How Is The Lyme Multiplex Assay Different From The Assay My Veterinarian Can Perform
Your veterinarian can perform a quick assay in-house that checks for antibodies against only one B. burgdorferi surface protein. The in-house assay cannot detect early infection, cannot determine vaccination status, and does not quantify the amount of antibodies your animal is producing. Quantifying antibodies is an important measure for successful treatment and to confirm cure from Lyme disease.
Lyme Disease: Symptoms & Side Effects
Lyme disease is a tick-born illness with over 150 symptoms, usually involving multiple systems. There are three stages of Lyme disease: early localized, early disseminated, and late persistent. If left untreated, it may progress into long-term disabilities. However, it is important to note that Lyme disease can lie dormant in your body for a prolonged period of time, and will invade when your immune system is compromised.
- Irritable bladder
- Upset stomach
- Pain in eyes, or swelling around eyes
- Oversensitivity to light
- Buzzing in ears
- Pain in ears, oversensitivity to sound
- Ringing in one or both ears
- Unexplained weight gain or loss
- Extreme fatigue
- Unexplained fevers
- Continual infections
- Symptoms seem to change, come and go
- Pain migrates to different body parts
- Early on, experienced a flu-like illness, after which you have not since felt well
- Twitching of facial or other muscles
- Facial paralysis
- Tingling of nose, cheek, or face
- Stiff or painful neck, creaks and cracks
- Jaw pain or stiffness
- Memory loss
- Confusion, difficulty in thinking
- Difficulty with concentration or reading
- Going to the wrong place
- Speech difficulty
- Stammering speech
- Any joint pain or swelling
- Stiffness of joints, back, neck
- Muscle pain or cramps
- Burning or stabbing sensations in the body
- Weakness or partial paralysis
- Numbness in body, tingling, pinpricks
- Poor balance, dizziness, difficulty walking
- Increased motion sickness
What Are The Symptoms Of Lyme Disease
Early symptoms of Lyme disease start between 3 to 30 days after an infected tick bites you. The symptoms can include:
- A red rash called erythema migrans . Most people with Lyme disease get this rash. It gets bigger over several days and may feel warm. It is usually not painful or itchy. As it starts to get better, parts of it may fade. Sometimes this makes the rash look like a “bull’s-eye.”
- Fever
- Muscle and joint aches
- Swollen lymph nodes
If the infection is not treated, it can spread to your joints, heart, and nervous system. The symptoms may include:
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of your body
- Facial palsy, which is a weakness in your facial muscles. It can cause drooping on one or both sides of your face.
- Arthritis with severe joint pain and swelling, especially in your knees and other large joints
- Pain that comes and goes in your tendons, muscles, joints, and bones
- Heart palpitations, which are feelings that your heart is skipping a beat, fluttering, pounding, or beating too hard or too fast
- Shooting pains, numbness, or tingling in the hands or feet
Read Also: Claritin Protocol For Lyme Disease
How You Get Lyme Disease
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks can be found in any areas with deep or overgrown plants where they have access to animals to feed on.
They’re common in woodland and moorland areas, but can also be found in gardens or parks.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
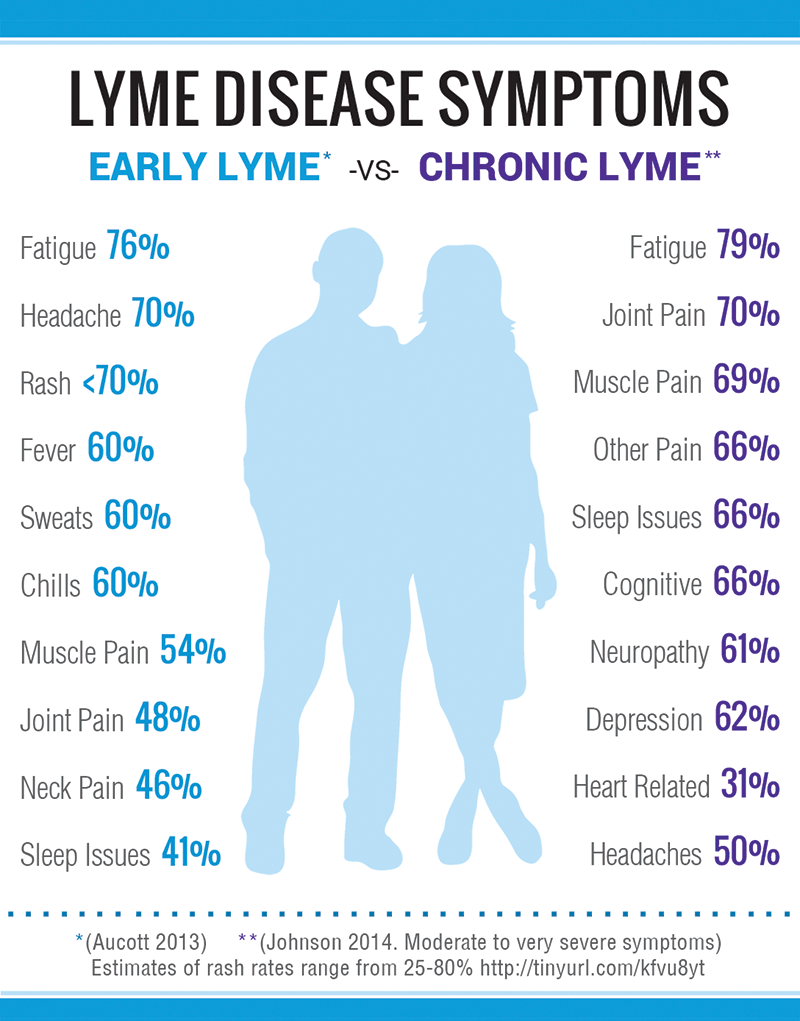
Chronic Lyme Disease Symptom Severity
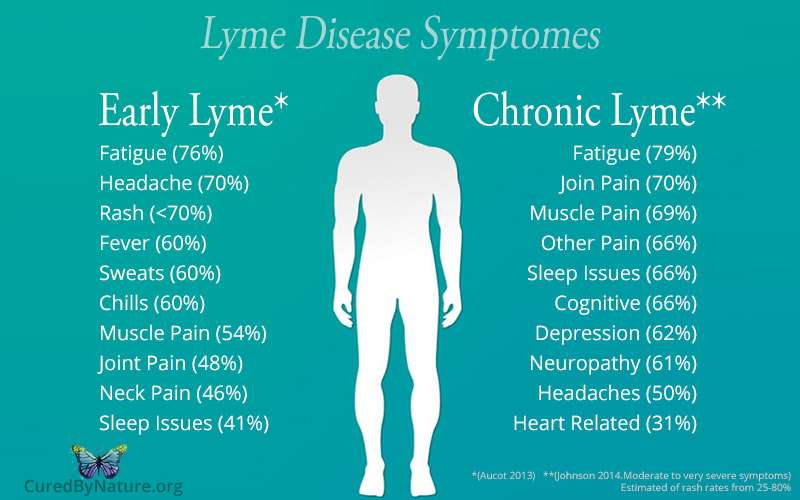
In LDos chronic Lyme disease survey, over 75% of patients reported at least one symptom as severe or very severe and 63% reported two or more such symptoms. Find out more about LDo peer-reviewed published surveys. The chart below shows the severity of ten common chronic Lyme symptoms.
The survey also found that patients with chronic Lyme disease have high disability and unemployment rates. Over 40% of patients with chronic Lyme disease reported that they currently are unable to work because of Lyme disease and 24% report that they have received disability at some point in their illness.
Read Also: Monastery Of Herbs Lyme Disease
When Should I Call The Doctor
If a tick bites you, call your doctor. Other conditions can cause similar symptoms, so it’s always a good idea to discuss them with your doctor. That way you can get checked and treated, if needed. Call right away if you get a red-ringed rash, lasting flu-like symptoms, joint pain or a swollen joint, or facial paralysis.
Long Term Effects Of Lyme Disease In Humans
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
You May Like: Neurological Disorders From Lyme Disease
How Long After Treatment Should The Horse/dog Be Re
Antibodies decrease slowly but gradually after the pathogen is cleared from the hosts circulation. Re-testing should not be performed too early. For horses/dogs with positive values for antibodies to OspF but negative values for antibodies to OspC , retesting should be done 3 months after the treatment was started. For horses with a positive OspC antibody value retesting can be done 6-8 weeks after the treatment started. At the time of retesting, a decrease of antibody levels can be expected in successfully treated animals. Serum antibodies may not have completely disappeared at this time. However, they should have dropped by about 40% of the original positive value.
Lymes Disease Prevention Tips
You and your loved ones can do your part to prevent tick bites and reduce your risk of Lyme disease.
- Know your surroundings. When in your yard or during outdoor activities, walk through designated trails and avoid overgrown areas.
- Spray before you go. Spray EPA-approved insect repellents on clothing when planning on being outdoors.
- Perform daily tick checks. Scan your clothes and entire body for ticks using a mirror for hard-to-see areas. Scan pets as well as they can carry ticks indoors.
- Remove attached ticks. If you spot a tick, remove it with sharp tweezers as soon as possible.
- Stay alert. Even if you dont see any attached ticks or remember being bitten, watch out for summer fevers or strange rashes as this can be a first sign.
- Encourage a tick-free environment. Modify your own backyard to reduce the presence of ticks. Keep patios and playground areas free of shrubs, bushes and other vegetation regularly maintain growth of all grass and plants in your yard.
- Practice prevention in your yard. Spray a pet-safe pesticide in your yard to reduce the number or ticks or prevent deer-resistant plants as deer are a food source for ticks.
Whether youre hiking, gardening or simply enjoying the outdoors this summer, ensure tick bites are part of your planning and preparation to avoid the bite that goes too far.
Don’t Miss: Old Lyme Homes For Sale
Importance Of The Study
The LymeProspect study shows that some Lyme patients remain limited in their physical and social functioning after treatment with antibiotics. In addition, fatigue, pain and concentration problems are reported more often by people with Lyme disease than by people without this disease: about 27% of the Lyme patients and 21% to 23% of the people without this disease. Also, the complaints of the Lyme patients were more severe. It is likely that such long-term symptoms may be the result of Lyme disease, but only in a small but substantial proportion of patients. It is important to acknowledge persistent symptoms and to obtain a better understanding of the causes of these symptoms. This can help prevent complaints and improve treatment.
Other Canine Diseases Carried By Ticks
Ticks can also carry several other less common but serious bacterial diseases affecting dogs, including anaplasmosis and babesiosis.
Anaplasmosis can involve symptoms similar to those for Lyme disease. Babesiosis can present with a wide range of symptoms, from sudden and severe shock, high fever, and dark urine to a slowly progressing infection with more subtle clinical signs. Diagnosis of both diseases includes blood tests similar to those used to check for Lyme disease.
Sometimes, dogs and people can become sick with co-infection of multiple tick-borne diseases, where more than one type of disease-causing bacteria is transmitted through a tick bite. This situation can make diagnosis and treatment even more challenging and difficult.
Don’t Miss: Does Lyme Disease Stay With You Forever
Lyme Disease Effects On The Brain
The first section of Lyme Brain discusses the fundamentals. What actually causes this condition? Research has shown that Lyme spirochetes can invade the brain and wreak all kinds of havoc. They damage nerve cells, trigger inflammation, release neurotoxins, and disrupt the balance of brain chemicals.
Ducharme lays all this out in plain language. She also explains how co-infections contribute to Lyme disease brain:
One of the reasons I believe that the actual brain fog, memory issues and difficulty with focus and concentration is Borrelia driven is because when I treat my patients with medications that primarily impact Borrelia and cross the blood-brain barrier, I see these symptoms improve, whereas the insomnia and wacky dreams tend to respond more to Babesia treatment. Really extreme psychiatric symptoms such as rages, and suicidal thoughts and behaviors, respond mostly to Bartonella treatment.
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Don’t Miss: How Do You Get Rid Of Lyme Disease
How Lyme Gets Into Your Brain
To understand how Lyme disease affects, the brain, its important to understand the different phases of the infection. Ticks, specifically deer ticks in the northeastern U.S., are the carriers of the bacteria spirochete Borrelia burgdorferi that causes Lyme disease. In particular, its the small, immature tick nymphs that feed on animals like the white-footed mouse, squirrels and other small mammals that serve as reservoirs for Borrelia burgdorferi. Later, an infected tick will attach themselves to a person or other mammal. Once attached, the tick will gorge on the blood of its host for several days. Many
Infection Phase
Even prior to entering the host, S. Borrelia Burgdorferi has its work to do. Host blood enters the tick gut during feeding, as S. Borrelia Burgdorferi simultaneously begins to multiply in preparation to travel to the ticks salivary glands. As the bacteria enter the host, there are several mechanisms that make it difficult for the immune system to attack and eradicate S. Borrelia Burgdorferi.
First, to avoid an immune response from the host, the bacteria decrease the number of surface proteins that signal a pro-inflammatory response. These proteins are normally found at high levels within the tick gut, but are significantly decreased during feeding periods.
Chronic Lyme Disease Patients Profoundly Debilitated
Many patients with chronic Lyme disease are profoundly debilitated. Investigators of the four NIH-sponsored retreatment trials documented that the patients quality of life was consistently worse than that of control populations and equivalent to that of patients with congestive heart failure. Pain levels were similar to those of post-surgical patients, and fatigue was on par with that seen in multiple sclerosis.
An LDo published survey of over 3,000 patients with chronic Lyme disease found that patients suffer a worse quality of life than most other chronic illnesses, including congestive heart failure, diabetes, multiple sclerosis and arthritis. Over 70% of patients with chronic Lyme disease reported fair or poor health. Similar results have been found in other studies. Many of the symptoms associated with Lyme disease are common in other diseases. The CDC surveillance criteria for confirmed cases specifically exclude most of the symptoms that patients report, including fatigue, sleep impairment, joint pain, muscle aches, other pain, depression, cognitive impairment, neuropathy, and headaches. However, these common symptoms can be severe and may seriously affect quality of life.
Don’t Miss: Fda Approved Lyme Disease Test
How Can Lyme Disease Last For Years
Category: Health Published: October 9, 2015
If treated, Lyme disease does not last for years. However, for some people, the after-effects of the disease can linger for months and sometimes even years. Alternative medicine providers call this condition “Chronic Lyme disease,” but this title is simply wrong. For a person who has been infected with Lyme disease and then treated, the bacteria that causes Lyme disease is measurably no longer present in his body, even though he may still feel some symptoms. The correct title for this condition is therefore “Post-treatment Lyme Disease Syndrome.”
Lyme disease is an infection caused by a bacteria known as Borrelia burgdorferi. This bacteria is delivered to humans through tick bites. From the bite site, the bacteria can enter the bloodstream and spread throughout the body. Usually, but not always, an infectious tick bite causes a characteristic red rash at the site of the bite. Other symptoms include fever, muscle soreness, headache, fatigue, and dizziness. In a few cases, symptoms can also include mood swings, memory loss, and sleep disturbance. If left untreated for too long, Lyme disease can lead to nerve damage, thereby causing shooting pain, numbness, and even paralysis.
The CDC states,
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Read Also: What Are Tests For Lyme Disease
Chances Of Developing Lyme Disease Depends On Three Factors:
Lyme disease is generally transmitted through infected blacklegged ticks typically found in grassy or wooded areas typical to the Northeast. According to the CDC, a tick has to be attached for at least 24 hours before it can transmit Lyme disease, and it doesnt help that ticks are typically found in hard-to-see areas such as the scalp, groin and armpit, often going unnoticed right away.
What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.
Also Check: Symptoms Of Lyme Disease In Dogs
What Should You Do If You Find A Tick
-
Don’t touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Don’t squeeze the tick, and don’t use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
How Is Lyme Disease Diagnosed
To make a diagnosis, your health care provider will consider:
- Your symptoms
- How likely it is that you were exposed to infected blacklegged ticks
- The possibility that other illnesses may cause similar symptoms
- Results of any lab tests
Most Lyme disease tests check for antibodies made by the body in response to infection. These antibodies can take several weeks to develop. If you are tested right away, it may not show that you have Lyme disease, even if you have it. So you may need to have another test later.
You May Like: Cure Lyme Disease Without Antibiotics
The Effects Of Lyme Disease On The Nervous System
A limping dancer, a student forced to the bench.
According to Dr. Erik Kolbenheyer, an internist, gastroenterologist, family doctor, occupational health specialist, doctor of traditional Chinese medicine, there are some particularly interesting cases of Lyme borreliosis, where the disease causes bizarre symptoms in the nervous system. The doctor, who, being personally affected by the disease, turns to his patients with excellent diagnostic sense and great empathy, presents two shocking cases from his own practice when young people became ill but fortunately, their quality of life essentially returned to its previous level.
In cases where the bacteria attack the nervous system, anxiety, depression, panic attacks, and strange movement disorders may appear. It is a very complex set of symptoms, so in these cases, the help of a neurologist is needed to examine the patient in other directions. As the symptoms of the nervous system can take on quite unusual forms, patients and relatives might panic.