The Chance Of Getting Lyme Disease
Not all ticks in England carry the bacteria that causes Lyme disease.
But it’s still important to be aware of ticks and to safely remove them as soon as possible, just in case.
Ticks that may cause Lyme disease are found all over the UK, but high-risk places include grassy and wooded areas in southern and northern England and the Scottish Highlands.
Ticks are tiny spider-like creatures that live in woods, areas with long grass, and sometimes in urban parks and gardens. They’re found all over the UK.
Ticks do not jump or fly. They attach to the skin of animals or humans that brush past them.
Once a tick bites into the skin, it feeds on blood for a few days before dropping off.
Amy Schumer Reveals Lyme Disease Diagnosis
The new three-dose vaccine is now entering phase 3 clinical trials, for which the company will enroll 6,000 participants from around the world, including children age 5 and up. After the initial doses, people may need an annual shot, as well, Torres said. “So it’s a bit more complicated than most vaccines, but certainly will protect against something that can be fairly dangerous.”
If the trial is successful, Pfizer and French biotech company Valneva could apply for approval from the U.S. Food and Drug Administration and the European Medicines Agency as soon as 2025, according to a press release.
And if this all sounds a little familiar, it might be because the FDA previously approved a vaccine for Lyme disease in 1998. But there wasn’t enough demand for the vaccine at the time, so the manufacturer withdrew it from the market just a few years later.
“Now we see Lyme disease cropping up and occurring more across the country,” Torres said, so there is likely to be more interest in a vaccine than there was in the past.
A recent study estimated that more than 14% of the world’s population have had Lyme disease.
Ticks Are Back Dartmouth Health Gives Tips To Stay Safe From Lyme Disease
- May 25, 2022
LEBANON While a mild winter in northern New England can seem like a good thing at the time, it often has the unfortunate side effect of ticks returning earlier than usual. Its not even June and residents of New Hampshire and Vermont are already seeing deer ticks which carry the bacteria which causes Lyme disease in the wild, in their pets fur and on themselves.
A tick doesnt hurt when it bites, and deer ticks are so tiny that they can go unnoticed on the body until they become engorged, or not at all unless the host develops Lyme symptoms.
The classic Lyme disease symptom is an expanding, flat rash that often looks like a bullseye, said Jeffrey Parsonnet, M.D., a physician in infectious disease and international health at Dartmouth Healths academic medical center, Dartmouth Hitchcock Medical Center and Dartmouth Hitchcock Clinics.
Other symptoms are flu-like aches, stiffness, fatigue and might develop five to seven days after receiving a bite. More advanced disease might cause swollen joints, infection of nerves responsible for heart rhythm regulation or neurologic disorders like Bells Palsy , pain in limbs or, rarely, brain infection.
While Lyme disease can be very serious, it can be prevented and treated. Parsonnet offers the following tips for keeping ticks at bay so you and your family can enjoy New Englands beautiful summer season.
You May Like: What Percentage Of Ticks Carry Lyme Disease
Biology And Management Of Ticks In New Hampshire
There are two families of ticks, the Ixodidae and Argasidae . Those of importance to hikers, campers, and pet owners are in the family Ixodidae. Therefore, this publication covers species of that group. Several species are important because they bite people and/or pets.
Some can also transmit diseases to the people or pets they bite.
This publication will help you learn what ticks look like, how they live, the diseases they spread, how to manage tick problems, and how to protect yourself from tick-borne diseases.
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Read Also: Justin Bieber Lyme Disease Treatment
Pesticides Used For Tick Control
Carbamates – Carbaryl is a broad spectrum insecticide which controls ticks well. Broad-spectrum means that it kills a very wide range of insects, including many beneficial species. Outdoors, the sunlight, oxygen and moisture work to break down the chemical relatively quickly. Residues typically kill pest insects for 5 to 10 days after spraying. Carbaryl is incorporated into some tick collars, plus some sprays sold for use around homes. It is very toxic to bees and many other beneficial insects, and moderately toxic to mammals.
Propoxur is another carbamate chemical that controls fewer kinds of insects . It is in some tick collars, and is highly toxic to mammals, so is used at low concentrations.
Formamidines – Amitraz is the only current tick-registered chemical in this group. It is in some tick collars for pets. It is a somewhat narrow spectrum material, effective on mites, ticks, and some insects. It has slight toxicity to people.
Insect Growth Regulators – These are relatively new chemicals. They interfere with the hormones that control insect development, which are quite different from human hormones. Immature stages of insects are vulnerable, but adults are not. These chemicals generally have very low risk of mammalian toxicity. Pyriproxifen and s-methoprene are in this group, and are in some flea & tick collars, and some indoor treatments. Both have low toxicity to people and other mammals. Methoprene is not very effective on ticks, but does kill fleas.
Testing Commonly Done With Our Patient During First Visit:
- Tick-borne disease antibody testing
- Chronic sinus and respiratory infections reducing immunity
- Viral infections stressing immunity and causing symptoms
- Hormone testing as needed
- Inflammation markers associated with tissue destruction associated with autoimmune disease. Patients can often have simultaneous infection and autoimmune process triggered.
- Other tests are ordered based on what is most clinically significant such as heavy metals, mold biotoxins, food intolerances
Our goal is to be proactive using treatments best suited for the patient. We dont claim to cure the infections, but the goal is to get patient to optimal health and improved function. We are trying to work ourselves out of a job by getting a patient through the process as efficiently as possible. We also understand these complex illnesses deserve patience and time. The goal is to treat the infection but also the body having the immune response to the microbe. We find that if you build the body up, you will get the best results in the clinic with an integrative approach. We focus on treatments which are anti-inflammatory, detoxifying, anti-microbial, and body balancing.
Read Also: How Do You Treat Lyme Disease In Dogs
Tick Bites Increasing In New Hampshire Health Officials Say
Mike Cherry, News Anchor/Reporter WMUR
Manchester, NH Health officials are warning that emergency department visits for tick bites in New Hampshire have been increasing since mid-March.
According to the Centers for Disease Control and Prevention, the Northeast leads the nation in the rate of tick bites.
Currently, the region averages 103 bites per 100,000 emergency department visits 10 times the central region of the country.
Were seeing a gamut of patients coming in with various stages of tick bites somewhere the ticks are still embedded, said Dr. James Martin, Medical Director at Urgent Care at Milford Medical Center.
New Hampshire is a prime location for deer ticks, which carry Lyme disease and results in a wide range of symptoms.
We have occasional patients who are actually ill from their tick bites, and they have headaches and fevers and maybe the rash, muscle aches and that type of thing, said.
Some Granite Staters said they are being extra cautious this year.
It seems to be getting progressively worse every single year, just little by little bit, but so far, its been good, resident Donna Barton said. The kids havent had Lyme or anything like that. But were definitely watching more whenever we go out in the woods. I wear long pants, long sleeves, that kind of thing.
If you find a tick on your skin, dont panic.
You can find resources on how to protect yourself on the CDC website or the Tick Free New Hampshire website.
Symptoms Of Lyme Disease
A circular or oval shape rash around a tick bite can be an early symptom of Lyme disease in some people.
The rash can appear up to 3 months after being bitten by an infected tick, but usually appears within 1 to 4 weeks. It can last for several weeks.
The rash can have a darker or lighter area in the centre and might gradually spread. It’s not usually hot or itchy.
The rash may be flat, or slightly raised, and look pink, red, or purple when it appears on white skin. It can be harder to see the rash on brown and black skin and it may look like a bruise.
Some people also get flu-like symptoms a few days or weeks after they were bitten by an infected tick, such as:
- a high temperature, or feeling hot and shivery
- headache
- tiredness and loss of energy
Some people with Lyme disease develop more severe symptoms months or years later.
This is more likely if treatment is delayed.
These more severe symptoms may include:
- pain and swelling in joints
- nerve problems such as pain or numbness
- heart problems
- trouble with memory or concentration
Recommended Reading: Can You Cure Lyme Disease Naturally
Some Tick Species Can Cause Multiple Illnesses
The black-legged tick may be known for spreading Lyme disease, but it can also transmit bacteria and viruses that cause other illnesses.
The most common of these secondary infections is anaplasmosis, a flu-like illness that is reported at rates as high as 500 cases per million people in Maine under half of the state’s incidence of Lyme disease, but greater than most states’ rates of RMSF.
Massachusetts used to be a high-incidence Lyme state like its neighbors, but the number of reported cases of Lyme disease in the state dropped drastically in 2016. In the meantime, the rate of anaplasmosis in the state has surpassed that of Lyme: same tick, different bacteria.
Ehrlichiosis, another lesser-known tick-borne illness, is spread by the lone star tick in the Southern and central US. In Missouri, the annual rate of ehrlichiosis is almost as high as the rate of RMSF. The disease has been reported as far west as Nebraska, but most cases occur in the eastern half of the country.
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Don’t Miss: How Do I Know If A Tick Has Lyme Disease
Signs Of Undiagnosed Lyme Disease
In the first 30 days, if you have Lyme Disease, possible symptoms include fever, chills, muscle and joint aches, swollen lymph nodes, fatigue, rash, and headache. You may or may not see the bullseye rash associated with Lyme Disease.
Lyme Disease blood tests are only 29-40% accurate in the first three weeks of infections. The CDC also says that tests are not likely to be positive for up to 4-6 weeks after infection, so it can be misdiagnosed. Often the medical provider will prescribe an antibiotic as a preventative if Lyme Disease is suspected. It’s a tricky disease, and can be very painful.
My own bout with Lyme Disease was very painful in my joints, after being undetected for weeks. Avoid the misery by taking the right precautions regularly and doing daily tick checks.
Could A Vaccine Help With Persistent Lyme Symptoms
For now, the clinical trials will just recruit people who’ve never had Lyme disease. But Torres said the vaccine may one day also be helpful for those dealing with persistent Lyme disease symptoms after a previous infection.
The idea is similar to what researchers are beginning to learn about using COVID-19 vaccines to treat persistent symptoms of long COVID, Torres said. For instance, he pointed to a study published in May in BMJ, which found that people who received a COVID-19 vaccine after testing positive were less likely to develop long COVID.
Experts are still investigating the biological reasons why long COVID happens and why a vaccine dose might help. One theory is that long COVID is a type of autoimmune response, in which the body’s immune system begins attacking its own healthy cells, Torres said. In that case, theoretically, “the vaccine helps the immune system fine-tune itself and target the germ it’s going after,” he said.
Another theory is that the virus is hidden away and “lingering” in a part of the body, Torres said. That can cause the symptoms to pop up every now and then, and a vaccine could help get them under control.
Of course, COVID-19 and Lyme disease are two different illnesses, but seeing this promising development with the COVID-19 vaccines points to a possible role for this new vaccine in treating long-term Lyme symptoms down the line.
Related:
You May Like: Muscle Testing For Lyme Disease
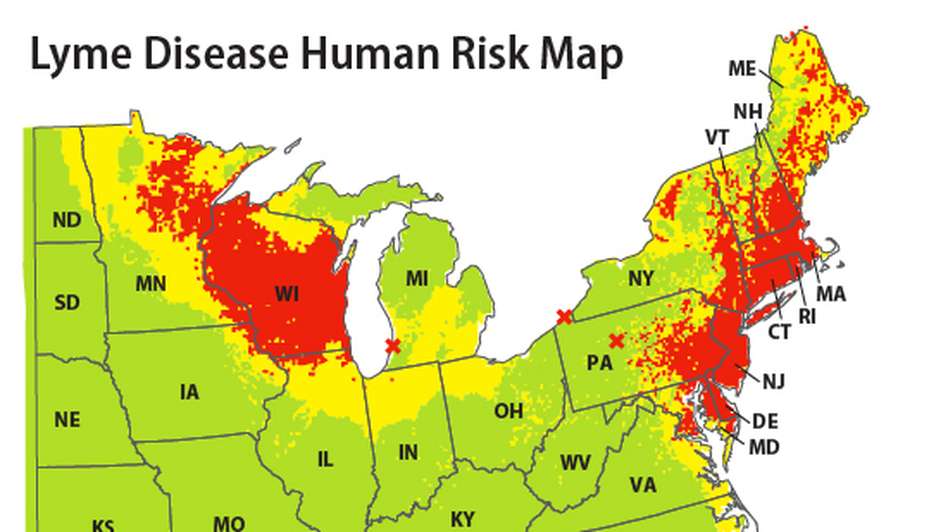
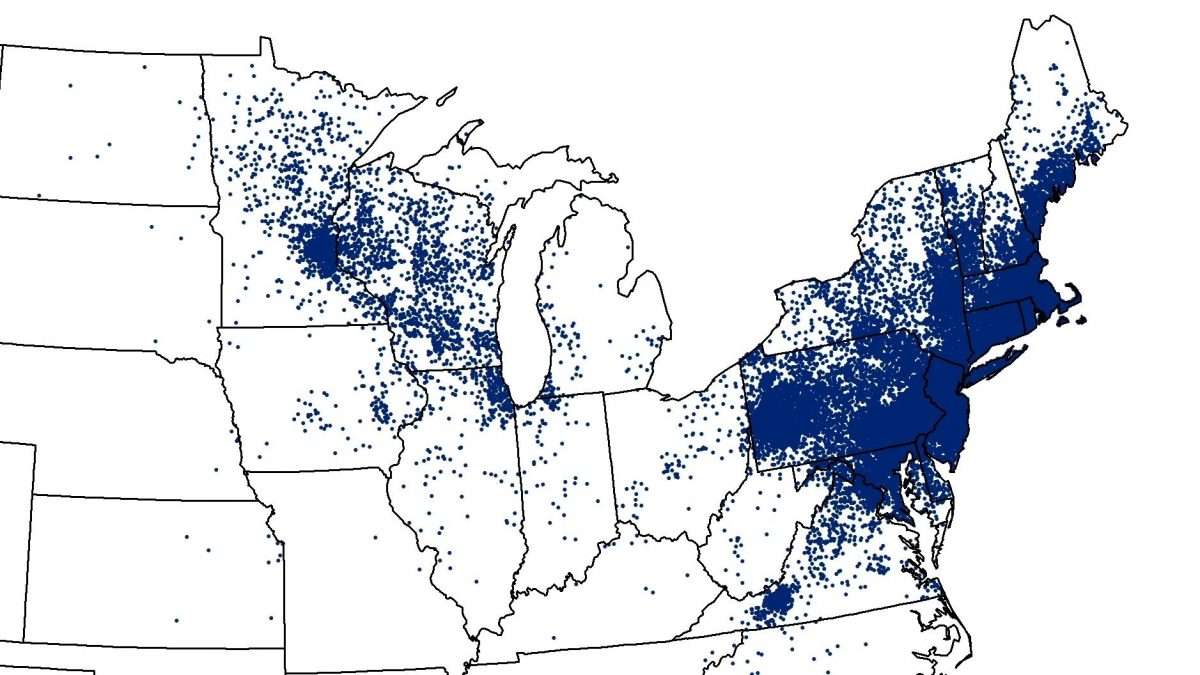
How Prevalent Is Lyme Disease Where You Live Find Out With This Interactive Map
Rashes. Fatigue. Swollen joints.
These are not the ingredients for a happy summer day. But they are the most common symptoms of Lyme disease, a tick-borne illness transmitted by deer ticks that have been infected with the bacteria Borrelia burgdorferi.
Mosquito, flea, and tick-borne illnesses in the United States tripled from 2004 to 2016, according to a new report from the Centers for Disease Control and Prevention. Massachusetts is one of the 14 states where, according to CDC, 95 percent of Lyme disease cases were reported in 2015. Experts estimate that 87,000 people per year in Massachusetts are infected with the bacteria Borrelia burgdorferi, which causes Lyme disease.
Thanks to increasing urban and suburban sprawl, forests are being parceled into smaller pockets of vegetation, said Northeastern University Distinguished Professor of Biology Kim Lewis, who directs Northeasterns Antimicrobial Discovery Center. Parks and backyards in the suburbs are now the perfect size to sustain mice, but not quite large enough to sustain foxes. That means mice can run rampant with no natural predators to keep their population at bay. And with mice, come ticks.
The sprawling of suburbia is a fairly recent phenomenon, Lewis said. You get more hosts for the ticks, and of course, you get more ticks.
As the clock ticks closer to summer and the height of tick season approaches, check out our interactive map to see the prevalence of Lyme disease in your state.
Lyme Disease Data Tables: Historical Data
| State |
|---|
| confirmed cases presented for all years except most recent*confirmed cases per 100,000 populationN = not notifiable |
| State |
|---|
| 7.8 |
| *incidence=confirmed cases per 100,000 personsHigh Incidence=average incidence of at least 10 confirmed cases per 100,000 for three reporting yearsN= not notifiableNote: Many high incidence states have modified surveillance practices. Contact your state health department for more information. |
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination website’s privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
Don’t Miss: Dr Gregory Bach Lyme Disease
Safe Removal Of Ticks
Since tick bites are painless, ticks are often discovered after they have begun to feed. Removal is fairly easy, provided it is done correctly. We recommend using tweezers to grasp the tick, rather than using bare fingers. Using bare fingers may contaminate them with a disease-causing organism.
Also, it is easier to get a firm grip of the head with tweezers. Firmly grasp the tick as close to its head as possible, and pull gently, using slow, steady pressure. DO NOT yank it or pull it sideways, since this could cause its head to break off inside the wound. It might take as long as a minute or two for removal. Some people find it easier to use a plastic tick spoon, called Ticked Off . You slide the spoon under the attached tick, fitting its mouthparts into the v-shaped notch. Then hold the body of the tick down with your thumb, and gently roll the handle of the spoon down, using leverage to pull the tick out. Be careful to fit the mouthparts into the smallest part of the notch, and do this as close to the skin as possible.
Touching a hot match to an embedded tick, or covering it with Vaseline or other substances arent recommended. They do not help to remove the tick, and we worry that they might increase the likelihood of the tick regurgitating into the host . Check to be sure the head comes out, rather than breaking off. The photographs should help determine if all of the head has come out. It may be wise to apply an antiseptic to the wound after removing the tick.