Why Do People Get Chronic Lyme Disease
Lyme Disease has eluded doctors for many years. Those who are bitten by the infectious deer tick usually do not realize they have been bitten and do not show the telltale sign of the bullseye rash anywhere on there skin. In fact, only 1 in 5 Lyme sufferers ever exhibit such a symptom, yet it is often the only clear-cut sign that doctors can solely identify as being representative of Lyme. If and when a person is diagnosed with Lyme, mainstream medical practitioners will usually treat him or her with a two-to-three week course of antibiotics. Considering Lyme disease is a bacterial infection, the antibiotic treatment seems practical and in some cases, will rid the person of Lyme completely.
However, if the disease has gone untreated, the likelihood that one short course of antibiotics will kill the bacteria entirely is unlikely. Although symptoms may disappear for a short while, the remaining bacteria will eventually flourish once more and many who have been treated will relapse back into full-blown, chronic Lyme.
In an even more unfortunate circumstance, some Lyme sufferers are diagnosed far too late into their infection. With such vague and overlapping symptoms, Lyme is often misdiagnosed or mistreated, leaving the patient with chronic pain that only seem to worsen with time. Although the disease is fairly common, doctors frequently dismiss Lyme in lieu of other medical problems including depression, chronic fatigue, andin the most extreme caseshypochondria.
Lyme Disease Alters Immune Cell Communication
Recent research out of Johns Hopkins University indicates that Borrelia burgdorferi alters communication between two types of immune cells dendritic cells and T-cells. Dendritic cells are cells that process antigens, toxic or foreign substances that induce an immune response in the body. Examples of antigens include bacterial toxins and food proteins. After processing antigens, dendritic cells pass the antigens on to T-cells, which are specially trained cells that are able to target and destroy specific pathogens. Borrelia appears to interfere with the normal communication between dendritic cells and T-cells, causing the receptors on dendritic cells to change structurally and induce T-cells to attack healthy cells in your own body.
How To Properly Manage Lyme Disease Autoimmunity
Clearing Lyme disease and other chronic infections is essential for resolving autoimmunity when a chronic infection is the root cause of autoimmunity. A Lyme-literate doctor can guide you through Lyme treatment. However, while youre undergoing Lyme treatment, what can you do to resolve autoimmunity and improve your symptoms and health? Conventional medicine has a minimal repertoire of treatments for autoimmunity, namely broad-spectrum immunosuppressants that are toxic and can have widespread, long-term damaging effects. A functional medicine approach that includes strategic nutritional changes is a powerful and safer alternative to immunosuppressants for addressing autoimmunity during Lyme treatment. The autoimmune protocol diet is particularly effective for autoimmunity.
Don’t Miss: Dr Jay Davidson Lyme Disease
Symptoms Of Lyme Disease
Early symptoms of Lyme disease typically present as a circular red skin rash around a tick bite called Erythema migrans. This red, circular, or oval-shaped rash often expands over a period of days and can reach up to 12 inches across. Sometimes the center clears as it enlarges resulting in a bull’s-eye appearance. It’s typically not itchy or painful but may feel warm to the touch. Some people develop this rash at more than one place on their bodies. The rash can appear up to a month after you’ve been infected, but it usually occurs within one to two weeks and can last for several weeks.
Not everyone with Lyme disease gets the rash. You may also have flu-like symptoms in the first few weeks of infection, such as tiredness, muscle pain, headaches, high temperature , chills, swollen lymph nodes, and joint pain .
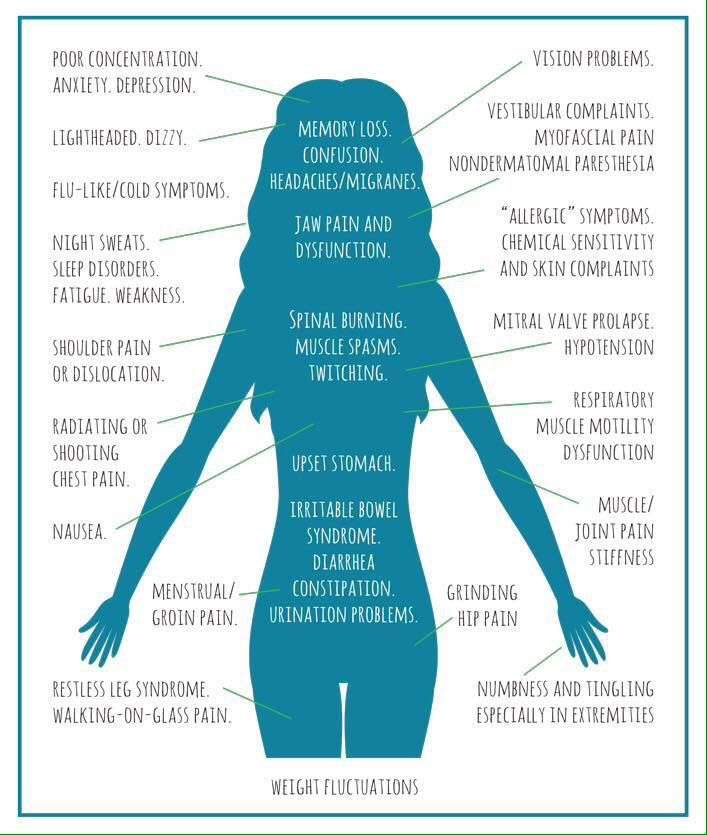
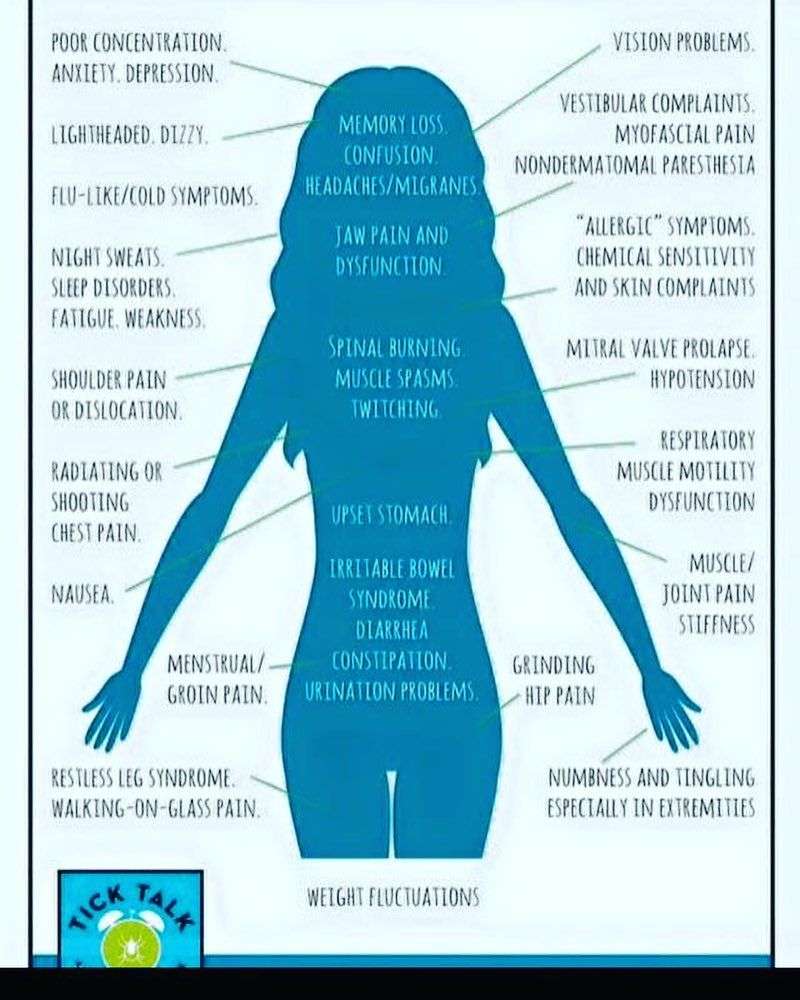
A few people with Lyme disease develop more serious symptoms weeks, months, or even years later. These include:
- Severe headaches and muscle pain
- Problems affecting the brain or nerves, such as memory problems, difficulty concentrating, and dizziness
- Pain in the joints and muscles often in the knees
- Heart problems such as heart palpitations, chest pain, and shortness of breath
- Inflammation of the membranes surrounding the brain and spinal cord
Disease signs and symptoms can appear quickly or gradually over time, and they are different for everyone.
Left untreated, Lyme disease may spread to your heart and nervous system.
Meet With An Autoimmune Or Lyme Disease Specialist
With any chronic condition such as Lyme disease, implementing effective & holistic treatments that will put you on the road to recovery is a top priority for all of us at LifeWorks Wellness Center.
We provide every patient with individualized, quality treatment. As one of Floridas top autoimmune disease clinics, our doctors understand what you are going through and can give you a proper diagnosis that will identify whether you are suffering from an autoimmune disease or even Lyme.
Recommended Reading: Lyme Disease In Dogs Prognosis
Autoimmune Disease And Lyme Disease
The incidence of PTLDS has increased over the years, and patients who have undergone antibiotic treatments are coming forward with symptoms they thought had disappeared long ago. Research has revealed that even long-term antibiotic treatment can leave some of the Lyme bacteria unscathed. When the bacteria is not completely eradicated, superficial symptoms can cascade into more serious, neurological conditions.
It is not surprising that chronic Lyme patients might also be afflicted with autoimmune diseases like multiple sclerosis or rheumatoid arthritis. What starts off as a disease bearing physical symptoms like sore joints and chest pain can transform into a chronic illness bearing symptoms of cognitive dysfunction, memory problems, chronic fatigue, and mood disorders.
Medical specialists believe the autoimmune response that triggers the aforementioned symptoms is a result of the residual damage that occurs during the initial infection. The outer coat of the Lyme bacteria is similar to tissue found in our nervous system, and it is believed that the immune system reacts to this leftover tissue, attacking it and mistakenly attacking neuronal tissue as well. Thus, the bacterial tissue that was not eliminated via antibiotics confuses the immune system. The onset of chronic symptoms thereafter are misattributed to other autoimmune diseases, and likewise, the autoimmune diseases may be a direct result of the Lyme infection itself.
Patients With No Lyme Disease
According to our clinical criteria, 44 patients did not have objective signs of Lyme disease at study entry. Based on clinical evaluation and chart and correspondence review, they did not have objective signs or symptoms either, at the time a presumable diagnosis of Lyme disease was made elsewhere. Thirty-two patients did not have IgG antibodies to B. burgdorferi at the time of study entry. However, 12 of these 44 patients did have IgG antibodies to B. burgdorferi.
Also Check: Lyme Disease Chain Of Infection
Lyme Disease Manifests As Autoimmune Disorder Sjgrens Syndrome
Lyme disease symptoms can mimic many other illnesses and have been linked to several autoimmune diseases including Sjögrens syndrome , Dermatomyositis , and Guillain-Barre syndrome . A case report by Smiyan entitled Sjögrens syndrome and lymphadenopathy unraveling the diagnosis of Lyme disease, reflects the importance of a thorough clinical evaluation.
A 43-year-old woman initially presented to an oncology clinic with symptoms of lymphadenopathy, a disease of the lymph nodes. She complained of low-grade fever, generalized swelling of lymph nodes, migrating aches in joints of arms and legs, dryness in mouth and eyes, weight loss, and fatigue for the past 6 months, writes Smiyan and colleagues. But clinicians were able to rule out lymphoma.
The patient, who also exhibited clinical signs of Sjögrens syndrome, an autoimmune disorder which impacts the glands that make tears and saliva, causing dry mouth and dry eyes, was then referred to a rheumatology clinic for evaluation.
The woman met the criteria for Sjögrens syndrome based on the following findings:
- Keratoconjunctivitis sicca
- Xerostomia
- Positive tests for antinuclear antibodies, anti-Ro , anti-La , anti-SS-A, and anti-SS-B IgG antibodies
- Negative tests for double-stranded DNA antibodies, anti-ribosomal P protein antibodies, anticentromere antibodies, Sm, Sm/RNP, RNP, Scl-70, and Jo-1 antibodies.
Related Articles:
References:
Other Tickborne Infections And Autoimmunity
Lyme disease is often not transmitted in isolation. The bite of a tick or another vector that transmits Lyme disease, such as biting flies, can transmit numerous other pathogens that can trigger autoimmunity. For example, Babesiosis, caused by the microscopic parasites Babesia microti and Babesia duncani, is also associated with autoimmunity, including positive ANA .
You May Like: Western Blot Test For Lyme Disease
What Causes Autoimmune Diseases
Most experts agree that autoimmune diseases are caused by environmental triggers. Common examples include foods , toxins , and viral or bacterial infections.
Indeed, there is growing evidence that Lyme disease and other bacterial infections can trigger autoimmune diseases, especially in patients who are genetically predisposed to them. Studies have documented several cases of Lyme disease that appeared to trigger or mimic autoimmune diseases, including Sjogrens syndrome, dermatomyocitis , rheumatoid arthritis , psoriatic arthritis , and spondyloarthritis .
What If A Tick Bites My Dog
The more ticks in your region, the likelier it is that your furry pal will bring them home.
Your dog is much more likely to be bitten by a tick than you are. And where Lyme disease is common, up to 25% of dogs have had it at some point.
About 10% of dogs with Lyme disease will get sick. 7-21 days after a tick bite, your dog might seem like theyâre walking on eggshells. They also might have a fever and enlarged lymph nodes. Plus, they might seem tired. Dogs also get antibiotics for Lyme.
What if my dog brings ticks into my home?
Use a tick control product on your pet to prevent Lyme disease. Also, have your dog vaccinated against Lyme.
Check your dogâs whole body each day for bumps. If you notice a swollen area, see if thereâs a tick there. If you find a tick, wear gloves while you use tweezers to separate it from your dog. Then, put it in soapy water or alcohol, or flush it down the toilet.
Use alcohol to clean the spot on your dog where the tick was attached. Keep an eye on that spot, and also on your dog to make sure theyâre behaving normally. If you notice any changes, check with your vet.
Show Sources
John Aucott, MD, assistant professor of medicine, Johns Hopkins University School of Medicine director, Johns Hopkins Lyme Disease Clinical Research Center.
CDC.
Morbidity and Mortality Weekly Report: âVital Signs: Trends in Reported Vectorborne Disease Cases — United States and Territories, 2004-2016.â
American College of Rheumatology.
Read Also: Tick Bite Test For Lyme Disease
What Is Chronic Lyme Disease
Lyme disease is an infection caused by the bacterium Borrelia burgdorferi. In the majority of cases, it is successfully treated with oral antibiotics. In some patients, symptoms, such as fatigue, pain and joint and muscle aches, persist even after treatment, a condition termed Post Treatment Lyme Disease Syndrome .
The term chronic Lyme disease has been used to describe people with different illnesses. While the term is sometimes used to describe illness in patients with Lyme disease, it has also been used to describe symptoms in people who have no clinical or diagnostic evidence of a current or past infection with B. burgdorferi . Because of the confusion in how the term CLD is employed, and the lack of a clearly defined clinical definition, many experts in this field do not support its use.
Autoimmune Disease And Lyme: The Connection
Research into autoimmune disease and Lyme have made a startling discovery. The long-term treatment with antibiotics only eradicates all the bacteria in a certain percentage of those affected. In others, where remnants of the bacteria persist, their initial symptoms could progress and result in damaging neurological health issues. Furthermore, many of these people develop various autoimmune conditions, including the likes of rheumatoid arthritis and multiple sclerosis. They could also end up suffering from conditions closely related to adrenal fatigue. These include, amongst others, memory issues, chronic fatigue, a decline in cognitive function, and even various mood disorders.
Your body’s autoimmune response to the bacteria may result from damage encountered while initially infected. The bacteria’s outer coat is similar to that of your nervous system tissue. Your immune cells that were reacting to the bacteria could end up attacking your own nervous system tissue. Essentially, the residual bacteria tissue causes an immune system response. This results in the many irregular diagnoses surrounding Lyme disease and the autoimmune disorders that develop because of this bacterial infection. So, autoimmune disease and Lyme has a definite connection.
Recommended Reading: Arthritis Caused By Lyme Disease
Lyme Infections Triggers Il
The Lyme disease autoimmune response appears to be mediated by an immune signaling molecule called IL-17. Early infection with Borrelia burgdorferi, the bacterium responsible for classic Lyme disease, triggers the production of interleukin-17 , a pro-inflammatory cytokine that regulates the immune response. IL-17 is helpful in the early stages of infection for defending the body against infection. However, chronic Lyme disease may lead to excessive production of IL-17 at high levels, IL-17 can trigger autoimmunity.
The Experience Of Lyme Disease
In our book, Conquering Lyme Disease: Science Bridges the Great Divide, we review several of the key features of Lyme disease that can make the experience of this illness so challenging, including:
- The politically charged climate
- The protean nature of manifestations of the illness
- The waxing and waning course of symptoms
- The psychological ramifications of having an “invisible” chronic illness and the experience of invalidation
- The challenge of having a disease that affects the brain and sensory system
- The impact of uncertainty surrounding diagnosis, treatment, and prognosis
Recommended Reading: Natural Remedies To Cure Lyme Disease
Lyme And Autoimmune Disease
When pathogenic infections invade tissues, the bacteria produce LPS which are found on their outer cell membrane and promote inflammation. These molecules are produced and fool the hosts immune system into thinking that there is a foreign invader. The body natural mounts an immune response, but the response is against its own tissue, yielding autoimmune disease.
Frequently we see autoimmune diseases associated with Lyme Disease and coinfections such as: MS, Lupus, Hashimotos Thyroiditis, Scleroderma, Graves Disease, Celiac Disease, etcEssentially, any tissue in the body can fall prey to autoimmune disease if the autoimmunity is driven by infection.
In 18 years of practice, most of my patients autoimmune conditions are completely erradicated with proper longterm antibiotic use as well as targeted nutraceuticals. If you decrease the infection in the tissue, the concentration of LPS decreases, inflammation decreases, and tissues can return to their healthy state. If infection is allowed to persist, autoimmune disease simply gets worse.
It is my belief that most if not all autoimmune disease is infection driven. The challenge becomes to identify the exact pathogen and then treat accordingly.
MOUNT VERNON LOCATION:
Chronic Lyme Disease Vs Post
Patients typically use the term chronic Lyme disease to describe the cluster of symptoms that started after getting Lyme disease and that persist despite having received a course of antibiotic treatment which has been deemed curative by the Infectious Diseases Society of America. Patients say, “I’m not cured. I have symptoms now that I never had before Lyme disease. I’m fatigued 90% of the day. My muscles ache. My brain is in a fog. I can’t think clearly any more. I’m super sensitive to light and sound. What is going on? Chronic Lyme disease does exist – I’m a living example of it!”
Whatever one calls it, the experience is the same. Most often these patients experience profound fatigue, pain, and/or cognitive impairment. Mild to moderate levels of depression and anxiety may also accompany these symptoms, as the functional limitations can lead to social isolation, inability to work, and loss of sense of one’s identity as a provider, caretaker, or friend. Sometimes patients find themselves identifying with Job – the just and good man in the Bible whose life was wrecked by illness, death of loved ones, and economic disaster he felt tormented by God.
Don’t Miss: Cbd Oil For Lyme Disease
Has Niaid Looked At The Potential Benefits Of Long
Yes. NIAID has funded three placebo-controlled clinical trials on the efficacy of prolonged antibiotic therapy for treating PTLDS. The published results were subjected to rigorous statistical, editorial, and scientific peer review.
These trials were designed to ensure that several key parameters were addressed:
- The susceptibility of B.burgdorferi to the antibiotics used
- The ability of the antibiotics to both cross the blood-brain barrier and access the central nervous system and to persist at effective levels throughout the course of therapy
- The ability of the antibiotics to kill bacteria living both outside and inside mammalian cells
- The safety and welfare of patients enrolled in the trials
The first clinical trial, which included two multicenter studies, provided no evidence that extended antibiotic treatment is beneficial. In those studies, physicians examined long-term antibiotic therapy in patients with a well-documented history of previous Lyme disease but who reported persistent pain, fatigue, impaired cognitive function, or unexplained numbness. Those symptoms are common among people reporting PTLDS. Patients were treated with 30 days of an intravenous antibiotic followed by 60 days of an oral antibiotic.
In 2016, a clinical trial conducted in the Netherlands also concluded that in patients with persistent symptoms attributed to Lyme disease, longer term treatment with antibiotics did not provide additional benefits compared with shorter term regimens.
Lyme Disease And Autoimmune Conditions
A Lyme disease infection is known to cause a weak immune system. To understand how this happens, the researchers isolated dendritic cells from healthy study participants and exposed them to Borrelia burgdorferi, finding that the bacterial infection causes receptor sites on the surface of dendritic cells, known as HLA-DRs, to mature and become active. Normally, these HLA-DRs cells would present antigens to killer T-cells, the immune system agents that remove invaders from the body.
The researchers believe that when the HLA-DRs interact with Borrelia burgdorferi, they are structurally changed and keep the dendritic cells from marking the bacterial proteins as foreign, which leads to the dendritic cells attracting T-cells, but instead of attacking the Lyme disease bacteria, instead attacks the healthy cells.
Senior author Mark Soloski, PhD, co-director for basic research at the centre, and professor of medicine at the Johns Hopkins University School of Medicine, said: We believe these observations are relevant not only to how Borrelia burgdorferi disrupts the immune system but other infections as well. Antibodies that react with a persons own tissues or organs have been reported in patients with infections, including COVID-19.
Read Also: Lyme Disease Specialist Raleigh Nc