Does Lyme Disease Create Lesions In Your Brain
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Lyme Disease Effects On The Brain
The first section of Lyme Brain discusses the fundamentals. What actually causes this condition? Research has shown that Lyme spirochetes can invade the brain and wreak all kinds of havoc. They damage nerve cells, trigger inflammation, release neurotoxins, and disrupt the balance of brain chemicals.
Ducharme lays all this out in plain language. She also explains how co-infections contribute to Lyme disease brain:
One of the reasons I believe that the actual brain fog, memory issues and difficulty with focus and concentration is Borrelia driven is because when I treat my patients with medications that primarily impact Borrelia and cross the blood-brain barrier, I see these symptoms improve, whereas the insomnia and wacky dreams tend to respond more to Babesia treatment. Really extreme psychiatric symptoms such as rages, and suicidal thoughts and behaviors, respond mostly to Bartonella treatment.
Lyme Sci: When Brain Inflammation Persists After Lyme Disease Treatment
In a new study, researchers from the Johns Hopkins School of Medicine have found evidence of chemical changes and widespread inflammation in the brains of patients with chronic symptoms following treatment for Lyme disease.
This Johns Hopkins study, in Journal of Neuroinflammation, supports the experience of hundreds of thousands of patients who have tried for years to have their chronic symptoms of pain, sleep disturbance, fatigue, and cognitive impairment validated.
What this study does is provide evidence that the brain fog in patients with post-treatment Lyme disease syndrome has a physiological basis and isnt just psychosomatic or related to depression or anxiety, says John Aucott, M.D., a senior author of the new paper and director of the Johns Hopkins Lyme Disease Research Center.
The fact is, too many patients with Lyme disease are left with chronic, debilitating symptoms following treatment for Lyme disease. In the nearly 40 years since the discovery of Lyme, no one has been able to determine why some patients get better with treatment and others remain ill.
Don’t Miss: Lyme Vaccine For Dogs How Often
Treating Neurological Lyme Disease
Though neurological and psychiatric symptoms can be reduced with antibiotic treatment, emotional and cognitive problems arising from late-stage or chronic Lyme often call for a broader range of interventions. This includes lifestyle changes in such areas as diet, exercise, and environment.
Again, its worth reiterating that the longer an infection goes undetected, the harder it is to treat, and the more likely it is that symptoms will require multi-pronged, multi-system interventions besides antibiotics alone.
Infectious Diseases And Mental Health
Lyme disease and TBRF are not the only infectious disease to have ties to mental illness. One of the earliest and most well-known examples of an infectious disease that causes neurological and psychiatric symptoms is syphilis.
This sexually transmitted disease, which like Lyme is caused by a spiral-shaped bacteria and treated at early stages with antibiotics, has been called the great imitator also like Lyme because its symptoms can be wide-ranging and non-specific, especially at late stages. That includes neurological and psychiatric symptoms that become much more likely the longer the disease goes untreated.
Given that ties between late-stage syphilis and mental illness have long been recognized by the medical community, it shouldnt be surprising that untreated Lyme disease poses similar risks to patients psychological wellbeing. Recent studies have investigated possible connections between Lyme disease and a host of mental health issues, including:
- Developmental disorders
- Seizures
- Suicide
Yet there are still many doctors and scientists who doubt the existence of chronic Lyme disease, and/or do not realize how many different borrelia cause TBRF, hurting patients chances of fighting both the diseases themselves and their mental health consequences.
Read Also: Lyme Disease Specialists In Pa
Cerebrovascular Manifestations Of Lyme Neuroborreliosisa Systematic Review Of Published Cases
- 1Department of Radiology, Medical University of Biaystok, Biaystok, Poland
- 2Department of Infectious Diseases and Neuroinfections, Medical University of Biaystok, Biaystok, Poland
- 3Department of Neurology, Medical University of Biaystok, Biaystok, Poland
- 4Faculty of Applied Informatics and Mathematics, Warsaw University of Life Sciences SGGW, Warsaw, Poland
- 5Independent Department, Laboratory of Molecular Imaging, Medical University of Biaystok, Biaystok, Poland
Background: Lyme neuroborreliosis is a disease caused by spirochete Borrelia burgdorferi, involving the nervous system. It usually manifests as lymphocytic meningoradiculitis, but in rare cases, it can also lead to cerebrovascular complications. We aimed to perform a systematic review of all reported cases of LNB complicated by central nervous system vasculitis and stroke or transient ischemic attack .
Materials and methods: We conducted a systematic review of literature between May 1987 and December 2016 with patients who presented with cerebrovascular course of LNB.
Cerebral vasculitis and stroke due to LNB should be considered, especially in patients who live in or have come from areas with high prevalence of tick-borne diseases, as well as in those without cardiovascular risk factors, but with stroke-like symptoms of unknown cause.
Whats The Difference Between Neurologic Lyme Disease And Ms
Olga Syritsyna, MD
Hearing the words you have Lyme disease or you have MS can be quite unsettling. And to complicate matters, when Lyme disease affects the central nervous system, the symptoms can be very similar to MS. So it can be hard to tell the difference to the untrained eye. Many doctors are generalists and not specially trained to diagnose either disease. Dr. Olga Syritsyna is a neurologist with subspecialty training in neurologic Lyme disease and MS.
What is neurologic Lyme disease?First, lets start with defining Lyme disease. Its a seasonal tick-borne infection caused by the borrelia burgdorferi bacteria that can affect multiple organs and systems in the body. Its named after Lyme, CT, where it was first identified in 1975. In about 15 percent of cases, Lyme disease affects the central nervous system. When it does, it is known as neurologic Lyme disease. Sometimes, people who think they may have Lyme disease find out they have MS . Lyme disease as an infection can act to trigger MS attacks. This is why being seen by a neurologist specially trained to know the differences is key.
Why choose Stony Brook for diagnosis and treatment of neurologic Lyme disease?For neurologic Lyme disease, Stony Brook has extensive experience in detecting antibodies to the borrelia burgdorferi bacteria that is carried by ticks and can affect the central nervous system. We do frequent lumbar punctures and perform a variety of tests on cerebrospinal fluid.
Read Also: Treating Lyme Disease With Essential Oils
What Is Lyme Disease
B. burgdorferi is spread by several species of hard-bodied ticks. In the United States, the disease is primarily spread by the blacklegged tick, or deer tick, and the western blacklegged tick. Ticks are known as hematophages, meaning they need blood to survive and move through their life cycle. Ticks generally become infected with B. burgdorferi in the first stage of their life cycle when they bite infected small mammals or birds. Subsequently, when they feed on the blood of a new host, B. burgdorferi will pass from the tick to the new host.
After their first blood meal, the tick enters its nymph stage, which is a part of the insect life cycle where the insect is not quite an adult but resembles the adult form. Nymphal ticks feed on small mammals or birds, which helps to spread B. burgdorferi among these populations.
Nymphal ticks can also feed on humans, however, and they are the most common source of Lyme disease because they are very small at that stage . Thus, they are more likely to go unnoticed while they are attached to a host, which allows them to stay attached for the amount of time it takes Lyme to be transmitted . Since humans aren’t thought to spread B. burgdorferi among themselves or to other animals, they are considered a dead-end host for the bacteria . Adult ticks can feed on humans too, but are most commonly found on large animals in the wild, like deer.
The Role Of Coinfections
Ticks carry more diseases than just Lyme and TBRF, and its not uncommon for patients to be infected with more than one type of disease-causing bacteria.
Common coinfections such as Babesiosis and Bartonellosis can not only cause neurological and psychiatric symptoms of their own, but they can also complicate the diagnostic process, delaying proper diagnosis and treatment all of which increase the risk of developing emotional, behavioral, or cognitive problems from the infection.
Recommended Reading: Colloidal Silver Lyme Disease Treatment
What Is Multiple Sclerosis
MS is a nervous system condition caused by immune system dysfunction. It affects your central nervous system. If you have MS, your immune system attacks the protective layer that covers nerve fibers, known as myelin. This causes problems in impulse transmission between your brain and spinal cord and the rest of your body, resulting in a range of symptoms.
MS is more commonly diagnosed in young adults and in those prior to middle age. Almost 1,000,000 people in the United States have it. It can range from mild to severe and is a lifelong condition.
Symptoms of MS can come and go but generally become more present with time. The exact causes of MS are unknown. Immunologic, environmental, infectious, and genetic factors are all suspected to contribute to this autoimmune condition.
Does Lyme Disease Cause Brain Lesions
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Also Check: Lyme Disease Blood Test Name
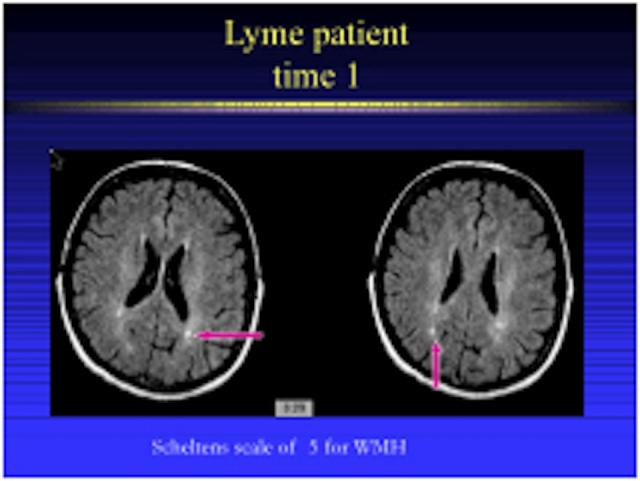
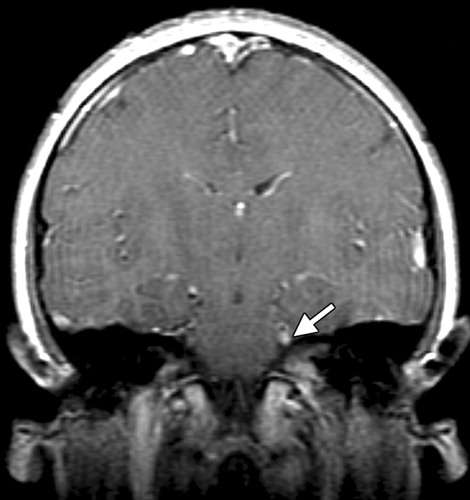
Imaging In Lyme Neuroborreliosis
There is limited knowledge of structural and functional changes in LNB with quantitative MRI techniques. Three studies have reported structural changes, and no difference between the patients and controls was found . However, these studies included a limited number of subjects and controls , so they probably lacked power to show subtle changes. Functional studies have been conducted with PET and with SPECT . These studies reported regional hypoactivity and hypoperfusion, but were hampered by heterogeneous study populations with non-specific symptoms and included individuals with uncertain diagnoses. Larger, prospectively conducted case-control studies are needed to learn more about imaging abnormalities in LNB.
Findings Correspond With Mylymedata
The symptoms and poor quality of life scores of the PTLDS patients in the JH study correspond with the of Phase 1 of the MyLymeData study. It collected data from 3,900 physician-diagnosed Lyme disease patients who were still ill.
When asked to name their worst symptoms, these MyLymeData participants most frequently reported neurological , fatigue , and musculoskeletal-associated symptoms .
A prior LymeDisease.org study confirmed what this JH study shows: chronic Lyme disease is associated with a worse quality of life than most other chronic illnesses, including congestive heart failure, diabetes, multiple sclerosis and arthritis.
Don’t Miss: How To Kill Lyme Disease Naturally
Get Tested And Treated Early
Studies acknowledge that up to 30% of patients go on to suffer further Lyme symptoms even after treatment, sometimes called Post-Treatment Lyme Disease Syndrome . One of the biggest risk factors for this condition is delayed treatment.
Research is finally, if slowly, catching up to the reality that letting Lyme disease slip through the cracks of insufficient diagnostic testing causes real suffering for patients. IGeneX is at the forefront of solving this problem, offering more sensitive and accurate testing for Lyme disease and other tick-borne diseases that can cause mental health problems when left untreated. Learn more today.
How Do You Treat Lyme & Tick
Access to proper tick bite treatment can often be hindered because there the medical community disagrees about how to identify those with Lyme Disease. Moreover, no perfect measures of identification exist. Lacking good measures for Lyme Disease, which has been readily accepted for decades, is compounded by lacking measures for the dozens of co-infections.
Diagnosis guidelines do not require positive blood work, yet many physicians erroneously use the CDC epidemiology study submission guidelines for diagnosis. Thus, patients are often forced to pay out of pocket for the best diagnostic tools available, which are through private lab companies.
Relying on incorrect guidelines means patients are told they must have 5 out of 10 bands to be diagnosed with Lyme. This creates a major barrier to quick and necessary tick bite treatment. Only clinical opinion after a physical exam is required to make a diagnosis of Lyme.
Recommended Reading: Medicine For Dogs With Lyme Disease
Acute Vs Chronic Lymedisease
There are some importantdifferences between acute and chronic Lyme disease. When infection occurs andthe bacteria enter the body, the immune system recognizes the microbes asharmful and begins fighting them. If the immune system is strong and robust,the initial symptoms may be very mild, and sometimes there wont be anysymptoms at all. This is why people often dont even realize theyve beeninfected.
In its early stages, Lymedisease is usually treated successfully with antibiotics. But if the infectionremains undiagnosed, the bacteria can go on living inside the cells withoutcausing any trouble for a long time. As they travel to other tissues andorgans, including the brain, they eventually disperse throughout the body. Theonly time symptoms might present is when the immune system weakens due toillness, extreme stress, or some other reason. This is when the bacteria startto flourish, causing a chronic infection.
Chronic Lyme disease occurswhen the entire microbiome is disrupted. After this has happened, the immune system continues todysfunction, which can lead to many different types of symptoms. This chronicphase can even last a lifetime.
Does Lyme Disease Affect The Brain And Nervous System
Lyme disease affects the nervous system. This statement is both accurate and terrifying since, for many of us, damage to the brain is the most feared consequence of disease. However, when it comes to Lyme disease, much of this fear is misplaced. Lyme disease can affect the lining of the brain, a disorder known as meningitis. Other than causing fever and bad headaches, this form of meningitis is remarkably benign nobody has ever died of it, and it has rarely if ever caused significant damage to any patients brain. On extremely rare occasions, the infection can involve the brain or spinal cord, disorders that are now extraordinarily rare. Other patients can develop inflammation of various nerves, e.g., the nerves that control the muscles on one side of the face this might occur in about 5% of untreated individuals. Other nerves can be affected, but even less frequently.
When considering these disorders, it is essential to recognize some key facts. First, the infection is highly responsive to antibiotics. Second, if the facial nerve has been severely damaged, there may be some residual weakness after treatment. However it is extraordinarily rare for there to be any permanent damage to the brain itself.
Don’t Miss: When Do Symptoms Of Lyme Disease Start
Insights On Neurological Lyme Disease
She rounds out her discussion of these issues by interviewing five professionals who know a lot about neurological Lyme disease. One is psychiatrist Robert Bransfield, MD, a top expert on how Lyme affects the brain . Another is Sandra Berenbaum, LCSW, with whom I co-authored the book When Your Child Has Lyme Disease: A Parents Survival Guide. Others are Leo Shea, Ph.D., who has extensive experience with neuropsychological testing of children and adults with Lyme disease health advocate/blogger Scott Forsgren, founder of BetterHealthGuy.com, who writes extensively on Lyme-related issues and Connie Strasheim, author of many books about Lyme disease. They all offer useful insights on the topic of Lyme disease brain.
Throughout the book, Ducharme offers practical information with a strong helping of optimism. As she writes early on:
I find that the majority of people with Lyme brain can find resolution or, at the very least, significant improvement of their symptoms.Im not saying its quick or easy, but I have seen remarkable improvements in people who started out very, very ill with horrible Lyme brain and are now back at work, running their families and living their lives as productive, happy people.
If you or a loved one has a problem with neurological Lyme disease symptoms, I think youll find this book both helpful and hopeful.
What Lyme Disease Does To Your Brain
is a bacterial infection that you catch when an infected deer tick bites you. The first symptoms can appear within a few days or weeks. They include a target-shaped , , fever, , , and . Often, doctors promptly recognize and treat Lyme disease with antibiotics. But when treatment is delayed, the infection can spread to other areas, including the nerves, liver and eyes. It can also spread to the central nervous systemthe brain and spinal cordand cause the following problems.
Don’t Miss: How To Check For Lyme Disease In Dogs
How Do You Diagnose Lyme & Tick
Lyme and tick-borne disease are complex diseases that produce physical, cognitive, and psychiatric symptoms that present differently in each patient. One person may experience severe joint pain, and another may have brain fog and anxiety. Yet, they both have a Tick-Borne illness.
Lyme Disease is a bacterial infection caused by a spiral-shaped bacteria, Borrelia burgdorferi . It is usually transmitted by the bite of an infected tick, but many also believe spiders and other biting insects can pass it on. Most people are shocked to learn that the bacteria can also be passed through the placenta of a pregnant woman to the fetus, which is referred to as congenital Lyme. Research from Schlesinger et al. denotes poor treatment outcomes for those with congenital Lyme.
Tick-borne disease symptoms may be acute, or they can wax and wane in a more long-term, chronic manner. Some symptoms appear immediately after a tick bite, but sometimes weeks, months or years pass before the disease presents making diagnosis and treatment even more complex. This waxing and waning of symptoms is confusing, leading to uncertainty regarding underlying cause. This makes one wonder if the tick bite or Lyme Disease one had months ago could be related to current symptoms.