Treating Neurologic Lyme Disease
Facial palsy is treated with oral antibiotics and Lyme meningitis can either be treated with oral or intravenous antibiotics, depending on severity. Most people experiencing the early onset of Lyme disease respond well to antibiotic therapy and fully recover. If you dont seek immediate treatment, there are varying degrees of permanent nervous system damage that may develop in late-stage Lyme disease.
To add to that, they will notice a slow degradation of the body functions leading to arthritis, heart problems, and neurological problems affecting the brain and the nervous system. Patients can experience persistent pain, fatigue, or cognitive disability that lasts as long as 6 months, sometimes even years.
Neurologic Lyme disease requires a specific intravenous antibiotic protocol to rid the bacteria from your central nervous system and brain tissue.
Get Tested And Treated Early
Studies acknowledge that up to 30% of patients go on to suffer further Lyme symptoms even after treatment, sometimes called Post-Treatment Lyme Disease Syndrome . One of the biggest risk factors for this condition is delayed treatment.
Research is finally, if slowly, catching up to the reality that letting Lyme disease slip through the cracks of insufficient diagnostic testing causes real suffering for patients. IGeneX is at the forefront of solving this problem, offering more sensitive and accurate testing for Lyme disease and other tick-borne diseases that can cause mental health problems when left untreated. Learn more today.
Neurological Infections In Travelers/immigrants
Many infectious diseases that affect the nervous system can be acquired from other parts of the United States or other parts of the world. In the United States, several regional viruses and fungi can cause encephalitis and/or meningitis that individuals coming from endemic regions may have been exposed to. Worldwide, neurocysticercosis, poliomyelitis, malaria, schistosomiasis, rabies, chikungunya virus, dengue fever, leptospirosis, Tick-Borne encephalitis virus, cycloviruses, and melioidosis are some of the infections that can be acquired which affect the nervous system.
Also Check: How To Check For Lyme Disease
How Lyme Disease Affects The Brain
Lyme disease has profoundeffects on the brain in about 15% of patients. According to some sources, thispercentage may even be higher, since thousands of cases are likely to remainundiagnosed every year.
Neuroborreliosis is the name for the neurological disorder caused by Lyme disease. The symptoms of neuroborreliosis include memory impairment, attention deficit, sleep disturbances, cranial nerve abnormalities, dyslexia, decreased verbal fluency, and sensitivity to light. In some cases, depression, anxiety, panic attacks, mood swings, hallucinations, and progressive dementia may also occur. In children, the most common symptoms of neuroborreliosis are headaches, behavioral changes, learning difficulties, and sleep disorders.
A small number of patientsexperience neurological symptoms after early antibiotic treatment for Lymedisease. This phenomenon is referred to as post-treatment Lyme diseasesyndrome and is probably caused by a widespread inflammation of the brain.
Why And How Lyme Disease And Tbrf Affect Mental Health
Lyme disease and TBRF can wreak havoc on a patients mental health in the following ways:
- Direct effects As with syphilis, the bacteria that causes Lyme disease and TBRF can invade the central nervous system and cause neurological and psychiatric symptoms that are organic in origin. This is what doctors call neurological Lyme disease or Lyme neuroborreliosis.
- Indirect effects The discomforts and challenges of living with and/or being treated for Lyme disease or TBRF can lead to anxiety, depression, and other mental health conditions that are not necessarily caused by the bacteria, but are indirectly caused or exacerbated .
Of course, these effects are not either/or, but rather can coexist and compound one another. Learn more about each below.
Read Also: Lyme Disease Blood Test Cost
What Neurocognitive & Neuropsychiatric Conditions Result From Lyme & Tick
Neurocognitive and Neuropsychiatric tick-borne disease symptoms can emerge either early or late in the disseminated phase of infection. In untreated Lyme Disease, the encephalopathy can be moderate to severe, and can wreak havoc on an individuals life. Unfortunately, the average person sees 5 to 7 doctors before they are correctly diagnosed . Lyme Connection: Leir Center Presentation).In one common scenario, an individual is certain they have Lyme and go to their physician.
The doctor then tells them they dont have it or dont meet the clinical criteria. Unless one takes control of their own medical care or sees a Lyme specialist, they may find themselves thinking they just have a psychiatric issue without a medical source. Individuals often go down this road only to find that they dont get much relief this way either.
Bransfield and Weintraub note there are hundreds of peer-reviewed articles address a causal association between Lyme Disease and mental symptoms. Fallon and Neilds note that 40% of patients with Lyme Disease develop neurologic involvement of either peripheral or central nervous system. The range of neurocognitive, neuropsychiatric and physical symptoms is wide.
Nested Pcr Provides Sensitive Detection For Borrelia Sp Dna
To determine the presence of Borrelia burgdorferi, we first investigated the presence of DNA in the brain samples. To this end, nested PCR was adapted to increase the sensitivity and specificity of the assay . DNA isolated from frontal cortex of an uninfected non-human primate was used as a negative control and as a positive control, DNA isolated from NHP frontal cortex tissue that was incubated with B. burgdorferi spirochetes was used . To prevent cross-contamination between positive control and autopsy specimens, DNA from autopsy tissue samples was isolated in laboratories that were never exposed to B. burgdorferi DNA.
Don’t Miss: What Is The Best Way To Treat Lyme Disease
Relationship Of Ptlds And Chronic Lyme Disease To B Burgdorferi Infection
The key questions concerning these 2 entities are whether they truly exist, and if they do, what might the underlying mechanism be? With regard to the existence of PTLDS, 30% or more of patients treated for Lyme disease may report persisting, subjective posttreatment symptoms. However, several controlled trials have shown that identical symptoms are equally common in patients without Lyme disease . The few studies suggesting relatively more frequent subjective symptoms following treated Lyme disease show no increase in corroborating objective abnormalities . Studies of the general population indicate that up to a third of the normal, healthy population experiences the same symptoms to a varying degree , the same frequency as that found in the control populations of Lyme disease posttreatment studies. In the absence of any objective evidence of disease in these treated patients, and given that the identical symptoms are equally prevalent in control individuals, it seems plausible that the entity PTLDS is simply an example of anchoring bias. Patients who have been treated successfully for Lyme disease and subsequently experience common symptoms that they have heard are attributable to PTLDS incorrectly conclude that these nonspecific symptoms are indeed the sequelae of B. burgdorferi infection, perpetuating the notion of this construct.
The Case Study Pathology Is Characteristic Of Dementia With Lewy Bodies
The fresh brain weighed 996 g and appeared atrophic Coronal sections through the left cerebral hemisphere and brain stem revealed mild enlargement of the lateral ventricle, particularly the temporal horn. The substantia nigra was normally pigmented or nearly so. Microscopically, nigral and cortical Lewy bodies, were seen with hematoxylin and eosin stain . Immunohistochemistry for -synuclein showed numerous immunoreactive Lewy bodies and fibers in substantia nigra, hippocampal formation and neocortex, Figures 4CE). IHC for hyperphosphorylated tau revealed intense staining of many limbic neurofibrillary tangles and neuropil threads , and of occasional neurofibrillary tangles in neocortex, but senile plaques were extremely rare, and each contained only a few fibrils . H& E showed prominent thickening of small blood vessels in gray and white matter, extensive mineralization of pallidal vessels, and rare microglial nodules in the hippocampal formation. Immunohistochemistry for Iba-1 , CD68 , and CD163 showed moderate numbers of activated microglia and large numbers of macrophages in hippocampal formation and spinal cord . In summary, we see DLB accompanied by features of Alzheimer’s disease, a common presentation.
You May Like: Getting A Tick Tested For Lyme Disease
Visualizing Brain Fog In Post
More than one in 10 people successfully treated with antibiotics for Lyme disease go on to develop chronic, sometimes debilitating and poorly understood symptoms of fatigue and brain fog that may last for years after their initial infection has cleared up.
Now, a Johns Hopkins team has used an advanced form of brain scan to show that 12 people with documented post-treatment Lyme disease syndrome all show elevation of a chemical marker of widespread brain inflammation, compared with 19 healthy controls.
Results of the study, published in Journal of Neuroinflammation, suggest new avenues for treating the long-term fatigue, pain, sleep disruption and brain fog associated with PTLDS. Theres been literature suggesting that patients with PTLDS have some chronic inflammation somewhere, but until now we werent able to safely probe the brain itself to verify it, says Jennifer Coughlin, a senior author and associate professor of psychiatry and behavioral sciences.
What this study does is provide evidence that the brain fog in patients with post-treatment Lyme disease syndrome has a physiological basis and isnt just psychosomatic or related to depression or anxiety, says John Aucott, director of the Johns Hopkins Lyme Disease Research Center.
In addition, the results suggest that drugs designed to curb neuroinflammation may be able to treat PTLDS, although clinical trials are needed first to determine the safety and benefit of such therapy, Aucott says.
What To Do If You Have A Blacklegged Tick Bite
Remove the tick by pulling it directly out with fine-tipped tweezers. Lift upward with slow and even pressure. Dont twist when removing it. Dont crush it or put soap or other substances on it. Dont apply heat to it.
Place the tick in a resealable container. See if you can identify what kind of a tick it is.
Immediately after removing the tick, wash your skin well with soap and water or with rubbing alcohol.
Not all ticks carry Lyme. The Lyme bacteria is transmitted only by blacklegged ticks in their nymph or adult stage.
Save the tick to show your doctor. The doctor will want to determine if its a blacklegged tick and if theres evidence of feeding. Ticks enlarge as they feed. Your risk of getting Lyme from an infected tick increases with the length of time that the tick fed on your blood.
Summary:
Pull the tick out with tweezers and save it in a resealable container for identification.
Recommended Reading: Arizona Lyme Disease Treatment Center
Are There Other Kinds Of Tick
Yes. While most people automatically think about Lyme Disease, they need to remember ticks carry multiple infections at the same time.
One common infectious disease that ticks carry is Babesia, a parasite that infects red blood cells and presents like malaria. It is difficult to detect, and symptoms can be mild. For example the, most common physical symptom is sweating. Babesia can lead to serious illness and when present with a co-infection, it can increase the severity of Lyme disease. Babesia is well known to be associated with neurocognitive and neuropsychiatric symptoms.
One teen patient experienced a sudden onset of anxiety for several years. The anxiety was so severe she she was unable to leave her home. Although she had all the telltale signs of tick-borne infection, specifically Babesia. Although other doctors missed this, in our first session I identified her as having Tick-Borne Disease
The QEEG brain map clearly showed the illness that the long list of physicians, psychiatrists, and psychologists three year period had missed. That led to never being treated properly., She could then be referred to a Lyme physician for proper treatment. Sadly, this teen had a clear-cut case of Lyme Disease and Tick-Borne Disease, but was never identified early and treated with antibiotics. This is an all too familiar story that leads to a case of Late-Disseminated Lyme, and more importantly, a lot of suffering and heartache.
‘lyme Rage’: Can Lyme Disease Affect Your Personality
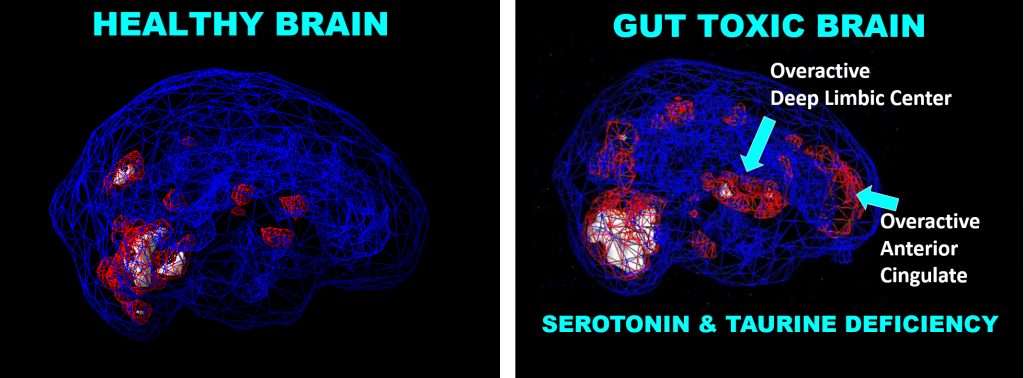
Roaming ticks can carry disease linked to mental problems, some believe.
July 30, 2009 — They’re tiny insects that can cause big problems. A rise in the number of ticks this year has infectious disease experts focused on the best way to treat the Lyme disease that the little buggers can spread.
Some 20,000 Americans are infected and treated every year, but countless others go undiagnosed. The illness has symptoms that include fever, fatigue and headaches, but if left untreated, Lyme disease can be more serious.
While there are physical symptoms of the disease that can include severe headaches, severe joint pain and even numbness in the hands or feet, many experts believe Lyme disease can rewire the human brain and affect personality.
“I’m convinced that Lyme in a chronic form can affect psychiatric issues, neurological issues and you can have neurological problems,” New York epidemiologist Dr. Daniel Cameron said.
The Center for Disease Control and Prevention notes that up to 5 percent of patients “may develop chronic neurological complaints months to years after infection.”
Lyme disease patient Kelly Kulesz told “Good Morning America” she saw herself change overnight because of her infection.
“They put me on stage fright medications,” Kulesz said. “Doctors thought it was obsessive compulsive disorder, but it’s just not.”
But not all experts believe Lyme disease causes such .
You May Like: Do Deer Get Lyme Disease
Signs And Symptoms Of Lyme Disease
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
Overview
Lyme disease is an underreported, under-researched, and often debilitating disease transmitted by spirochete bacteria. The spiral-shaped bacteria, Borrelia burgdorferi, are transmitted by blacklegged deer ticks. Lymes wide range of symptoms mimic those of many other ailments, making it difficult to diagnose .
The blacklegged ticks can also transmit other disease-causing bacteria, viruses, and parasites. These are known as coinfections . These ticks that transmit Lyme are increasing their geographical spread. As of 2016, they were found in about half the counties in 43 of 50 states in the United States .
Lyme is the fifth most reported of notifiable diseases in the United States, with an estimated 329,000 new cases found annually . Some studies estimate that there are as many as 1 million cases of Lyme in the United States every year .
Most people with Lyme who are treated right away with three weeks of antibiotics have a good prognosis.
But if youre not treated for weeks, months, or even years after infection, Lyme becomes more difficult to treat. Within days of the bite, the bacteria can move to your central nervous system, muscles and joints, eyes, and heart .
Here is a list of 13 common signs and symptoms of Lyme disease.
Why Choose Hope Brain & Body Recovery Center For Treatment
When seeking treatment for neurological conditions, you shouldnt settle for anything but the most premium treatment. Dr. Joseph Schneider has over 30 years of clinical experience and has attended to over 11,000 patients with a wide array of neurological conditions.
Dr. Schneider has firsthand experience with neurological treatment, having suffered a stroke in 2017. Thanks to his incredibly talented associates and personal knowledge of treatment methods, has made a miraculous recovery. He has devoted his life to the neurological health of his patients and uses his firsthand experience of the recovery process to improve the treatment methods used at Hope Brain & Body Recovery Center.
Choosing Hope Brain & Body Recovery Center gives you access to some of the most modern technical treatment equipment available. We utilize a wide range of modern diagnostic equipment that helps our specialists build some of the most comprehensive neurological profiles for our patients. This means we are able to offer more accurate diagnoses, discover underlying conditions, as well as use the information to create therapy plans that are uniquely designed for each patient.
Read Also: What Can I Give My Dog For Lyme Disease
Insights On Neurological Lyme Disease
She rounds out her discussion of these issues by interviewing five professionals who know a lot about neurological Lyme disease. One is psychiatrist Robert Bransfield, MD, a top expert on how Lyme affects the brain . Another is Sandra Berenbaum, LCSW, with whom I co-authored the book When Your Child Has Lyme Disease: A Parents Survival Guide. Others are Leo Shea, Ph.D., who has extensive experience with neuropsychological testing of children and adults with Lyme disease health advocate/blogger Scott Forsgren, founder of BetterHealthGuy.com, who writes extensively on Lyme-related issues and Connie Strasheim, author of many books about Lyme disease. They all offer useful insights on the topic of Lyme disease brain.
Throughout the book, Ducharme offers practical information with a strong helping of optimism. As she writes early on:
I find that the majority of people with Lyme brain can find resolution or, at the very least, significant improvement of their symptoms.Im not saying its quick or easy, but I have seen remarkable improvements in people who started out very, very ill with horrible Lyme brain and are now back at work, running their families and living their lives as productive, happy people.
If you or a loved one has a problem with neurological Lyme disease symptoms, I think youll find this book both helpful and hopeful.
The Role Of Coinfections
Ticks carry more diseases than just Lyme and TBRF, and its not uncommon for patients to be infected with more than one type of disease-causing bacteria.
Common coinfections such as Babesiosis and Bartonellosis can not only cause neurological and psychiatric symptoms of their own, but they can also complicate the diagnostic process, delaying proper diagnosis and treatment all of which increase the risk of developing emotional, behavioral, or cognitive problems from the infection.
Recommended Reading: Lyme Disease Symptoms Mayo Clinic
How Do You Diagnose Lyme & Tick
Lyme and tick-borne disease are complex diseases that produce physical, cognitive, and psychiatric symptoms that present differently in each patient. One person may experience severe joint pain, and another may have brain fog and anxiety. Yet, they both have a Tick-Borne illness.
Lyme Disease is a bacterial infection caused by a spiral-shaped bacteria, Borrelia burgdorferi . It is usually transmitted by the bite of an infected tick, but many also believe spiders and other biting insects can pass it on. Most people are shocked to learn that the bacteria can also be passed through the placenta of a pregnant woman to the fetus, which is referred to as congenital Lyme. Research from Schlesinger et al. denotes poor treatment outcomes for those with congenital Lyme.
Tick-borne disease symptoms may be acute, or they can wax and wane in a more long-term, chronic manner. Some symptoms appear immediately after a tick bite, but sometimes weeks, months or years pass before the disease presents making diagnosis and treatment even more complex. This waxing and waning of symptoms is confusing, leading to uncertainty regarding underlying cause. This makes one wonder if the tick bite or Lyme Disease one had months ago could be related to current symptoms.