Lyme Is Not The Only Threat
As mentioned earlier in this article, there is another group of borrelia that causes a disease that is similar to, but biologically distinct from, Lyme. This disease, called Tick-Borne Relapsing Fever or TBRF, is often characterized by fevers that wax and wane every few days. However, many patients never experience relapsing fevers or any fevers at all. Like those of Lyme and other tick-borne diseases, TBRF symptoms can often go undetected or be mistaken for other conditions, which can give the disease time to develop into neurological symptoms.
So, as with Lyme, it is crucial to get an early and accurate diagnosis of TBRF. Be aware that TBRF will not show up on a Lyme test the test must be designed to test for TBRF borrelia in order to show accurate results. If symptoms are Lyme-like but test results are negative, doctors should consider the possibility of TBRF.
What Is Neurologic Lyme Disease
Neurologic symptoms of Lyme disease occur when the Lyme disease bacteria affect the peripheral or central nervous systems.
- Cranial nerve involvement: When the cranial nerves are affected, facial palsy can occur on one or both sides of the face.
- Peripheral nerve involvement: When the peripheral nerves are affected, patients can develop radiculoneuropathy which can cause numbness, tingling, shooting pain, or weakness in the arms or legs.
- Central nervous system involvement: When the central nervous system is affected, Lyme meningitis can cause fever, headache, sensitivity to light, and stiff neck.
Out of every 100 patients whose cases are reported to CDC, 9 have facial palsy, 4 have radiculopathy, and 3 have meningitis or encephalitis. Because of reporting practices, this statistic may overestimate how often these manifestations are seen by clinicians.
What Are Neurologic Manifestations Of Lyme Disease
Neurologic involvement, also known as Lyme neuroborreliosis, is reported in 5-20% of cases. In the United States, cranial neuropathy is the most common manifestation of early neurologic Lyme disease. Other manifestations include meningitis and encephalopathy.
Cranial neuropathies, especially facial nerve palsy , develop in approximately 3% of Lyme disease patients. In endemic areas, Lyme disease is the most commonly identified cause of acquired facial palsy, especially in children. Headache, absence of previous herpetic lesions, and meningeal symptoms are noted in most pediatric Lyme disease patients with facial palsy.
When meningitis is involved, symptoms usually occur 2-10 weeks following infection. Headache, neck pain or stiffness, and photophobia typically indicate meningeal irritation. The headache of Lyme disease typically is described as waxing and waning, and the severity varies from mild to severe, even in patients with frank meningitis. Persistent headache alone is a rare presentation of Lyme disease but should be considered in patients in endemic areas during summertime.
Borrelia encephalopathy most commonly manifests as a mild confusional state accompanied by disturbances in memory, concentration, mood, sleep, personality, and/or language occurring months to years after the infection. Depression and irritability are also common.
References
Feder HM Jr. Lyme disease in children. Infect Dis Clin North Am. 2008 Jun. 22:315-26, vii. .
You May Like: When To Treat Lyme Disease
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040″ rel=”nofollow”> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Understanding Symptoms Of Neurological Lyme
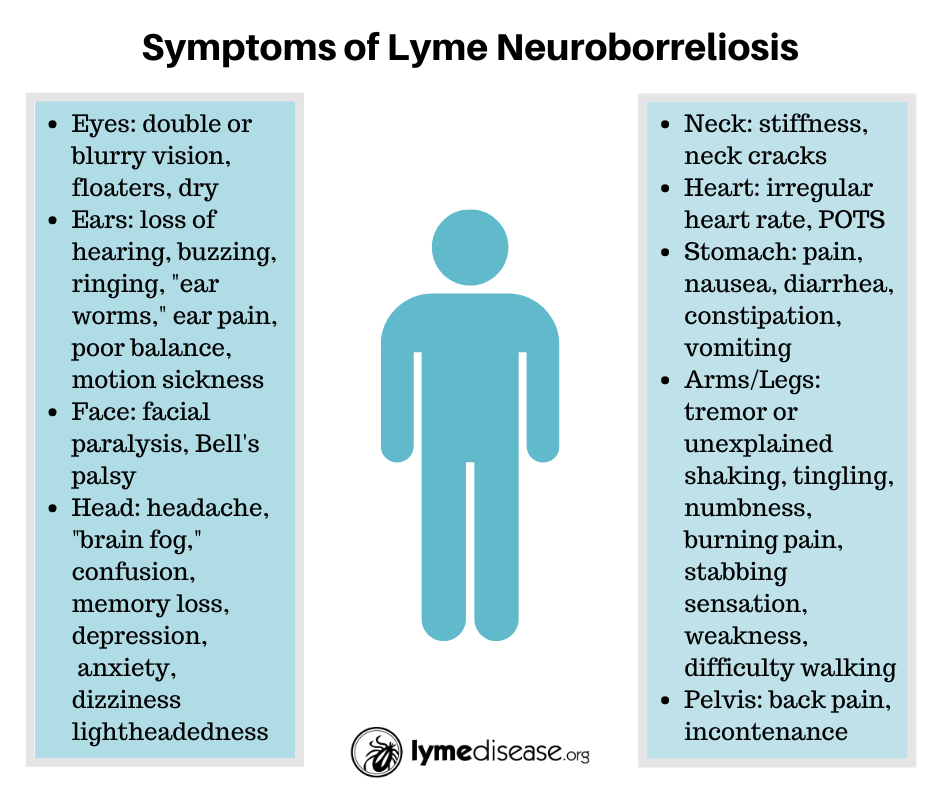
Lyme neuroborreliosis is thought to occur in about 15% of Lyme disease cases but a definite percentage is impossible to pin down. Everyone with Lyme disease experiences some neurological symptoms, but a specific composit of symptoms that constitute neurological Lyme is not well defined. Making matters worse, the Centers for Disease Control , does not recognize LNB as a separate entity, and it doesnt acknowledge the existence of a chronic form of Lyme disease.
The most common initial symptom is neurogenic pain that starts in the back and radiates down the legs. With that comes weakness, numbness, and tingling in the lower extremities.
Another common presenting symptom of LNB is facial nerve palsy , which is characterized by temporary paralysis on one side of the face. Some people also experience sound sensitivity and discomfort in the ear on the paralyzed side, and if youre unable to close that eye, dry eye can occur. Most people recover fully from Bells palsy, with improvement in the first few weeks and continuing for three to six months, but a minority of people have symptoms for life.
Symptoms of LNB are thought to occur from infiltration of white blood cells immune cells like lymphocytes and plasmocytes into the white matter of the brain and the spinal cord, otherwise known as the central nervous system . This is associated with an increase in inflammatory immune messengers, called cytokines, in cerebrospinal fluid.
Recommended Reading: International Lyme And Associated Diseases Society
Treating Lyme Neuroborreliosis In Children
Recommendations for treating children and adults
-
Antibiotic treatment should be carried out in the case of Lyme neuroborreliosis with inflammatory cerebrospinal fluid syndrome .
-
In the case of a possible Lyme neuroborreliosis , antibiotic treatment may be considered after a thorough differential diagnosis and if there is no evidence of another disease.
-
Antibiotic treatment should take place over a period of 14 days or 1421 days .
-
Reference is made to the S2k Guideline Cutaneous Lyme Borreliosis for the treatment of polyneuropathy associated with acrodermatitis chronica atrophicans .
-
If a distally symmetrical polyneuropathy is suspected as a manifestation of Lyme neuroborreliosis without accompanying ACA , the same procedure recommended for possible Lyme neuroborreliosis can be used.
-
Cerebral vasculitis resulting from Lyme borreliosis should be treated with antibiotics in accordance with the recommendations for late Lyme neuroborreliosis.
-
Analogous to the recommendations for cerebral vasculitis of another aetiology , the additional administration of steroids and/or 100 mg/d of ASS can be considered for cerebral vasculitis resulting from Lyme borreliosis.
-
In addition to antibiotic treatment, symptoms should also be treated .
Recommendation for choosing antibiotics for children and adults
Recommendations for monitoring the treatment of children and adults
Reports From The Literature
The literature search by using stringent diagnostic criteria disclosed only seven additional patients with dementia as a leading symptom of definitive LNB. These cases were reported in detail, so they can serve for the description of characteristic features. The data of all 10 patients are summarized in Table and .
Read Also: Are Lyme Disease Tests Reliable
Pots Constipation And Lyme Disease
POTS stands for postural orthostatic tachycardia syndrome which means the heart rate will increase when someone changes position, from laying or sitting to standing. POTS is very common in late-stage Lyme disease since the autonomic nervous system does not maintain tone in blood vessels causing a drop in blood pressure. When the blood pressure drops, the heart rate has to increase to stabilize blood pressure. Mast cell activation syndrome is another common cause of POTS and MCAS is frequently seen as a consequence of Lyme disease.
Another common symptom associated with autonomic nervous system dysfunction is constipation. Termed gastroparesis, constipation can happen when the nerve that signals intestinal muscular contraction become damaged by the bacteria and the resulting immune response.
Lyme Disease Effects On The Brain
The first section of Lyme Brain discusses the fundamentals. What actually causes this condition? Research has shown that Lyme spirochetes can invade the brain and wreak all kinds of havoc. They damage nerve cells, trigger inflammation, release neurotoxins, and disrupt the balance of brain chemicals.
Ducharme lays all this out in plain language. She also explains how co-infections contribute to Lyme disease brain:
One of the reasons I believe that the actual brain fog, memory issues and difficulty with focus and concentration is Borrelia driven is because when I treat my patients with medications that primarily impact Borrelia and cross the blood-brain barrier, I see these symptoms improve, whereas the insomnia and wacky dreams tend to respond more to Babesia treatment. Really extreme psychiatric symptoms such as rages, and suicidal thoughts and behaviors, respond mostly to Bartonella treatment.
Don’t Miss: How To Determine If You Have Lyme Disease
Treatment Of Chronic Lyme Disease
Damage to the peripheral and autonomic nervous system is common in late-stage Lyme disease. Numbness, tingling, burning and nerve pain experienced in peripheral neuropathy and radiculitis require effective treatment of the involved infections. Therapies directed at decreasing the inflammatory response by the immune system and repair of the damaged nerves is also part of the strategy when treating symptoms associated with chronic neurological Lyme disease.
Neuropathy is one of the most debilitating and challenging to treat symptoms of chronic neurological Lyme disease. Intravenous immunoglobulin therapy can be useful at reversing any form of neuropathy including CIDP caused by Lyme disease. The biggest hurdle in using IVIG as a therapy is the expense , so insurance coverage of this therapy is typically necessary. Often, criteria for health insurance approval is a positive nerve conduction study and a biopsy demonstrating small fiber neuropathy. Treatments are usually once per month, and it can take 6-18 months to see results.
Other therapies can also be helpful in treating the untoward neurological effects of Lyme disease. Work with a Lyme-literate doctor to determine the most effective therapies for the infection and subsequent immune-mediated inflammatory response that is causing your symptoms.
The Effects Of Lyme Disease On The Nervous System
A limping dancer, a student forced to the bench.
According to Dr. Erik Kolbenheyer, an internist, gastroenterologist, family doctor, occupational health specialist, doctor of traditional Chinese medicine, there are some particularly interesting cases of Lyme borreliosis, where the disease causes bizarre symptoms in the nervous system. The doctor, who, being personally affected by the disease, turns to his patients with excellent diagnostic sense and great empathy, presents two shocking cases from his own practice when young people became ill but fortunately, their quality of life essentially returned to its previous level.
In cases where the bacteria attack the nervous system, anxiety, depression, panic attacks, and strange movement disorders may appear. It is a very complex set of symptoms, so in these cases, the help of a neurologist is needed to examine the patient in other directions. As the symptoms of the nervous system can take on quite unusual forms, patients and relatives might panic.
You May Like: Where Can I Get Lyme Disease Test
Neurological Lyme Disease: What You Need To Know
Lyme disease can manifest in a seemingly endless number of ways. While the spectrum of symptoms is similar for most sufferers, the worst of the bunch varies from person to person. And for those who have a predominance of neurological symptoms, the disease can feel especially debilitating and difficult to overcome.
Thats in large part because neurological Lyme also referred to as Lyme neuroborreliosis is often confused with other serious neurological conditions such as multiple sclerosis and Parkinsons Disease, which can be scary and overwhelming. And because most doctors lack an understanding of Lyme disease in general, and especially of Lyme associated with a predominance of neurological symptoms, LNB often goes unrecognized.
So how to know if the symptoms youre experiencing do signify LNB, and where do you go from there to find relief? Keep reading for information that could provide the turning point in your recovery.
Treatment For The Neurological Complications Of Lyme Disease

Review question
Are antibiotics effective for the treatment of Lyme disease affecting the nervous system?
Background
In humans, a bacterium called Borrelia burgdorferi causes Lyme disease. People become infected when bitten by ticks carrying the bacterium. The person may experience symptoms in the joints, skin, muscles, and nervous system , the brain, and the spinal cord). Without antibiotic treatment, neurological Lyme disease either may resolve or cause long-term problems. Neurological Lyme disease differs between Europe and the United States, probably because of differences in B. burgdorferi. Limited information exists about which antibiotics are better for the treatment of neurological Lyme disease.
Study characteristics
Key results and quality of the evidence
The seven studies were too different for their results to be combined, so we analyzed them individually.
None of the studies provided clear evidence that one antibiotic was better than another. One study failed to find evidence that a second and longer treatment with an oral antibiotic offered any extra benefit following initial intravenous treatment with ceftriaxone. As none of the other studies used a dummy treatment , the extra benefit offered by antibiotic treatment over recovery that occurs naturally is unknown. In general, the treatment was tolerated well, although the quality of adverse event reporting in most studies appeared to be low.
The evidence is current to October 2016.
You May Like: Arizona Lyme Disease Treatment Center
What Is Lyme Disease
Lyme disease is a severe condition that can disguise itself as several other health problems. Some of the symptoms include:
- muscle aches and pain
- migraines
- rashes
If it is diagnosed early on, the symptoms can be treated with antibiotics. Still, if Lyme is left untreated, it can lead to long-lasting chronic symptoms, including nerve damage.
Neurological Symptoms Of Early Lyme Disease
The onset of neurological symptoms can occur between one week and two months following a tick bite. In this early stage of neurological involvement, common symptoms have emerged. Meningitis from the Borrelia bacteria will present with nausea/vomiting, mild to severe headaches and a stiff neck. Light sensitivity and fever may also occur. However, meningitis caused by Lyme disease may be less severe than other bacterial infections so may be misdiagnosed as viral meningitis.
Encephalitis, or inflammation of the brain, can cause confusion, sleepiness, mood swings, personality changes or hallucinations. When the cranial nerves are affected in early Lyme disease, facial nerve palsy can cause muscle weakness or paralysis on one or both sides of the face leading to facial drooping. Additional cranial nerve symptoms include difficulty with eye closure, moving lips and smiling, and wrinkling of the forehead. Vision and smell can also be affected by cranial nerve inflammation.
Don’t Miss: What Are The Symptoms Of Lyme Disease From A Tick
Treatment For Neurological Lyme Disease
After defining the problem, she moves on to solutions. The next section deals with pharmaceutical approaches to Lyme disease in the brain, including an explanation of the blood-brain barrier and what drugs can effectively penetrate it. She discusses medications that reduce inflammation, as well as those to stabilize neurological function, balance mood and help people think more clearly.
Section 3 discusses natural approaches to Lyme disease in the brain: antimicrobials, such as Cats Claw and teasel root anti-inflammatories, such as curcumin and stephania root antioxidants, such as glutathione neurotransmitter support and essential oils such as peppermint and frankincense.
Section 4 deals with nutrition. Readers of her earlier book, The Lyme Diet, will find familiar themes: avoid gluten, dairy, sugar, caffeine, alcohol and additives such as MSG.
Ducharme explains about therapies to help the brain, including neurofeedback, Brainwave Entrainment, and hyperbaric oxygen. She covers sleep and exercise. She reviews different kinds of psychotherapy for patients with Lyme brain.
Indirect Pathogen Detection In Serum
3.3.1 Serodiagnosis, antibody detection
In the case of early Lyme borreliosis, Borrelia-specific IgM antibodies can be detected starting week 3 p.i. and IgG antibodies starting week 6 p.i. . However, the use of VlsE or C6 peptide as a test antigen means that IgG antibodies can now often be detected as early as IgM antibodies . High IgG antibody concentrations are usually found in late manifestations of Lyme borreliosis ) , . A detectable humoral immune response does not always follow the usual course known from other infectious diseases: the measurable antibody response may be absent in an early, localised manifestation . At the same time, there may be no measurable IgM response, for example in the case of reinfections , . In the context of very early antibiotic treatment, a measurable humoral immune reaction may also fail to appear . On the other hand, the positive detection of borrelia-specific IgM and/or IgG antibodies alone is not an indication of an illness from Borrelia burgdorferi since
Antibody detection and test sensitivity based on disease stage
Borrelia infections with asymptomatic seroconversion can occur and
elevated IgG and IgM antibody titres are not uncommon in healthy individuals for years following sufficiently treated Lyme borreliosis , , .
Borrelia serology is not suitable for monitoring antibiotic treatment of Lyme borreliosis and follow-up testing is therefore not recommended , .
3.3.2 Diagnostically relevant Borrelia antigens
Early immune response
Read Also: Herbs To Cure Lyme Disease
The 3 Obstacles To Neurological Lyme Disease Treatment
Chronic Lyme disease is often associated with neurological symptoms that are both debilitating and increasingly difficult to treat. At Envita we understand Lyme disease better than anyone and we are familiar with the struggle patients experiencing neurological Lyme symptoms face. There are three major areas of conflict that patients with neurological Lyme symptoms battle.
Envita Medical Centers doesn’t make any guarantee of outcomes. Results are not typical and will vary from person to person and should not be expected.
Neurological Manifestations In Adults
Garin-Bujadoux-Bannwarth syndrome is the most common manifestation of acute Lyme borreliosis in adults in Europe after erythema migrans , , .
In Europe, isolated meningitis is mainly observed in children , , , , .
The symptoms of radiculitis develop on average 46 weeks after the tick bite or after the erythema migrans , . Segmental pain occurs first, which intensifies at night and whose localisation can change. Often the pain is initially localised in the extremity where the tick bite or erythema migrans was first observed , . The patient experiences pain that is burning, nagging, stabbing or tearing in nature and responds only slightly to conventional analgesics. It often peaks within a few hours or days. Three-quarters of patients develop neurological deficits after 14 weeks, and pareses are more frequent than sensory disorders , .
About 60% of patients with Bannwarths syndrome have cranial nerve deficits.
Involvement of the central nervous system is rare and occurs in only around 4% of Lyme neuroborreliosis cases , . Its onset is gradual and it is frequently chronic. The most common manifestation is myelitis with spastic atactic gait disturbance and bladder dysfunction , . Symptoms can develop over days or several months. Some patients suffer from severe tetra- or paraparesis. Approximately 60% of patients with myelitis have additional signs of encephalitis and around 40% have cranial nerve involvement. Encephalitis has no clinical properties specific to the pathogen.
Recommended Reading: Dr Thomas Moorcroft Lyme Disease