debris they are the garbage collectors of the immune system. Macrophages engulf debris from dead cells and then break it down with strong acid and potent free radicals.
This process is happening in the body all the timeyou couldnt survive without it. As long as the collection of debris doesnt exceed the capacity of the immune system to clean it up, you never know its happening. Its deemed inflammation only when accumulation of debris from cell turnover is greater than the immune system can process.
Tissues congested with debris stresses cells. When cells suffer, you feel it as symptoms. The type of symptoms depend on the types and location of cells that are suffering. Symptoms associated with inflammation can be transient and localized when cell injury is finite, such as with an acute injury, or chronic and systemic when cell injury is ongoing, such as with chronic Lyme disease or really any chronic illness.
Lets take a look at inflammation in more detail, particularly chronic inflammation as it impacts people with Lyme disease, along with the best ways to quash it.
How Is It Treated
The main treatment for Lyme disease is antibiotics. These medicines usually cure Lyme disease within 3 weeks of starting treatment.
It’s important to get treatment for Lyme disease as soon as you can. If it goes untreated, Lyme disease can lead to problems with your skin, joints, nervous system, and heart. These can occur weeks, months, or even years after your tick bite. The problems often get better with antibiotics, but in rare cases they can last the rest of your life.
Don’t Miss: Lab Work For Lyme Disease
Overview Of Lyme Disease Pain Control
Most people with Lyme have pain. In this article I review the causes of Lyme pain and the steps a person can take to control and eliminate pain. I provide a strategy for controlling Lyme disease pain which uses:
- Sleep,
- Anti-cytokine herbs and supplements to lower inflammation,
- Supplements that support repair of mitochondria cell energy factories,
- Low dose naltrexone ,
- Medical marijuana and/or CBD oil,
- Magnesium to relax muscles,
Should You Use Antibiotics
Different antibiotics may be used to treat children and adults. The decision to take medicines for Lyme disease may be based on one or more of these factors:
- You have symptoms of Lyme disease, especially the red, circular rash, and a history of exposure to ticks in geographic regions where Lyme disease is known to occur.
- Blood tests show that you have antibodies to the Lyme disease bacteria in your blood, spinal fluid, or joint fluid.
- You are pregnant or breastfeeding and are bitten by a tick.
Recommended Reading: Lyme Disease And Muscle Pain
What Causes Chronic Lyme Disease
The CDC says 10% to 20% of people treated for Lyme disease develop ongoing symptoms. These can include fatigue, joint and muscle pain, and thinking problems. The symptoms can last more than 6 months.
No one knows what causes chronic Lyme disease. One theory is the infection damages tissues or alters the immune system.
Some pain experts think the immune systemâs reaction to the Lyme infection causes changes that increase pain sensations and contribute to fatigue and poor sleep.
More research is underway.
No matter the cause, the symptoms are real. But most patients get better over time.
Show Sources
Neurologic Pain In Lyme Disease
Lyme disease can also cause neurologic pain. Nerve pain has qualities of sharp, stabbing, shooting, piercing, or electrical type pain. These qualities of pain occur when Lyme germs directly injure nerves. Or it occurs as a result of inflammation of those nerves from cytokines.
There is a second type of nerve pain known to occur in people with fibromyalgia and MS, that likely occurs in people with Lyme disease. This is due to infection in the brain activating a brain immune cell called microglia. When infections activate Toll-like receptors on microglia, this leads to neurologic pain felt throughout the body. Some think this is the cause of the muscle pain seen in people with fibromyalgia. It is also likely a major cause of the myalgia seen in Lyme disease.
Lyme Disease Pain Strategy
For nerve pain due to microglia activation in the brain, one strategy is to block the Toll-like receptors to stop the microglia from turning on. LDN helps with this.
Another strategy is to decrease the inflammation of nerves. LDN, anti-cytokine herbs, and medical marijuana/cbd oil may help with this.
The last nerve strategy is to decrease the nerve signals that transmit nerve pain. Sleep helps with this, medical marijuana/cbd, prescriptions anti-seizure prescriptions and anti-depression prescriptions can help this too.
Recommended Reading: Natural Remedies To Cure Lyme Disease
When Should You Call Your Doctor
- A tick is attached to your body and you are unable to remove the entire tick.
- You have a circular red rash that expands over the course of several days, especially if you know you were recently exposed to ticks. You may also have flu-like symptoms, such as fatigue, headache, stiff neck, fever, chills, or body aches.
- You feel very tired or have joint pain , irregular heartbeats, severe headache, or neck pain.
- You are pregnant or nursing and you think you may have been exposed to ticks.
Transmission Dynamics Of Tbds
Pathogens can be acquired by ticks while feeding on infected hosts. In suitable tick vectors, TBPs have the ability to persist throughout the molting process to the next instar, a phenomenon called transstadial transmission. The efficiency of vertical transmission, from female tick to her offspring, varies from non-detectable for B. burgdorferi and B. microti , to ~40% for B. venatorum to close to 100% for R. helvetica . Ixodes ricinus is capable to transmit more than twenty different pathogenic parasites, bacteria and viruses via their blood meal to vertebrate hosts . Pathogen transmission by ticks requires many often unexplored tick-pathogen interactions, from the migration of these pathogens from the gut to their secretion in tick saliva .
Transmission dynamics can also be affected by weather and climatic conditions. The seasonal synchrony of larval and nymphal stages is an important driver of non-systemic transmission of TBEV via co-feeding of infected nymphs with uninfected larvae. This synchrony in tick activity and feeding, in turn, is affected by temperature patterns, in particular autumn cooling and spring warming . Climate change might therefore not only affect the distribution of ticks themselves, but also the distribution and nymphal infection rate of TBEV, and maybe also of other TBPs .
Read Also: Snow Plowing East Lyme Ct
Genetic Engineering For Reservoir And Vector Incompetence
The advent of CRISPR/Cas technologies have made targeted engineering of mice feasible. By incorporating the CRISPR/Cas machinery into an engineered cassette called a gene-drive and inserting it into the chromosome, animals can pass along the engineered trait in a dominant, non-Mendelian pattern as the inserted gene will create a copy of itself onto the other chromosome. Investigators have proposed using this tool to create B. burgdorferi resistant mice carrying a gene to express an anti-OspA antibody . Proof of principle studies are being carried out in mice without the use of the gene drive, but ultimately, use of gene drive technology could prove to be a low-cost mechanism for changing reservoir competence of an entire population of mice. However, the path to using this technology will be difficult due to concerns about the ability to control unforeseen events caused by a self-replicating, engineered mutation.
A similar genetic engineering strategy could be undertaken with a focus on ticks. Engineering ticks to be of a single sex to reduce tick populations or elimination of specific proteins required for vector competence could be an effective strategy for controlling tick transmitted diseases. Similar strategies have been proposed for mosquitos in the control of dengue virus . However, Ixodes tick biology with its 2-year cycle, may make tick gene drive approaches very challenging.
What Are The Stages Of Lyme Infection
There are three stages:
- Early localized Lyme: Flu-like symptoms like fever, chills, headache, swollen lymph nodes, sore throat, and a rash that looks like a bull’s-eye or is round and red and at least 2 inches long
- Early disseminated Lyme: Flu-like symptoms like pain, weakness, or numbness in your arms and legs, changes in your vision, heart palpitations and chest pain, a rash , and a type of facial paralysis known as Bellâs palsy
- Late disseminated Lyme: This can happen weeks, months, or years after the tick bite. Symptoms might include arthritis, severe fatigue and headaches, dizziness, trouble sleeping, and confusion.
About 10% of people treated for Lyme infection donât shake the disease. They may go on to have three core symptoms: joint or muscle pain, fatigue, and short-term memory loss or confusion. This is called post-treatment Lyme disease syndrome. It can be hard to diagnose because it has the same symptoms as other diseases. Plus, there isn’t a blood test to confirm it.
Experts arenât sure why Lyme symptoms donât always go away. One theory is that your body keeps fighting the infection even after the bacteria are gone, like an autoimmune disorder.
Recommended Reading: What Is Lyme Disease And What Are The Symptoms
Stage : Early Disseminated Lyme Disease
Early disseminated Lyme disease occurs several weeks to months after the tick bite.
Youll have a general feeling of being unwell, and a rash may appear in areas other than the tick bite.
This stage of the disease is primarily characterized by evidence of systemic infection, which means infection has spread throughout the body, including to other organs.
Symptoms can include:
- disturbances in heart rhythm, which can be caused by Lyme carditis
- neurologic conditions, such as numbness, tingling, facial and cranial nerve palsies, and meningitis
The symptoms of stages 1 and 2 can overlap.
What’s The Best Way To Prevent A Tick Bite
Ticks can’t fly or jump. But they live in shrubs and bushes and can grab onto you when you pass by. To avoid getting bitten:
- Wear pants and socks in areas with lots of trees and when you touch fallen leaves.
- Wear a tick repellent on your skin and clothing that has DEET, lemon oil, or eucalyptus.
- For even more protection, use the chemical permethrin on clothing and camping gear.
- Shower within 2 hours after coming inside. Look for ticks on your skin, and wash ticks out of your hair.
- Put your clothing and any exposed gear into a hot dryer to kill whatever pests might be on them.
How do you know if you’ve been bitten?
Since ticks are so small, you’ve got to have pretty good eyes to see them.
If you have a small, red bump on your skin that looks like a mosquito bite, it could be a tick bite. If it goes away in a few days, itâs not a problem. Remember, a tick bite doesnât necessarily mean you have Lyme disease.
If you notice a rash in the shape of a bull’s-eye, you might have a tick bite. Talk to your doctor about treatment.
If you have an allergic reaction to ticks, you’ll notice a bite right away.
You May Like: Can Lyme Disease Cause Liver Damage
Clinical Presentation Of Other Tbds
In Europe, human babesiosis is caused by B. microti, B. divergens and B. venatorum . All Babesia species infect erythrocytes and cause haemolysis, leading to the clinical manifestations of fever, anaemia, jaundice, haemoglobinuria and potentially also renal insufficiency. Over 40 human babesiosis cases have been reported in Europe, mostly in asplenic patients. Other risk factors are immunosuppression, depletion of mature B-cells and old age . Judging from the discrepancy between case reports and seroprevalence, an asymptomatic and/or self-limiting course is common . Although serious infection appears to be uncommon, when acquired, the disease has a mortality rate of 42% in B. divergens and 5% in B. microti . Babesia divergens is the causal agent of bovine babesiosis in Europe. The clinical picture is similar to that seen in humans, with a bimodal seasonal occurrence of the disease that is associated with I. ricinus activity. In cattle, an inverse age resistance phenomenon is present in which calves up to the age of 912 months are susceptible for infection, but resistant to disease .