Chronic Lyme Disease Symptoms
If Lyme disease is not diagnosed and treated early, it may become late-stage or chronic. This may also occur when early treatment is inadequate. While some symptoms of chronic or late stage Lyme disease are similar to those of early Lyme, as the graphic below shows, there are important differences.
Lyme disease may spread to any part of the body and affect any body system. Typically, it affects more than one body system. In our survey, which drew over 5,000 responses, patients with chronic Lyme disease reported an average of three severe or very severe symptoms, with 74% reporting at least one symptom as severe or very severe.
An extensive list of symptoms of chronic Lyme disease was developed by Dr. Joseph Burrascano, a pioneer in treating chronic Lyme disease.
How Is Lyme Disease Diagnosed
Lyme disease is usually diagnosed via a blood test called an ELISA, or an enzyme-linked immunosorbent assay, explains Dr. Ormond. It can detect antibodies to B. burgdorferi, the bacteria that causes Lyme disease.
Less often, a doctor might test someones cerebrospinal fluid for antibodies via a lumbar puncture . This is usually done if a patient is experiencing symptoms that indicate their central nervous system has been affected, continues Dr. Ormond.
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Read Also: Old Lyme Beach Homes For Sale
How To Identify Tick Bites
Ticks arenât like bugs that bite you and then fly away or scoot off. When one gets on your body, it sets up camp. It finds a place to eat, then burrows its head into your skin and starts feeding. And itâll stay there for several days.
Most likely, you wonât feel anything because the bite doesnât hurt, and it isnât usually itchy. Because ticks are often very small, you might not see it either. At first, it might just look like a fleck of dirt. As it feeds though, it swells up and can be easier to find.
You might get a small red bump where the tick bites you. Some peopleâs bodies react to ticks with 1 to 2 inches of redness around the bite. That red area wonât get any bigger, unless itâs really a rash, which is a sign of disease.
Ticks typically bite people in warm, moist, or hairy areas, like the:
- Scalp
- Groin
- Skin between your fingers and toes
Once a tick finds a place to feed, it will stay there anywhere from a few days to 2 weeks. Ticks bite once and use that site to feed on your blood until theyâre full. A tick will fall off on its own once itâs full. You wonât get multiple bites from a tick. Most tick bites are painless and cause only a minor reaction. Only sometimes do they transmit disease.
Atypical Lyme Rashes And Less
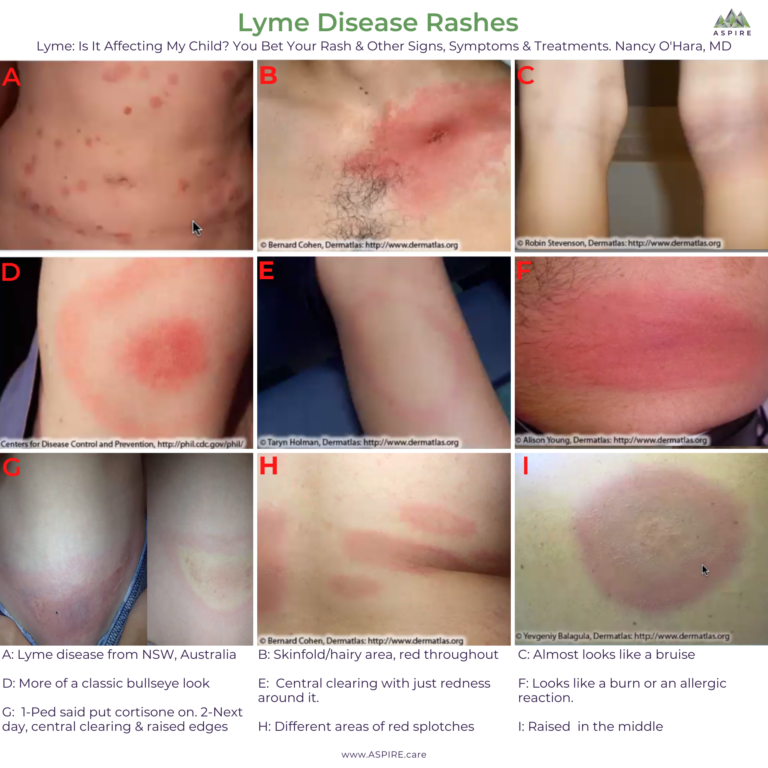
In some cases, the Lyme disease rash doesnt look like a bulls eye at all. It can be blistered , cause a bluish swelling , be uniform in color instead of banded, be oval or triangular in shape, or just look like a large red area . You can see a picture of atypical Lyme disease on a black man here.
There are also many instances of Lyme rashes which are considered to be bulls-eye shaped, but dont have the white band inside. The message? Dont expect a Lyme rash to look like a perfect bulls eye. If you suspect Lyme, contact your doctor!
Recommended Reading: Symptoms Of Lyme Disease In Humans After Tick Bite
What Are The Symptoms Of Chronic Lyme Disease
Chronic Lyme disease is not a recognized condition. However, some symptoms can persist past treatment. This has led doctors to describe the phenomenon as post-treatment Lyme disease syndrome . PTLDS occurs in about 520% of people who receive Lyme disease treatment. It may cause symptoms such as:
- fatigue
Stage : Quickly Expanding Rash
After being bitten by a black-legged tick, a quickly growing rash can appear. This is the earliest stage of Lyme disease, known as stage 1.
Most people who develop a rash, get it within days or weeks of being bitten by a tick.
Where you see the rash: If you develop a rash, it appears near the tick bit you. For most people, that means the back, groin, armpit, or a lower leg. However, a tick can bite you anywhere.
What the rash can look like: You may see a spot or bump on the skin, which is the bite mark. Around or near the bite mark, a rash develops. Some people see the bulls-eye rash . You can also have one of the other rashes shown here.
Early rash caused by Lyme disease
Notice the bite mark in the center of this early rash, which will expand quickly.
Bull’s-eye rash on woman’s upper arm
This is another early sign of Lyme disease.
Lyme disease rash with lighter color on the outside
This rash has expanded, but you can still see the bite mark in the center.
Rash from Lyme disease has begun to clear
As the rash begins to clear, the redness fades.
If you develop a rash during this stage, you may notice that it:
-
Feels smooth and warm to the touch
-
Causes a burning sensation
-
Itches or feels painful
-
Has an outer edge that feels scaly or crusty
When the rash and symptoms begin: According to the Centers for Disease Control and Prevention , the rash begins 3 to 30 days after the tick bites you.
About 50% of people who have Lyme disease develop flu-like symptoms , which include:
Recommended Reading: Pictures Of Tick Bites With Lyme Disease
How Do You Get Lyme Disease
Lyme disease is transmitted through the bite of an infected tick, most often a baby tick called a nymph . That sounds scary like the moment a tick lands on your or your kid, youre potentially going to get Lyme. However, thats not the case. Mordue explains that it takes 36-48 hours in order for the pathogen to be transmitted. In other words, the tick has to stay on your body for at least a day and half to actually infect you. That is one reason it is so important to check yourself for ticks after potential exposure to an environment likely to have ticks, she explains.
So what environments have ticks? Ticks tend to be near the ground, in leaf litter, grasses, bushes and fallen logs. High risk activities include playing in leaves, gathering firewood and leaning against tree trunks, explains Dorothy Leland, board president of LymeDisease.org. Yet even if youre not doing any of that, youre not completely in the clear. Ticks can be in a local park or your yard too, or even take a ride into your house on your dog. Watching out for ticks throughout the summer, no matter what youre doing, is important.
Where Is Lyme Disease A Problem
Since 1975 when it was first noted, thousands of cases have been reported in the USA. Lyme disease is less common in the UK. 730 cases were confirmed in 2015 in England and Wales. Not all are reported so the total number of cases each year is unknown. However, it is estimated to be 2,000 to 3,000. This is because many cases are not formally diagnosed and clear away without any treatment. Many people affected are forestry workers and other outdoor workers but visitors and holidaymakers to countryside areas where ticks are found are at risk.
Over half of infections acquired in the UK are known to have been caught in the southern counties of England. Areas where it is most common tend to be centres of outdoor activity – in particular, the New Forest, Thetford Forest, the South Downs, Exmoor, the Lake District, the North York moors and the Scottish Highlands. Up to a fifth of Lyme disease is caught while abroad – in particular, the USA, France, Germany, Austria, Scandinavia and eastern and central Europe.
Read Also: Best Cure For Lyme Disease
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040″ rel=”nofollow”> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Severe Pain Numbness Or Tingling In Your Joints And Muscles
Around 60% of patients will develop joint pain or even arthritis as their Lyme disease progresses, according to a Johns Hopkins University School of Medicine study. Usually, it starts in the joints closest to where you were bitten and can spread from there, especially to areas like the knees. The pain isnt usually constant, though. Experts dont fully understand why, but the symptoms can wax and wane over a period of weeks or months, Sellati says.
Over time, the disease can attack the cartilage in the joints and lead to tissue damage, says Linda Yancey, M.D., an infectious disease specialist with Memorial Hermann Katy Hospital in Katy, TX.
Like many of the other problems caused by Lyme disease, this one is also triggered by inflammation. The damage to tissues, bone, and cartilage is caused by the production of pro-inflammatory proteins, the same protein responsible for damage caused by rheumatoid arthritis, Sellati says.
Recommended Reading: What Are The Signs Of Lyme Disease In A Dog
What Is The Outcome
If you are treated with antibiotic medication in stage one of the disease, you have a very good chance of a complete cure with no further problems.
If you are not treated in stage one, you may go on to develop some symptoms of stage two or three. However, these are often mild and transient symptoms such as a skin rash or mild joint pains. Some people develop more severe symptoms if they progress to stage two or three. Treatment with antibiotics during stage two or three is also usually curative. However, a prolonged course of antibiotics may be needed. It may be difficult to treat post-Lyme syndrome, as it is not yet known what causes these ongoing symptoms. However, most eventually clear up with time.
Infection with Lyme disease does not produce lifelong immunity so you will need to continue with tick bite prevention measures to reduce the risk of further infection.
Further reading and references
How Does Lyme Disease Present For Different Age Groups
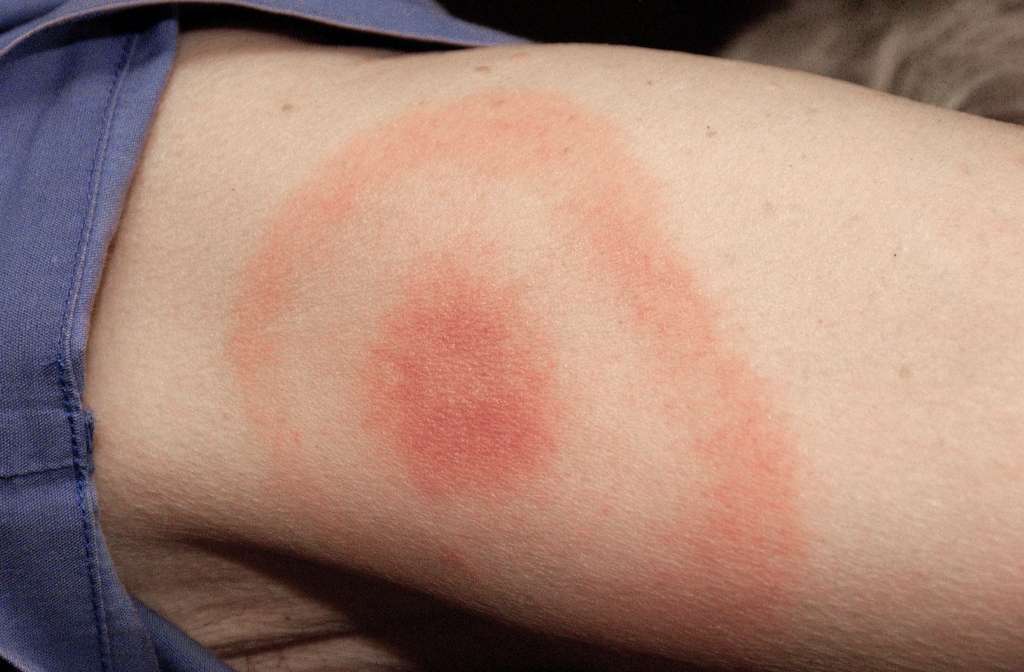
There isnt one age group where Lyme presents more or less severely: Lyme disease presents similarly in babies, kids, and adults. However, Mordue notes that there is substantial variability of disease presentation and severity between people. In other words, two siblings who are both bitten by a tick while out in the woods may have very different symptoms. Children, however, are more likely to get it than adults since children typically spend more time outdoors, and because tall grasses are proportionally taller for young children.
Fatigue, headache, and fever are common symptoms of early Lyme disease. Joint pain is another potential symptom: Some children may present with a swollen, painful joint as their first symptom of Lyme disease, though this is considered a later manifestation, Szantyr explains. While the knee is most commonly written about, it can be wrists, elbows, hips, ankles, even the TMJ. If your child is old enough to tell you something hurts, take note, write it on the calendar, check their temperature and remember what you have been doing and whether there is a possibility of tick exposure For younger children, notice if they are limping, if they are not playing in their usual way, if they seem a little less like themselves.
Read Also: All Pro Automotive Old Lyme
A Leading Cause Of Misdiagnosis Is The Failure To Recognize The Lyme Disease Rash When Present
Available blood tests are antibody-based for Lyme disease and do not accurately diagnose Lyme disease in the first few weeks of infection. False negative tests are a problem in acute Lyme disease. Therefore, early Lyme disease is a clinical diagnosis. Recognizing signs and symptoms can be vital to receiving appropriate early treatment and patient care, especially in the COVID-19 era.
Exhaustion Fuzzy Thinking And Other Cognitive Problems
Borrelia burgdorferi is one of the few bacteria that can cross the blood-brain barrier and infect the central nervous system, explains Timothy J. Sellati, Ph.D., Chief Scientific Officer for the Global Lyme Alliance. That can lead to inflammation of the brain, which can affect your central nervous system function in a few different ways.
One of those is extreme fatigue, which affects as many as 76% of people with advanced Lyme disease, according to research. Trouble concentrating, loss of coordination, and short-term memory loss are other possible problems, occurring in up to 24% of people. In extreme cases where the disease is left untreated for extended periods, you might even develop facial weakness and behavioral changes, Sellati says.
Also Check: Lyme Disease Test Turnaround Time
How To Remove Ticks
Tick bites aren’t always painful. You may not notice a tick unless you see it on your skin. Check your skin and your children’s or pets’ skin after being outdoors.
To remove a tick:
The risk of getting ill is low. You don’t need to do anything else unless you become unwell.
When Should I Go See My Doctor
Anyone who has been bitten by a black-legged deer tick is at risk for Lyme disease. The highest risk groups include those living in or visiting endemic areas, especially people who spend significant time outdoors such as gardeners, hikers, or outdoor workers.
Patients should seek advice from their doctor if they have a suspicious round expanding red skin lesion, and/or show signs of summer-flu, particularly during Lyme disease season, which is highest-risk late spring through July/August. If those circumstances apply or symptoms persist it is very important to go to a physician.
For the west coast and other more temperate regions Lyme disease can be a year-round concern.
In the later disseminated stages, Lyme disease can be a much more insidious and complex illness. An individual should seek medical care if experiencing symptoms such as prolonged fevers, unexplained fatigue, painful joints, new or unusual headache, or heart or neurologic symptoms. If unexplained viral-like symptoms last for more than 1-2 weeks, please seek the advice of a physician.
Read Also: Monastery Of Herbs Lyme Disease
What If A Tick Bites My Dog
The more ticks in your region, the likelier it is that your furry pal will bring them home.
Your dog is much more likely to be bitten by a tick than you are. And where Lyme disease is common, up to 25% of dogs have had it at some point.
About 10% of dogs with Lyme disease will get sick. 7-21 days after a tick bite, your dog might seem like theyâre walking on eggshells. They also might have a fever and enlarged lymph nodes. Plus, they might seem tired. Dogs also get antibiotics for Lyme.
What if my dog brings ticks into my home?
Use a tick control product on your pet to prevent Lyme disease. Also, have your dog vaccinated against Lyme.
Check your dogâs whole body each day for bumps. If you notice a swollen area, see if thereâs a tick there. If you find a tick, wear gloves while you use tweezers to separate it from your dog. Then, put it in soapy water or alcohol, or flush it down the toilet.
Use alcohol to clean the spot on your dog where the tick was attached. Keep an eye on that spot, and also on your dog to make sure theyâre behaving normally. If you notice any changes, check with your vet.
Show Sources
John Aucott, MD, assistant professor of medicine, Johns Hopkins University School of Medicine director, Johns Hopkins Lyme Disease Clinical Research Center.
CDC.
Morbidity and Mortality Weekly Report: âVital Signs: Trends in Reported Vectorborne Disease Cases — United States and Territories, 2004-2016.â
American College of Rheumatology.
Knowing The Symptoms To Look For Can Help Diagnose Lyme Disease Early On When It’s Easily Treatable
Karen Pallarito tells stories grounded in science and backed by solid reporting. As Senior Conditions Editor for Health, she covers COVID-19 plus umpteen other health and wellness topics. Her freelance portfolio includes pieces for The Washington Post, U.S. News & World Report, Working Mother, Westchester Magazine, and the news syndicate HealthDay, among others. Karen started her career as a health policy reporter in the nation’s capital, where she covered congressional hearings on Medicare and Medicaid. From the late 90s to the early aughts, she reported on health business for Reuters Health and contributed to its medical and consumer health newswires. Prior to that, she was Modern Healthcare’s New York Bureau Chief. A fellow of the Association of Health Care Journalists’ 2019 class on Comparative Effective Research, Karen is committed to helping people understand the benefits and harms of clinical interventions and exposing racial/ethnic disparities in healthcare. When not on deadline, you might find her whipping up something in the kitchen, working out, bingeing on cable news, or indulging in some form of mind candy .
- Pin
Its super important that we think of all the tick-borne diseasesnot just Lyme, Dr. Flanagan tells Health. Babesia, a parasite that causes babesiosis, is treated differently than Borrelia, for example.
Don’t Miss: Lyme Disease In Brain Treatment