Your Immune System Autoimmune Disease And Lyme
Now, your immune system’s reaction to the Borrelia burgdorferi bacteria infection is typical: perceive stress and get the NEM started, with inflammation a typical part of this process. But research, which has identified a protein marker showing this bacterial infection, has discovered the way this bacterium works that results in a continued inflammatory response.
Unlike other bacteria, Borrelia burgdorferi can make a comeback even when your immune response and the conventional treatment worked perfectly. This means that this bacterium could stay in your body for an exceptionally long time.
Your body’s immune system, as the first line of defense, will send in a nonspecific attack to get rid of what it sees as a foreign pathogen. And if this does not work, it will take a few days to study the pathogen and then formulate a new attack to take care of the issue. But no matter how long it ultimately takes to kill off these bacteria, the damage was done. Your body’s inflammatory load increased to such a large extent, which could cause many of the inflammatory conditions previously mentioned.
To make matters worse, your body’s own constant inflammatory response produces irritations. And when this happens, these irritations cause stress. This, in turn, further fuels an inflammatory reaction. So, your body’s inflammatory response becomes a cyclical reaction of inflammation, response, inflammation, etc.
Easy misdiagnosis
Three Stages Of Lyme Disease: Common Symptoms
Lyme disease can be divided into three stages based on symptoms: early localized, early disseminated and late.
Early localized stage includes symptoms like red growing rash, flu-like symptoms, headache, fatigue, fever, muscle pain, neck stiffness and joint stiffness. These are the most common symptoms that people with Lyme disease experience. A person can develop these symptoms within 1-28 days after the tick bite.
Early disseminated disease includes large rash which tends to expand, as well as swelling of lymph nodes, joint pain, palsy of cranial nerves and eye pain. It can even manifest itself as heart-related problems, like myocarditis or pericarditis. Stage 2 disease develops between 3-12 weeks after the bite.
Late disease includes symptoms like arthritis, which mostly affects large joints like knees. Late Lyme disease can take months or years to develop, so by the time a patient gets symptoms, they might not even remember about their encounter with ticks.
Symptoms arent uniform across people and depend on the stage of Lyme disease. Also, its important to note that Lyme disease symptoms in children are very similar to those in adults. Major clinical manifestations appear on skin, central nervous system, joints and heart.
The Autoimmune Protocol Diet
The AIP is a specialized version of a Paleo diet that eliminates foods that may stimulate the immune system and harm the gut, where much of the immune system resides and where autoimmunity is theorized to begin in many cases. AIP also focuses heavily on optimizing dietary nutrient density and incorporating foods that mitigate inflammation and support a healthy gut. I have used AIP innumerable times with clients to reduce and even reverse autoimmune disease processes with excellent results. In recent years, the autoimmune protocol has been studied in scientific trials and found to improve symptoms and markers of autoimmune activity in people with autoimmune diseases, ulcerative colitis, and Crohns diseases, including reducing calprotectin. The AIP diet has also been found to decrease systemic inflammation and improve symptoms and quality of life in Hashimotos disease.
The AIP removes the following foods from the diet for at least three months:
-
Nightshades, such as tomatoes and peppers
You May Like: What Happens When You Get Lyme Disease
Autoimmune Disease And Lyme: The Connection
Research into autoimmune disease and Lyme have made a startling discovery. The long-term treatment with antibiotics only eradicates all the bacteria in a certain percentage of those affected. In others, where remnants of the bacteria persist, their initial symptoms could progress and result in damaging neurological health issues. Furthermore, many of these people develop various autoimmune conditions, including the likes of rheumatoid arthritis and multiple sclerosis. They could also end up suffering from conditions closely related to adrenal fatigue. These include, amongst others, memory issues, chronic fatigue, a decline in cognitive function, and even various mood disorders.
Your body’s autoimmune response to the bacteria may result from damage encountered while initially infected. The bacteria’s outer coat is similar to that of your nervous system tissue. Your immune cells that were reacting to the bacteria could end up attacking your own nervous system tissue. Essentially, the residual bacteria tissue causes an immune system response. This results in the many irregular diagnoses surrounding Lyme disease and the autoimmune disorders that develop because of this bacterial infection. So, autoimmune disease and Lyme has a definite connection.
Lyme Disease And Autoimmune Conditions

A Lyme disease infection is known to cause a weak immune system. To understand how this happens, the researchers isolated dendritic cells from healthy study participants and exposed them to Borrelia burgdorferi, finding that the bacterial infection causes receptor sites on the surface of dendritic cells, known as HLA-DRs, to mature and become active. Normally, these HLA-DRs cells would present antigens to killer T-cells, the immune system agents that remove invaders from the body.
The researchers believe that when the HLA-DRs interact with Borrelia burgdorferi, they are structurally changed and keep the dendritic cells from marking the bacterial proteins as foreign, which leads to the dendritic cells attracting T-cells, but instead of attacking the Lyme disease bacteria, instead attacks the healthy cells.
Senior author Mark Soloski, PhD, co-director for basic research at the centre, and professor of medicine at the Johns Hopkins University School of Medicine, said: We believe these observations are relevant not only to how Borrelia burgdorferi disrupts the immune system but other infections as well. Antibodies that react with a persons own tissues or organs have been reported in patients with infections, including COVID-19.
Recommended Reading: At Home Lyme Disease Test
Lyme Vs Autoimmune Disease: Similarities Differences And Misdiagnoses
Physicians and researchers have made important discoveries about the connections between Lyme disease and autoimmune diseases. While more research is still needed, the existing evidence can be useful for both physicians and patients in understanding and treating their symptoms.
In this article, well cover some basic information on autoimmune diseases, how Lyme disease may trigger them, and how the similarities between the symptoms of Lyme and symptoms of some autoimmune diseases can lead to a missed or misdiagnosis.
Autoimmune Diseases And Lyme Disease: Misdiagnosis Or Complication Of Lyme
As mentioned above, there are documented correlations between Lyme and autoimmune diseases. The evidence shows that Lyme disease may trigger an autoimmune disease, or it may mimic an autoimmune disease.
What does this mean for patients and physicians? It comes down to the importance of getting an accurate and timely diagnosis if you suspect Lyme or another tick-borne disease. The longer Lyme disease goes untreated, the stronger the chance that it will spread to multiple body systems and possibly trigger an autoimmune response.
Because Lyme disease symptoms mimic symptoms of so many other conditions, including autoimmune diseases, it is notoriously tricky to diagnose. One of the most common Lyme disease misdiagnoses is the autoimmune disease rheumatoid arthritis , characterized by chronic joint pain.
If a patient with Lyme is diagnosed with RA without the Lyme being detected and treated, not only can the arthritic symptoms of Lyme persist and worsen, but the Lyme can also go on to affect more systems, causing neurological and psychiatric symptoms, heart problems, and more. In rare cases, untreated Lymecan even be fatal.
Also Check: Late Stage Lyme Disease Test
Lyme And Autoimmune Disease
When pathogenic infections invade tissues, the bacteria produce LPS which are found on their outer cell membrane and promote inflammation. These molecules are produced and fool the hosts immune system into thinking that there is a foreign invader. The body natural mounts an immune response, but the response is against its own tissue, yielding autoimmune disease.
Frequently we see autoimmune diseases associated with Lyme Disease and coinfections such as: MS, Lupus, Hashimotos Thyroiditis, Scleroderma, Graves Disease, Celiac Disease, etcEssentially, any tissue in the body can fall prey to autoimmune disease if the autoimmunity is driven by infection.
In 18 years of practice, most of my patients autoimmune conditions are completely erradicated with proper longterm antibiotic use as well as targeted nutraceuticals. If you decrease the infection in the tissue, the concentration of LPS decreases, inflammation decreases, and tissues can return to their healthy state. If infection is allowed to persist, autoimmune disease simply gets worse.
It is my belief that most if not all autoimmune disease is infection driven. The challenge becomes to identify the exact pathogen and then treat accordingly.
MOUNT VERNON LOCATION:
Addressing Autoimmune Disease And Lyme: Conventional Versus Holistic Healthcare Measures
Autoimmune disease and Lyme could cause some serious neurological damage as well as leave you with a few autoimmune-related health issues causing damage to joints, bones, gut, muscles, and bones. Please remember, however, that you would not present all the various complications arising from this bacterial infection. But you may have a few.
Conventional medicine, to a large extent, depends on the use of antibiotics in addressing the bacterial infection and then addressing the arising symptoms separately. The use of the medications used in treating the various associated symptoms could have their own set of contraindications and side effects. These, unfortunately, could result in you feeling worse while your weakened body tries its best to counteract them.
The holistic approach is quite different. It is one that looks at your diet, lifestyle, and environmental factors that could worsen your condition. This approach, although seemingly general in nature, helps the body to heal itself and get out of the cycle of self-destruction caused by a cyclical immune response. Other holistic approaches include ozone therapy, low-level laser therapy, and herbal supplements. With any approach, it’s important to consult with your healthcare provider as each body is different and you might need a blend of both approaches.
Recommended Reading: Deer Ticks Carry Lyme Disease
Is Lyme Disease Autoimmune
The relationship between Lyme disease and autoimmunity is controversial. Some researchers in the Lyme disease space claim that chronic Lyme disease doesnt exist. They argue that people previously infected with Lyme disease who experience symptoms beyond the standard course of antibiotics are suffering from a purely autoimmune phenomenon, referred to as post-treatment Lyme disease or a post-Lyme autoimmune syndrome. However, those who argue for the existence of post-Lyme autoimmune syndrome dont ask, what might be the cause of the autoimmunity? The term post-Lyme autoimmune syndrome discredits the possibility of chronic, ongoing Lyme disease infection as an autoimmune trigger. So what is the truth? Can chronic Lyme disease cause autoimmunity?
Lyme disease is known to evade antibiotic treatment and persist in the body, creating a chronic infection. As well discuss shortly, there are several known mechanisms through which chronic infections trigger autoimmune processes. Based on the available research, it is highly likely that chronic Lyme disease triggers autoimmunity, NOT that autoimmune disease spontaneously appears after Lyme treatment, in the absence of ongoing infection.
How does Lyme disease trigger an autoimmune response? Here are a few mechanisms linking Lyme disease and autoimmune disease:
Lyme Disease And Other Tick
Ticks are a type of arachnid that have evolved to feast on blood. A tick bite in itself is harmless, but the bacterial and viral infections that can result range from mildly inconvenient to deadly.
The majority of human infections happen in spring and summer when the ticks go through the nymphal stage, and are the size of a poppy seed. Ticks can be hard to identify in the larval or nymphal stages.
If you find a tick attached to your skin, the best way to remove it is with a pair of tweezers, and ensure that you clean and protect the wound after. Do not squash the tick, as this can also transmit disease. Read on to learn about Lyme disease and other tick-borne diseases.
Don’t Miss: How To Cure Lyme Disease Naturally
Legal Mandates To Cover Unproven Treatments
The state of Connecticut, meanwhile, enacted a law on June 18, 2009, “to allow a licensed physician to prescribe, administer or dispense long-term antibiotics for a therapeutic purpose to a patient clinically diagnosed with Lyme disease.” The states of Rhode Island, California, Massachusetts, New Hampshire, Vermont, New York, Maine, and Iowa have similar laws.
Massachusetts and Rhode Island have laws mandating insurance coverage for long-term antibiotic therapy for Lyme disease when deemed medically necessary by a physician. In 1999 Connecticut had passed a similar, though somewhat more restrictive law.
New Thoughts On Lyme Disease And Autoimmune Illnesses
by Dr. Rogers | May 3, 2021 | Chronological, Primary Care |
Morning everyone!
Welcome to another edition of the Doctors Note where we talk about whats on our minds when it comes to your health.
This week were going to be talking about something that doctors hate to see come into their office. They cringe when people come in and say they have this disease, and thats Lyme disease.
A lot of my new research on Lyme disease is based on a book I finished a few months ago called Chronic by a prominent Yale Epidemiologist, Dr. Steven Phillips and Dana Parish.
Also Check: Fasting To Cure Lyme Disease
Lyme Disease Alters Immune Cell Communication
Recent research out of Johns Hopkins University indicates that Borrelia burgdorferi alters communication between two types of immune cells dendritic cells and T-cells. Dendritic cells are cells that process antigens, toxic or foreign substances that induce an immune response in the body. Examples of antigens include bacterial toxins and food proteins. After processing antigens, dendritic cells pass the antigens on to T-cells, which are specially trained cells that are able to target and destroy specific pathogens. Borrelia appears to interfere with the normal communication between dendritic cells and T-cells, causing the receptors on dendritic cells to change structurally and induce T-cells to attack healthy cells in your own body.
Cunningham Panel Results Indicate Lyme Disease May Trigger Autoimmune Dysfunction
This newly published study, which examined Lyme disease and the immune system, illustrates molecular mimicry targeting neural tissue after Borrelia burgdorferi infection. The authors test the hypothesis that autoantibodies produced in patients with early Lyme disease and Post-Treatment Lyme Symptoms cross-react with neuronal antigens and potentially lead to Lyme disease sequelae. The authors conclude that patients with Lyme disease have a greater frequency of certain anti-neuronal autoantibodies and functional neuronal activation compared to community controls without a history of Lyme disease 1.
Elevated autoantibody results measured by the Cunningham Panel in this study included anti-lysoganglioside GM1, anti-D1R, and anti-D2R. Elevated CaMKII activation suggests that antineuronal antibodies have functional significance.
A heightened immunological response triggered by repeated infection with Bb may increase the risk for neurologic and neuropsychiatric symptoms among patients with previously treated LD .
This study examined 179 serum samples for the presence of Lyme disease and immune system reactivity. Patients were assigned to one of four groups:
Also Check: Realtor Com East Lyme Ct
How To Treat Lyme Disease To Fight Autoimmunity
Ill be honest with you, Lyme is one of the most complex conditions to treat and it takes time and hard work.
Simply prescribing an antibiotic doesnt do the trick once inflammation is systemic, the condition is chronic, or there are autoimmune complications involved.
You need a holistic approach that supports your immune system from the ground up so that your body can fight back against the disease and restore a normal inflammatory response.
This includes eating a nutrient-rich, anti-inflammatory diet, relieving stress, getting plenty of sleep, promoting detox, and overcoming any underlying deficiencies and imbalances.
That being said, Ive seen patients make tremendous progress with a functional medicine approach to Lyme disease.
The patient I mentioned earlier is currently leaps and bounds from where she was before. She is now living life how she wants to, as opposed to what her body and illness was letting her do before.
About the Author: Dr. Seth Osgood is a Doctor of Nursing Practice, Board Certified Family Nurse Practitioner and Institute of Functional Medicine Certified Practitioner. Dr. Osgood received his post-graduate training in Functional Medicine through the IFM and from working with Dr. Amy Myers. He has helped people from around the world improve their health utilizing a Functional Medicine approach.
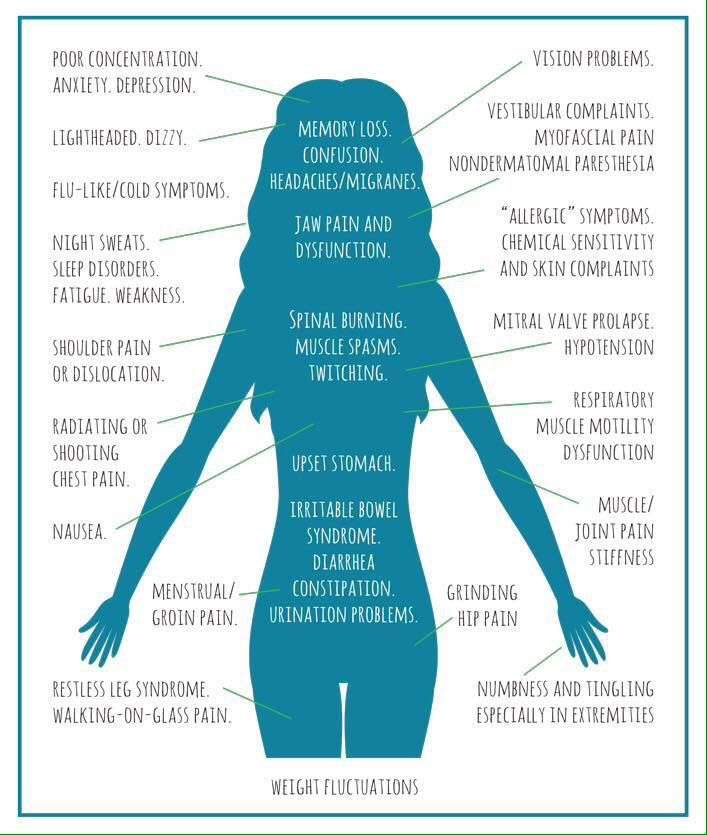
Symptoms Of Lyme Disease
Early symptoms of Lyme disease typically present as a circular red skin rash around a tick bite called Erythema migrans. This red, circular, or oval-shaped rash often expands over a period of days and can reach up to 12 inches across. Sometimes the center clears as it enlarges resulting in a bull’s-eye appearance. It’s typically not itchy or painful but may feel warm to the touch. Some people develop this rash at more than one place on their bodies. The rash can appear up to a month after you’ve been infected, but it usually occurs within one to two weeks and can last for several weeks.
Not everyone with Lyme disease gets the rash. You may also have flu-like symptoms in the first few weeks of infection, such as tiredness, muscle pain, headaches, high temperature , chills, swollen lymph nodes, and joint pain .
A few people with Lyme disease develop more serious symptoms weeks, months, or even years later. These include:
- Severe headaches and muscle pain
- Problems affecting the brain or nerves, such as memory problems, difficulty concentrating, and dizziness
- Pain in the joints and muscles often in the knees
- Heart problems such as heart palpitations, chest pain, and shortness of breath
- Inflammation of the membranes surrounding the brain and spinal cord
Disease signs and symptoms can appear quickly or gradually over time, and they are different for everyone.
Left untreated, Lyme disease may spread to your heart and nervous system.
Read Also: How Long Do Lyme Disease Test Results Take