Phylogenetic Diversity And Human Disease Taxonomy And Disease
B. burgdorferi was thought to be the sole genospecies in the United States until 1995 when Marconi and associates isolated B. andersonii from cottontail rabbits and I. dentatus ticks. Subsequently, it became evident that enzootic cycles exist involving non-sensu stricto species and specialist ixodid ticks with strong, selective host preferences and little or no proclivity to bite humans. Perhaps the best characterized of these is B. bissettii , transmitted by I. pacificus, I. affinis and I. spinipalpis and recovered and/or detected by PCR throughout the United States in ticks and a variety of vertebrates and, in rare instances, humans . Molecular evidence for infection of humans by B. americana and B. andersonii, particularly in Southern states, also has been reported . Moreover, B. mayonii was recently isolated from a few human specimens in upper midwestern U.S. . However, in the United States, B. burgdorferi remains the primary agent of disease.
Lyme Disease In Children
As noted earlier, Lyme disease began as an affliction of children and it continues so to this day. The clinical manifestations of Lyme disease in children, as in adults, mainly involve the skin, central nervous system, joints, and heart . The primary EM lesion in children is most commonly found on the head and neck , arms or legs , or lower back . Awareness of EM in the head and neck is important because such lesions can be hidden by the hairline. Less frequently lesions can be found over the abdomen , the axilla , the groin , or the chest . Most single EM lesions in children are uniformly erythematous however, they also can have central erythema or clearing and, in rare instances, painful central ulcerations . Children also may present with constitutional symptoms, including fever , fatigue , headache and arthralgias . The presence of multiple EMs has been documented in up to 40% of children and most have associated fever , fatigue , and headache . Similar to adults with Lyme disease, ~20% of children may present with constitutional symptoms as the only manifestation . Practitioners in endemic areas need to have a high index of suspicion to avoid missing the diagnosis in such children.
Maternal-fetal transmission of B. burgdorferi has never been definitively documented, and epidemiologic investigations have failed to establish an association between infection and adverse outcomes of pregnancy .
What Can I Expect Long Term If My Child Has Lyme Disease
If Lyme disease is caught and treated early, most children will make a full recovery. Some children with Lyme disease go on to experience what’s called a post-infectious syndrome with symptoms that may include feeling fatigue, joint aches and pains, headaches, difficulty sleeping, and problems concentrating. Since the infection itself is gone by this time, doctors generally don’t prescribe antibiotics. Each child is different, but it’s not uncommon for symptoms of post-infectious syndrome to linger for months, or even years, and they can be made worse by stress or other illness. But most children do make a full recovery.
Blacklegged, or deer, ticks are very small, so it helps to know what to look for when doing a tick check. Adults are about the size of sesame seeds and in the nymph or larva stage, they can be as tiny as a poppy seeds.
Don’t Miss: Natural Ways To Get Rid Of Lyme Disease
Can Patients With Lyme Disease Have Persistent Symptoms After Treatment
It is clear that a proportion of patients with confirmed evidence of previous Lyme disease continue to have symptoms after standard antimicrobial treatment. The terms chronic Lyme disease and post-Lyme disease syndrome have been applied by some clinicians to patients with symptoms persisting more than six months after treatment with the recommended agents. Persistent symptoms include fatigue, generalized musculoskeletal pain and cognitive impairment without objective findings or microbiological evidence of active infection.
Given that some patients have persistent symptoms after treatment of their Lyme disease, the question has been raised of whether there is benefit to prolonged antimicrobial therapy. Four randomized placebo controlled trials, all conducted in the US, have addressed this issue. The larger of the studies included two separate studies of patients clinically diagnosed with acute Lyme disease. Both studies enrolled patients who had previously been treated with a recommended antibiotic regimen and reported ongoing symptoms. The subjects were placed into the seropositive or seronegative study according to their serological status at the time of enrollment. There were 129 patients enrolled in the two studies, and participants were randomly assigned to receive either ceftriaxone 2 g daily for 30 days followed by doxycycline for 60 days, or placebo. Outcome measures included cognition, memory, pain and activities of daily living.
Early Disseminated Lyme Disease
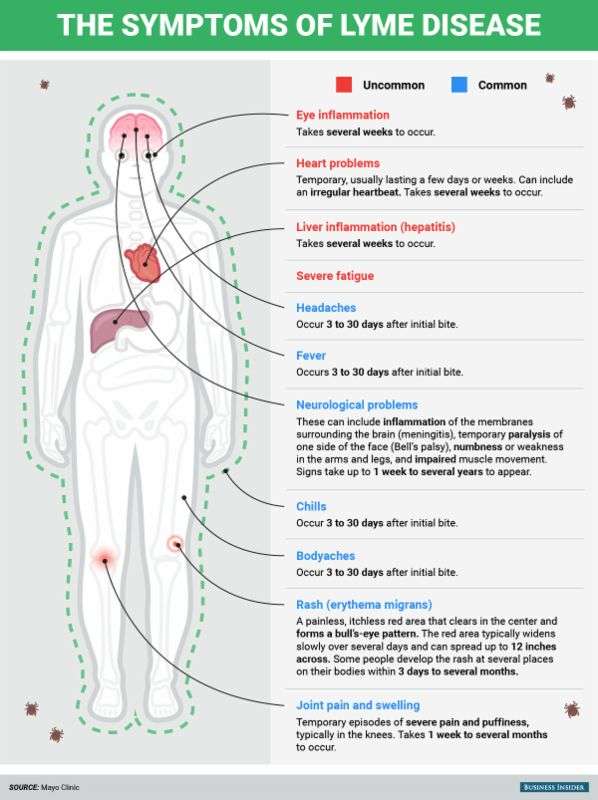
If Lyme disease is left untreated, it may progress to early disseminated Lyme disease, which spreads from the bite location to other parts of the body. It may begin to affect the skin, nervous system, and heart. This stage can occur days to months following the initial infection.Neurologic symptoms occur in approximately 10% of untreated people.
Inflammation of the nervous system can cause:
- Facial paralysis
- Fever
- Numbness, tingling, shooting pain, or weakness in the arms or legs
- Sensitivity to light
- Severe headache or neck stiffness
Lyme carditis, which affects approximately 5% of people in this stage, occurs when the infection reaches the heart tissue and slows down the heart rate too much. Some people may not have any symptoms, while others may experience severe effects requiring hospitalization.
Symptoms include:
- Light-headedness
- Shortness of breath
During this stage, you may develop multiple erythema migrans rashes on areas distant from the original bite. You may also experience headaches, muscle or joint pain, or extreme fatigue.
Early disseminated Lyme disease can be treated with oral or intravenous antibiotics for two or more weeks, depending on the severity of the symptoms.
You May Like: What Does Lyme Disease Rash Look Like
What Are The Signs And Symptoms Of Lyme Disease By Stages
There are three stages of Lyme disease, which are outlined below.
Stage 1 Early Localized Disease
- Occurs one to 30 days after a tick bite
- characteristic skin rash of Lyme disease
- migrating red rash with bullseye appearance occurring at or near the site of the tick bite
- asymptomatic or itches orburns
- develops around seven days after the tick bite
- rash expands over a matter of days
- an untreated rash may persist for two to three weeks
Stage 3 Late Disease
Stage 3 Lyme disease occurs months to years after the initial infection or a period of latency. Most patients presenting with the late disease do not have erythema migrans because the rash urges the patient to seek treatment earlier.
Symptoms of Stage 3 Lyme Disease may include the following:
- Skin manifestation:
- Acrodermatitis chronica atrophicans: found almost exclusively in patients of European descent. It commonly affects older women with bluish-red discoloration on the back of the hands, feet, knees, and elbows.
Who Is At Risk Of Lyme Disease And Why
An individual must first be bitten by a tick that is infected with B. burgdorferi for infection to occur. While infected ticks can be sporadically deposited in different regions in Canada by migratory birds, the risk of getting Lyme disease is greatest in an area where the ticks are persistently present or endemic, and the risk depends on the proportion of ticks that are infected. Even in areas where the ticks have become endemic, the proportion infected by this spirochete varies and is evolving. Clinicians may want to check with their local public health departments to understand where the current Lyme endemic areas are within their jurisdiction. It is important to obtain a thorough travel history from the patient, as Lyme disease is endemic in other areas of North America and Europe, and travel-related Lyme disease accounts for a proportion of the documented cases in Canada. It is also important to relay this travel history or suspicion of European Borrelia infection to the diagnostic laboratory, as the confirmatory testing for North American and European Borrelia strains differs.
Also Check: Dr Emilia Eiras Lyme Disease
How To Prevent Post
While you may not be able to prevent post-treatment Lyme disease syndrome, you can take precautions to prevent coming into direct contact with infected ticks. The following practices can reduce your likelihood of getting Lyme disease and developing persistent symptoms.
If a tick bites you, contact your doctor. You should be observed for 30 days for signs of Lyme disease. You should also learn the signs of early Lyme disease and seek prompt treatment if you think youre infected. Early antibiotic intervention may reduce your risk of developing chronic symptoms.
The signs of early Lyme disease can occur from 3 to 30 days after a bite from an infected tick. Look for:
- a red, expanding bulls-eye rash at the site of the tick bite
How You Get Lyme Disease
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks can be found in any areas with deep or overgrown plants where they have access to animals to feed on.
They’re common in woodland and moorland areas, but can also be found in gardens or parks.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
Don’t Miss: Lyme Disease Association Doctor Referral
What Should You Do If You Find A Tick
-
Dont touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Dont squeeze the tick, and dont use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
Read Also: How To Detect Lyme Disease
Lyme Disease Vaccine News For 2018
– Tufts University announced that when people are exposed to Lyme bacteria, the potential host produces a substance the bacteria use to grow. The investigators believe a testing mechanism that detects these autoantibodies could be the fastest and most accurate way to test for Lyme disease.
– Valneva SE and Pfizer Inc. reported other positive Phase 2 data for their Lyme disease vaccine candidate, VLA15. Valneva and Pfizer plan to proceed with a three-dose primary series vaccination schedule in a planned Phase 3 clinical trial based on these new results. The trial will evaluate VLA15 in adults and pediatric subjects five years of age and above and is expected to be initiated in 2022, subject to regulatory approval.
– MassBiologic’s Lyme PrEP has begun a phase 1 clinical trial to test for the safety of Lyme PrEP and to determine how long it lasts in the bloodstream in humans. Lyme PrEP uses a monoclonal antibody.
– Yale researchers are developing an mRNA vaccine against Lyme disease.
– The U.S. CDC published Estimating the Frequency of Lyme Disease Diagnoses, United States, 20102018. Using commercial insurance claims data, we estimated that Lyme disease was diagnosed and treated in about 476,000 patients in the USA annually during 20102018. The CDC said these results underscore the need for accurate diagnosis and improved prevention.
Read Also: Does Bravecto Prevent Lyme Disease
Lyme Disease Vaccine Candidates In 2022
VLA15 is a multivalent Lyme Disease vaccine candidate that targets the outer surface protein A of Borrelia. It is designed for prophylactic, active immunization against Lyme disease, aiming for protection against most human pathogenic Borrelia species.
Yale researchers stated they developed an mRNA vaccine against Lyme disease that triggers an immune response at the tick bite site and provides partial protection against the disease-causing bacteria.
The National School of Tropical Medicine at Baylor College of Medicine, along with Texas Children’s Hospital’s Center for Vaccine Development, received an $860,000 grant from the Department of Defense to develop a recombinant protein vaccine for Lyme disease.
Lyme PrEP – Lyme PrEP uses a single human antibody to kill the bacteria in the tick’s gut while the tick drinks its victim’s blood before the bacteria can get into the human host.
What Happens If Chronic Lyme Disease Is Left Untreated
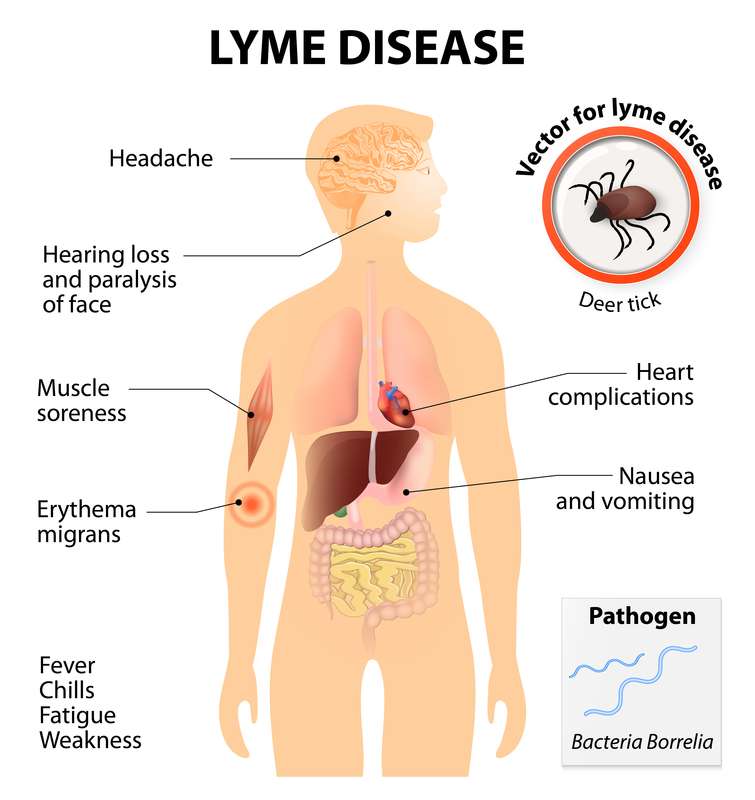
When you think you have been bitten by a tick, its important to schedule an appointment at Kotsanis Institute of Functional Medicine with Dr. Constantine Kotsanis. When left untreated, chronic Lyme disease can cause memory loss, inflammation around your heart and throughout your body, nerve damage, autoimmune disease, and other long-term heart problems. The good news is that Lyme disease is treatable, especially when we catch symptoms early in Grapevine, TX. We have successfully administered medication with Lyme disease treatment to our patients to rid their bodies of this infection.
Read Also: What Tick Has Lyme Disease
Intraspecies Genotypes Are Associated With Distinct Clinical Phenotypes
Several studies have now demonstrated differential pathogenicity among various genotypes within B. burgdorferi . As a generalization, RST1 genotypes contain ospC alleles associated with invasive disease, whereas RST3 genotypes contain predominantly noninvasive ospC alleles . For example, RST1 strains are more often detectable in blood in mice and humans , suggesting that they disseminate more readily and/or reach higher numbers in blood. Moreover, RST1 OspC type A strains are associated with more symptomatic early infection in patients with EM, and they more frequently cause antibiotic-refractory Lyme arthritis than other strains . The greater disease severity and propensity for dissemination of RST1 vs RST3 genotypes was corroborated experimentally in the murine model . The data also suggest that RST1 strains are likely a contributing factor in the prevalence and severity of Lyme disease in the Northeastern U.S. . In the mouse model, RST1 OspC type A strains have higher transmission efficiency from mice to ticks than other strains . In addition, they appear to be a recently evolved clonal lineage that may be an important factor in the emergence of the Lyme disease in the northeastern U.S. .
When To See Your Gp
You should see your GP if you develop any of the symptoms above, after being bitten by a tick .
Make sure you let your GP know if youve spent time in woodland or heath areas. Diagnosing Lyme disease is often difficult as many of the symptoms are similar to other conditions.
A spreading rash some days after a known tick bite should be treated with antibiotics. This is without waiting for the results of a blood test.
Blood tests can be carried out to confirm the diagnosis after a few weeks. These can be negative in the early stages of the infection. You may need to be re-tested if Lyme disease is still suspected after a negative test result.
Don’t Miss: Symptoms Of Lyme In Child
Who Is At Risk For Lyme Disease
Anyone can get a tick bite. But people who spend lots of time outdoors in wooded, grassy areas are at a higher risk. This includes campers, hikers, and people who work in gardens and parks.
Most tick bites happen in the summer months when ticks are most active and people spend more time outdoors. But you can get bitten in the warmer months of early fall, or even late winter if temperatures are unusually high. And if there is a mild winter, ticks may come out earlier than usual.
Is There A Test For Lyme Disease
Diagnosing Lyme disease can be difficult as symptoms can vary between individuals and can also be similar to other illnesses. Health care providers use information on symptoms, potential exposure to infected black-legged ticks, and laboratory blood testing to diagnose the disease. Laboratory tests alone may not always detect Lyme disease, especially if it is in the early stages of infection. If an individual develops symptoms of Lyme disease after being bitten by a tick or visiting a known at risk area for Lyme disease, they should see their family doctor right away. The earlier a diagnosis is made, the greater the chance of a successful treatment. For more information about diagnosing Lyme disease visit www.canada.ca/Lymedisease.
Also Check: Do Ticks In Florida Carry Lyme Disease
What Are The Symptoms Of Lyme Disease
Early symptoms of Lyme disease start between 3 to 30 days after an infected tick bites you. The symptoms can include:
- A red rash called erythema migrans . Most people with Lyme disease get this rash. It gets bigger over several days and may feel warm. It is usually not painful or itchy. As it starts to get better, parts of it may fade. Sometimes this makes the rash look like a “bull’s-eye.”
- Fever
- Muscle and joint aches
- Swollen lymph nodes
If the infection is not treated, it can spread to your joints, heart, and nervous system. The symptoms may include:
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of your body
- Facial palsy, which is a weakness in your facial muscles. It can cause drooping on one or both sides of your face.
- Arthritis with severe joint pain and swelling, especially in your knees and other large joints
- Pain that comes and goes in your tendons, muscles, joints, and bones
- Heart palpitations, which are feelings that your heart is skipping a beat, fluttering, pounding, or beating too hard or too fast
- Shooting pains, numbness, or tingling in the hands or feet