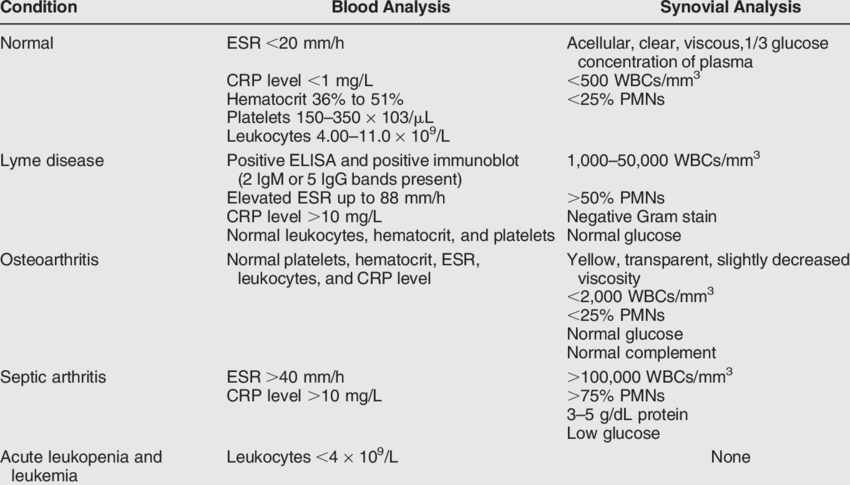
What Is The Role Of Synovial Fluid Analysis In The Workup Of Lyme Disease
In patients with Lyme arthritis, synovial fluid is usually inflammatory, with cell counts ranging from 500-98,000/µL reported. In adult patients, the fluid should also be examined for crystals to rule out gout and pseudogout.
One study that included 63 patients with Lyme arthritis found that although the majority had positive polymerase chain reaction results for B burgdorferi DNA in synovial fluid, none of the samples tested were positive for B burgdorferi messenger RNA , even when the specimen was obtained before initiation of antibiotic treatment. These results suggest that detection of B burgdorferi DNA in synovial fluid is not a reliable test for active joint infection in Lyme disease.
Whats The Purpose Of A Synovial Fluid Analysis
If you have joint symptoms like:
- Pain
- An infection like
- Bleeding disorders like hemophilia or von Willebrand disease
- A disease that break down joints over time, like osteoarthritis
Your doctor might also use this test to see if your treatment for your joint condition is working.
If your doctor thinks you need this test, ask them how to prepare. Let them know if you take blood thinners or any other medication.
Synovial Fluid Analysis Imaging And Other Tests
On presentation, joint aspiration is usually done for diagnostic purposes to rule out the presence of other arthritides such as crystalline arthropathy or staphylococcal septic arthritis. Joint fluid white cell counts are usually inflammatory in the range , but cell counts as low as 500 or as high as 100,000 cells/mm3 have been reported. Although tests for rheumatoid factor or antinuclear antibodies typically yield negative results, antinuclear antibodies in low titer may be detected. Peripheral white blood cell counts are usually within the normal range, but inflammatory markers, such as ESR and CRP, may be elevated. Imaging studies are not required for diagnosis or are not typically performed. The major reason for imaging studies in Lyme arthritis is when there are concerns for alternative diagnoses.
In patients with Lyme arthritis, plain films, MRI scanning or ultrasound typically show non-specific joint effusions, while MRI studies utilizing contrast dye, may display synovial thickening or enhancement. In adult patients, imaging studies may show co-incidental degenerative changes or chronic mechanical injuries, but these abnormalities would not be expected to cause significant synovitis or inflammation. Lyme arthritis is not rapidly erosive, but with longer arthritis durations, joint damage can be seen on radiographic studies. Finally, MRI scanning may be useful in the planning of synovectomies by determining the extent of synovitis within the joint.
You May Like: What Kind Of Antibiotics Treat Lyme Disease
Bacterial Strains Cell Lines And Growth Conditions
A clone of the B. burgdorferi type strain B31 was used in all experiments involving this bacterium. Other bacteria used in this study include S. aureus SA113, B. subtilis 168, and E. coli K-12 MG1655. Unless otherwise noted, B. burgdorferi was cultured at 34 °C in complete BSK II medium containing 6% rabbit serum . All other bacteria were grown at 37 °C in LB medium. HEK 293-derived human NOD1 and NOD2 reporter cell lines were cultured at 37 °C under 5% CO2 in RPMI medium containing 10% FBS and blasticidin S , Zeocin , and Normocin . Fresh PBMCs from healthy human subjects were obtained from mixed donor samples and used in assays in the recommended PBMC culture medium .
Borrelia Burgdorferi Peptidoglycan Is A Persistent Antigen In Patients With Lyme Arthritis
See allHide authors and affiliations
- For correspondence:
Contributed by Christine Jacobs-Wagner, May 11, 2019
Don’t Miss: Can You Get Lyme Disease More Than Once
Serologic Testing For Lyme Disease
The mainstay in diagnosing Lyme arthritis is serologic testing. In the USA, the CDC currently recommends a two-test approach in which samples are first tested for antibodies to B. burgdorferi by enzyme-linked immunosorbent assay and those with equivocal or positive results are subsequently tested by Western blotting , with findings interpreted according to the CDC criteria. In contrast with early infection, when some patients may be seronegative, all patients with Lyme arthritis, a late disease manifestation, have positive serologic results for IgG antibodies to B. burgdorferi, with expansion of the response to many spirochetal proteins. When serum samples were tested with microarrays of more than 1200 spirochetal proteins, 120 proteins, primarily outer-membrane lipoproteins, were found to be immunogenic, and patients with Lyme arthritis had IgG reactivity to as many as 89 proteins. Serologic testing should be performed only in serum, as serologic tests in synovial fluid are not accurate.
Box 1 Significance & Innovations
- To our knowledge, this is the first reported series comparing clinical and laboratory features and outcomes of Lyme arthritis between children and adults.
- Children with Lyme arthritis were found to present more acutely than adults.
- Synovial white cell counts were found to be significantly higher in children than adults, often approaching counts observed with septic arthritis.
- Despite the acute, intense inflammatory response observed in children with Lyme arthritis compared to adults, children recovered faster and received less antibiotic therapy.
Don’t Miss: What Tests Are Done For Lyme Disease
Acute Lyme Arthritis Presenting In Bilateral Hips Of An Elderly Patient: A Case Report
Lawrence M Asprec*1, Mitchell K Freedman2, Jeffrey A Gehret3 and George W Young3
1Senior Resident in Physical Medicine and Rehabilitation, Thomas Jefferson University Hospital at Sidney Kimmel Medical College, Philadelphia, USA
2Medical Director of Physical Medicine and Rehabilitation, Associate Professor, Rothman Orthopaedic Institute, 925 Chestnut Street, 5th Floor, Philadelphia, USA
3Department of Physical Medicine and Rehabilitation, Division of Pain Management, Rothman Orthopaedic Institute, 925 Chestnut Street, 5th Floor, Philadelphia, USA
Lyme Arthritis: Highly Treatable Slow To Resolve
EXPERT ANALYSIS FROM THE ANNUAL PEDIATRIC INFECTIOUS DISEASES CONFERENCE SPONSORED BY CHILDREN’S HOSPITAL COLORADO
VAIL, COLO. Arthritis is far and away the most common manifestation of late Lyme disease, affecting up to 30% of children whose early-stage disease went untreated.
Lyme arthritis presents with a distinctive clinical picture. Nevertheless, this common condition is often initially mismanaged as a joint sprain or other orthopedic injury, with the correct diagnosis coming only following referral after a month or more with no improvement, according to Dr. Roberta L. DeBiasi, acting chief of the division of pediatric infectious diseases at Childrens National Medical Center, Washington.
Dr. Roberta L. DeBiasi
“We see tons of kids with Lyme arthritis. We get two or three cases every week in our clinic,” she said at the conference.
Lyme arthritis occurs months to years after an untreated exposure to Borrelia burgdorferi. Affected patients typically present with a history of recurrent, weeks- or months-long attacks of joint swelling in one or a few joints. The knee is by far the most common site, but other large joints can be involved, as can the temporomandibular joint. An involved knee may swell up to literally the size of a basketball, yet the child has no fever, erythema, or systemic complaints, and surprisingly little pain given the effusion size.
Dr. DeBiasi reported having no financial conflicts.
Read Also: Lyme Disease Specialist Raleigh Nc
B Burgdorferi Pg Has An Unusual Chemical Composition
We first characterized the chemical composition and architecture of purified PGBb. Liquid chromatography and mass spectrometry analysis of cellosyl-digested PG revealed several unusual features . For instance, whereas the sugar backbone of the PGBb is made up of alternating N-acetylglucosamine and N-acetylmuramic acid , similar to other bacterial PGs, we also observed the occasional presence of an N-acetylhexosamine linked to GlcNAc . To our knowledge, such a modification has not been reported in any other PGs characterized to date. Another feature of the PGBb was the presence of l-ornithine linked to a single glycine , which is congruent with an earlier chemical amino acid analysis . The presence of l-Orn has been reported in other spirochetes . It is, otherwise, a rare deviation from the typical PG dichotomy in the bacterial domain , which generally features a diaminopimelic acid or lysine at the third amino acid position of the stem peptide. We confirmed the presence of l-Orn in PGBb by using two methods: gas chromatography coupled to mass spectrometry and 3H-l-Orn radiolabeling followed by high-performance liquid chromatography analysis and liquid scintillation counting .
Is There Anything Else I Should Know
A blood or urine uric acid or blood glucose test may be ordered to compare concentrations with those in the synovial fluid. If a healthcare practitioner suspects that an individual has a systemic infection, then a blood culture may be ordered in addition to the synovial fluid analysis.
Joint injury, surgery, and joint replacement can increase the risk of developing an infection in a joint.
Read Also: Untreated Lyme Disease Years Later
B Burgdorferi Pg Elicits Proinflammatory Cytokine Responses In Human Peripheral Blood Mononuclear Cells
LA is characterized by marked synovial hypertrophy and inflammation. As in other forms of inflammatory arthritis, proinflammatory cytokines such as IL-1, TNF, IL-6, and IL-8 are found in the synovial fluid of patients with LA . Consistent with these previous observations, we found that virtually all major proinflammatory markers were significantly up-regulated in the synovial fluid of patients with LA relative to their serum , ranging from 4- to 2,000-fold increases in TNF, IL-1, IL-1, IL-6, IL-8, IL-17F, and INF production . Inflammation of this magnitude often coincided with a secondary response involving production of antiinflammatory cytokines, including IL-10, the level of which was also significantly increased in the synovial fluid of LA patients .
Cytokine profile in serum and synovial fluid samples from patients with LA or after in vitro stimulation of human PBMCs with PGBb. Bee-swarm plots showing levels of indicated cytokines in LA patient samples. Horizontal black lines indicate geometric means . Pound signs indicate samples that yielded no signal but were included for completeness, as zero values cannot be displayed on log-scale axes. Cytokine levels produced by control human PBMCs stimulated by PBS or 100 g/mL polymeric PG or mutanolysin-digested PG for 72 h. The 18-h results are shown in SI Appendix, Fig. S7A. All stimulatory studies were performed on pooled, mixed donor samples assayed in duplicate .
What Is Synovial Fluid
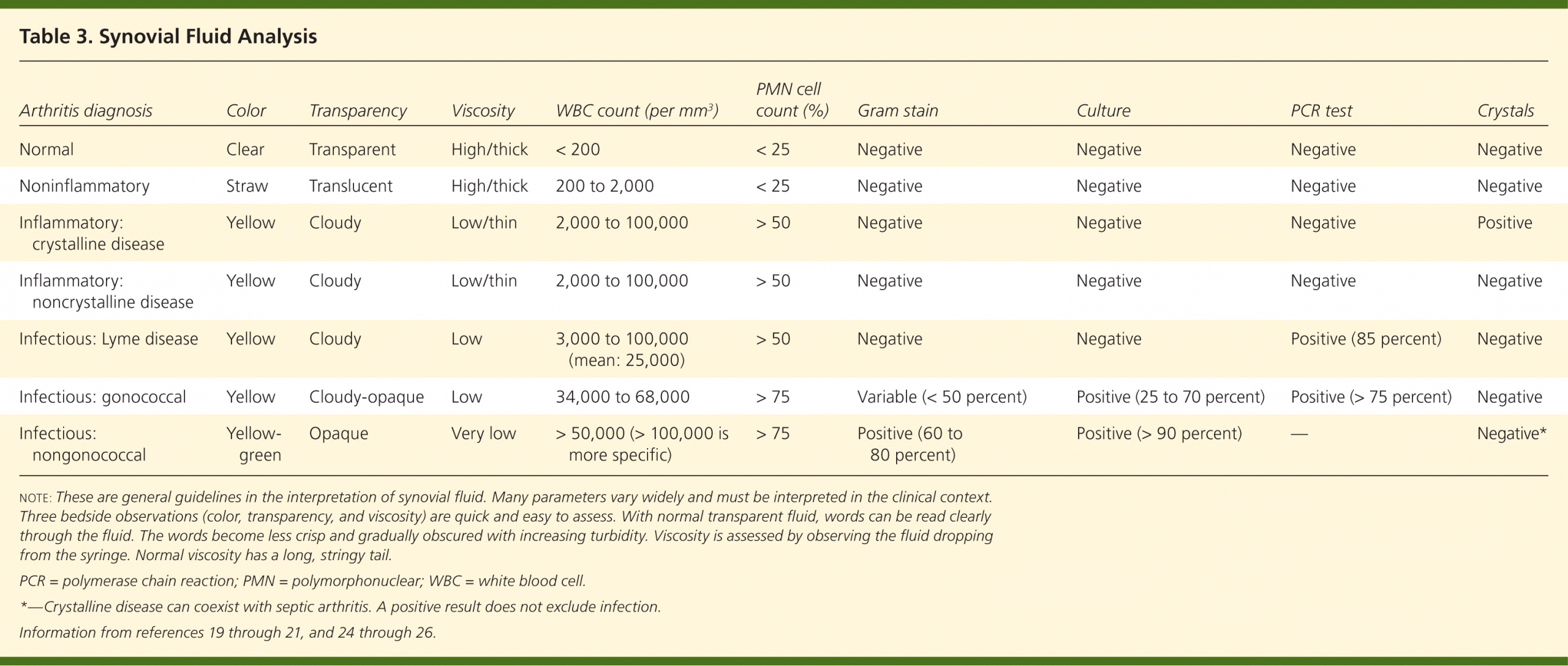
Synovial fluid is the thick liquid that lubricates your joints and keeps them moving smoothly. Itâs on all of your joints, including in your knees, shoulders, hips, hands, and feet.
Joint conditions like arthritis, gout, infections, and bleeding disorders can change how your synovial fluid looks and feels. A sample of this fluid taken during a procedure called an arthrocentesis can help your doctor figure out whatâs causing your symptoms.
You May Like: Dr Emilia Eiras Lyme Disease
Synovial Fluid Cell Counts Do Not Accurately Differentiate Arthritis Types
Synovial fluid white blood cell counts may not be the most optimal method to differentiate septic arthritis from arthritis caused by Lyme disease, according to findings from a new study published in Pediatrics. For a more accurate diagnosis of Lyme disease, newer-generation diagnostics are needed to avoid both underdiagnosis and overdiagnosis of Lyme disease to plan appropriate management.
Patients with septic hip arthritis require surgical drainage, but it can be a challenge for clinicians to identify these individuals without performing unnecessary invasive procedures. In this study, the authors examined the predictive ability of synovial fluid WBC counts in patients with hip monoarthritis to see whether they can be used to differentiate septic arthritis from disease related to Lyme disease accurately.
A retrospective cohort study was conducted that included 238 patients with acute monoarticular arthritis of the hip who underwent arthrocentesis at 3 emergency departments located in Lyme endemic areas. Within this group, 26 had , 32 had Lyme arthritis, and 180 had other types of arthritis. Those with septic arthritis had a higher median synovial fluid WBC count vs patients with Lyme arthritis . In addition, 18 people with Lyme disease had synovial fluid WBC counts 50 000 cells/µL, and of those who underwent surgical drainage , 13 subsequently received a diagnosis of Lyme disease.
How To Get Tested
A synovial fluid analysis is ordered by a doctor. The test may be ordered by your primary care provider, a specialist such as a rheumatologist, who specializes in treating joint diseases, or an orthopedist or orthopedic surgeon, who specializes in bone and connective tissue disorders.
A synovial fluid analysis is conducted on joint fluid, which is extracted from the joint through a procedure called arthrocentesis. Arthrocentesis is typically performed in the office of the provider who orders the test, or in another medical setting, like a hospital. Arthrocentesis is administered by a medical professional who has been trained in the procedure, such as a physician, physicians assistant, or nurse practitioner.
Recommended Reading: Fda Approved Lyme Disease Test
B Burgdorferi Pg Material Is Detected In Synovial Fluid Samples From Patients With La After Antibiotic Treatment
As patients with LA produce a specific anti-PGBb IgG response, we next sought to determine whether we could detect antigenic PGBb material in the synovial fluid of patients with LA. To this end, we generated a polyclonal anti-PGBb antiserum through immunization of New Zealand White rabbits with PGBb. The polyclonal antiserum was specific for PGBb, as it did not react with other common PG types in a competitive ELISA . By using this same competitive ELISA, we did not detect PGBb in control synovial fluid samples . We also failed to detect PGBb in the sera of patients with LA . However, 92% of the tested LA synovial fluid samples contained tens to hundreds of picograms of PG material per milliliter . The amount of PG detected strongly correlated with the anti-PGBb IgG level found in the same synovial fluid sample , indicating that the antigenic material detected by our rabbit polyclonal antiserum is likely PGBb. Our results show that PGBb is present in LA synovial fluid samples before and after oral and IV antibiotic treatment .
Detection of PGBb in synovial fluid samples of patients with LA. Competitive ELISA using rabbit antiserum raised against PGBb to quantify the concentration of PG present in each sample. Horizontal black lines indicate means . Plot showing the PGBb concentration of each sample as a function of its anti-PGBb IgG level. The linear fit and the Pearson correlation coefficient for the LA synovial fluid samples are also shown.
Health’citizen Scientists’ Take On Tick
As for the new study, it leaves open the question of whether there are still bacteria in the joints of patients with Lyme arthritis, Lewis said. The authors think that the peptidoglycan remains in synovial fluid after the pathogen is gone. My guess is that the pathogen remains in the joints and sheds the antigen. It would be good to know how things really are.
When it comes to finding physical explanations for patient symptoms, its not necessary to determine whether PTLDS is caused by lingering bacteria or to a malfunctioning immune system, said Dr. Peter Novak, an assistant professor of neurology at Harvard Medical School and director of the autonomic laboratory at Brigham and Womens Hospital. Novak, who also was not involved in the new study, and his colleagues have discovered patients end up with damage to their small nerves and also diminished blood flow to certain areas of the brain.
He suspects that damage is due to changes in the immune system that were kicked off by the Lyme infection and remain after the bacteria have been obliterated. As for patients who experience improvement when treated with long courses of antibiotics, Novak believes this is because many antibiotics also have an anti-inflammatory effect.
So, while others look for ways to test for the presence or absence of the bacteria, Novaks strategy is to try to make patients feel better by treating their symptoms.
FOLLOW NBC HEALTH ON &
Read Also: How Do You Get Rid Of Lyme Disease
How Is A Synovial Fluid Analysis Performed
First, your doctor will give you a local anesthetic to numb your joint. Then, they’ll put a needle in and take some fluid out. How much depends on the size of the joint and how many tests you’re going to have.
Your doctor will send your fluid to a lab, where a technician will do one or more of these:
- Check your fluid’s color and thickness
- Measure chemicals like glucose, protein, and uric acid
- See how many red and white blood cells and crystals your fluid has
- Test for bacteria, viruses, or other germs
What Are The Symptoms
The main feature of Lyme arthritis is obvious swelling of one or a few joints. While the knees are affected most often, other large joints such as the shoulder, ankle, elbow, jaw, wrist, and hip can also be involved. The joint may feel warm to the touch or cause pain during movement. Joint swelling can come and go or move between joints, and it may be difficult to detect in the shoulder, hip, or jaw. Lyme arthritis typically develops within one to a few months after infection.
Recommended Reading: Lab Work For Lyme Disease
Key Points For Healthcare Providers