Diagnosing Cervical Spinal Stenosis
Dr. Rowe recommends MRI studies in individuals with abnormal findings following a careful neurological examination. Those findings include pathologically brisk reflexes, a positive Hoffmans sign, abnormal Romberg sign, or other abnormalities suggestive of a cervical myelopathy. A family history of the disease can also support getting an MRI. Dr. Rowe emphasized that he does not obtain cervical spine MRIs in all ME/CFS patients.
Showing hyperreflexia, clonus and a positive Hoffmans sign
Both Rowe and Heffetz suggested that the bias associated with a chronic fatigue syndrome and fibromyalgia diagnosis may be causing some doctors to not dig deep enough when confronted with signs of spinal stenosis.
Because few doctors will think of spinal stenosis in connection with ME/CFS or FM, showing them Dr. Rowes case report and Dr. Heffetzs fibromyalgia study ) should help. Both papers specifically note that spinal stenosis can cause the symptoms associated with ME/CFS and fibromyalgia.
Various medical websites cite a variety of tests used to diagnose spinal stenosis. If spinal stenosis is being checked, though, other spinal issues sometimes associated with ME/CFS and FM such as craniocervical instability, Chiari malformation and tethered cord syndrome should be checked at the same time. CCI requires a top-of-the-line MRI. Testing with the head extended / flexed appears to be recommended for both spinal stenosis and CCI.
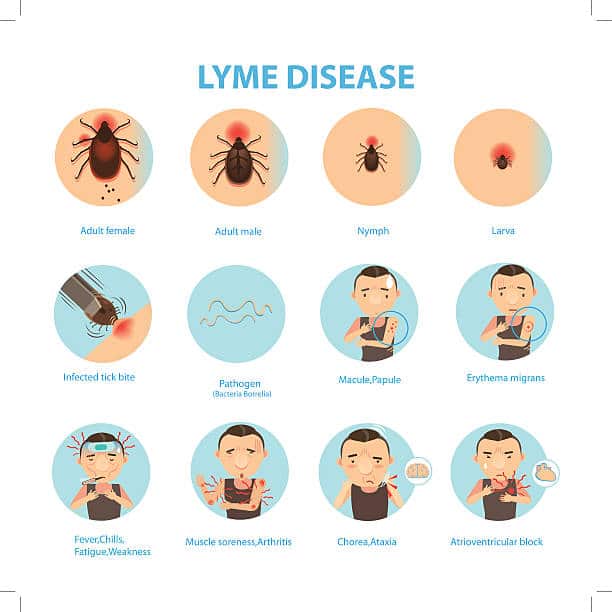
What Causes Lyme Disease
Lyme disease is caused by bacteria. Infected ticks spread the bacteria by biting people or animals.
Two types of ticks carry the Lyme disease bacteria in Canada. They are:
- Deer ticks. They spread the disease in the eastern and south-central areas of Canada.
- Western black-legged ticks. They spread the disease along the Pacific coast, mostly in southern British Columbia.
Remove ticks as soon as you notice them. Infected ticks usually don’t spread Lyme disease until they have been attached for at least 36 hours.
The Extended Effects Of Lyme Disease
If you are reading this, it is likely that your doctor has already diagnosed you with Lyme disease, and they have put you on a treatment regimen. It is also likely that while some of your symptoms have cleared up, the joint pain and debilitating headaches continue.
This is not uncommon. Many individuals diagnosed with Lyme disease find relief from some of the annoying symptoms, but the pain, the hampered motor skills, and the inflammation persist. This is in part because of the way Lyme disease compromises your immune system. It leaves your body prone to inflammation and to infection.
Many Lyme disease sufferers say that some days they cannot even get out of bed. It is not uncommon for adults diagnosed to quit their job. Children and teenagers diagnosed with Lyme disease may opt to study at home because of the pain and frustration of Lyme disease.
Read Also: What Tests Are Done For Lyme Disease
What You Need To Know
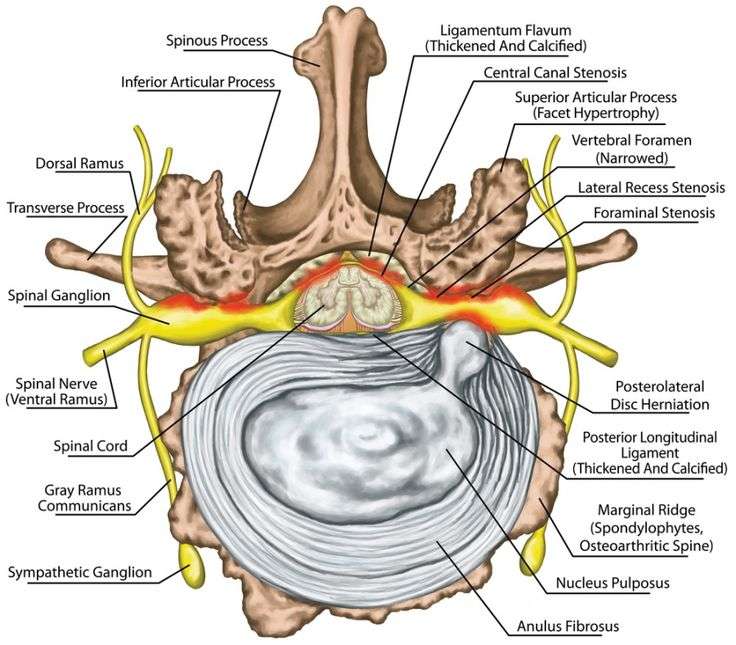
- Radiculopathy describes a range of symptoms produced by the pinching of a nerve root in the spinal column.
- The pinched nerve can occur at different areas along the spine .
- Symptoms of radiculopathy vary by location but frequently include pain, weakness, numbness and tingling.
- A common cause of radiculopathy is narrowing of the space where nerve roots exit the spine, which can be a result of stenosis, bone spurs, disc herniation or other conditions.
- Radiculopathy symptoms can often be managed with nonsurgical treatments, but minimally invasive surgery can also help some patients.
Neck Pain From Lyme Disease

Lyme disease is commonly associated with tick bites and a big circular rash. However, a tick bite does not hurt and many people do not recall being bit or seeing the rash. Further complicating matters, Lyme disease symptoms may start out minor and not become problematic for months or longer.
Lyme disease causes neck pain in more than 30% of cases. Watch:Neck Pain Causes Video
Media reports rarely focus on neck pain with Lyme disease, but some estimates note that it occurs in more than 30% of the cases and is typically one of the earlier symptoms.1 Recognizing Lyme disease early and seeking treatment can make a big difference in the outcome.
Don’t Miss: Lyme Disease Doctors In Virginia
British Columbia Specific Information
Ticks are tiny bugs which feed on blood. For information on ticks, removing ticks, and how to avoid being bitten, see HealthLinkBC File #01 Tick Bites and Disease. You may also be interested in the HealthLinkBC File #96 Insect Repellent and DEET.
While most tick bites do not result in diseases, some can. Some of the diseases passed on by ticks include relapsing fever, tularemia, Rocky Mountain Spotted Fever , Q Fever and anaplasmosis. The most well-known is Lyme disease. For more information on Lyme Disease, visit BC Centre for Disease Control – Lyme Disease .
Should You Use Antibiotics
Different antibiotics may be used to treat children and adults. The decision to take medicines for Lyme disease may be based on one or more of these factors:
- You have symptoms of Lyme disease, especially the red, circular rash, and a history of exposure to ticks in geographic regions where Lyme disease is known to occur.
- Blood tests show that you have antibodies to the Lyme disease bacteria in your blood, spinal fluid, or joint fluid.
- You are pregnant or breastfeeding and are bitten by a tick.
Read Also: When Should You Get Tested For Lyme Disease
Chronic Pain Due To Lyme Disease
In late 1975, a group of Yale scientists traveled to Lyme, Connecticut to investigate what they thought was an outbreak of rheumatoid arthritis . The most common symptom among the 51 patients was recurrent attacks of knee swelling. Others remembered a round rash before the onset of other symptoms . We now know these patients were suffering from Lyme disease, named for the town in which it was discovered. Today, Lyme disease is the most common vector-borne illness in the United States in 2019, a total of 34,945 confirmed and probable cases of Lyme disease were reported to the CDC . In large part due to advocacy efforts by people with Lyme disease, chronic pain due to the condition is gaining awareness from the medical community.
The exact cause of PTLDS is not known, leading to debate surrounding appropriate treatment . Some practitioners suggest continued antibiotic therapy, but evidence shows that it does not improve chances of recovery and might even cause complications . A range of medications can be used to reduce pain and discomfort, such as prescription or OTC pain relievers, NSAIDs and intra-articular steroids for joint swelling some research even suggests TNF inhibitors . Other sufferers find relief through yoga, homeopathy, and Reiki . Fortunately, an increasing number of doctors are receptive to the existence of PTLDS, which means that treatment and management approaches will continue to improve.
References
Is Your Back Pain Caused By Lyme Disease
Back pain can have a number of different causes. One potential cause that you may not immediately think about is Lyme disease. Lyme disease tends to be especially prevalent during the summer months when the weather is warm and people are more likely to be outside in nature. To learn more about how Lyme disease can cause back pain, we must first understand what Lyme disease is, how it spreads, and how it affects the body.
Lyme disease is a bacterial infection that is spread by infected ticks. It is most commonly spread by the blacklegged tick, which is commonly referred to as deer ticks. These ticks are found throughout the eastern United States and infect an estimated 329,000 individuals annually. Within that number, around 15% of people with Lyme disease can experience back pain.
Lyme disease affects the body in a few different ways. One of the first distinguishing signs of Lyme disease is a circular rash that forms on the skin surrounding the tick bite. Additionally, Lyme disease can also cause fatigue, fever, and pain in the muscles and joints. It can also cause a phenomenon known as Lyme arthritis.
- P.O. Box 631, Westwood, NJ 07675
Doctors
Also Check: Early Signs Of Lyme Disease In Humans
What Is Lumbar Spinal Stenosis
Lumbar spinal stenosis is a narrowing of the spinal canal in the lower back, known as the lumbar area.
This usually happens when bone or tissueor bothgrow in the openings in the spinal bones. This growth can squeeze and irritate nerves that branch out from the spinal cord.
The result can be pain, numbness, or weakness, most often in the legs, feet, and buttocks.
Early Prediction Of Outcomes
Prompt diagnosis and treatment of Lyme disease is important to avoid the associated complications. Patients with cardiac conduction abnormalities, arthritis, and neurologic manifestation typically respond well to antibiotic therapy. Often, these patients do not require long term cardiac pacing or orthopedic intervention after receiving adequate antibiotic treatment.
Also Check: Do All Ticks Cause Lyme Disease
Prolotherapy The Curve Of The Neck And Blood Flow
In this image, the progression and degeneration of the cervical spine are demonstrated, from the Lordotic curve to the Military curve to the Kyphotic curve to the S curve of severe osteoarthritis.
In February 2016 a paper appeared in the Medical Science Monitor: International Medical Journal of Experimental and Clinical Research. Here medical university researchers in Turkey made these observations:
- The vertebral arteries proceed in the transverse foramen of each cervical vertebra. Considering that the vertebral arteries travel in a close anatomical relationship to the cervical spine, we speculated that the loss of cervical lordosis may affect vertebral artery hemodynamics. .
This is research with which we have seen empirical evidence in our over 27 years of regenerative medicine practice. To fix the problems related to the cervical spine, you need to restore the natural curvature of the neck.
In the medical journal Brain Circulation , doctors wrote up their analysis of case study patients who had cervical lordosis. They wrote that if you restored the natural curve to the neck, you could immediately increase cerebral blood flow as pressure is removed from the cerebral artery.
Here are the learning points of this research. They present a good summary of what we discussed in this article:
What Increases Your Risk
The main risk factor for Lyme disease is exposure to ticks that are infected with Lyme disease bacteria. In areas where Lyme disease is widespread, such as the eastern and south-central areas of Canada, southern British Columbia, and northeastern United States, several factors may increase your risk, including:
- Spending time outdoors during the warm months of the year when ticks are most active. This is usually between May and November, with peak activity in June and July.
- Having indoor/outdoor pets. They can bring infected ticks into the house. Although dogs and cats can become infected with the Lyme disease bacteria, they cannot pass the illness to humans. But the infected ticks can drop off the animal and then bite and infect a person.
- Having a stone fence or a bird feeder near your house. Stone fences often become homes for mice, and mice may feed on spilled seed from a bird feeder. Where there are mice, there are ticks.
Remove ticks right away, as soon as you notice them. Your risk for getting Lyme disease increases the longer a tick is attached to your body. Ticks generally cannot transmit Lyme disease until they are attached for at least 36 hours.
Don’t Miss: How To Cure Lyme Disease
Upper Respiratory Infections Can Cause Atlantoaxial Instability
The last example is a rare condition called Grisels Syndrome. First documented in the 1830s, it is a form of non-traumatic atlantoaxial instability that generally occurs after an upper respiratory infection. It can also develop following post-operative inflammation in susceptible individuals. Children are thought to be more susceptible because their atlantoaxial joint, specifically the transverse ligament, is naturally more lax. Children with Down Syndrome are also more susceptible. I wonder if people with connective tissue disorders like Ehlers-Danlos Syndrome or Marfan Syndrome are as well. Its most obvious sign is torticollis, a stiff, turned neck.
Treatments include addressing the infection, administering anti-inflammatories, immobilization the neck , andbedrest. Early treatment is crucial to prevent long-term sequelae. If Grisels syndrome is detected and treated early, surgical fusion can usually be avoided.
The closest analogy to my form of cervical pathology, CCI/AAI, is Grisels syndrome. I cant help but wonder if at the time of my viral onset, had I addressed the inflammation taken antivirals much earlier aggressively rested and protected my neck, might have I avoided the long-term sequelae that came in full force 18 months later, the cluster of symptoms that we call ME?
Symptoms Of Autoimmune Spinal Disorders
With the exception of rheumatoid arthritis, many autoimmune spinal diseases start with sacroiliac joint involvement, the joints in the back of the pelvis. One of these diseases attacks the SI joint bilaterally but most of these disorders only cause unilateral SI joint injury.
The classic first symptoms are pain and stiffness in the morning that disappears with activity. Fatigue is also a common symptom of these rheumatologic conditions that affect the spine. Stiffness that disappears with exercise is very typical for spinal autoimmune disorders. Be forewarned that lumbar degenerative disc disease can also display similar symptoms.
Rheumatoid arthritis, psoriasis, ulcerative colitis, Crohns disease, Reiters syndrome, ankylosing spondylitis, lupus , myositis, polymyalgia rheumatica, and DISH are some of the spondyloarthropathy diseases associated with spine pain and stiffness.
Also Check: Ways To Get Lyme Disease
Available Or Current Treatment Guidelines
The Infectious Diseases Society of America and International Lyme and Associated Diseases Society have both released official treatment guidelines. For asymptomatic tick bite the IDSA recommends one 200 mg dose of doxycycline whereas the ILADS recommends doxycycline 100 mg BID for 20 days. For erythema migrans the IDSA recommends doxycycline, amoxicillin, or cefuroxime for 14-21 days. ILADS recommends 28-42 days of therapy with the same antibiotics or azithromycin for at least 21 days. The IDSA does not recommend additional antibiotics after this, whereas ILADS recommends discussing treatment desires with the patient if clinical improvement continues while on antibiotics.
What Is Neurologic Lyme Disease
Neurologic symptoms of Lyme disease occur when the Lyme disease bacteria affect the peripheral or central nervous systems.
- Cranial nerve involvement: When the cranial nerves are affected, facial palsy can occur on one or both sides of the face.
- Peripheral nerve involvement: When the peripheral nerves are affected, patients can develop radiculoneuropathy which can cause numbness, tingling, shooting pain, or weakness in the arms or legs.
- Central nervous system involvement: When the central nervous system is affected, Lyme meningitis can cause fever, headache, sensitivity to light, and stiff neck.
Out of every 100 patients whose cases are reported to CDC, 9 have facial palsy, 4 have radiculopathy, and 3 have meningitis or encephalitis. Because of reporting practices, this statistic may overestimate how often these manifestations are seen by clinicians.
Recommended Reading: How Do You Get Tested For Lyme Disease
Spinal Fluid Proteins Distinguish Lyme Disease From Chronic Fatigue Syndrome
- Date:
- Public Library of Science
- Summary:
- Patients who suffer from neurologic post treatment Lyme disease and those with the chronic fatigue syndrome report similar symptoms. However, unique proteins discovered in spinal fluid can distinguish those two groups from one another and also from people in normal health, according to new research.
Patients who suffer from Neurologic Post Treatment Lyme disease and those with the chronic fatigue syndrome report similar symptoms. However unique proteins discovered in spinal fluid can distinguish those two groups from one another and also from people in normal health, according to new research conducted by a team led by Steven E. Schutzer, MD, of the University of Medicine and Dentistry of New Jersey — New Jersey Medical School, and Richard D. Smith, Ph.D., of Pacific Northwest National Laboratory.
This finding, published in the journal PLoS ONE, also suggests that both conditions involve the central nervous system and that protein abnormalities in the central nervous system are causes and/or effects of both conditions.
This research represents the most comprehensive analysis of the complete CSF proteome to date for both Chronic Fatigue Syndrome and Neurologic Post Treatment Lyme disease . Prior to this study, many scientists believed that CFS was an umbrella category that included nPTLS. However these results call those previous suppositions into question.
Late Persistent Lyme Disease
If Lyme disease isn’t promptly or effectively treated, damage to the joints, nerves, and brain may develop months or years after you become infected. It is the last and often the most serious stage of the disease.
Symptoms at this stage may include:
- Arthritis that most often affects the knee. A small number of people eventually get chronic Lyme arthritis, which causes recurring episodes of swelling, redness, and fluid buildup in one or more joints that last up to 6 months at a time.
- Numbness and tingling in the hands, feet, or back.
- Feeling very tired.
- Not being able to control the muscles of the face.
- Problems with memory, mood, or sleep, and sometimes problems speaking.
- Heart problems, which are rare but can occur months to even years after you are bitten by an infected tick. The most serious heart problemssuch as inflammation of the structures surrounding the heart usually resolve without any lifelong damage. Unfortunately, heart problems can be the first sign of Lyme disease in a small number of people who didn’t have early symptoms.
Stage 2 and stage 3 symptoms may be the first signs of Lyme disease in people who didn’t have a rash or other symptoms of early infection.
Read Also: How To Kill Lyme Disease Naturally
Key Points About Sciatica
- Sciatica is described as pain that originates in the sciatic nerve and radiates through the buttocks down to the leg and feet.
- People between 30 and 50 years old are most likely to develop sciatica.
- Disc herniation, spinal stenosis, and spinal bone spurs are the most frequent causes of sciatica.
- Symptoms of sciatica range from pain in the lower back, or buttocks to shooting pain down the leg and inability to move your legs or feet.
- Most patients do not need invasive treatment for sciatica. Many can find symptoms of relief with rest and self-care measures.