How Is Lyme Disease Transmitted
Ticks usually live in woods or tall grasslands in Canada, the United States, Europe, and Asia. Ticks can become infected with Borrelia burgdorferi by feeding on infected wild animals, and then can spread the bacteria when they feed on blood from the host. Ticks cannot fly – they hang onto small bushes or tall grasses and are usually found close to the ground. They wait for an animal or person to pass near them and when the animal or person makes contact, the ticks attach themselves to the skin to feed.
In North America, Lyme disease is transmitted mainly by two species of ticks:
- Blacklegged tick , Ixodes scapularis.
- Western blacklegged tick, Ixodes pacificus.
The Public Health Agency of Canada states that there no evidence that Lyme disease can spread from person-to-person. Pets, especially dogs, can get Lyme disease, but there is no evidence that pets can spread the infection directly to humans. They may, however, carry infected ticks into the home or yard which may increase the chance of transmission.
Lyme Disease: How To Prevent Detect And Treat
The arrival of spring and rising temperatures means the return and multiplication of ticks. The month of May is dedicated to raising awareness of Lyme disease and helping to educate the public about the symptoms and cause of this disease.
In Europe, it is considered the most widespread vector-borne disease* in theregion and more than 360,000 cases have been reported over the past two decades. In France, the Pasteur Institute reported an estimated annual incidence rate of approximately 53 per 100,000 people between 2009 and 2017.
On this occasion, UNRIC interviewed Dr. Océane Sorel, a specialist in virology, immunology and member of the United Nations Team Halo**, about this disease. You can also find her on Instagram, @thefrenchvirologist where she popularizes medical science with humour.
What is Lyme disease?
It is an infectious disease caused by a bacterium called Borrelia burgdorferi. It is transmitted by a tick bite infected with the bacteria.
When an infected tick bites you, the bacteria passes into your body through its saliva, then multiplies and spreads.*
It takes some time for the bacteria to be transmitted, which is why the risk of infection is usually low when the tick is on your body for less than 24 hours.
This disease is transmitted only through tick bites and cannot be transmitted from human to human.
What are the symptoms?
There may also be flu-like symptoms such as fever, chills, headache or body aches.
When and how to get diagnosed?
What If Lyme Disease Goes Untreated
If Lyme disease goes untreated, it can affect other systems in the body. According to the , common symptoms of later stage Lyme disease include:
- severe headaches and neck stiffness
- additional erythema migrans rashes on other areas of the body
- facial palsy, which is a loss of muscle tone or droop on one or both sides of the face
- arthritis with severe joint pain and swelling, particularly in the knees and other large joints
- intermittent pain in tendons, muscles, joints, and bones
- heart palpitations or an irregular heartbeat
- episodes of dizziness or shortness of breath
- inflammation of the brain and spinal cord
- nerve pain
- shooting pains, numbness, or tingling in the hands or feet
Also Check: How Soon Does Lyme Disease Show Up In Humans
The Igenex Lyme Immunoblot Solves These Problems
IGeneX has developed a serological test that increases specificity without sacrificing sensitivity that has changed how to test for Lyme disease. It uses specifically created recombinant proteins from multiple species and strains of Lyme borreliae and reduces inconsistencies in reading and interpreting the test bands.
More species detected The Lyme ImmunoBlot tests for more species of Lyme borreliae than the traditional ELISA and Western blot tests, reducing the risks of false negatives due to the inability to detect antibodies to a certain strain or species of Lb. The test includes all Borrelia-specific antigens relevant in North America and Europe, not just B. burgdorferi B31 or 297.
The result is a single test that replaces at least 8 Western blots.
More accurate testing The ImmunoBlot uses specific recombinant proteins that are sprayed in precise amounts onto specific locations on the membrane strip, allowing for greater control of the quantity and location of the antigens. This makes reading the bands much more accurate and consistent.
Earlier detection The ImmunoBlot can detect infections at multiple stages of illness, letting you catch infections earlier.
The IgM and IgG ImmunoBlots superior specificity and sensitivity make them the best Lyme disease test available.
What You Need To Know About Lyme Disease
-
Lyme disease is an infection caused by the spiral-shaped bacteria Borrelia burgdorferi, which is most commonly transmitted by a tick bite.
-
There are over 300,000 estimated new cases of Lyme disease in the United States each year.
-
The symptoms of Lyme disease depend on the how long the infection has been present in the body. The first sign of Lyme disease is often an expanding round or oval red “bullseye” rash.
-
If left untreated, people may develop neurological symptoms and heart problems, and have an approximately 60 percent chance of developing Lyme arthritis.
You May Like: Lyme Disease Symptoms In Animals
Diagnosis Of Lyme Disease
Many cases of Lyme disease are initially misdiagnosed. Lyme disease can be difficult to diagnose because early symptoms of fever, severe fatigue, and achiness are also common in many other illnesses. In addition, diagnostic blood tests are not always dependable, particularly in early disease. However, the round expanding red lesion rash is a unique sign that is more specific for Lyme disease, and many times a diagnosis can be made based on the tell-tale erythema migrans rash itself. Yet, it is important to understand that the erythema migrans rash is not always present or recognizable, and symptoms can fluctuate.
Think the Lyme disease rash is always a bulls-eye? Think again.Think its a spider bite? Think again. Please refer to our poster of varied rash manifestations as a helpful Lyme disease rash identification tool.
Recognizing the Lyme disease erythema migrans rash can be crucial to early diagnosis and treatment.
Despite common belief, the stereotypical ring within a ring bullseye rash is only present in a minority of Lyme disease patients. Instead, the majority of Lyme disease rashes are uniformly red or blue-red and do not have a central clearing or bullseye. Sometimes the site of the tick bite is clearly visible in the center of this lesion. The erythema migrans rash is almost always round or oval and expands over days to a diameter greater than 2. The Lyme rash is often confused with a spider bite, despite spider bites not expanding in this way.
What Are The Signs And Symptoms Of Lyme Disease
Tick bites are usually painless and most people do not know they have been bitten. Signs and symptoms of Lyme disease vary greatly from person to person, and may appear anywhere between 3 to 30 days after a person has been bitten.
Symptoms often include:
- Swollen lymph nodes.
- Skin rash.
One sign of infection can be an expanding rash, sometimes referred to as a “bull’s eye” rash because it may have rings spreading from the bite site ). It is important to note that rashes without the bull’s eye may occur, and that rashes do not appear in every case of Lyme disease infection.
The PHAC states that if left untreated, more severe symptoms may occur and can last from months to years. Severe symptoms may include:
- Severe headaches
- Additional EM skin rashes..
- Neurological disorders
- Nervous system disorders, including facial paralysis or Bell’s palsy .
- Intermittent muscle, joint, tendon, and bone aches
- Arthritis with severe joint pain and swelling, particularly the knees and less commonly in other joints such as the ankle, elbow, and wrists.
If untreated, a condition called late disseminated Lyme disease may occur. PHAC reports symptoms include recurring arthritis , nervous system and/or neurological problems. Symptoms can also include numbness and/or paralysis . Deaths from Lyme disease are rare but may occur.
PHAC provides more information on Lyme Disease.
Recommended Reading: Is Lyme Disease A Bacterial Infection
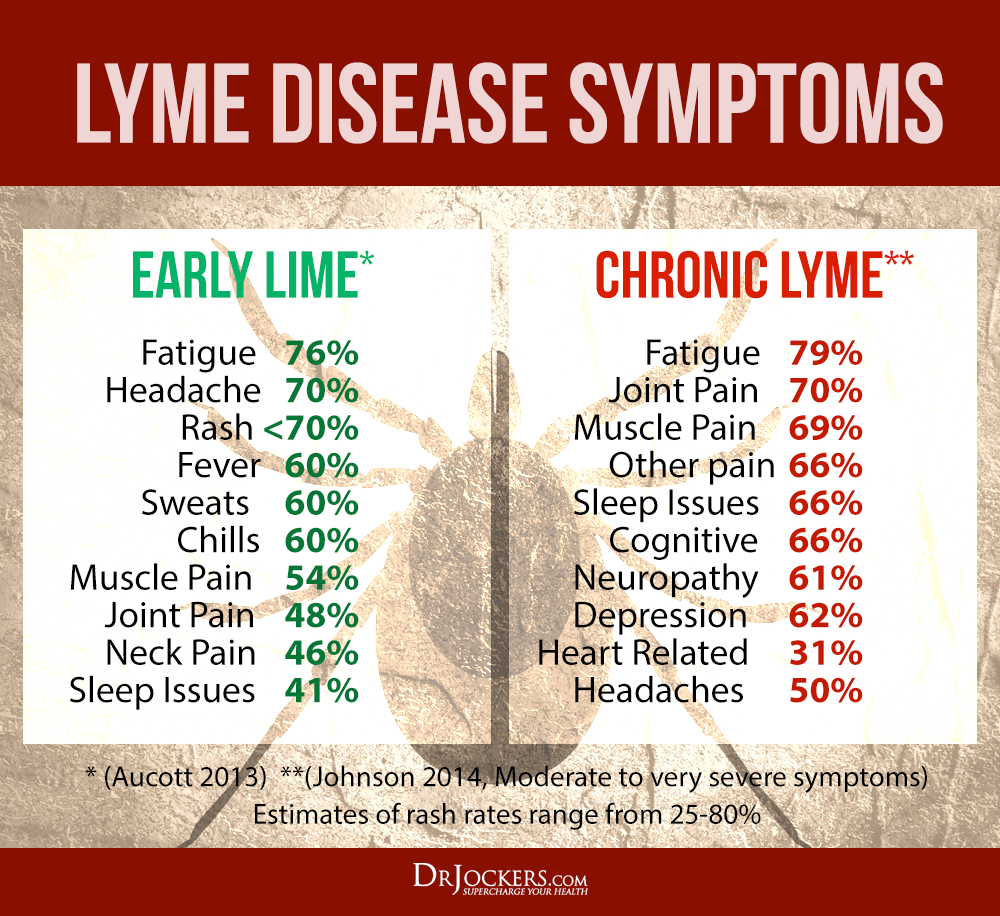
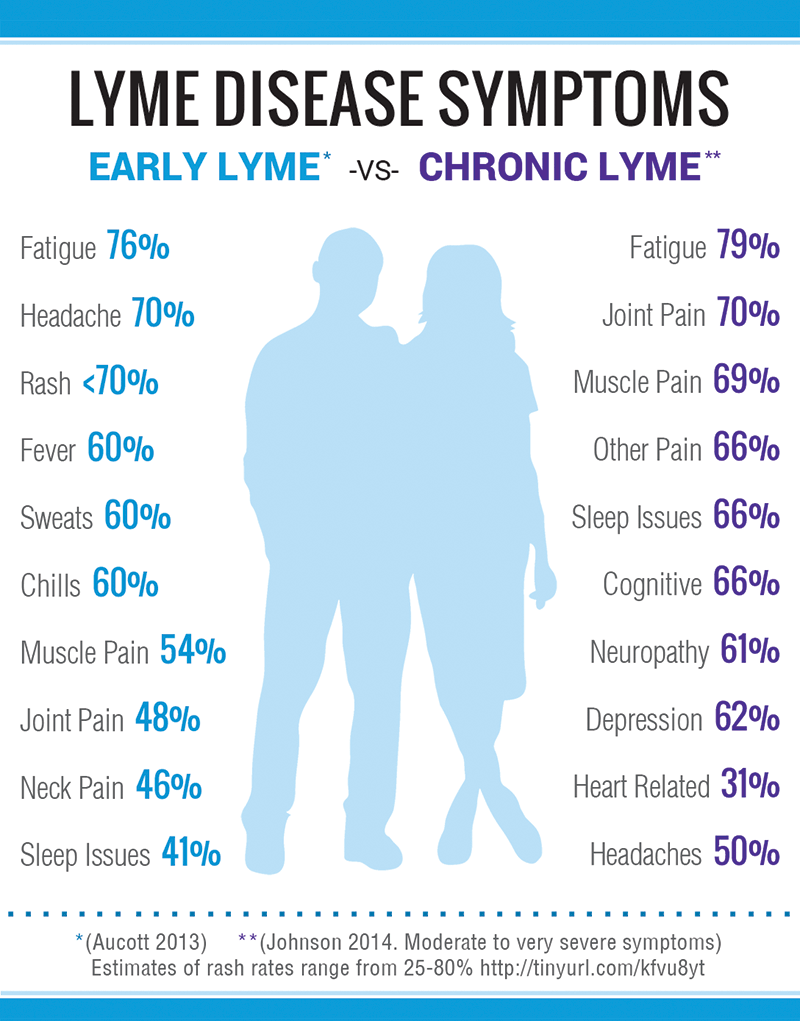
Chronic Lyme Disease Patients Profoundly Debilitated
Many patients with chronic Lyme disease are profoundly debilitated. Investigators of the four NIH-sponsored retreatment trials documented that the patients quality of life was consistently worse than that of control populations and equivalent to that of patients with congestive heart failure. Pain levels were similar to those of post-surgical patients, and fatigue was on par with that seen in multiple sclerosis.
An LDo published survey of over 3,000 patients with chronic Lyme disease found that patients suffer a worse quality of life than most other chronic illnesses, including congestive heart failure, diabetes, multiple sclerosis and arthritis. Over 70% of patients with chronic Lyme disease reported fair or poor health. Similar results have been found in other studies. Many of the symptoms associated with Lyme disease are common in other diseases. The CDC surveillance criteria for confirmed cases specifically exclude most of the symptoms that patients report, including fatigue, sleep impairment, joint pain, muscle aches, other pain, depression, cognitive impairment, neuropathy, and headaches. However, these common symptoms can be severe and may seriously affect quality of life.
How Lyme Disease Is Diagnosed
Your doctor or other healthcare provider may have difficulty diagnosing Lyme disease because many of its symptoms are similar to those of other disorders and illnesses. The only distinctive sign unique to Lyme disease is absent in at least a quarter of the people who become infected. Although a tick bite is an important clue for diagnosis, many people can’t recall having been recently bitten by a tick. This isn’t surprising because the deer tick is tiny, and a tick bite is usually painless.
Also Check: Do You Get A Rash With Lyme Disease
Early Symptoms Of Lyme Disease
Early symptoms will typically develop 1 to 4 weeks after being bitten, however, they can appear anytime between 3 to 30 days after exposure.
Many people with early-stage Lyme disease develop a distinctive circular red rash usually, but not always, at the site of the tick bite.
The rash is often described as looking like a bulls-eye on a dart board and is known as erythema migrans. The affected area of skin will be red and the edges may feel slightly raised.
The size of the rash can vary significantly and it may expand over several days or weeks. Typically, its around 15cm across but it can be much larger or smaller than this.
Some people may develop several rashes on different parts of their body. However, around one in every 3 people with Lyme disease do not report seeing a rash.
As well as a rash, people with early Lyme disease may experience any of the following:
- flu-like symptoms such as fever and sweats, chills, fatigue, neck pain or stiffness, headaches, joint or muscle pains
- paralysis of the facial muscles, typically only on one side of the face
- nerve pains, which may be shooting, sharp or prickly and which follow the course of the nerve
How To Remove A Tick
Removing a tick is the same for humans and animals. Its important you do not crush or damage the tick because it could cause Lyme bacteria to pass from the tick into your bloodstream.
How to remove a tick.
Read Also: Lyme Disease In Dogs Prognosis
How Do You Diagnose The Later Stages Of Lyme Disease
Disseminated Lyme disease, due to unsuccessful or delayed treatment, can become disabling. The bacteria can leave the skin where it was initially inoculated by the tick and travel through the bloodstream to numerous systems of the body, primarily joints, heart, brain, muscles and the nervous system.
Late disseminated Lyme disease has a wide range of presentations including joint pain, extreme fatigue, neuromuscular pain, cardiac problems, headaches, and other central nervous system dysfunction. There are some distinguishable signs of later stage Lyme disease including facial palsy in the second stage, and swollen knees in the third stage that are somewhat specific for Lyme disease, but not absolutely, because there are other causes of Bells Palsy and swollen knees.
Diagnosis can be confirmed by serology blood tests which measure the antibodies that are formed by the immune system in response to the Lyme disease bacterial infection. Collection of cerebrospinal fluid by lumbar puncture may be indicated in neurologic cases that may involve the central nervous system.
How To Avoid Getting A Tick Bite
You might be at risk if you live, work in, or visit a wooded area, or an area with tall grasses and bushes .
You may also be at risk if you are involved in outdoor activities such as hiking, camping and gardening.
You may be bitten by a tick and not even know it.
Heres what you can do to avoid getting a tick bite.
Read Also: Arthritis Caused By Lyme Disease
Sign Up For Our Newsletter
Disclaimer: The above material is provided for information purposes only. The material is not nor should be considered, or used as a substitute for, medical advice, diagnosis, or treatment, nor does it necessarily represent endorsement by or an official position of Global Lyme Alliance, Inc. or any of its directors, officers, advisors or volunteers. Advice on the testing, treatment or care of an individual patient should be obtained through consultation with a physician who has examined that patient or is familiar with that patients medical history. Global Lyme Alliance, Inc. makes no warranties of any kind regarding this Website, including as to the accuracy, completeness, currency or reliability of any information contained herein, and all such warranties are expressly disclaimed.
What Abnormal Results Mean
A positive ELISA result is abnormal. This means antibodies were seen in your blood sample. But, this does not confirm a diagnosis of Lyme disease. A positive ELISA result must be followed up with a Western blot test. Only a positive Western blot test can confirm the diagnosis of Lyme disease.
For many people, the ELISA test remains positive, even after they have been treated for Lyme disease and no longer have symptoms.
A positive ELISA test may also occur with certain diseases not related to Lyme disease, such as rheumatoid arthritis.
You May Like: Rentals In East Lyme Ct
Stage : Early Disseminated Lyme Disease
Early disseminated Lyme disease occurs several weeks to months after the tick bite.
Youll have a general feeling of being unwell, and a rash may appear in areas other than the tick bite.
This stage of the disease is primarily characterized by evidence of systemic infection, which means infection has spread throughout the body, including to other organs.
Symptoms can include:
- disturbances in heart rhythm, which can be caused by Lyme carditis
- neurologic conditions, such as numbness, tingling, facial and cranial nerve palsies, and meningitis
The symptoms of stages 1 and 2 can overlap.
What Is The Difference Between This Indirect Blood Diagnostic Test And A Direct Test
Direct diagnostic tests measure the presence of the bacteria directly and are much more reliable than tests looking for indirect measurement of antibodies that measure a persons immune response to an infection. Lyme disease diagnoses and disease management would benefit from validated diagnostic tests that directly measure the infection such as a culture, PCR test, or antigen detection tests. Direct tests are vital to the management of other infectious diseases such as HIV, hepatitis C, strep, and COVID-19, but have not yet become widely available for Lyme disease.
Read Also: Lyme Disease Treatment Without Antibiotics
Are There Any Risks To Lyme Disease Tests
There is very little risk to having a blood test or a lumbar puncture. If you had a blood test, you may have slight pain or bruising at the spot where the needle was put in, but most symptoms go away quickly. If you had a lumbar puncture, you may have pain or tenderness in your back where the needle was inserted. You may also get a headache after the procedure.
Diagnostic Test Performance In Early Lyme Disease
Testing for LD in patients exhibiting signs and symptoms of LD for less than 30 days is challenging as the performance of available test protocols is not optimal for making clinical decisions. This is largely due to the time required for the infected individuals immune system to mount a reaction. This is why researchers have explored the use of a variety of targets including VlsE and C6 expressed after infection, Osp C and Fla B expressed by the feeding tick to detect infection sooner . However, cross-reactivity and genetic variability within the targets has limited the diagnostic performance of any single target . Thus the results of expected sensitivities and specificities in emphasize the importance of physician evaluation and informed judgement when deciding to treat rather than rely entirely on imperfect serological test protocols. Notable findings in the table include the higher specificity associated with the two-tier testing method and the poor and highly variable sensitivity of serological tests in the initial stages of disease when an individual is mounting an immune response to B. burgdorferi.
You May Like: Side Effects Of Lyme Disease In Humans