Lyme Disease Joint Pain And Arthritis
Lyme disease and joint pain unfortunately go hand in hand, as Lyme-related arthritis is commonly found in Lyme disease sufferers. If you have Lyme arthritis, you have swollen, painful joints that cause stiffness and pain. It is found in people who are in the late stages of Lyme disease. According to an article in Science Daily, approximately 60 percent of patients with untreated Lyme disease will develop related arthritis.
Lyme arthritis is caused by the bacteria that causes Lyme disease getting into your joints and causing inflammation of your tissues. Over time, this can cause damage to your cartilage. Most cases of Lyme arthritis are short-lasting and affect only one large joint.
Lyme arthritis can affect your:
- Knees
- Elbows
- Shoulders
In the U.S., its estimated that about 60 percent of untreated Lyme disease patients will experience intermittent episodes of swelling and lyme disease joint pain for months to years after they are infected by a tick bite.
Thankfully, most Lyme arthritis cases can be treated with antibiotics and NSAIDs, although some people may require surgery to remove some diseased tissue. Around ten percent of untreated patients may go on to develop chronic arthritis, reports Johns Hopkins Arthritis Center.
Can Lyme Disease Be Prevented
To prevent Lyme disease, you should lower your risk of getting a tick bite:
- Avoid areas where ticks live, such as grassy, brushy, or wooded areas. If you are hiking, walk in the center of the trail to avoid brush and grass.
- Use an insect repellent with DEET
- Treat your clothing and gear with a repellant containing 0.5% permethrin
- Wear light-colored protective clothing, so you can easily see any ticks that get on you
- Wear a long-sleeve shirt and long pants. Also tuck your shirt into your pants and your pant legs into your socks.
- Check yourself, your children, and your pets daily for ticks. Carefully remove any ticks you find.
- Take a shower and wash and dry your clothes at high temperatures after being outdoors
Centers for Disease Control and Prevention
How Should A Tick Be Removed
Grasp the mouthparts with tweezers as close as possible to the attachment site. Be careful not to squeeze, crush or puncture the body of the tick, which may contain infectious fluids. Pull firmly and steadily upward to remove the tick. After removing the tick, thoroughly disinfect the bite site and wash hands. The NYSDOH has created a video on proper tick removal and a printable card with steps on how to remove ticks . See or call a doctor if there are concerns about incomplete tick removal. Do not attempt to remove ticks by using petroleum jelly, lit cigarettes or other home remedies because these may actually increase the chance of contracting a tick-borne disease.
Read Also: Main Symptoms Of Lyme Disease
Phylogenetic Diversity And Human Disease Taxonomy And Disease
B. burgdorferi was thought to be the sole genospecies in the United States until 1995 when Marconi and associates isolated B. andersonii from cottontail rabbits and I. dentatus ticks. Subsequently, it became evident that enzootic cycles exist involving non-sensu stricto species and specialist ixodid ticks with strong, selective host preferences and little or no proclivity to bite humans. Perhaps the best characterized of these is B. bissettii , transmitted by I. pacificus, I. affinis and I. spinipalpis and recovered and/or detected by PCR throughout the United States in ticks and a variety of vertebrates and, in rare instances, humans . Molecular evidence for infection of humans by B. americana and B. andersonii, particularly in Southern states, also has been reported . Moreover, B. mayonii was recently isolated from a few human specimens in upper midwestern U.S. . However, in the United States, B. burgdorferi remains the primary agent of disease.
Lyme Disease In Humans
1Department of Medicine, UConn Health, Farmington, CT 06030, USA
2Department of Pediatrics, UConn Health, Farmington, CT 06030, USA
3Departments of Genetics and Genome Sciences, UConn Health, Farmington, CT 06030, USA
4Departments of Molecular Biology and Biophysics, UConn Health, Farmington, CT 06030, USA
5Department of Immunology, UConn Health, Farmington, CT 06030, USA
Don’t Miss: What Are The Early Signs Of Lyme Disease
What Tests Are Used To Diagnose B Mayonii
Your healthcare provider may order a blood test to look for infection. Limited available information suggests that patients with B. mayonii infection develop antibodies that are similar to those of patients infected with B. burgdorferi. Therefore, Lyme disease serologic testing may help in diagnosing patients with B. mayonii. In some cases, B. mayonii bacteria may also be seen on a blood smear. Infection with B. mayonii can be specifically identified by Lyme disease molecular tests at Mayo Clinic. Lyme disease, including infection with B. mayonii, can be diagnosed without testing when patients have signs and symptoms consistent with Lyme disease and a history of possible exposure to blacklegged ticks.
Treatment For Neurological Lyme Disease
After defining the problem, she moves on to solutions. The next section deals with pharmaceutical approaches to Lyme disease in the brain, including an explanation of the blood-brain barrier and what drugs can effectively penetrate it. She discusses medications that reduce inflammation, as well as those to stabilize neurological function, balance mood and help people think more clearly.
Section 3 discusses natural approaches to Lyme disease in the brain: antimicrobials, such as Cats Claw and teasel root anti-inflammatories, such as curcumin and stephania root antioxidants, such as glutathione neurotransmitter support and essential oils such as peppermint and frankincense.
Section 4 deals with nutrition. Readers of her earlier book, The Lyme Diet, will find familiar themes: avoid gluten, dairy, sugar, caffeine, alcohol and additives such as MSG.
Ducharme explains about therapies to help the brain, including neurofeedback, Brainwave Entrainment, and hyperbaric oxygen. She covers sleep and exercise. She reviews different kinds of psychotherapy for patients with Lyme brain.
Also Check: Do You Get A Rash With Lyme Disease
What Can I Expect Long Term If My Child Has Lyme Disease
If Lyme disease is caught and treated early, most children will make a full recovery. Some children with Lyme disease go on to experience whats called a post-infectious syndrome with symptoms that may include feeling fatigue, joint aches and pains, headaches, difficulty sleeping, and problems concentrating. Since the infection itself is gone by this time, doctors generally dont prescribe antibiotics. Each child is different, but its not uncommon for symptoms of post-infectious syndrome to linger for months, or even years, and they can be made worse by stress or other illness. But most children do make a full recovery.
Blacklegged, or deer, ticks are very small, so it helps to know what to look for when doing a tick check. Adults are about the size of sesame seeds and in the nymph or larva stage, they can be as tiny as a poppy seeds.
Differential Gene Expression Tick Transmission And Back Again
Because animals syringe-inoculated with in vitro-cultivated organisms develop manifestations indistinguishable from animals inoculated with ticks , the arthropod phases of the bacterial life cycle might be considered irrelevant to pathogenesis. However, in the real world, Lyme disease spirochetes are transmitted by ticks and, therefore, the tick-mammal interface must be regarded as the starting point for the infectious process . Indeed, there is now overwhelming evidence that spirochetes in feeding ticks undergo complex alterations in their transcriptional and protein profiles that are not reproduced by in vitro culture conditions . Collectively, these changes enable the spirochete to adapt physiologically to the feeding midgut environment , while, at the same time, preparing it for challenges looming during the mammalian phase . They also promote binding to the bacterial surface of serum proteins that exploit mammalian proteolytic systems to facilitate dissemination from tick to mammal and protect against complement-mediated lysis . The obligatory time course for this programmatic sequence explains why spirochetes are infrequently transmitted to mice or humans when ticks are attached for less than 48 h. It is critical for physicians to be aware of this time frame because it establishes the window of opportunity for antimicrobial prophylaxis and can be used to provide re-assurance to individuals who removed recently attached ticks that their risk of infection is low.
Read Also: Are Lyme Disease Tests Accurate
Is Lyme Disease Curable
The tick-borne illness can be treated with antibiotics, and most people make a full recovery within weeks or months. So why is there so much confusion?
In much of the country, spring and summer mean warmer weather and spending more time outdoors. Unfortunately, it also means that the ticks that carry Lyme disease bacteria may be out in full force, especially in wooded or grassy areas.
About 30,000 cases of Lyme disease are reported each year to the U.S. Centers for Disease Control and Prevention, although experts estimate that 10 times that amount may actually be infected. Thats concerning, because if left untreated, Lyme disease can cause nerve damage, memory loss, dangerous inflammation around the heart, and other permanent health problems.
But the good news is that Lyme disease is also very treatableespecially when its diagnosed soon after symptoms begin. Lyme disease is always curable, Daniel Kuritzkes, MD, chief of the Division of Infectious Diseases at Brigham and Womens Hospital in Boston, tells Health. The medications we have are very effective at getting rid of the infection. Heres what else you need to know.
RELATED: How Do You Get Lyme Disease?
Which Organs Can Lyme Disease Damage
Although Lyme can cause damage to allorgans in the body, the most notable organs are the brain and heart. When itattacks the brain and central nervous system, patients can suffer cognitiveimpairment such as memory loss, poor concentration, problems with sleep, andvarious mood changes. The disease does this by crossing the blood-brain barrier and multiplying and inhibiting the proper function and transferof blood and oxygen to where it needs to be.
Lyme carditis is the disorder that occurswhen the bacteria that causes Lyme makes its way into the heart tissue. When itdoes, it wreaks havoc on the communication system and electrical signals fromthe upper and lower chambers of the heart, resulting in light-headedness,fainting, heart palpitations, and an abnormal heartbeat.
Because the cells of the bacteria thatcause Lyme disease are able to disguise themselves under a biofilm, the immunesystems ability to properly attack the actual infection is threatened. Thiscauses the released immune cells to attack the body instead of the bacteria.Lyme disease bacteria cells also have a way of hiding in plain sight, meaningthat if theres too much of a threat to their existence, they can lay dormantuntil theyre able to flourish again. This leads to the illness becomingchronic and harder to treat in the long run, which aids in the bacterias waron the body and all organs.
Featured image byRobina Weermeijer on Unsplash
Read Also: Best Herbal Treatment For Lyme Disease
Stage : Early Localised Lyme Disease
The symptoms for this stage normally begin within a few days to weeks after infection from the tick bite. In some cases of Lyme disease, you may not notice signs of infection during this stage.
The bacteria begin to multiply in the bloodstream, with the first sign being that of a red, circular rash. It might look a lot like a bulls eye.
This rash will develop at the site of the tick bite. It is not painful or itchy, just warm to touch. It is known as erythema migrans and will most likely disappear within four weeks.
With or without the rash, you may develop flu-like symptoms. These can include:
- A loss of energy
- Vision changes
Stage : Quickly Expanding Rash
After being bitten by a black-legged tick, a quickly growing rash can appear. This is the earliest stage of Lyme disease, known as stage 1.
Most people who develop a rash, get it within days or weeks of being bitten by a tick.
Where you see the rash: If you develop a rash, it appears near the tick bit you. For most people, that means the back, groin, armpit, or a lower leg. However, a tick can bite you anywhere.
What the rash can look like: You may see a spot or bump on the skin, which is the bite mark. Around or near the bite mark, a rash develops. Some people see the bulls-eye rash . You can also have one of the other rashes shown here.
Early rash caused by Lyme disease
Notice the bite mark in the center of this early rash, which will expand quickly.
Bulls-eye rash on womans upper arm
This is another early sign of Lyme disease.
Lyme disease rash with lighter color on the outside
This rash has expanded, but you can still see the bite mark in the center.
Rash from Lyme disease has begun to clear
As the rash begins to clear, the redness fades.
If you develop a rash during this stage, you may notice that it:
-
Feels smooth and warm to the touch
-
Causes a burning sensation
-
Itches or feels painful
-
Has an outer edge that feels scaly or crusty
When the rash and symptoms begin: According to the Centers for Disease Control and Prevention , the rash begins 3 to 30 days after the tick bites you.
About 50% of people who have Lyme disease develop flu-like symptoms , which include:
Don’t Miss: How Is Lyme Disease Caused
Hematogenous Dissemination And Organ System Invasion
Little is known about the mechanisms by which circulating spirochetes recognize and invade target organs. Studies with cultured human umbilical vein endothelial cells have shown that organisms rapidly attach to vascular endothelium and negotiate their way through intercellular junctions , subsequently attaching to subendothelial matrix components . Real-time intravital confocal microscopy revealed that transmigration through capillaries and post-capillary venules in vivo is a multi-step process engaged in by only a small percentage of GFP-expressing spirochetes introduced intravenously into mice . The role of the adhesin BBK32 in trans-endothelial migration was described above.
How Is The Lyme Multiplex Assay Different From The Assay My Veterinarian Can Perform
Your veterinarian can perform a quick assay in-house that checks for antibodies against only one B. burgdorferi surface protein. The in-house assay cannot detect early infection, cannot determine vaccination status, and does not quantify the amount of antibodies your animal is producing. Quantifying antibodies is an important measure for successful treatment and to confirm cure from Lyme disease.
Read Also: How Long Does A Lyme Blood Test Take
What Type Of Illness Does B Mayonii Cause
Based on limited information, illness caused by B. mayonii appears similar to that caused by B. burgdorferi, but with a few differences. Like B. burgdorferi, B. mayonii causes fever, headache, rash, and neck pain in the days after infection and can cause arthritis after a few weeks of illness. Unlike B. burgdorferi, B. mayonii can also cause nausea and vomiting large, widespread rashes and a higher concentration of bacteria in the blood.
Does Treatment Immediately After A Tick Bite Negate Signs Of Early Infection
Not every tick carries B. burgdorferi. The infection rate of ticks also varies with geographic region. Therefore, treatment should not be performed based on a tick bite alone. If the tick was found on the animal it can be sent in for B. burgdorferi PCR. PCR for Anaplasma can be performed simultaneously if requested. If the tick was infected, early treatment can be considered. However, a tick must feed for at least 24 hours on an animal or human for B. burgdorferi transmission to occur. Only a serological test will confirm whether transmission of B. burgdorferi occurred and the animal was infected. Antibodies can be detected in infected animals as early as 3-4 weeks after infection. Lyme Multiplex testing is recommended after that time. Treatment can be initiated immediately afterwards if antibody levels are positive. Treatment during this early infection phase is generally very effective.
Recommended Reading: How To Get A Tick Checked For Lyme Disease
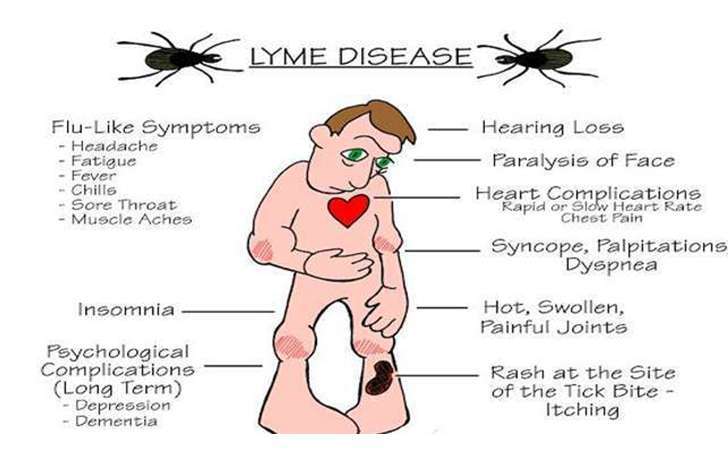
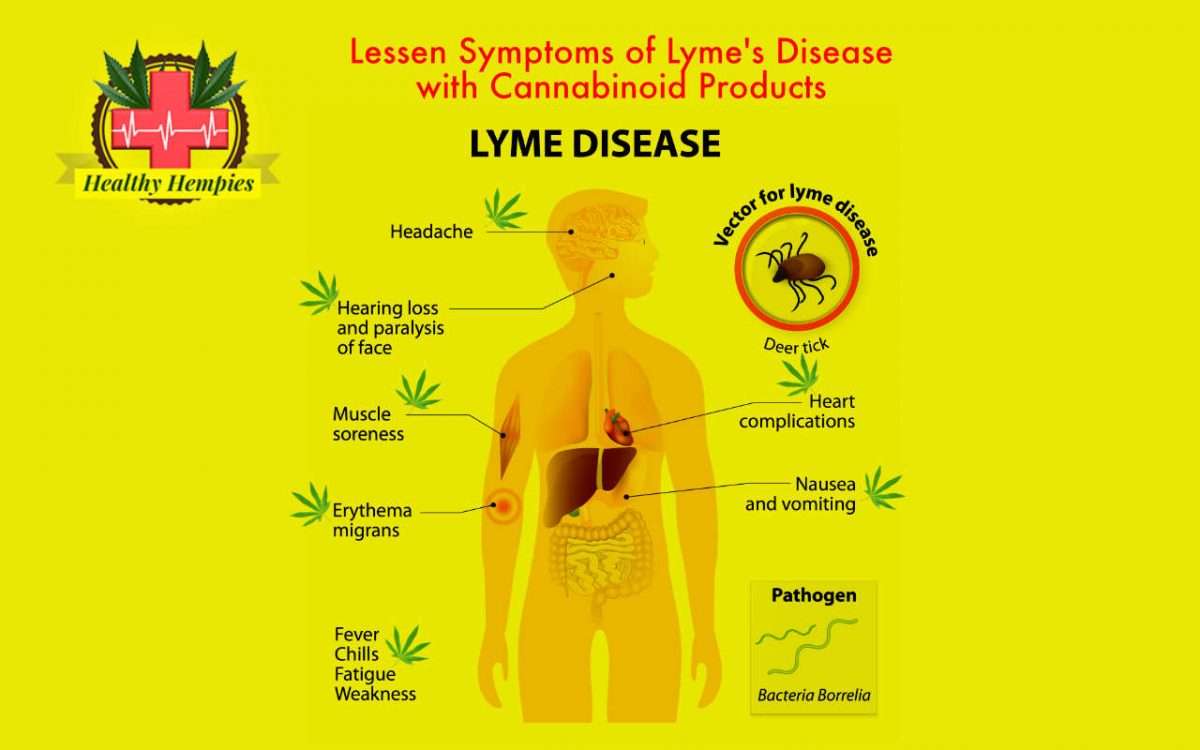
What Are The Symptoms Of Lyme Disease In Humans Center
Lyme disease is an infection that is transmitted by ticks and is the most common vector-borne disease in the US. It is caused by infection with the spiral-shaped bacteria Borrelia burgdorferi or Borrelia mayonii that resides in the stomach of the ticks. The infected ticks of the genus Ixodes, commonly called black-legged deer ticks, transmit this disease to humans via tick bites. Read more: What Are the Symptoms of Lyme Disease in Humans? Article
Also Check: Does Lyme Disease Cause High Blood Pressure
What Are The Treatments For Lyme Disease
Lyme disease is treated with antibiotics. The earlier you are treated, the better it gives you the best chance of fully recovering quickly.
After treatment, some patients may still have pain, fatigue, or difficulty thinking that lasts more than 6 months. This is called post-treatment Lyme disease syndrome . Researchers dont know why some people have PTLDS. There is no proven treatment for PTLDS long-term antibiotics have not been shown to help. However, there are ways to help with the symptoms of PTLDS. If you have been treated for Lyme disease and still feel unwell, contact your health care provider about how to manage your symptoms. Most people do get better with time. But it can take several months before you feel all better.
Don’t Miss: Antibiotics Used For Lyme Disease
Who’s At Risk And Where Are Ticks Found
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
Ticks are found throughout the UK and in other parts of Europe and North America. There are a high number of ticks in the Scottish Highlands.
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.