Are There Any Risks To Lyme Disease Tests
There is very little risk to having a blood test or a lumbar puncture. If you had a blood test, you may have slight pain or bruising at the spot where the needle was put in, but most symptoms go away quickly. If you had a lumbar puncture, you may have pain or tenderness in your back where the needle was inserted. You may also get a headache after the procedure.
Access To Lyme Disease Testing Services
This guidance on the laboratory diagnosis of Lyme disease is intended for healthcare professionals in the UK. Patients concerned about possible Lyme infection should consult an appropriate healthcare professional, for example their GP, in the first instance.
Health professionals wishing to discuss a possible case or ascertain local arrangements for testing should contact a local Infection specialist .
NHS testing for Lyme disease is available through local service providers and the Rare and Imported Pathogens Laboratory at PHE Porton where ISO15189 accredited confirmatory testing is also provided. RIPL is also introducing a testing service for neurological Lyme disease.
RIPL provides medical and laboratory specialist services to the NHS and other healthcare providers, covering advice and diagnosis of a wide range of unusual bacterial and viral infections, including Lyme disease.
RIPL continuously updates its methods and will make further information on Lyme disease diagnostic testing available as it arises.
Where Lyme Disease Occurs
In the United States, Lyme disease typically occurs in the Northeast, Mid-Atlantic, and North Central states. It has also been reported to occur in Northern California. The most prevalent strain causing Lyme Disease in the United States is Borrelia burgdorferi.
If you live or have traveled to a state where Lyme disease is endemic, this increases your risk. Lyme disease is endemic in the following states: California, Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, Washington DC, West Virginia, and Wisconsin. For regulatory reasons, Everlywell is not able to offer testing in New Jersey, New York, or Rhode Island.
You May Like: What Are The Signs Of Lyme Disease In A Dog
How We Chose The Best At
When evaluating the companies for the best at-home Lyme disease tests, we looked at several key factors in order to provide you with the best information. For one, accuracy was extremely important, so we looked at testing centers with the best reviews and certifications. Every test mentioned in this article has been evaluated and awarded for their laboratory accuracy when dealing with their at-home tests.
Since Lyme disease is so severe and a misdiagnosis can have awful repercussions, we also considered how others reviewed the at-home tests.
Is There A Blood Test For Lyme Disease
If your doctor suspects that you have Lyme disease, they may order two blood tests. These will look for signs that your body is trying to fight it off. The results are most precise a few weeks after youâve been infected.
These tests are:
ELISA test. This test canât check for the bacteria that causes Lyme disease. It can only look for your immune systemâs response to it.
Once Borrelia burgdorferi gets into your blood, your body begins to make special proteins called antibodies to fight it off. The ELISA test checks for those antibodies.
Although itâs the most common way to check for Lyme disease, the ELISA test isnât perfect. It can sometimes give false âpositiveâ results. On the other hand, if you have it done too soon after youâve been infected, your body may not have developed enough antibodies for the test to detect them. This will give you a ânegativeâ result even though you do have Lyme disease.
Western blot test. Whether your ELISA test comes back positive or negative, your doctor will need to do this blood test, too.
A Western blot uses electricity to split certain proteins in your blood into patterns. This is then compared to the pattern of people known to have Lyme disease.
At least five band matches means that you have Lyme disease. Still, not all labs have the same standards. Thereâs a chance that you could get a âpositiveâ result from one and a ânegativeâ result from another.
- Alzheimerâs disease
Also Check: How To Know If I Have Lyme Disease
What If Your Lyme Disease Test Is Positive
Its important to note that a positive result doesnt mean you have a diagnosis of Lyme disease. The tests will show that antibodies are present in your blood, but a physician will need to order another type of test before you get an official diagnosis.
If someone gets a positive at-home test, definitely see your doctor, says Dr. Puja Uppal, a board certified family medicine physician and the chief medical officer at Think Healthy.
A physician will likely order both an enzyme-linked immunosorbent assay and a Western blot test, which check for antibodies specific to Borrelia burgdorferi. They will consider the results of both these tests, along with your symptoms, to make an accurate diagnosis.
Does The Time Of Year Matter In The Diagnosis Of Lyme Disease
Since Lyme disease is a tick-borne infection, the seasonality of the disease is linked tightly to the life cycle and behavior of ticks. May, June, July, and early August are the biggest risk months for acquiring first stage Lyme disease in the US. This is the feeding time for nymph and adolescent ticks which are difficult to see. A viral-like illness in those early summer months might be Lyme disease. There is also some transmission of Lyme disease via adult ticks in the fall and winter and throughout the year anytime the temperature is above 40 degrees, but to a lesser degree.
The risk of acute Lyme disease is more of a year-round risk in more temperate regions such as northern California and the pacific northwest. Later stage Lyme disease, however, can manifest at any time.
Read Also: How To Fight Lyme Disease
What Abnormal Results Mean
A positive ELISA result is abnormal. This means antibodies were seen in your blood sample. But, this does not confirm a diagnosis of Lyme disease. A positive ELISA result must be followed up with a Western blot test. Only a positive Western blot test can confirm the diagnosis of Lyme disease.
For many people, the ELISA test remains positive, even after they have been treated for Lyme disease and no longer have symptoms.
A positive ELISA test may also occur with certain diseases not related to Lyme disease, such as rheumatoid arthritis.
Who Should Not Be Tested
The American College of Physicians recommends against testing in patients:
-
Presenting with nonspecific symptoms without objective signs of Lyme disease
-
With low pretest probability of infection based on epidemiologic exposures and clinical features
-
Living in Lyme-endemic areas with no history of tick exposure
-
Presenting less than 1 week after tick exposure
-
Seeking a test of cure for treated Lyme disease.
Read Also: Dogs And Lyme Disease Treatment
Can I Be Assured That The Type Of Lyme Disease Testing Carried Out In Ireland Is Accurate
Yes. Irish laboratories operate to a very high standard of quality. Laboratories in Ireland follow the testing guidelines of the US Centres for Disease Control and prevention , Infectious Disease Society of America , European Federation of Neurological Societies and British Infection Association . These guidelines provide information on which of the currently available laboratory tests have enough evidence to accurately diagnose Lyme disease.
It is important that patients who are concerned about Lyme disease seek help and receive a firm diagnosis in Ireland to ensure continued medical care. It is important to ensure that your symptoms and lab results are considered together to make sure your diagnosis is as correct as possible.
Unexplained Pain And Other Sensations
Some people with Lyme may have sharp rib and chest pains that send them to the emergency room, suspecting a heart problem 00090-7/abstract%20″ rel=”nofollow”> 27).
When no problem is found, after the usual testing, the ER diagnosis is noted as an unidentified musculoskeletal cause.
You can also have strange sensations like skin tingling or crawling, or numbness or itchiness 00090-7/abstract%20″ rel=”nofollow”> 27).
Other symptoms have to do with cranial nerves.
- Ear-ringing . Tinnitus can be a nuisance, especially at bedtime when it seems to get louder as youre trying to fall asleep. About 10 percent of people with Lyme experience this (
- Hearing loss. One study reported that 15 percent of Lyme patients experienced loss of hearing .
- Jaw pain or toothaches that are not related to actual tooth decay or infection.
Summary:
Don’t Miss: What Symptoms Does Lyme Disease Cause
What Does An At
Once ordered, an at-home Lyme disease test kit is delivered to your home, where you can collect the sample privately and comfortably. The kit will include the instructions, the sample collector, and the box to return the sample.
Once the results are ready, you will receive them in your email or through the company’s online portal, or they will be sent to your doctors office.
Notes On Serological Tests

For patients with illness lasting over a month, only IgG testing should be performed . A positive IgM test alone is not sufficient to diagnose current disease in these patients.
Due to antibody persistence, a positive serological test cannot distinguish between active and past infection.
Serological tests:
- should not be done as a test of cure
- cannot be used to measure treatment response
The EIA test:
- may yield false-positive results when used as a stand-alone test
- may cross-react with antibodies to commensal or pathogenic spirochetes
- there may be some viral infections for certain autoimmune diseases
Also Check: Can You Donate A Kidney If You Have Lyme Disease
Targeting Fats To Fight Lyme
We started this current work to learn how Borrelia burgdorferi acquires key nutrients, like fats, for growth, says Gwynne. The Lyme bacteria, despite being a very successful pathogen, is much more dependent than other bacteria on acquiring nutrients from its environment.
In the process of our research, we found that the organism takes fats called phospholipids directly from its surroundings in the host, and puts them on its surface, says Hu, the Vice Dean of Research at the school and Paul and Elaine Chervinsky Professor of Immunology. That finding led us to look to see if the direct use of a host fat by the bacteria might lead the immune system to recognize it as a foreign substance and create antibodies to it.
What the scientists discovered is that both animals and patients infected with the Lyme bacterium developed autoantibodies to multiple phospholipids. Because autoantibodies can be damaging to the host, these autoantibodies are tightly regulated and tend to disappear quickly once the stimulating factor is removed.
The antibodies also seem to develop much more quickly than traditional antibodies to the Lyme bacterialikely because your body has previously created these autoantibodies and downregulated them, says Hu.
Lyme Disease In Europe And Asia
Lyme disease can also occur in Europe and Asia, where Borrelia garinii and Borrelia afzelii are most commonly found.
Ticks infected with a Lyme disease bacterium can be found in woodlands across the European continent from northern Turkey to northern Sweden. However, Lyme disease is considered endemic in central Europe, where the following countries have the highest tick infection rates: Austria, Czech Republic, southern Germany,Switzerland, Slovakia, and Slovenia. In Europe, Lyme disease is primarily transmitted by the castor bean tick.
Lyme disease has been reported throughout Asia, as well, such as in Russia, Mongolia, northern China, Japan, and Koreaâ âthough infection from a Lyme disease bacterium appears to be relatively uncommon in these areas. In Asia, Lyme disease is transmitted by the taiga tick .
Recommended Reading: Dr Al Miller Lyme Disease
How You Get Lyme Disease
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks can be found in any areas with deep or overgrown plants where they have access to animals to feed on.
They’re common in woodland and moorland areas, but can also be found in gardens or parks.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
What Happens During Lyme Disease Testing
Lyme disease testing is usually done with your blood or cerebrospinal fluid.
For a Lyme disease blood test:
- A health care professional will take a blood sample from a vein in your arm, using a small needle. After the needle is inserted, a small amount of blood will be collected into a test tube or vial. You may feel a little sting when the needle goes in or out. This usually takes less than five minutes.
If you have symptoms of Lyme disease affecting your nervous system, such as neck stiffness and numbness in hands or feet, you may need a test of cerebrospinal fluid . CSF is a clear liquid found in your brain and spinal cord. During this test, your CSF will be collected through a procedure called a lumbar puncture, also known as a spinal tap. During the procedure:
Read Also: Can Lyme Disease Cause Blood Clots
Signs And Symptoms Of Lyme Disease
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
Overview
Lyme disease is an underreported, under-researched, and often debilitating disease transmitted by spirochete bacteria. The spiral-shaped bacteria, Borrelia burgdorferi, are transmitted by blacklegged deer ticks. Lymes wide range of symptoms mimic those of many other ailments, making it difficult to diagnose .
The blacklegged ticks can also transmit other disease-causing bacteria, viruses, and parasites. These are known as coinfections . These ticks that transmit Lyme are increasing their geographical spread. As of 2016, they were found in about half the counties in 43 of 50 states in the United States .
Lyme is the fifth most reported of notifiable diseases in the United States, with an estimated 329,000 new cases found annually . Some studies estimate that there are as many as 1 million cases of Lyme in the United States every year .
Most people with Lyme who are treated right away with three weeks of antibiotics have a good prognosis.
But if youre not treated for weeks, months, or even years after infection, Lyme becomes more difficult to treat. Within days of the bite, the bacteria can move to your central nervous system, muscles and joints, eyes, and heart .
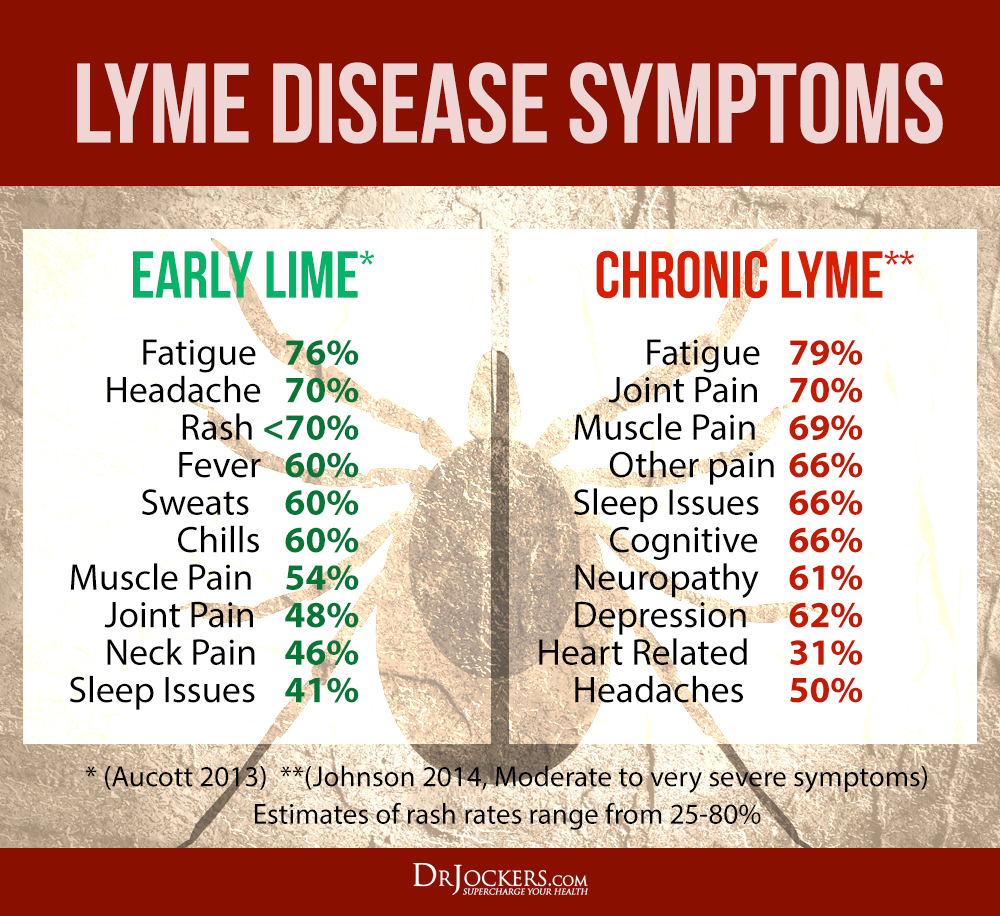
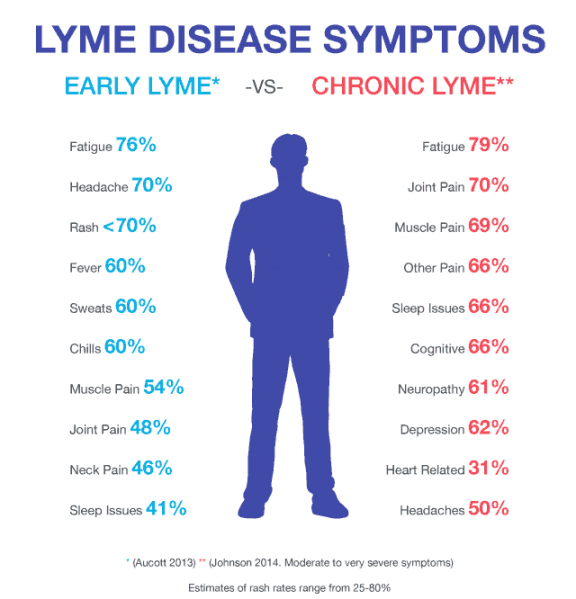
Here is a list of 13 common signs and symptoms of Lyme disease.
Synovial Fluid Pcr For B Burgdorferi
Although reported in a few patients, it is exceedingly difficult to culture B. burgdorferi from synovial fluid in patients with Lyme arthritis. This is presumably due to the fact that joint fluid, with its many inflammatory mediators, is an extremely hostile environment. In spiked cultures, adding small amounts of joint fluid results in rapid killing of spirochetes. In contrast, polymerase chain reaction testing of synovial fluid for B. burgdorferi DNA often yields positive results before antibiotic therapy ,, and usually becomes negative following antibiotic treatment. However, spirochetal DNA may persist after spirochetal killing, which limits its use as a test for active infection. Moreover, PCR testing has not been standardized for routine clinical use. Therefore, in most cases, the appropriate clinical picture and a positive serologic result are sufficient for diagnosis of Lyme arthritis, and PCR testing serves as an optional test to further support the diagnosis.
Recommended Reading: Symptoms Of Lyme Disease After Tick Bite
Negative C6 Elisa On Serum
Early clinical Lyme disease in the form of erythema migrans with associated history of a tick bite should be treated empirically. There is no need for testing unless there are further symptoms.
A negative ELISA result in the early stages of Lyme disease does not exclude infection. If acute Lyme disease is suspected but serology results are negative, we recommend that the test is repeated in 4-6 weeks with a fresh sample to look for seroconversion.
In patients with long term symptoms a negative ELISA test usually excludes Lyme disease as a cause of these symptoms. Information on differential diagnosis for patients with persistent symptoms and negative Lyme disease serology results is available.
Testing Beyond The Lab
Certain types of symptoms require evaluation by diagnostic procedures conducted by specialists in their respective fields. These symptoms include:
- Neurological symptoms: Severe neurological symptoms are evaluated with a nerve conduction test and MRI of the brain to assess the nervous system. The purpose is ruling out multiple sclerosis.
- Cardiac symptoms: Heart symptoms like chest pain and irregular heartbeat are evaluated by EKG and Holter monitor . Findings may lead to cardiac catheterization.
- GI symptoms: Stomach pain and symptoms are often evaluated by an upper endoscopy. Lower intestinal and colon symptoms are evaluated by colonoscopy. Routine colon cancer screening with colonoscopy is recommended every 10 years for everyone over 50.
Don’t Miss: Antibiotics Used For Lyme Disease
If My Dog Tests Positive Does He Need To Be Treated
The decision to treat Lyme disease is somewhat controversial since many infected dogs show no signs of illness. Factors that would support treatment include:
a moderate to high value of QC6 signs of illness compatible with Lyme disease at the time of testing a history of illness compatible with Lyme disease within the past year the presence of abnormal levels of protein in the urine.