Controversy : Validity Of Persistent Manifestations Being Attributable To Lyme Disease
Many patients report ongoing symptoms following treatment for Lyme disease, yet physicians disagree over the nature of these symptoms., Some physicians discount the likelihood that posttreatment symptoms are directly related to the earlier Lyme infection.,, This sentiment is expressed in articles with titles such as Dispelling the Chronic Lyme Disease Myth and in the often-stated phrase, I don’t believe in chronic Lyme. Instead, the suggestion is that patients are simply reporting symptoms commonly seen in the general population or those of a secondary condition such as fibromyalgia or chronic fatigue syndrome.,
Other physicians hold that such symptoms are most likely directly attributable to the previous infection and represent treatment failure. This group notes that most of the reported posttreatment symptoms began before treatment and that the original Lyme diagnoses were, in part, based on their very existence.
Studies demonstrate that symptoms commonly reported by persistent Lyme disease patients occur more frequently in that group than in matched controls or an age-matched subset of the general population.,, For example, 41% of the subjects in Asch and colleagues’ study reported having arthritis. This is 5 times higher than the rate of arthritis in the general US population ages 18 to 44 years.
Antibiotic Treatment For Early
The first line of treatment for early Lyme disease is antibiotics. The most commonly prescribed antibiotics include:
- Doxycycline
- Amoxicillin
- Cefuroxime axetil
These antibiotics are most often administered orally, though intravenous administration is necessary for some patients. Programs are typically 2 weeks long but can be as long as 4 or more weeks.
The Centers for Disease Control and Prevention and the Infectious Diseases Society of America maintain that most cases of Lyme disease clear up quickly from a short course of antibiotics. However, as you will see later in this article, there is much evidence showing that Lyme that is not detected early can actually be very difficult to treat and that even early treatment can be unsuccessful. The presence of coinfections can also complicate the treatment process, again emphasizing the need for comprehensive testing at a specialty lab.
Finally, as acknowledged by the CDC, some Lyme patients experience ongoing or recurrent symptoms despite having received treatment for Lyme. These patients are said to have Post-Treatment Lyme Disease Syndrome . Is this caused by untreated coinfections, persistence of Bb , permanent damage, or an as-yet unidentified immune system problem? The jury is still out, but all may be possible.
What Are The Side Effects Of Lyme Disease Treatments
Antibiotics, like all medications, have the potential for side effects. Any antibiotic can cause skin rashes, and if an itchy red rash develops while on antibiotics, a patient should see their physician. Sometimes symptoms worsen for the first few days on an antibiotic. This is called a Herxheimer reaction and occurs when the antibiotics start to kill the bacteria. In the first 24 to 48 hours, dead bacterial products stimulate the immune system to release inflammatory cytokines and chemokines that can cause increased fever and achiness. This should be transient and last no more than a day or two after the initiation of antibiotics.
The most common side effect of the penicillin antibiotics is diarrhea, and occasionally even serious cases caused by the bacteria Clostridium difficile. This bacterial overgrowth condition occurs because antibiotics kill the good bacteria in our gut. It can be helpful to use probiotics to restore the good bacteria and microbiome balance.
Also Check: How To Treat Dogs For Lyme Disease
Probable Late Lyme Disease
Table presents demographic and clinical characteristics of the 13 patients with probable late Lyme disease in comparison to patients with other Lyme disease and non-Lyme disease related diagnoses. The median age at illness onset was 61 in patients with probable late Lyme disease. The majority of the patients in the overall sample, with exception of those with confirmed late Lyme arthritis, presented with some combination of fatigue, generalized musculoskeletal pain, and cognitive complaints. By definition, patients with probable late Lyme disease had no history of physician documented or treated EM rash and no objective clinical signs associated with late Lyme disease. However, 38% recalled a rash consistent with EM at illness onset not documented or diagnosed by a physician. In some cases the rash was felt by the patient or physician to be atypical for Lyme disease because of the lack of the classic bulls eye appearance or because the rash did not meet the minimum 5cm size in the CDC surveillance criteria . This proportion of prior patient-documented rash in the absence of physician diagnosed erythema migrans was higher in the probable late Lyme disease group when compared to the other four disease groups .
What Is The Staging For Lyme Disease
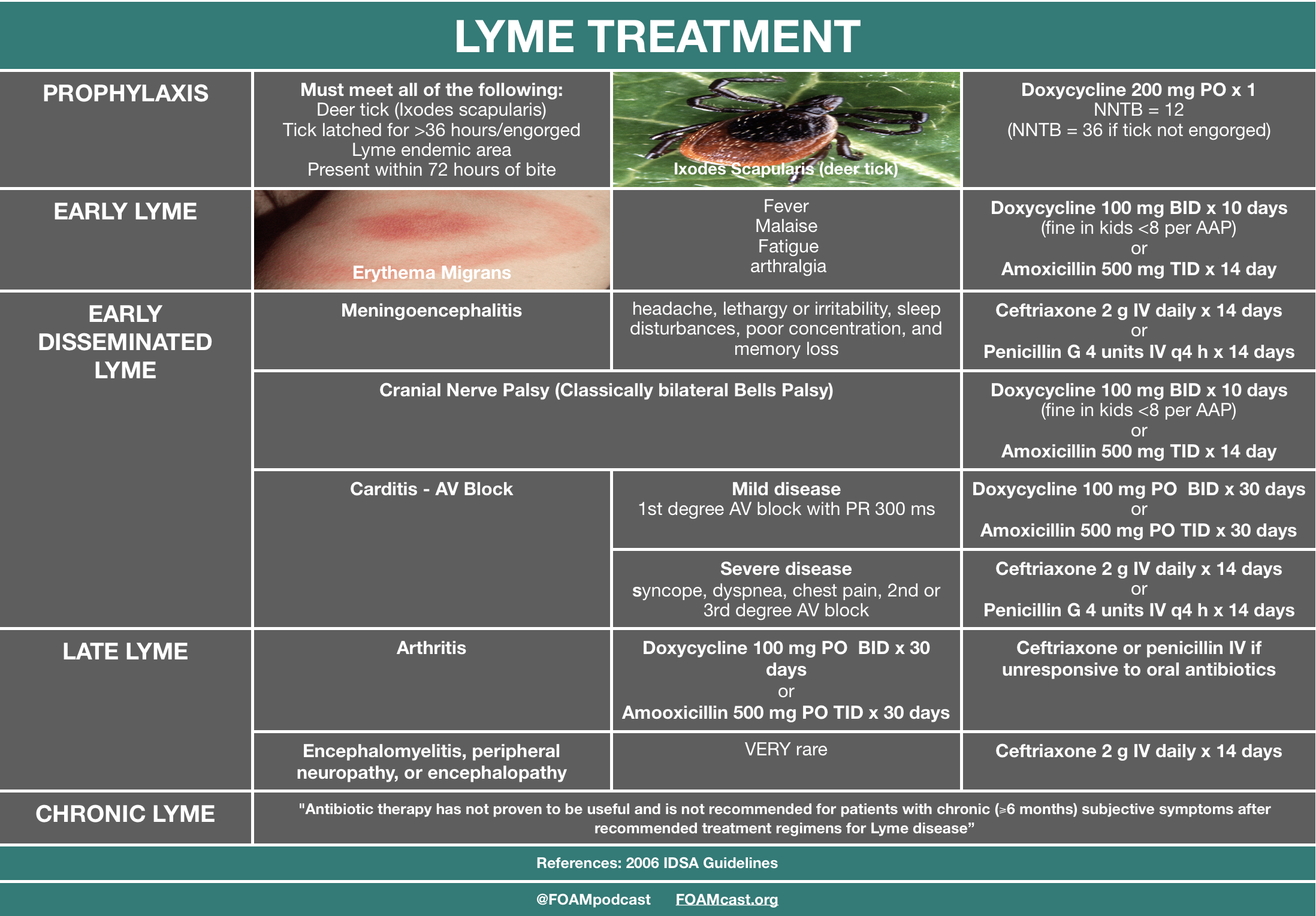
Lyme disease is categorized into three stages:
- Localized: Occurs within several days of the tick bite. Symptoms include redness and irritation at the site of the tick bite, along with flu-like symptoms such as fever, chills, and muscle aches.
- Disseminated: Occurs within weeks of a tick bite. If untreated, the infection spreads to other parts of the body and new symptoms occur.
- Persistent: Late infection, may occur within months to years after the initial tick bite. Arthritis and neurological symptoms are common in this stage.
Don’t Miss: What Tick Has Lyme Disease
Controversy : Significance Of Persistent Lyme Disease
While characterized by some as the aches and pains of daily living, there is growing recognition of the potential significance of persistent Lyme disease. Evidence from 4 National Institutes of Health -sponsored retreatment trials, well-conducted patient surveys, and a large medical claims database demonstrates that the physical, social, and economic costs of persistent Lyme disease for individuals can be substantial and are an economic burden for the country as a whole.,
A retrospective study using an expansive medical insurance claims database identified 52 795 individuals diagnosed and treated for Lyme disease who met the study’s strict criteria. Comparing health care costs within this group, total costs over a 12-month posttreatment period were $3800 higher for patients who had 1 or more posttreatment Lyme disease symptoms than for those who had none. The magnitude of the sample size and conservative study design make the findings particularly compelling.
Taken together, the trial, survey, and database evidence clearly identify that the health and financial costs associated with persistent Lyme disease are significant and should not be casually dismissed.
What Do I Do If I Find A Tick On My Skin
Dont panic. Use fine-tipped tweezers to grasp the tick as close to the skins surface as possible. Pull up with steady, even pressure. Be careful not to squeeze or twist the tick body. Sometimes parts of the tick remain in the skin. You can leave them alone or carefully remove them the same way you would a splinter. Do not use heat , petroleum jelly, or other methods to try to make the tick back out on its own. These methods are not effective.
Wash the area where the tick was attached thoroughly with soap and water. Keep an eye on the area for a few weeks and note any changes. Call your doctor if you develop a rash around the area where the tick was attached. Be sure to tell your doctor that you were bitten by a tick and when it happened.
Recommended Reading: Symptoms Of Lyme Disease In Dogs
What Is Chronic Lyme Disease
Lyme disease is an infection caused by the bacterium Borrelia burgdorferi. In the majority of cases, it is successfully treated with oral antibiotics. In some patients, symptoms, such as fatigue, pain and joint and muscle aches, persist even after treatment, a condition termed Post Treatment Lyme Disease Syndrome .
The term chronic Lyme disease has been used to describe people with different illnesses. While the term is sometimes used to describe illness in patients with Lyme disease, it has also been used to describe symptoms in people who have no clinical or diagnostic evidence of a current or past infection with B. burgdorferi . Because of the confusion in how the term CLD is employed, and the lack of a clearly defined clinical definition, many experts in this field do not support its use.
Late Or Chronic Lyme Disease Treatment
Experts agree that the earlier you are treated the better, since early treatment is often successful. Unfortunately, a substantial portion of patients treated with short-term antibiotics continue to have significant symptoms. The quality of life of patients with chronic Lyme disease is similar to that of patients with congestive heart failure. Doctors dont agree about the cause of these ongoing symptoms. The primary cause of this debate is flawed diagnostic testing. There is currently no test that can determine whether a patient has active infection or whether the infection has been eradicated by treatment.
The IDSA thinks Lyme disease symptoms after treatment represent a possibly autoimmune, post-Lyme syndrome that is not responsive to antibiotics. The IDSA essentially regards Lyme disease as an acute infection like strep throat that can be treated with a short course of antibiotics. The IDSA guidelines are now eight years old and do not reflect recent science.
ILADS physicians believe that ongoing symptoms probably reflect active infection, which should be treated until the symptoms have resolved. These physicians use treatment approaches employed for persistent infections like tuberculosis, including a combination of drugs and longer treatment durations. The ILADS guidelines have just recently been updated using a rigorous review of the medical literature.
You May Like: Beach House Rentals Old Lyme Ct
What Are The Signs And Symptoms Of Stage 3 Lyme Disease
Late or chronic Lyme disease refers to manifestations that occur months to years after the initial infection, sometimes after a period of latency. Signs and symptoms of chronic Lyme disease are primarily rheumatologic and neurologic. Acrodermatitis chronica atrophicans, the cutaneous feature of late-stage Lyme disease, is found almost exclusively in European patients.
Most patients presenting with late disease do not have a history of erythema migrans, because the rash typically leads to earlier treatment, which prevents the development of late disease. However, other manifestations of the disease may coexist or may have occurred in the past. Thus, a history of Bell palsy, aseptic meningitis, arthritis, acral paresthesias or dysesthesias , or cognitive dysfunction may be diagnostically useful.
Maladaptive host responses can lead to a variety of syndromes in stage 3, as follows :
- Postinfectious Lyme arthritis Massive inflammatory synovial proliferation, usually in a knee
- Posttreatment Lyme disease syndrome Pain, neurocognitive impairment, fatigue
- Autoimmune joint disease Rheumatoid arthritis, psoriatic arthritis, or peripheral spondyloarthropathy
- Autoimmune neurologic disease Chronic idiopathic demyelinating polyneuropathy
Lyme arthritis is the hallmark of stage 3 Lyme disease. It tends to involve large joints . Arthritis must be differentiated from arthralgia, which is common in early disease.
References
Symptoms Of Post Treatment Lyme Disease
- Include severe fatigue, musculoskeletal pain, & cognitive problems
- Can significantly impact patients health and quality of life
- Can be debilitating and prolonged
Our research indicates the chronic symptom burden related to PTLD is significant. Although often invisible to others, the negative impact on quality of life and daily functioning is substantial for PTLD sufferers.
The chronic symptom burden related to Lyme disease is considerable, as shown on the left side of the graph above, and statistically significantly greater than the aches and pains of daily living experienced by the control group, on the right.
Also Check: Post Treatment Lyme Disease Syndrome Treatment
What Is Late Lyme Disease
Lyme disease, also known as Lyme borreliosis, is caused by an infection with the bacteria Borrelia burgdorferi. This bacteria is disseminated through tick bites. Infected ticks usually bite small mammals, who do not develop any kind of infection from the bacteria. When humans are exposed to B. Burgdorferi from a tick bite, however, they can develop Lyme disease.
People who work outside or spend time in woodland areas, where there is greater potential for exposure to tick bites, are most at risk of infection.
Lyme disease is a condition which progresses in stages:
Treatment For Other Forms Of Lyme Disease
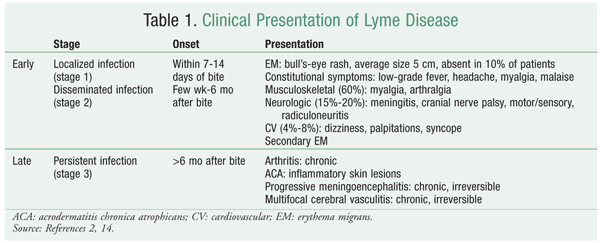
People with other forms of disseminated Lyme disease may require longer courses of antibiotics or intravenous treatment with antibiotics such as ceftriaxone. For more information about treating other forms of Lyme disease, see:
The National Institutes of Health has funded several studies on the treatment of Lyme disease that show most people recover within a few weeks of completing a course of oral antibiotics when treated soon after symptom onset. In a small percentage of cases, symptoms such as fatigue and myalgia can last for more than 6 months. This condition is known as post-treatment Lyme disease syndrome , although it is also sometimes called chronic Lyme disease. For details on research into chronic Lyme disease and long-term treatment trials sponsored by NIH, visit the visit the National Institutes of Health Lyme Disease web siteexternal icon.
You May Like: Does Lyme Disease Have A Cure
What Is The Treatment For Lyme Disease
The first-line standard of care treatment for adults with Lyme disease is doxycycline, a tetracycline antibiotic. Other antibiotics that have activity against borrelia include the penicillin-like antibiotic, amoxicillin, and the second generation cephalosporin, Ceftin. The mainstay of treatment is with oral antibiotics, but intravenous antibiotics are sometimes indicated for more difficult to treat cases of neurologic-Lyme disease, such as meningitis, and cases of late Lyme arthritis.
How Is Lyme Disease Treated
For early Lyme disease, a short course of oral antibiotics such as doxycycline or amoxicillin is curative in the majority of the cases. In more complicated cases, Lyme disease can usually be successfully treated with three to four weeks of antibiotic therapy.
In patients who have non-specific symptoms after being treated for Lyme disease and who have no evidence of active infection , studies have shown that more antibiotic therapy is not helpful and can be dangerous.
Recommended Reading: How Do You Get A Tick Tested For Lyme Disease
What Is Post Treatment Lyme Disease
Post Treatment Lyme Disease represents a research subset of patients who remain significantly ill 6 months or more following standard antibiotic therapy for Lyme disease. PTLD is characterized by a constellation of symptoms that includes severe fatigue, musculoskeletal pain, sleep disturbance, depression, and cognitive problems such as difficulty with short-term memory, speed of thinking, or multi-tasking. In the absence of a direct diagnostic biomarker blood test, PTLD has been difficult to define by physicians, and its existence has been controversial. However, our clinical research shows that meticulous patient evaluation when used alongside appropriate diagnostic testing can reliably identify patients with a history of previously treated Lyme disease who display the typical symptom patterns of PTLD.
Early Lyme Disease Treatment
ILADS doctors are likely to recommend more aggressive and longer antibiotic treatment for patients. They may, for instance, treat high risk tick bites where the tick came from an endemic area, was attached a long time, and was removed improperly. They may treat a Lyme rash for a longer period of time than the IDSA recommends, to ensure that the disease does not progress. They are unlikely to withhold treatment pending laboratory test results.
You May Like: Does Lyme Disease Stay With You Forever
Why Are Antibiotics The First Line Of Treatment For Lyme Disease
The use of antibiotics is critical for treating Lyme disease. Without antibiotic treatment, the Lyme disease causing bacteria can evade the host immune system, disseminate through the blood stream, and persist in the body. Antibiotics go into the bacteria preferentially and either stop the multiplication of the bacteria or disrupt the cell wall of the bacteria and kill the bacteria . By stopping the growth or killing the bacteria the human host immune response is given a leg up to eradicate the residual infection. Without antibiotics, the infection in Lyme disease can evade the host immune system and more readily persist.
Stage : Early Localized Disease
Symptoms of Lyme disease usually start 1 to 2 weeks after the tick bite. One of the earliest signs of the disease is a bulls-eye rash.
The rash occurs at the site of the tick bite, usually, but not always, as a central red spot surrounded by a clear spot with an area of redness at the edge. It may be warm to the touch, but it isnt painful and doesnt itch. This rash will gradually fade in most people.
The formal name for this rash is erythema migrans. Erythema migrans is said to be characteristic of Lyme disease. However, many people dont have this symptom.
Some people have a rash thats solid red, while people with dark complexions may have a rash that resembles a bruise.
The rash can occur with or without systemic viral or flu-like symptoms.
Other symptoms commonly seen in this stage of Lyme disease include:
Also Check: Whats Lyme Disease In Humans