When To See Your Gp
You should contact your GP or dial NHS 111 promptly if you feel unwell with any of the symptoms described above after being bitten by a tick or after spending time in areas where ticks may live.
Take this leaflet with you if you are unsure what to say and remember to let your GP know if youve recently had a tick bite or spent time in areas where ticks may live.
Diagnosing Lyme disease can be difficult as many of the symptoms are similar to other conditions. A spreading erythema migrans rash appearing some days after a known tick bite is characteristic and should be treated with antibiotics.
If you dont have this rash but do have other symptoms of Lyme disease, blood tests can be carried out that look for antibodies against the borrelia bacteria.
Blood tests can be negative in the early stages of the infection as the antibodies take some time to reach levels that can be detected.
You may need to be re-tested if Lyme disease is still suspected 4 to 6 weeks after a first negative test result.
If you have long-lasting symptoms, you may be referred to a specialist in microbiology, infectious diseases, rheumatology, or neurology as appropriate for further investigation and management.
Symptoms Of Lyme Disease
A circular or oval shape rash around a tick bite can be an early symptom of Lyme disease in some people.
The rash can appear up to 3 months after being bitten by an infected tick, but usually appears within 1 to 4 weeks. It can last for several weeks.
The rash can have a darker or lighter area in the centre and might gradually spread. It’s not usually hot or itchy.
The rash may be flat, or slightly raised, and look pink, red, or purple when it appears on white skin. It can be harder to see the rash on brown and black skin and it may look like a bruise.
Some people also get flu-like symptoms a few days or weeks after they were bitten by an infected tick, such as:
- a high temperature, or feeling hot and shivery
- tiredness and loss of energy
Some people with Lyme disease develop more severe symptoms months or years later.
This is more likely if treatment is delayed.
These more severe symptoms may include:
- pain and swelling in joints
- nerve problems such as pain or numbness
- trouble with memory or concentration
Lyme Disease Rashes And Look
Circular, expanding rash with target-like appearance.
Expanding rash with central crust
Expanding lesion with central crust on chest.
Expanding erythema migrans
Photo Credit: Reprinted from Bhate C, Schwartz RA. Lyme disease: Part I. Advances and perspectivesexternal icon. J Am Acad Dermatol 2011 64:619-36, with permission from Elsevier.
Description:Early, expanding erythema migrans with nodule.
Multiple rashes, disseminated infection
Early disseminated Lyme disease multiple lesions with dusky centers.
Red, oval plaque
Red, expanding oval-shaped plaque on trunk.
Expanding rash with central clearing
Circular, expanding rash with central clearing.
Bluish hued rash, no central clearing
Bluish hued without central clearing.
Expanding lesion, no central clearing
Expanding lesion without central clearing on back of knee.
Red-blue lesion with central clearing
Red-blue lesion with some central clearing on back of knee.
Insect bite hyper-sensitivity
Large itchy rash caused by an allergic reaction to an insect bite.
Fixed drug reaction
Description:A skin condition that occurs up to two weeks after a person takes a medication. The skin condition reappears at the same location every time a person takes that particular medication.
Ringworm
Description:Ringworm is a common skin infection that is caused by a fungus. Its called ringworm because it can cause a ring-shaped rash that is usually red and itchy with raised edges.
Pityriasis rosea rash
Granuloma annulare rash
Don’t Miss: Neurological Symptoms Of Lyme Disease In Dogs
Achy Stiff Or Swollen Joints
Joint pain and stiffness, often intermittent, are early Lyme symptoms. Your joints may be inflamed, warm to the touch, painful, and swollen. You may have stiffness and limited range of motion in some joints .
Pain may move around. Sometimes your knees may hurt, whereas other times its your neck or your heels. You may also have bursitis . Bursae are the thin cushions between bone and surrounding tissue.
The pain may be severe, and it may be transitory. More than one joint may be affected. Most often the large joints are involved .
People often attribute joint problems to age, genetics, or sports. Lyme should be added to that list, as these statistics indicate:
- One study estimates that 80 percent of people with untreated Lyme have muscle and joint symptoms .
- Fifty percent of people with untreated Lyme have intermittent episodes of arthritis .
- Two-thirds of people have their first episode of joint pain within six months of the infection .
- Use of anti-inflammatory drugs may mask the actual number of people with joint swelling .
Summary:
Joint pain that comes and goes, or moves from joint to joint, could be a sign of Lyme.
Enhancing Healthcare Team Outcomes
The key to Lyme disease is prevention and this requires an interprofessional team approach. All healthcare workers including the nurse practitioner, pharmacist, and primary care provider should provide patient education on measures to prevent tick bites while hiking or working outdoors. In areas where ticks are common, cleaning up of the environment by removing the underbrush and spraying an insecticide may reduce the tick burden in the area. The outdoors person should be told to wear appropriate garments and be familiar with the skin features of the tick bite. The nurse should educate the patient on how to remove the tick from the skin and when to seek medical assistance. The pharmacist should educate the patient on medication compliance for those who have been confirmed to have acquired Lyme disease.
Nurses should educate parents how to inspect their children for ticks at the end of an outdoor event, in an endemic area. While there are many repellants on the market, it is best to avoid them as the risk of harm is greater than any benefit. If one is going to use a repellant, DEET is the one product that is safe, however, it is not 100% effective. finally, the pharmacist should educate the patient about the harms of taking prophylactic doxycycline a better strategy is to remove the tick as soon as it is visualized.
Outcomes
Recommended Reading: Can Mosquitoes Carry Lyme Disease
Including Clinical Symptoms For The Diagnosis Of Lyme Disease
Laboratory testing for Lyme disease is known to have low sensitivity. Lyme specialty laboratories have improved testing methodologies to increase test sensitivity, but they still produce false-negative results. Furthermore, lab tests only provide objective information. Including subjective clinical symptoms improves the accuracy of diagnosis. For example, is there another significant lab result that explains the patients symptom picture?
An individualized approach is particularly significant when dealing with complex and poorly understood multisystem diseases. In opposition to this conservative and traditional approach , some have attempted to oversimplify the diagnosis of Lyme disease by reducing the diagnosis to reliance upon the U.S. CDC surveillance definition. However, the surveillance definition has never been intended to be a sole diagnostic criterion, particularly in late-stage disease.
Which Areas Are More Likely To Have It
The tick that causes Lyme disease has been moving from the Northeast and upper Midwest into the Southern and Western U.S., Mexico, and Canada. Cases in California and Florida are on the rise. After a drop between 2017 and 2018, the numbers jumped a little bit in 2019.
But most Lyme cases in 2019 were in 15 states: Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New
Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, West Virginia, and Wisconsin. Washington, DC, is also a hotspot.
In 2019, Pennsylvania had the most Lyme infections, with 6,763. New York was next, with 2,847 cases.
In the Southern U.S., where itâs hotter, ticks stay under leaves so they don’t dry out. This means people donât get Lyme from Southern ticks very often because they don’t usually come out to bite.
Even though people only report about 30,000 cases of Lyme infection in the U.S. each year, there are actually around 476,000 a year. The same tick also can spread other diseases, including babesiosis, anaplasmosis, and Powassan virus. Those diseases are also on the rise in the U.S.
Whoâs likeliest to get Lyme disease?
Boys up to age 15 and men between the ages of 40 and 60 are the most likely to get Lyme disease. Thatâs because they tend to play outside and go camping, hunting, and hiking.
Why are there more ticks now than there used to be?
There are several reasons why Lyme is spreading. Some of these are:
Recommended Reading: Lyme Disease And Nerve Damage
How Much Does It Cost To Treat A Horse For Lyme Disease
Lyme disease is a relatively big problem for horses. The cost for treatment usually depends on the type of diagnosis, severity of infection, type of treatment, location, and if veterinary care is necessary for anything outside of administering antibiotics.Symptoms of Lyme disease are not always obvious, which means diagnosis can be difficult. However, if the horse shows common symptoms of Lyme disease – fever, lethargy, swollen joints or pain – their vet should be able to diagnose them quickly and recommend treatment.The cost of treatment ranges from around $400-$500 per horse, with antibiotics costing about $20-$40 each at retail prices. Veterinary care also has an associated cost that ranges from about $100-$300 per horse depending on how many treatments are needed and their severity.
How You Get Lyme Disease
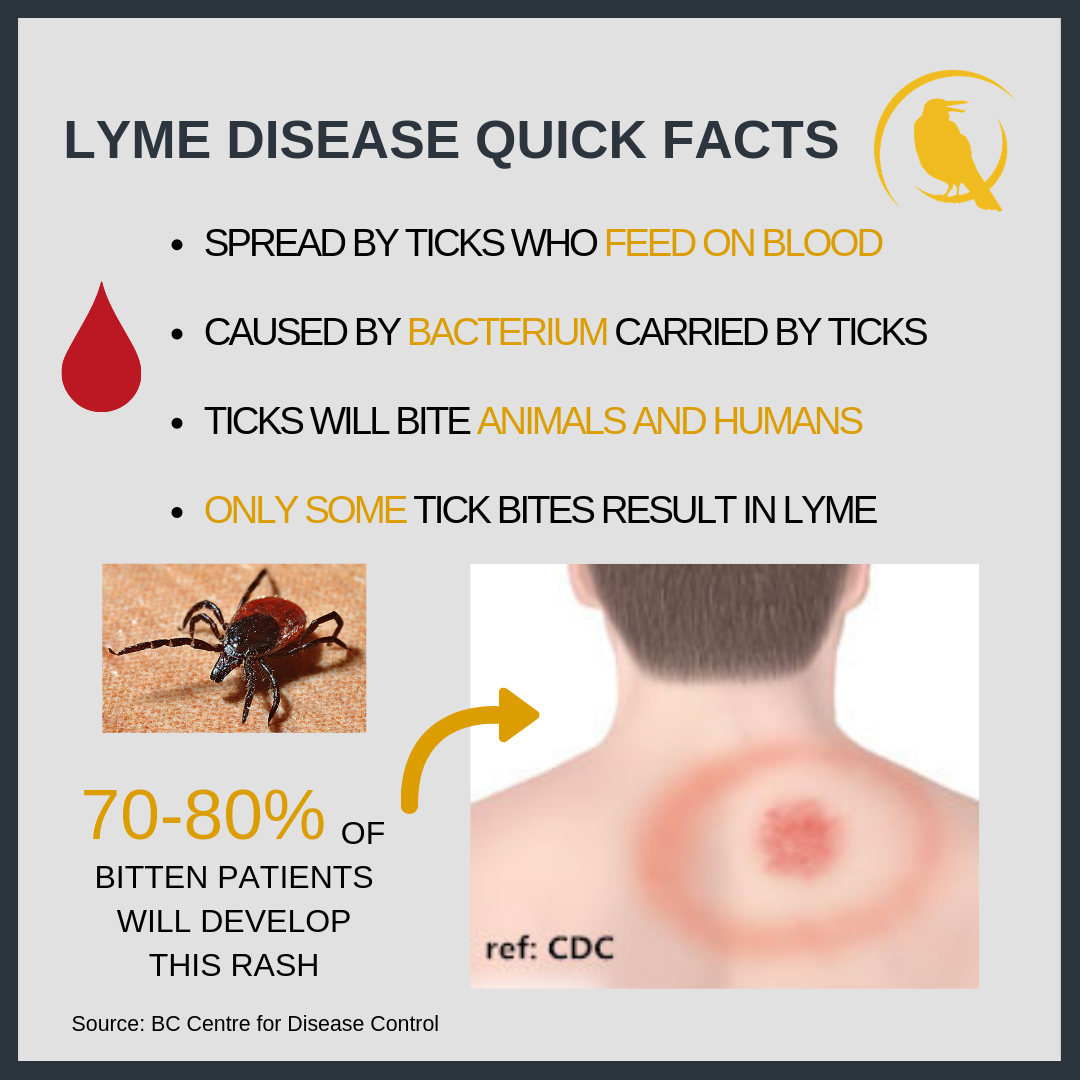
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
Also Check: Antibiotics Given For Lyme Disease
What Do You Do If There’s A Tick Under Your Skin
Use a pair of fine-tipped tweezers to remove it as soon as possible. Pull upward with steady pressure. If parts of the tick are still in your skin, try to get those with the tweezers, too. After everything is out, clean the bite area with rubbing alcohol or soap and water.
You probably wonât get infected if you remove the tick within 36 to 48 hours.
How do you throw away a tick?
Put it in soapy water or alcohol, stick it to a piece of tape, or flush it down the toilet.
Unusual Symptoms Of Lyme Disease
This brings us to unusual symptoms of Lyme disease, especially in chronic cases.
Uncommon chronic Lyme disease symptoms may include the following :
- Shooting pain or generalized pain
These symptoms may come along with common issues like fatigue and joint pain, and they may also come and go. You might also notice that many of these symptoms are quite general and could pertain to any number of conditions. This is how chronic Lyme disease earned the nickname the great imitator, making it difficult to diagnose in the late stages .
Some additional conditions that can occur with chronic Lyme disease include fibromyalgia, meningitis , inflammation of the heart , Parkinsonism , carpal tunnel syndrome, and arthritis .
This isnt to say that you should worry about developing these conditions. We only mention them because, although theyre not considered common, they have occurred in some cases. These conditions also underline the importance of finding a Lyme-literate practitioner and pursuing diagnosis and treatment as soon as possible.
Also Check: How Long For Lyme Disease Test Results
What Are The Complications Of Lyme Disease
Lyme disease affects people differently. Relapse and incomplete treatment responses happen. Relapse and incomplete treatment responses happen. Complications of untreated early-stage disease include:
-
Frequent hospitalizations to manage the disease
Some of these complications result in chronic, debilitating conditions.
Some people may develop post-Lyme disease syndrome . A condition also known as chronic Lyme disease includes PLDS, but also other syndromes. Usually, these are characterized by persistent musculoskeletal and peripheral nerve pain, fatigue, and memory impairment.
What If My Symptoms Continue Or Come Back After Treatment
Follow-up is a mainstay of care for patients with Lyme disease and other tick-borne infections. If symptoms have not resolved, if they return after treatment is stopped, or if new symptoms develop, it is important for your healthcare provider to consider persistent infection as a possible cause of your illness. The bacteria that cause Lyme disease have been shown in the lab as well as in animal and human studies to be able to survive despite antibiotic treatment.
Make sure to discuss other conditions and symptoms with your doctor. A provider must take into account pre-existing conditions, other illnesses, as well as co-infections from other tick-borne organisms, when mapping out a treatment course.
Recommended Reading: Can Lyme Disease Be Cured In Dogs
What Happens At Your Appointment
The GP will ask about your symptoms and consider any rash or recent tick bites you know about.
Lyme disease can be difficult to diagnose. It has similar symptoms to other conditions and there’s not always an obvious rash.
2 types of blood test are available to help confirm or rule out Lyme disease. But these tests are not always accurate in the early stages of the disease.
You may need to be retested if you still have Lyme disease symptoms after a negative result.
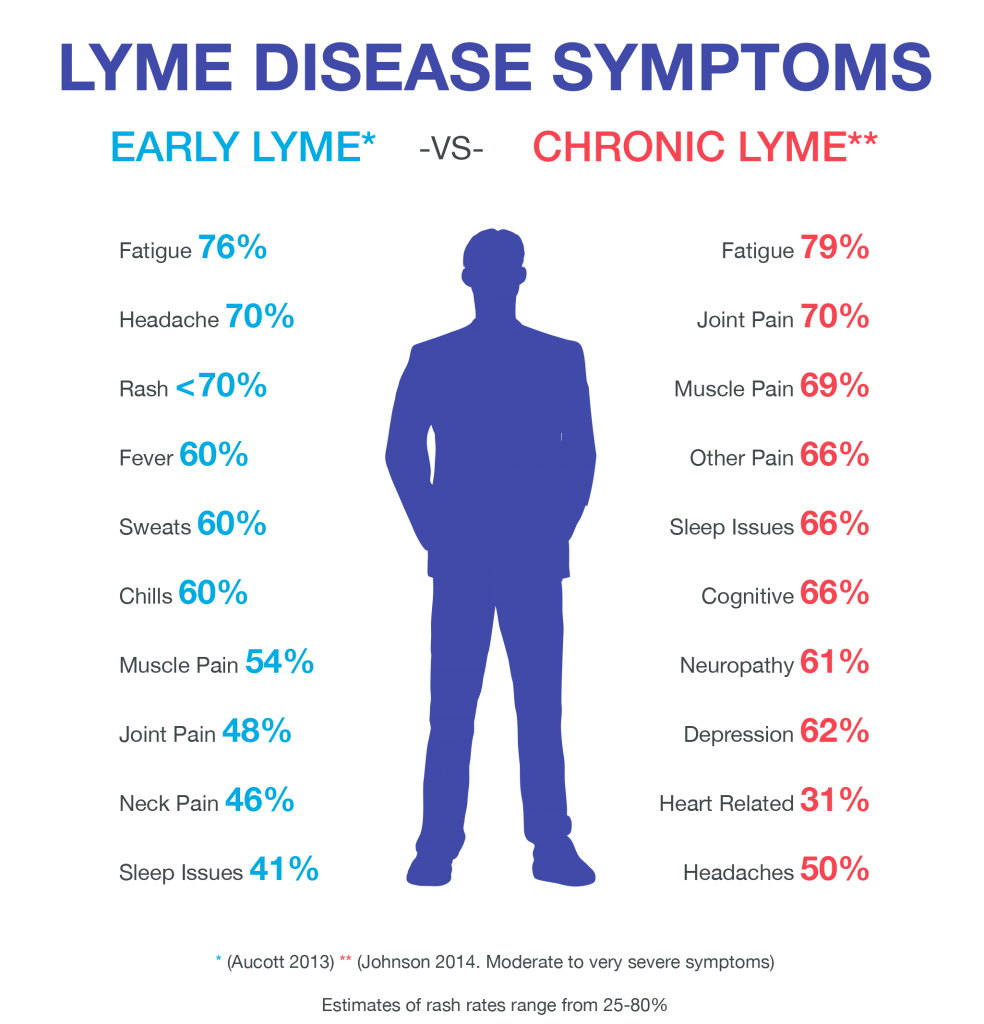
The Numbers On Chronic Lyme
Because Lyme disease is commonly missed or misdiagnosed, statistics vary on how many Lyme patients go on to experience chronic symptoms. The following research nonetheless paints a basic picture of the problem.
- An estimated 5-20% of patients may have chronic symptoms after getting Lyme disease, according to the Columbia University Irving Medical Center.
- The treatment failure rate for chronic Lyme disease patients was estimated at 26-50% in 2004, compared to 16-39% for early Lyme patients, according to Lymedisease.org.
- Up to 15-40% of late-stage Lyme patients develop neurological disorders, which are responsible for many common symptoms of chronic Lyme disease.
Experts dont know for sure why some people experience persistent symptoms, even with treatment. However, some believe the Lyme infection may trigger an auto-immune response that manifests in the chronic symptoms detailed below.
Recommended Reading: Lyme Disease In Dogs Cure
How Can I Tell If I Have Lyme Disease
Lyme disease should be clinically diagnosed. This means a medical professional must evaluate your symptoms, physical findings, exposure risk, and any test results to determine whether you have the disease. No single factor or test result is enough to determine whether you do or do not have Lyme or other tick-borne illnesses.
Why Isnt A Test Result Enough To Tell Me If I Have Lyme
Common tests for Lyme disease include ELISAs and Western blots. Both tests work by detecting the patients antibodies reacting to the Borrelia burgdorferi bacteria. Many factors affect that response and the tests ability to measure it, and can produce both false positive and false negative results. Although the CDC recommends a two-step testing process, consisting of an ELISA as a first test, followed by a Western Blot only if the ELISA is positive or uncertain, i.e. no further testing if the first step is negative, this testing scheme is insensitive. Additionally, positive results might reflect an old, rather than current infection. This is why testing is only one part of the information that contributes to making the diagnosis.
You May Like: How Long Before Lyme Disease Symptoms Appear
Can I Catch Lyme Disease From My Dog
Dogs are not a direct source of infection for people. Lyme disease cant be transmitted from one pet to another, nor from pets to humans, except through tick bites. However, a carrier tick could come into your house on your dogs fur and get on you.
If your dog is diagnosed with Lyme disease, you and any other pets have probably been in the same outdoor environment and may also be at risk, so it is a good idea to consult with your physician and veterinarian to see whether you should test other pets or family members.
When Should I See My Healthcare Provider
If you feel sick after having spent time in areas where ticks might live, you should make an appointment with your healthcare provider.
If you received a Lyme disease diagnosis and you dont feel well after taking all of your antibiotics, contact your provider. This is especially true if you have symptoms like a stiff neck or mental confusion.
You May Like: What Are The 3 Stages Of Lyme Disease
Is Lyme Disease Curable In Horses
Lyme disease is a tick-borne illness. It is caused by an infection with Borrelia burgdorferi bacteria, which is transmitted to people through the bite of infected ticks. Borrelia burgdorferi can cause symptoms such as fever, weight loss, fatigue, stiffness of the neck and joints, lameness and swollen lymph nodes. Lyme disease can affect both humans and animals.In humans, the disease can be cured if it’s caught early enough. However, this may not be the case for horses as the symptoms are not as obvious. It can be difficult to diagnose due to its similarities with other diseases and its lack of symptoms in the early stages.Lyme disease in horses cannot be cured but treatment usually helps control the symptoms.The antibiotics Doxycycline and Amoxicillin are often prescribed to help control symptoms of Lyme disease in horses.There is no vaccine for Lyme disease and early detection and treatment is critical.
Cognitive Neurological And Psychological Symptoms
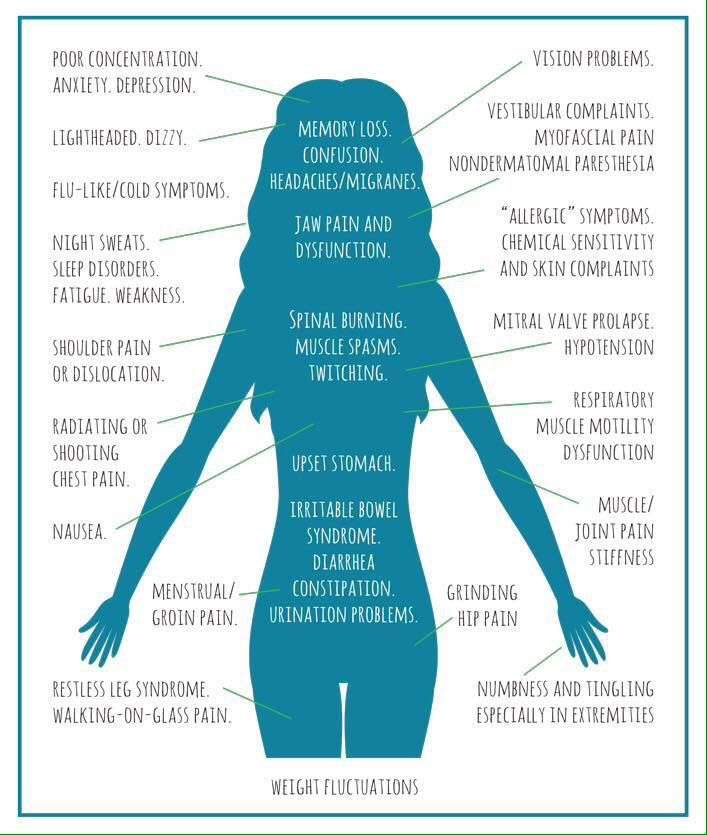
Lyme disease can cause cognitive, neurological, and, in some cases, psychological symptoms. It can affect the central, cranial, and peripheral nervous systems.
When the bacteria affect the nervous systems, it can cause neurological symptoms. They :
- Central nervous system: This may cause sensitivity to light, issues with vision, stiff neck, fever, or headache.
- Cranial nervous system: This may cause facial palsy, which is drooping facial features on one or both sides of the face.
- Peripheral nervous system: This may cause tingling or numbness, a sharp, shooting pain, and weakness in the arms or legs.
The symptoms can often resemble those of other disorders, which could lead to misdiagnosis.
Don’t Miss: Red Light Therapy For Lyme Disease