Autoimmune Diseases And Lyme Disease: Misdiagnosis Or Complication Of Lyme
As mentioned above, there are documented correlations between Lyme and autoimmune diseases. The evidence shows that Lyme disease may trigger an autoimmune disease, or it may mimic an autoimmune disease.
What does this mean for patients and physicians? It comes down to the importance of getting an accurate and timely diagnosis if you suspect Lyme or another tick-borne disease. The longer Lyme disease goes untreated, the stronger the chance that it will spread to multiple body systems and possibly trigger an autoimmune response.
Because Lyme disease symptoms mimic symptoms of so many other conditions, including autoimmune diseases, it is notoriously tricky to diagnose. One of the most common Lyme disease misdiagnoses is the autoimmune disease rheumatoid arthritis , characterized by chronic joint pain.
If a patient with Lyme is diagnosed with RA without the Lyme being detected and treated, not only can the arthritic symptoms of Lyme persist and worsen, but the Lyme can also go on to affect more systems, causing neurological and psychiatric symptoms, heart problems, and more. In rare cases, untreated Lyme can even be fatal.
Meet With An Autoimmune Or Lyme Disease Specialist
With any chronic condition such as Lyme disease, implementing effective & holistic treatments that will put you on the road to recovery is a top priority for all of us at LifeWorks Wellness Center.
We provide every patient with individualized, quality treatment. As one of Floridas top autoimmune disease clinics, our doctors understand what you are going through and can give you a proper diagnosis that will identify whether you are suffering from an autoimmune disease or even Lyme.
Is Lyme Disease Autoimmune
The relationship between Lyme disease and autoimmunity is controversial. Some researchers in the Lyme disease space claim that chronic Lyme disease doesnt exist. They argue that people previously infected with Lyme disease who experience symptoms beyond the standard course of antibiotics are suffering from a purely autoimmune phenomenon, referred to as post-treatment Lyme disease or a post-Lyme autoimmune syndrome. However, those who argue for the existence of post-Lyme autoimmune syndrome dont ask, what might be the cause of the autoimmunity? The term post-Lyme autoimmune syndrome discredits the possibility of chronic, ongoing Lyme disease infection as an autoimmune trigger. So what is the truth? Can chronic Lyme disease cause autoimmunity?
Lyme disease is known to evade antibiotic treatment and persist in the body, creating a chronic infection. As well discuss shortly, there are several known mechanisms through which chronic infections trigger autoimmune processes. Based on the available research, it is highly likely that chronic Lyme disease triggers autoimmunity, NOT that autoimmune disease spontaneously appears after Lyme treatment, in the absence of ongoing infection.
How does Lyme disease trigger an autoimmune response? Here are a few mechanisms linking Lyme disease and autoimmune disease:
Don’t Miss: What Kind Of Ticks Cause Lyme Disease
Holistic Health Care And Chronic Lyme
It is more than apparent that in the case of Lyme disease, practical antibiotic treatments are not always effective in treating the disease. With up to 20% of diagnosed Lyme patients experiencing chronic Lyme even after being administered long-term antibiotic treatments, its important for those afflicted with chronic Lyme to find treatments that work to rid the body of the devastating bacteria and rebuild the integrity of the immune system so it may fight the residual bacteria that causes the chronic symptoms in the first place.At LifeWorks Wellness Center, an all natural holistic healthcare approach has been used to successfully treat chronic Lyme patients all over the country. With individualized treatments tailored specifically to the patients needs, our holistic approach is sure to alleviate the symptoms and address the cause of the disease at its root.
If It Isnt Chronic Lyme What Is It
One day two summers ago, I woke up with a headache behind my right eye and muscle pain in my legs and back. By the end of the day, everything hurt. My skin felt so sensitive I tried not to rest my arm on the table. I was 32 and had always been healthy. I assumed Id get better in a week.
A month went by, and now I had a low-grade fever in addition to daily back and muscle pain. The fever returned at the same time every afternoon, escorted by a host of other strange symptoms: the bridge of my nose burned and swelled , one knee and my jaw seemed to want to unhinge themselves, and I could suddenly, disconcertingly feel my urethraa part of the body that is truly not meant to be felt, in my opinion, but which was now painfully swollen. My right hand sometimes hurt too much to use, and a deep ache radiated through my butt cheeks.
After five months of daily fever and flu symptoms, I was so weak I struggled with stairs. I started spending a significant part of each day in bed. I still wasnt sure what was wrong with me, but I knew it had to be something terrible. So why did test after test continue to come back negative? My primary doctor kept sending me to specialists, but, to my surprise, most of them seemed not to recognize my symptoms as indicating a specific condition.
Extremely general, they said.
Nebulous.
Systemic.
They seemed rushed. They didnt seem to have the time to investigate further.
Take Advil, I was told by several doctors in a row.
Yes, 20.
She did.
Don’t Miss: New Treatment For Lyme Disease
Big Misconceptions Around Lyme Disease
A lot of people think that Lyme disease is relatively rare, but its actually one of the fastest-growing infectious diseases in the US. There are an estimated 329,000 new cases each year, which is 10x higher than the Centers for Disease Control predicted just a few years ago and a 320% increase from the 90s.
You may have also heard that the first sign of Lyme disease is a bullseye-shaped rash. However, not everyone gets this telltale rash and basic tests often dont pick it up, which is why its easy for patients and doctors to miss.
The third big misconception is that its an acute, short-lived sickness. Most people, and honestly most doctors, think you get bitten by a tick, you get sick, you take antibiotics, and you get better.
In reality, a lot of people develop chronic persistent Lyme either because it doesnt get diagnosed and treated, or because it isnt fully treated and youre left with lingering symptoms.
In these cases, there are often co-infections at play, such as Bartonella, Babesia, Mycoplasma, or Rickettsia. They are called co-infections because they are also passed on with the tick bite that transmitted the Lyme disease. They are important to identify because they can be just as problematic for your health.
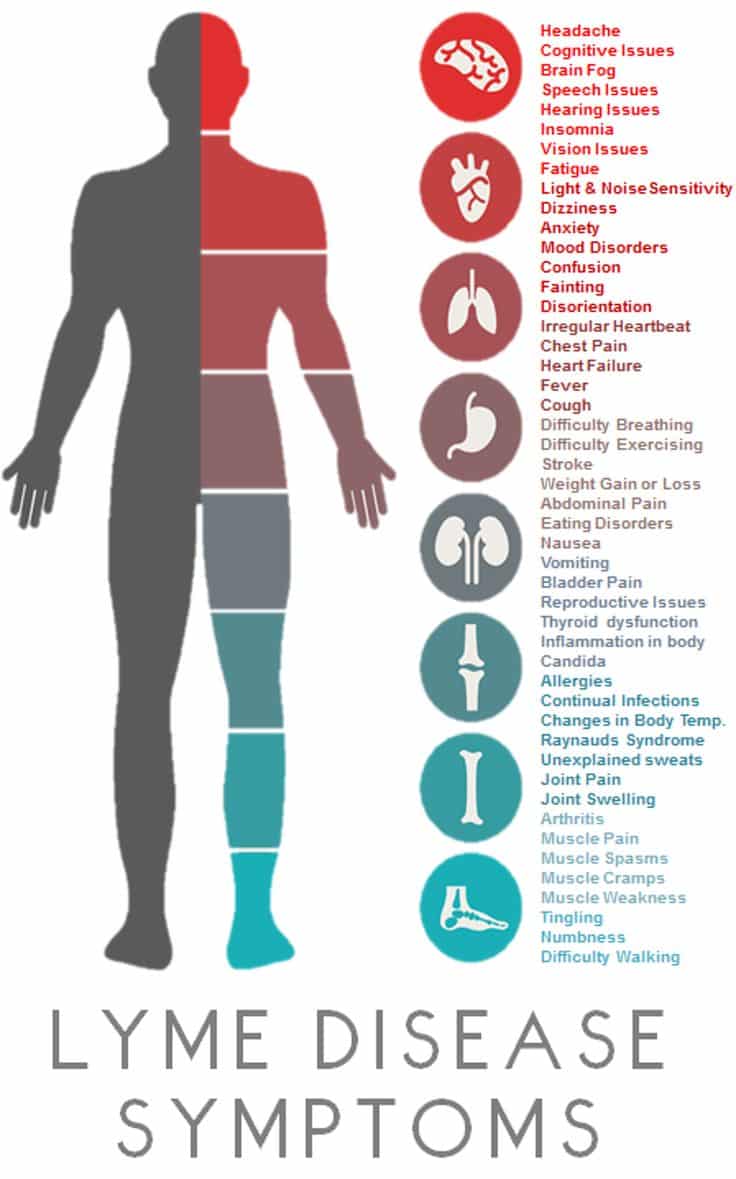
Symptoms Of Lyme Disease
Early symptoms of Lyme disease typically present as a circular red skin rash around a tick bite called Erythema migrans. This red, circular, or oval-shaped rash often expands over a period of days and can reach up to 12 inches across. Sometimes the center clears as it enlarges resulting in a bull’s-eye appearance. It’s typically not itchy or painful but may feel warm to the touch. Some people develop this rash at more than one place on their bodies. The rash can appear up to a month after you’ve been infected, but it usually occurs within one to two weeks and can last for several weeks.
Not everyone with Lyme disease gets the rash. You may also have flu-like symptoms in the first few weeks of infection, such as tiredness, muscle pain, headaches, high temperature , chills, swollen lymph nodes, and joint pain .
A few people with Lyme disease develop more serious symptoms weeks, months, or even years later. These include:
- Severe headaches and muscle pain
- Problems affecting the brain or nerves, such as memory problems, difficulty concentrating, and dizziness
- Pain in the joints and muscles often in the knees
- Heart problems such as heart palpitations, chest pain, and shortness of breath
- Inflammation of the membranes surrounding the brain and spinal cord
Disease signs and symptoms can appear quickly or gradually over time, and they are different for everyone.
Left untreated, Lyme disease may spread to your heart and nervous system.
Recommended Reading: How Do You Cure Lyme Disease
Late Lyme Disease Discovery
To make matters worse, a large portion of people with Lyme disease only realize they have the condition after some time. This could result from an initial misdiagnosis or incorrect treatment. The result is lasting symptoms that worsen over time.
These people, often initially thought to suffer from either chronic fatigue or depression, have also been thought of as hypochondriacs in certain extreme cases. And all this while they had Lyme disease!
Lyme Disease & Pans: Whats The Connection
After a fun family hike in the woods, every parent checks for the big 3 sunburn, poison ivy, and ticks. Plucking ticks from skin once arriving home from a hike isnt such a big deal. However, should ticks be attached to the skin for a longer period of time before being removed, they can leave behind lyme disease, which is a big deal.
Though lyme disease is curable, it can trigger whats known as pediatric acute-onset neuropsychiatric syndrome .
Lyme disease and PANS are both rare but serious conditions. While you shouldnt obsessively worry about your child contracting them, its useful to know what to look for and how to seek help if symptoms arise.
Recommended Reading: Lyme Disease Immune System Weakened
The Autoimmune Protocol Diet
The AIP is a specialized version of a Paleo diet that eliminates foods that may stimulate the immune system and harm the gut, where much of the immune system resides and where autoimmunity is theorized to begin in many cases. AIP also focuses heavily on optimizing dietary nutrient density and incorporating foods that mitigate inflammation and support a healthy gut. I have used AIP innumerable times with clients to reduce and even reverse autoimmune disease processes with excellent results. In recent years, the autoimmune protocol has been studied in scientific trials and found to improve symptoms and markers of autoimmune activity in people with autoimmune diseases, ulcerative colitis, and Crohns diseases, including reducing calprotectin. The AIP diet has also been found to decrease systemic inflammation and improve symptoms and quality of life in Hashimotos disease.
The AIP removes the following foods from the diet for at least three months:
-
Nightshades, such as tomatoes and peppers
-
Nuts and seeds
Is Lyme Not An Autoimmune Disease
Lyme disease is said to be an autoimmune disorder, but this is not necessarily true. This is because it is a systemic bacterial infection. The reason why Lyme disease is considered an autoimmune disorder is because the body’s immune system recognizes the cell that the tick-borne bacteria infects and hides in as foreign and attacks it, which can cause damage to healthy tissue. A previously healthy cell infected by the bacterium and attacked by the immune system doesnt necessarily indicate an autoimmune response since the body is targeting an infected cell.
The immune system’s response to Lyme disease also causes some symptoms that might be confused with those of autoimmune disorders as they are similar . These symptoms include joint pain and fatigue.
However, there is a key difference between how the immune system responds to Lyme disease and how it responds to other autoimmune disordersin most autoimmune diseases, the immune system attacks healthy cells for no reason. Additionally, in most autoimmune diseases, the antibodies that attack the healthy cells remain in the bloodstream long after the infection or illness has disappeared. In Lyme disease, however, these antibodies are only present when a person is infected with Borrelia burgdorferi .
To search for the best Neurology Healthcare Providers in Croatia, Germany, India, Malaysia, Spain, Thailand, Turkey, Ukraine, the UAE, UK and the USA, please use the Mya Care search engine.
References:
Don’t Miss: What Are The Signs Of Lyme Disease In A Dog
How To Treat Lyme Disease To Fight Autoimmunity
Ill be honest with you, Lyme is one of the most complex conditions to treat and it takes time and hard work.
Simply prescribing an antibiotic doesnt do the trick once inflammation is systemic, the condition is chronic, or there are autoimmune complications involved.
You need a holistic approach that supports your immune system from the ground up so that your body can fight back against the disease and restore a normal inflammatory response.
This includes eating a nutrient-rich, anti-inflammatory diet, relieving stress, getting plenty of sleep, promoting detox, and overcoming any underlying deficiencies and imbalances.
That being said, Ive seen patients make tremendous progress with a functional medicine approach to Lyme disease.
The patient I mentioned earlier is currently leaps and bounds from where she was before. She is now living life how she wants to, as opposed to what her body and illness was letting her do before.
About the Author: Dr. Seth Osgood is a Doctor of Nursing Practice, Board Certified Family Nurse Practitioner and Institute of Functional Medicine Certified Practitioner. Dr. Osgood received his post-graduate training in Functional Medicine through the IFM and from working with Dr. Amy Myers. He has helped people from around the world improve their health utilizing a Functional Medicine approach.
How To Properly Manage Lyme Disease Autoimmunity
Clearing Lyme disease and other chronic infections is essential for resolving autoimmunity when a chronic infection is the root cause of autoimmunity. A Lyme-literate doctor can guide you through Lyme treatment. However, while youre undergoing Lyme treatment, what can you do to resolve autoimmunity and improve your symptoms and health? Conventional medicine has a minimal repertoire of treatments for autoimmunity, namely broad-spectrum immunosuppressants that are toxic and can have widespread, long-term damaging effects. A functional medicine approach that includes strategic nutritional changes is a powerful and safer alternative to immunosuppressants for addressing autoimmunity during Lyme treatment. The autoimmune protocol diet is particularly effective for autoimmunity.
Recommended Reading: How Fatal Is Lyme Disease
Chronic Lyme Disease Vs Post
Patients typically use the term chronic Lyme disease to describe the cluster of symptoms that started after getting Lyme disease and that persist despite having received a course of antibiotic treatment which has been deemed curative by the Infectious Diseases Society of America. Patients say, Im not cured. I have symptoms now that I never had before Lyme disease. Im fatigued 90% of the day. My muscles ache. My brain is in a fog. I cant think clearly any more. Im super sensitive to light and sound. What is going on? Chronic Lyme disease does exist Im a living example of it!
Whatever one calls it, the experience is the same. Most often these patients experience profound fatigue, pain, and/or cognitive impairment. Mild to moderate levels of depression and anxiety may also accompany these symptoms, as the functional limitations can lead to social isolation, inability to work, and loss of sense of ones identity as a provider, caretaker, or friend. Sometimes patients find themselves identifying with Job the just and good man in the Bible whose life was wrecked by illness, death of loved ones, and economic disaster he felt tormented by God.
Dont Miss: Cbd Oil For Lyme Disease
What Causes Autoimmune Diseases
Most experts agree that autoimmune diseases are caused by environmental triggers. Common examples include foods , toxins , and viral or bacterial infections.
Indeed, there is growing evidence that Lyme disease and other bacterial infections can trigger autoimmune diseases, especially in patients who are genetically predisposed to them. Studies have documented several cases of Lyme disease that appeared to trigger or mimic autoimmune diseases, including Sjogrens syndrome, dermatomyocitis , rheumatoid arthritis , psoriatic arthritis , and spondyloarthritis .
You May Like: What Are The Symptoms Of Neurological Lyme Disease
Autoimmune Disease And Lyme Disease
The incidence of PTLDS has increased over the years, and patients who have undergone antibiotic treatments are coming forward with symptoms they thought had disappeared long ago. Research has revealed that even long-term antibiotic treatment can leave some of the Lyme bacteria unscathed. When the bacteria is not completely eradicated, superficial symptoms can cascade into more serious, neurological conditions.
It is not surprising that chronic Lyme patients might also be afflicted with autoimmune diseases like multiple sclerosis or rheumatoid arthritis. What starts off as a disease bearing physical symptoms like sore joints and chest pain can transform into a chronic illness bearing symptoms of cognitive dysfunction, memory problems, chronic fatigue, and mood disorders.
Medical specialists believe the autoimmune response that triggers the aforementioned symptoms is a result of the residual damage that occurs during the initial infection. The outer coat of the Lyme bacteria is similar to tissue found in our nervous system, and it is believed that the immune system reacts to this leftover tissue, attacking it and mistakenly attacking neuronal tissue as well. Thus, the bacterial tissue that was not eliminated via antibiotics confuses the immune system. The onset of chronic symptoms thereafter are misattributed to other autoimmune diseases, and likewise, the autoimmune diseases may be a direct result of the Lyme infection itself.
A New Study Has Shown That The Bacteria That Causes Lyme Disease Alters The Immune System Causing It To Attack The Healthy Cells In The Human Body
The bacteria that causes Lyme disease Borrelia burgdorferi has been shown to stop communication between dendritic cells and T-cells, which normally signals for a response against foreign invaders.
The study, carried out by researchers at the Johns Hopkins Lyme Disease Clinical Research Center, has demonstrated that the bacteria alters dendritic cells, which normally present proteins from pathogens such as bacteria and viruses, known as antigens, to immune system T-cells, which then signals an immune response against any viruses or infections.
The study has been published in Frontiers in Medicine.
Also Check: How Would I Know If I Had Lyme Disease