Asian Artist Assaulted On Opening Night Of The Chinese Lady’ At Nyc Theater
There is no credible scientific evidence that Lyme disease is spread through sexual contact. Published studies in animals do not support sexual transmission , and the biology of the Lyme disease spirochete is not compatible this route of exposure . The ticks that transmit Lyme disease are very small and easily overlooked. Consequently, it is possible for sexual partners living in the same household to both become infected through tick bites, even if one or both partners doesnt remember being bitten.
Can Lyme disease be transmitted through breast milk?
There are no reports of Lyme disease being spread to infants through breast milk. If you are diagnosed with Lyme disease and are also breastfeeding, make sure that your doctor knows this so that he or she can prescribe an antibiotic thats safe for use when breastfeeding.
Can Lyme disease be transmitted during a blood transfusion?
Although no cases of Lyme disease have been linked to blood transfusion, scientists have found that the Lyme disease bacteria can live in blood from a person with an active infection that is stored for donation. Individuals being treated for Lyme disease with an antibiotic should not donate blood. Individuals who have completed antibiotic treatment for Lyme disease may be considered as potential blood donors. The Red Cross provides additional information on the most recent criteria for blood donation.
Is it true that you can get Lyme disease anywhere in the U.S.?
DIAGNOSIS, TESTING, AND TREATMENT
How Do You Know If Your Lyme Disease Is Treated And Finished
Patients ask me this question all the time. We diagnose the disease, we treat with antibiotics, or herbs, or homeopathics. We feel better. We stop the treatment. And either we continue to feel better, or we relapse and have to start all over again.
Is there no way to test whether the spirochete is gone?
The Lyme disease.org website has an excellent article ondiagnosis of Lyme disease.
The National Geographic website has a good description of the deer tick, and thehistory of Lyme disease.
Standard Lyme testing includes the following:
- ELISA or IFA test
- If that test is positive, then a Western Blot test is run
- If 5 out of the 10 possible Lyme bands are positive, you are diagnosed with Lyme disease
- If fewer than 5 of the 10 possible bands are positive, you are diagnosed as negative.
Not all the bands which appear on a Western blot are specific to Lyme disease even though one ofthose non-specific bands is required by the CDC for diagnosis.
Two of the bands which are specific to Lyme disease are not on the CDC list of bands required to be positive.
How much sense does that make?
For more detailed information about the IFA and Western blot testing, check out theIGeneX website.
There is another test that can give us an idea whether the Lyme disease is actually gone out of our systems. This is an inflammatory marker, so it tells us whether there is continued inflammation or whether that inflammation is no longer present.
Bottom line:
Key Points To Remember
- Most Lyme disease tests are designed to detect antibodies made by the body in response to infection.
- Antibodies can take several weeks to develop, so patients may test negative if infected only recently.
- Antibodies normally persist in the blood for months or even years after the infection is gone therefore, the test cannot be used to determine cure.
- Infection with other diseases, including some tickborne diseases, or some viral, bacterial, or autoimmune diseases, can result in false positive test results.
- Some tests give results for two types of antibody, IgM and IgG. Positive IgM results should be disregarded if the patient has been ill for more than 30 days.
Don’t Miss: What To Do If I Have Lyme Disease
Alternative Diagnostic Tests Not Available At Ripl
Tests used in the NHS and PHE to identify Lyme disease are well characterised, standardised, and are highly reproducible between laboratories. They are the methods of choice recommended in the 2018 NICE Lyme disease guideline, following an extensive review of the evidence and literature. International external quality assurance schemes are in place to ensure consistency between different centres offering these tests.
Several private laboratories in Europe and the USA offer an alternative type of test called an ELISpot to diagnose Lyme disease. This looks for different markers in blood samples compared to conventional validated Lyme disease serology tests. The laboratories using these tests in the diagnosis of Lyme disease do not publish their methods, and have not produced any peer reviewed publications on their clinical value.
This makes it very difficult to verify their results, especially as there are no national or international EQA schemes for Lyme disease ELISpot tests and therefore no independent verification of performance between laboratories. Without independent evidence it is impossible to determine the validity of results produced using these alternative tests.
RIPL cannot interpret the results of alternative diagnostic tests.
How Can I Tell If Treatment Is Working
If joint lameness is the presenting sign, improvement may be noted after 3-5 days starting antibiotics. A dog’s response to therapy can be assessed by repeating the QC6 test six months after treatment is complete. Dogs that start with a moderate to high QC6 value typically show a 50% reduction or more in the QC6 at six months, indicating that treatment has been successful. Dogs that have a lower initial QC6 value may not show such dramatic reductions in the QC6 at six months, although the value should still be lower than the starting point if treatment has been successful.
A persistently high QC6 suggests treatment may not have been complete or that the dog became reinfected after treatment was stopped.
Also Check: Where To Buy Lyme Vaccine For Dogs
How To Determine Where You Are
In my clinical experience, the best predictor of when treatment is done, or where you are in your treatment for Lyme or the coinfections is to follow the symptoms. If testing is negative, but you still have a lot of symptoms, then there is a good possibility, the germs are still active and require further treatment. For more information about how to determine to stop treatment see Finished? And How to Prevent Relapse.
Serological Testing Of Serum For The Diagnosis Of Lyme Disease
The most commonly used tests look for antibodies to the Borrelia species that cause Lyme disease in the UK and Europe, but they also detect infections from strains of Borrelia from the US.
The antibody response takes several weeks to reach a detectable level, so antibody tests in the first few weeks of infection may be negative. If the first sample was taken within 4 weeks from the start of symptoms and is negative and there is a clinical suspicion of Lyme disease, then retesting in 4 to 6 weeks may be useful.
It is very rare for patients to have negative antibody tests in longstanding infections. Borrelia antibodies persist indefinitely in some patients and this does not indicate continuing disease or a need for re-treatment.
Serological testing for Lyme disease in the UK and much of the world follows a two-step approach using commonly available antibody screening tests as a first stage, followed by immuno-blotting of samples that give positive or indeterminate results in the screening tests.
Sensitive screening tests are used at the first stage of testing but have the disadvantage of occasionally detecting other diseases and producing false positive results. RIPL uses the C6 Lyme ELISA for screening
Samples giving positive or indeterminate preliminary screening test results are then tested in a more specific system to confirm the presence of Borrelia-specific antibodies. RIPL uses the Borrelia ViraChip® IgG, IgM test for this purpose
Read Also: Essential Oils For Lyme Disease
Your Test Was Not Sensitive Enough
Many doctors and labs adhere diligently to the two-step tests for Lyme disease approved by the FDA and recommended by the CDC, which involves an initial enzyme-linked immunosorbent assay followed by a Western blot test. Both tests are designed to detect antibodies in the patients blood to the B. burgdorferi bacteria. According to the CDC, both must be positive for a patient to be diagnosed with Lyme disease.
However, recent studies have raised concerns about the Lyme disease test accuracy, particularly the ELISA, which has been found to have a poor sensitivity rate, or ability to detect antibodies in the blood. Recent studies, in fact, report that the ELISA and Western blot can miss up to 60 percent of well-defined Lyme disease cases.
The Chance Of Getting Lyme Disease
Not all ticks in England carry the bacteria that causes Lyme disease.
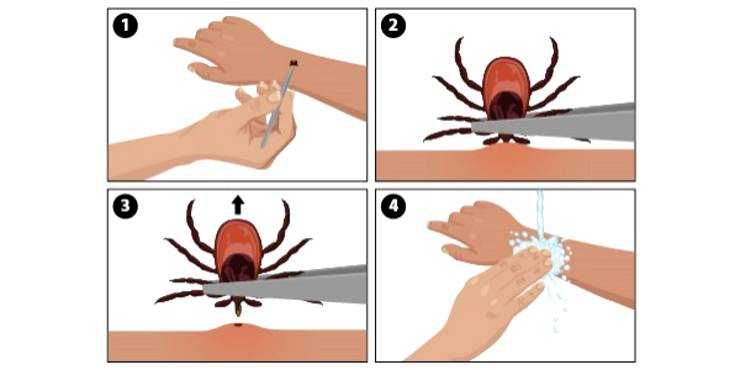
But it’s still important to be aware of ticks and to safely remove them as soon as possible, just in case.
Ticks that may cause Lyme disease are found all over the UK, but high-risk places include grassy and wooded areas in southern and northern England and the Scottish Highlands.
Ticks are tiny spider-like creatures that live in woods, areas with long grass, and sometimes in urban parks and gardens. They’re found all over the UK.
Ticks do not jump or fly. They attach to the skin of animals or humans that brush past them.
Once a tick bites into the skin, it feeds on blood for a few days before dropping off.
Recommended Reading: How To Treat Chronic Lyme
Can We Test Fluids Other Than Serum
Yes, CSF samples can be submitted from horses with neurological signs. The CSF sample needs to be submitted together with a serum sample from the same animal and taken at the same time. The relative increase of antibodies in CSF can indicate local production of antibodies in the CNS. Typically, one or two antibody values are increased more than 2-fold if B. burgdorferi contributes to the neurologic condition.
For other samples, contact the lab first .
Is It Possible For Lyme Disease To Be Misdiagnosed As Amyotrophic Lateral Sclerosis Are There Similarities In Symptoms Between These Two Diseases
The question of a relationship between Lyme Disease and ALS first received significant academic attention when Dr. John Halperin who was then a neurologist at Stony Brook conducted a study in which he compared the frequency of blood test positivity to the agent of Lyme disease among patients with ALS to community controls. The results indicated a higher percentage of the ALS patients were seropositive for Lyme Disease. Since then, there have been isolated case reports both in the media and one or two in the academic literature indicating that a patient had been misdiagnosed with an ALS-like illness only later to be re-diagnosed and treated for Lyme disease with good clinical response. Although we suspect that there may be rare individuals who have symptoms similar to ALS but actually have proximal motor neuropathy caused by Lyme disease, the vast majority of patients with ALS are not thought to have Lyme disease as the cause of their serious disease. Clinical trials have been underway using antibiotics for ALS not because there is belief that ALS is caused by a microbe but because these antimicrobial agents have other properties as well, such as decreasing inflammation or decreasing glutamatergic excitotoxicity. The studies examining intravenous ceftriaxone as a treatment for ALS were not successful.
You May Like: What Are The Long Term Symptoms Of Lyme Disease
What Is The Treatment For Lyme Disease
The first-line standard of care treatment for adults with Lyme disease is doxycycline, a tetracycline antibiotic. Other antibiotics that have activity against borrelia include the penicillin-like antibiotic, amoxicillin, and the second generation cephalosporin, Ceftin. The mainstay of treatment is with oral antibiotics, but intravenous antibiotics are sometimes indicated for more difficult to treat cases of neurologic-Lyme disease, such as meningitis, and cases of late Lyme arthritis.
Lyme Disease And Other Tick Borne Illnesses
Ticks carry a number of diseases, most notably Lyme Disease. They can create significant health risks for humans and companion animals.
What diseases can ticks transmit?
Ticks can transmit a number of diseases including:
- Anaplasmosis
- Bourbon Virus
Which ticks transmit diseases? Any tick can transmit diseases, but certain diseases are linked with certain ticks. All of the above illnesses are associated with ticks that are present in New Jersey.
What is Lyme Disease? Lyme Disease is the most common tick borne illness in the United States. It is transmitted by the deer tick. A tick has to be present on the skin for at least about 48 hours to transmit the infection, so detection and removal of ticks is important in prevention.
How is Lyme disease treated? Lyme disease can be treated with antibiotics. First-line treatments include doxycycline, amoxicillin, or cefuroxime for adults and children. Sometimes IV antibiotics are used if the Lyme disease is impacting the heart or brain. Once a patient is showing improvement, they may be switched from IV to oral antibiotics. The treatment is 7 to 14 days. If a patient has developed Lyme arthritis, which can be a late-stage symptom of Lyme disease, they may have a longer course of oral antibiotics.
What are signs of tick borne illnesses?
Signs and symptoms of tick borne illnesses vary with the illness and can show up 7 to 21 days after exposure. They include:
- Red spots
- Altered Mental State
Don’t Miss: What Is The Test For Lyme Disease Called
What Is A Lyme Disease Blood Test
A Lyme disease blood test is used to determine if you have contracted Borrelia burgdorferi , the bacterium that causes Lyme disease. Lyme disease tests are conducted with a routine blood draw.
While there are other species of Borrelia that cause Lyme disease, B. burgdorferi is the most common cause in the United States. Most antibody tests in the United States only test for B. burgdorferi, but other species-specific tests are available depending on a persons travel history.
Lyme disease is transmitted to humans through ticks that are infected with Borrelia.
- dizziness
- shortness of breath
Lyme disease can be difficult to diagnose. Ticks are very small, and the bites are not always noticeable. Symptoms of the disease can vary from person to person. Not everyone experiences the classic bulls-eye rash pattern around a tick bite.
It should be noted that testing is not always required to make a diagnosis. For people with a classic bulls-eye rash living in a high risk area, testing is not recommended for diagnosis.
Your doctor will use the results of a Lyme disease antibody test, along with the report of your symptoms, to confirm a diagnosis.
Antibodies are proteins your body makes in response to foreign or harmful substances called antigens. Common antigens include:
- bacteria
- fungi
- chemicals
If you have never been exposed to B. burgdorferi, you will not have any Lyme disease antibodies in your bloodstream. In this case, your test will be negative.
Dont Be Fooled By The Repeat Test
People with Lyme want to know if treatment is working – especially if they are not feeling better. The truth is, there are no biologic markers or immune system tests that show if you have recovered or are recovering from Lyme and coinfections. Repeating elispot tests like those offered by Armin Labs, or western blot tests and immunoblot tests offered by IGenex do not have any scientific proof to show they can predict the end of treatment or where you are in your treatment.
Simply put, retesting is not scientifically valid.
Also Check: How To Treat Post Lyme Disease Syndrome
Is Treatment 100% Effective
Scientists are divided on this topic. Some studies suggest that that even long-term antibiotics may not completely clear infection dogs may get sick again at some point after antibiotic treatment is stopped. Other studies suggest that complete clearance of infection is possible with antibiotic treatment. Further research is required to answer this question.
Negative C6 Elisa On Serum
Early clinical Lyme disease in the form of erythema migrans with associated history of a tick bite should be treated empirically. There is no need for testing unless there are further symptoms.
A negative ELISA result in the early stages of Lyme disease does not exclude infection. If acute Lyme disease is suspected but serology results are negative, we recommend that the test is repeated in 4-6 weeks with a fresh sample to look for seroconversion.
In patients with long term symptoms a negative ELISA test usually excludes Lyme disease as a cause of these symptoms. Information on differential diagnosis for patients with persistent symptoms and negative Lyme disease serology results is available.
You May Like: How To Cure Lyme Disease In Dogs
Problems With Testing For Lyme Disease
The problem is that Lyme disease is critically misunderstood by many people in the medical profession. Most doctors are not very well-versed in Lyme disease. Testing is not reliable. Many medical professionals are simply not educated about chronic Lyme disease to recognize and treat it. Conventional doctors often have a difficult time diagnosing, understanding, or treating something that they cannot see or isolate. Hence, Lyme disease diagnosis and treatment may be one of the most controversial and difficult issues in medicine. There are a lot of grey areas, a lot of misunderstandings, and unreliable testing, so going to a Lyme-literate practitioner is critical.
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Read Also: Can Lyme Disease Cause Leg Weakness