What Should I Do If I Am Bitten By A Tick
If you experience a tick bite, the best way to remove it is by taking the following steps:
- Tug gently but firmly with blunt tweezers near the “head” of the tick at the level of your skin until it releases its hold on the skin.
- Avoid crushing the tick’s body or handling the tick with bare fingers as you could exposure yourself to the bacteria in the tick.
- Wash the bite area thoroughly with soap and water.
- DO NOT use kerosene, petroleum jelly , or hot cigarette butts to remove the tick.
- DO NOT squeeze the tick’s body with your fingers or tweezers.
What Do You Do If There’s A Tick Under Your Skin
Use a pair of fine-tipped tweezers to remove it as soon as possible. Pull upward with steady pressure. If parts of the tick are still in your skin, try to get those with the tweezers, too. After everything is out, clean the bite area with rubbing alcohol or soap and water.
You probably wonât get infected if you remove the tick within 36 to 48 hours.
How do you throw away a tick?
Put it in soapy water or alcohol, stick it to a piece of tape, or flush it down the toilet.
Questions To Ask Your Doctor
- I found a tick embedded in my skin, but I cant get it out. What should I do?
- Ive been bitten by a tick. Do I need to be seen?
- Do I need a blood test to confirm Lyme disease?
- Which antibiotic is best for me?
- How long will I have to take the antibiotic?
- What tick or insect repellent should I use for me or my child?
- How long will the symptoms last?
- What should I do if I still dont feel well a long time after I was bitten?
Read Also: What’s The Cure For Lyme Disease
Can Lyme Disease Be Prevented
To prevent Lyme disease, you should lower your risk of getting a tick bite:
- Avoid areas where ticks live, such as grassy, brushy, or wooded areas. If you are hiking, walk in the center of the trail to avoid brush and grass.
- Use an insect repellent with DEET
- Treat your clothing and gear with a repellant containing 0.5% permethrin
- Wear light-colored protective clothing, so you can easily see any ticks that get on you
- Wear a long-sleeve shirt and long pants. Also tuck your shirt into your pants and your pant legs into your socks.
- Check yourself, your children, and your pets daily for ticks. Carefully remove any ticks you find.
- Take a shower and wash and dry your clothes at high temperatures after being outdoors
Centers for Disease Control and Prevention
Lyme Disease: Symptoms & Side Effects

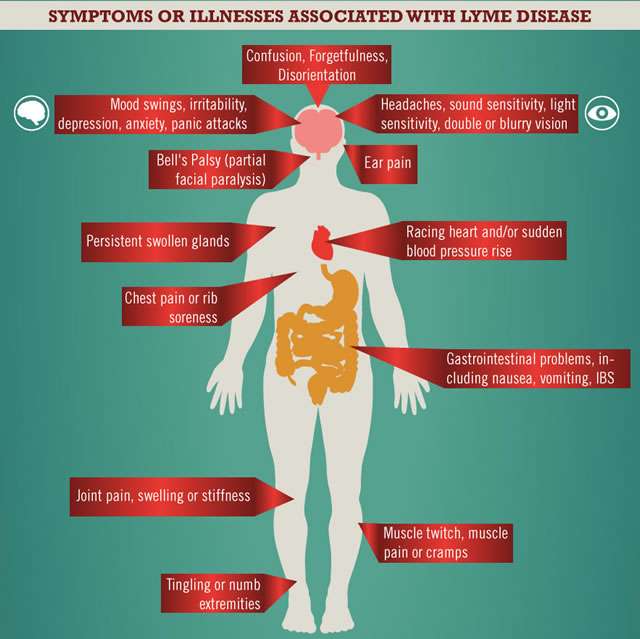
Lyme disease is a tick-born illness with over 150 symptoms, usually involving multiple systems. There are three stages of Lyme disease: early localized, early disseminated, and late persistent. If left untreated, it may progress into long-term disabilities. However, it is important to note that Lyme disease can lie dormant in your body for a prolonged period of time, and will invade when your immune system is compromised.
- Irritable bladder
- Upset stomach
- Pain in eyes, or swelling around eyes
- Oversensitivity to light
- Buzzing in ears
- Pain in ears, oversensitivity to sound
- Ringing in one or both ears
- Unexplained weight gain or loss
- Extreme fatigue
- Unexplained fevers
- Continual infections
- Symptoms seem to change, come and go
- Pain migrates to different body parts
- Early on, experienced a flu-like illness, after which you have not since felt well
- Twitching of facial or other muscles
- Facial paralysis
- Tingling of nose, cheek, or face
- Stiff or painful neck, creaks and cracks
- Jaw pain or stiffness
- Memory loss
- Confusion, difficulty in thinking
- Difficulty with concentration or reading
- Going to the wrong place
- Speech difficulty
- Stammering speech
- Any joint pain or swelling
- Stiffness of joints, back, neck
- Muscle pain or cramps
- Burning or stabbing sensations in the body
- Weakness or partial paralysis
- Numbness in body, tingling, pinpricks
- Poor balance, dizziness, difficulty walking
- Increased motion sickness
Recommended Reading: Can You Donate Plasma If You Have Lyme Disease
How You Get Lyme Disease
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks can be found in any areas with deep or overgrown plants where they have access to animals to feed on.
They’re common in woodland and moorland areas, but can also be found in gardens or parks.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
Prevention Of Lyme Disease
People should take precautions to avoid being bitten by a tick. If people may have been exposed to ticks, they should check their whole body very carefully after each possible exposure and remove any ticks they find. Checking is effective because ticks must usually be attached for more than a day and a half to transmit Lyme disease.
Also Check: What Type Of Doctor Treats Lyme Disease
What Do I Do If I Find A Tick On My Skin
Dont panic. Use fine-tipped tweezers to grasp the tick as close to the skins surface as possible. Pull up with steady, even pressure. Be careful not to squeeze or twist the tick body. Sometimes parts of the tick remain in the skin. You can leave them alone or carefully remove them the same way you would a splinter. Do not use heat , petroleum jelly, or other methods to try to make the tick back out on its own. These methods are not effective.
Wash the area where the tick was attached thoroughly with soap and water. Keep an eye on the area for a few weeks and note any changes. Call your doctor if you develop a rash around the area where the tick was attached. Be sure to tell your doctor that you were bitten by a tick and when it happened.
What Is Post Treatment Lyme Disease
Post Treatment Lyme Disease represents a research subset of patients who remain significantly ill 6 months or more following standard antibiotic therapy for Lyme disease. PTLD is characterized by a constellation of symptoms that includes severe fatigue, musculoskeletal pain, sleep disturbance, depression, and cognitive problems such as difficulty with short-term memory, speed of thinking, or multi-tasking. In the absence of a direct diagnostic biomarker blood test, PTLD has been difficult to define by physicians, and its existence has been controversial. However, our clinical research shows that meticulous patient evaluation when used alongside appropriate diagnostic testing can reliably identify patients with a history of previously treated Lyme disease who display the typical symptom patterns of PTLD.
You May Like: Lyme Disease Head Pressure Treatment
Stage : Late Disseminated Lyme Disease
Late disseminated Lyme disease occurs when the infection hasnt been treated in stages 1 and 2. Stage 3 can occur months or years after the tick bite.
This stage is characterized by:
- arthritis of one or more large joints
- brain disorders, such as encephalopathy, which can cause short-term memory loss, difficulty concentrating, mental fogginess, problems with following conversations and sleep disturbance
- numbness in the arms, legs, hands, or feet
The Unfortunate Connection Between Lyme Disease And Mental Illness
Carol has been a patient of mine for over five years. We have walked through some of the most difficult times in her life as she dealt with her failing marriage and then divorce, a move, significant career changes, undiagnosed medical issues, and co-parenting teenagers.
Yet during our discussions, there was an undercurrent of, I dont feel right. Her feelings were understandable given her life circumstances. But when life settled down, her complaints of pain, stress, fogginess, anxiety, and depression intensified. One medical doctor after the other ran tests with no conclusive diagnosis so she was labeled psychosomatic.
But that didnt make sense given that fact that she was consistent in therapy, did what was asked, and had significant improvements in several areas of her life. Something else seemed to be wrong. Finally, she found a doctor who tested her for Lyme disease, and she was properly diagnosed.
What is Lyme Disease? Lyme disease is aninfectious diseasecaused by abacteriaand spread byticks resulting in a suppression of the immune system. It can develop into a chronic multisystemic illness affecting the nervous system causing neurologic and psychiatric symptoms. These symptoms can mimic paranoia, dementia, schizophrenia, bipolar, panic attacks, depression, eating disorders, and obsessive-compulsive behaviors.
Also Check: Ivermectin Dose For Lyme Disease
Why Are Antibiotics The First Line Of Treatment For Lyme Disease
The use of antibiotics is critical for treating Lyme disease. Without antibiotic treatment, the Lyme disease causing bacteria can evade the host immune system, disseminate through the blood stream, and persist in the body. Antibiotics go into the bacteria preferentially and either stop the multiplication of the bacteria or disrupt the cell wall of the bacteria and kill the bacteria . By stopping the growth or killing the bacteria the human host immune response is given a leg up to eradicate the residual infection. Without antibiotics, the infection in Lyme disease can evade the host immune system and more readily persist.
Stage : Early Disseminated Lyme Disease
Early disseminated Lyme disease occurs several weeks to months after the tick bite.
Youll have a general feeling of being unwell, and a rash may appear in areas other than the tick bite.
This stage of the disease is primarily characterized by evidence of systemic infection, which means infection has spread throughout the body, including to other organs.
Symptoms can include:
- disturbances in heart rhythm, which can be caused by Lyme carditis
- neurologic conditions, such as numbness, tingling, facial and cranial nerve palsies, and meningitis
The symptoms of stages 1 and 2 can overlap.
Also Check: How Do You Tell If You Have Lyme Disease
Symptoms Of Post Treatment Lyme Disease
- Include severe fatigue, musculoskeletal pain, & cognitive problems
- Can significantly impact patients health and quality of life
- Can be debilitating and prolonged
Our research indicates the chronic symptom burden related to PTLD is significant. Although often invisible to others, the negative impact on quality of life and daily functioning is substantial for PTLD sufferers.
The chronic symptom burden related to Lyme disease is considerable, as shown on the left side of the graph above, and statistically significantly greater than the aches and pains of daily living experienced by the control group, on the right.
Risk Factors For Persistent Symptoms After Treatment For Lyme Disease
Patients with the most severe symptoms on clinical presentation are the most likely to have persistent symptoms during convalescence. Severe headache, arthritis, arthralgias, and fatigue at presentation predicted persistent symptoms in a retrospectively examined cohort of 215 patients. In a prospective treatment trial for early Lyme disease, persistent symptoms at several late follow-up visits were more common in patients who had more symptoms, higher symptom scores and multiple erythema migrans lesions. Patients with a longer duration of symptoms may also be at greater risk of persistent symptoms: a review of 38 subjects who had been previously treated for Lyme disease found that persistent somatic and neuropsychological sequelae were strongly associated with prolonged illness before treatment.
You May Like: How To Pay For Lyme Treatment
Lyme Vaccine Side Effects In Dogs
Lyme Disease can be a very serious disease for dogs. A vaccine for such a feared disease is great in theory. However many, many pets have had serious side effects from the Vaccine for Lyme Disease including behavioral changes, arthritis, pain, vomiting, lethargy, loss of consciousness, and death.
Earth Clinic readers have shared many alarming stories of reactions in their dogs to the Lyme Vaccine.
Anne from Wisconsin tells us, “My vet suggested my coonhound mix, Trixie, be vaccinated for Lyme disease even though I use tick prevention all year. Within 3 days she was having trouble moving her head and neck and “screamed” if anyone bumped her. She is normally somewhat crazy, jumping and barking at everything, but she stopped barking completely.”
“Maxsmom25” from UT shares that her four month old puppy had a reaction to the Lyme Vaccine, “It was terrifying. He went limp and was vomiting, luckily we were still at the vet so they were able to reverse it. But now I am terrified about going back to continue vaccinations!”
In Virginia, Pamela’s 11 year old dog went lame within 24 hours of receiving the Lyme Disease Vaccine.
The Confusing Terminology Of Chronic Lyme Disease
The mere name chronic Lyme disease is in itself a source of confusion. Lyme disease, in conventional use, specifically describes infection with the tick-borne spirochete B burgdorferi sensu lato. The diagnosis chronic Lyme disease, by incorporating that terminology, connotes a similar degree of microbiologic specificity the addition of the word chronic further implies that there is some distinction between chronic Lyme disease and other manifestations of the infection. This distinction in itself is problematic because several manifestations of Lyme disease may indeed present subacutely or chronically, including Lyme arthritis, acrodermatitis chronicum atrophicans, borrelial lymphocytoma, and late Lyme encephalopathy.
Chronic Lyme disease, however, has no clinical definition and is not characterized by any objective clinical findings. The only published attempt to define CLD provisionally produced a description too broad to distinguish CLD from myriad other medical conditions, and the case definition did not mention evidence of B burgdorferi infection . The absence of a definition makes it impossible to investigate whether a patient population with putative CLD has evidence of infection with B burgdorferi this would seem to be a basic requirement to include a syndrome within the term Lyme disease. It stands to reason that it is impossible to even posit a well-designed antibiotic trial when the study population is undefined.
Recommended Reading: Stop And Shop East Lyme
What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.
Microbiologic Investigations Into Chronic Lyme Disease
There is very little microbiologic evidence that supports persistent B burgdorferi infection in patients who lack objective manifestations of Lyme disease, such as erythema migrans, arthritis, meningitis, and neuropathies. Advocates for CLD contend that our ability to detectB burgdorferi is hampered by current technology and an incomplete scientific understanding of B burgdorferi, and that conventional diagnostic testing misses patients with CLD., Naturally, this raises the question of why we should assume that chronic B burgdorferi infection exists at all if we are so ill-equipped to detect it. Even when chronically symptomatic patients have a well-documented history of treated Lyme disease, investigators have been unable to document persistent infection. A recent study in which ticks were allowed to feed on persistently symptomatic posttreatment patients yielded molecular evidence of B burgdorferi in 1 of 16 patients and no patient had cultivatable organisms.
Because validated testing methods fail to support the connection between B burgdorferi and clinically diagnosed CLD, physicians who specialize in CLD often turn to alternative tests. This has included the use of novel culture techniques, detection of B burgdorferi DNA in urine specimens, and enumeration of CD57-positive lymphocytes. Independent investigations, however, have repudiated the validity of these tests.
Recommended Reading: Symptoms Of Lyme Disease In Dogs
Extended Antibiotics For The Treatment Of Post
Three research groups have examined prospectively the effectiveness of prolonged antibiotic courses for post-Lyme disease syndromes., All trials had strict entrance criteria similar to the aforementioned definition of PLDS. The Klempner and colleagues study reported 2 parallel trials in which their cohort of 129 subjects was divided into seropositive and seronegative arms. Subjects randomized to treatment groups received 30 days of intravenous ceftriaxone followed by 60 days of oral doxycycline. Those randomized to the placebo arm received IV placebo for 30 days, followed by an oral placebo for 60 days. The primary outcome was health-related quality of life as assessed by standardized instruments . These instruments were administered at baseline, and then 30, 90, and 180 days. There was no difference in any outcome measure between placebo and treatment groups in either the seropositive or seronegative arm, or in a detailed battery of neuropsychological tests that was published subsequently. Although all patients had complained of cognitive dysfunction at baseline , objective measures of cognitive function, such as memory and attention, were normal compared with age-referenced normative data. Depression, anxiety, and somatic complaints improved in both the antibiotic and placebo arms groups between baseline and day 180.
Lyme Vaccine Side Effects

The side effects of the Lyme vaccine mimic those of the actualdisease because of the proteins within it that pets arent typicallyexposed to. Experts have found this vaccine to cause arthritis,problems of the heart and nervous system, skin problems, and suddenkidney failure. Many veterinarians have reported that pets given theLyme vaccine display all the symptoms of Lyme disease, but bloodsamples taken from the pets showed no evidence that the pets contractedthe disease itself.
Research on the vaccine conducted on animals in a controlledenvironment found that those that were given a Lyme vaccine were morelikely to develop arthritis. This discovery has made veterinariansextra weary of vaccinating pets that are predispose to an autoimmunedisorder.
The adjuvants in the bacterin form of the Lyme vaccine are whatexperts believe causes the adverse side effects in the inoculation. Therecombinant form of the vaccine is less likely to cause adverse sideeffects as it doesnt contain adjuvants.
Recommended Reading: Lyme Disease And Joint Pain