When Should I Call The Doctor
If a tick bites you, call your doctor. Other conditions can cause similar symptoms, so it’s always a good idea to discuss them with your doctor. That way you can get checked and treated, if needed. Call right away if you get a red-ringed rash, lasting flu-like symptoms, joint pain or a swollen joint, or facial paralysis.
Be Ready For Trial And Error
Lyme-related joint pain takes time to both diagnose and treat. In the meantime, there are many things you can do to decrease inflammation and pain. As every Lyme patient is different, try not to get too frustrated if what works for someone else doesnt work for you. Be patient as you experiment with diet, herbs, exercise, alignment, and releasing tight fascia. You will find tools that help you. Reach out and surround yourself with people who understand you and are on your side. We are all healing together.
Lyme Disease And Rheumatoid Arthritis: Similarities Differences And Why A Misdiagnosis Can Be Deadly
Home » Tick Talk » Lyme Disease and Rheumatoid Arthritis: Similarities, Differences and Why a Misdiagnosis Can be Deadly
Because its symptoms mimic those of so many other diseases both tick-borne and otherwise Lyme disease is often misdiagnosed. One of the most common Lyme disease misdiagnoses is Rheumatoid Arthritis , a chronic condition with less clear causes than Lyme disease.
Though there are many fundamental differences between these two conditions, its true that arthritic pain stemming from Lyme disease can often look like RA. In fact, Lyme was first discovered and documented in part because of a group of children presenting with arthritis symptoms in Lyme, Connecticut.
So, if youre experiencing joint pain, how can you tell the difference? If youve been bitten by a tick or think youre at risk for a tick-borne disease, its extremely important not to delay seeking medical attention or ignore any arthritic pain that might be associated with Lyme disease. Continue reading to better understand the differences and similarities between Lyme disease and arthritis.
Lyme Disease: Causes and Risk Factors
Lyme disease is a tick-borne infectious disease caused by the spiral-shaped bacteria Borrelia burgdorferi sensu lato. Though Lyme is treatable with antibiotics, it can worsen, change symptoms, spread to the neurological system, become a chronic condition, and even become life-threatening if not diagnosed and treated right away.
Common Symptoms of Lyme Disease
You May Like: What Tests Are Done For Lyme Disease
Risk Factors For Early Disseminated Lyme Disease
Youre at risk for early disseminated Lyme disease if youve been bitten by an infected tick and remain untreated during stage 1 of Lyme disease.
Youre at an increased risk of contracting Lyme disease in the United States if you live in one of the areas where most Lyme disease infections are reported. They are:
- any of the Northeastern states from Maine to Virginia
- the north central states, with the highest incidence in Wisconsin and Minnesota
- parts of the West Coast, primarily northern California
Certain situations also can increase your risk of coming into contact with an infected tick, such as:
- gardening, hunting, hiking, or doing other outside activities in areas where Lyme disease is a potential threat
- walking or hiking in high grass or wooded areas
- having pets that may carry ticks into your home
Lyme Disease And The Cdc
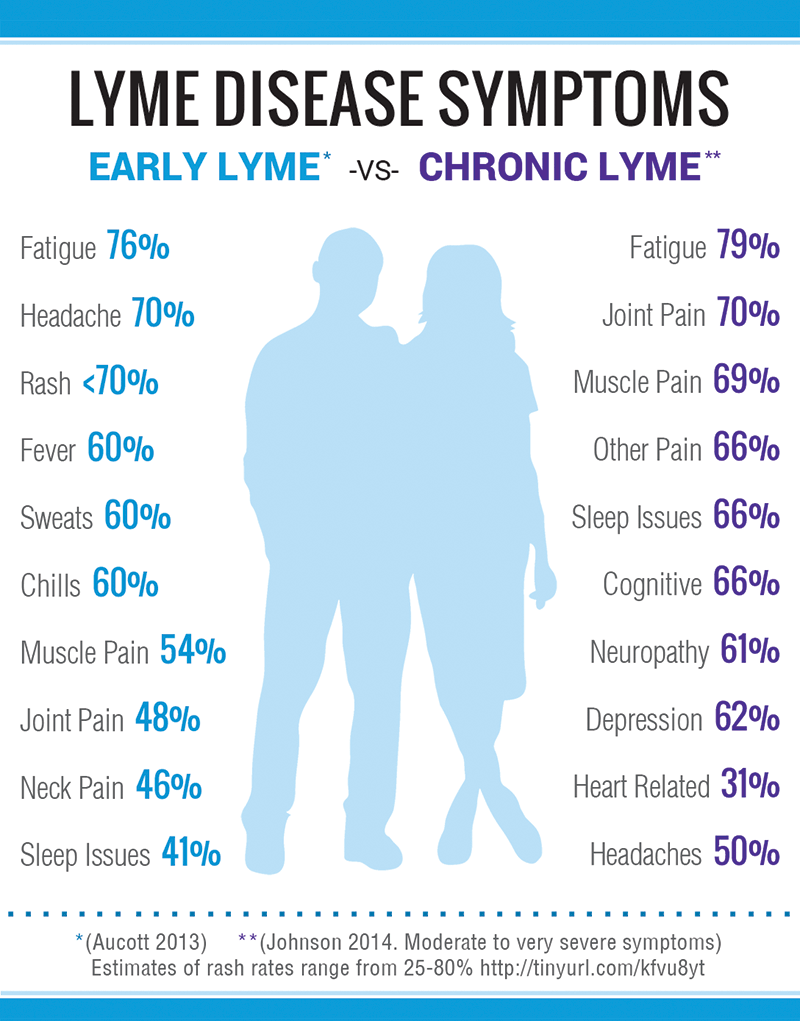
In order for the Centers for Disease Control to recognize a Lyme case for surveillance purposes, there must be objective findings, such as positive blood tests, Bells palsy or joint swelling . The chart below reflects the CDC-reviewed surveillance case manifestations from 2001 to 2010.
This situation contributes to what many experts view as severe undercounting of Lyme disease by the CDC.
Recommended Reading: Antibiotics For Lyme Disease In Humans
Chronic Lyme Pain & Headaches
The pain caused by Lyme disease and other tick-borne illnesses can be widespread and excruciating. It can affect muscles, joints, nerves and bones, and manifest in any area of the body. Treatment varies greatly depending on the type and severity of the pain, but it is important to take a multi-faceted approach. Medications and various alternative therapies all have their place in the treatment of pain symptoms. Pain medicine specialists can help determine the best treatment.
Pain can have a damaging impact on the immune system, adding to the importance of effectively treating it. Pain management is absolutely essential to those with compromised immune systems, because the pain experience further reduces the immune reaction. If you have Lyme disease pain, you are less likely to be active, to sleep properly, or to eat properly because your mind is constantly trying to fight off the pain response. There is little time for anything else, and it is consuming.
Absence, or at least management, of pain is a health necessity, especially in the sleep response. You can’t heal if you can’t sleep properly. And, your body is on constant alert, which imposes extra stress levels, which further reduces immunity! It’s a viscious circle!
What Are Signs And Symptoms Of The Third Stage Of Lyme Disease
Late stage Lyme disease can result when treatment is unsuccessful or started too late due to unrecognized symptoms or misdiagnosis. The late disseminated stage occurs months or years after initial infection and can have a major impact on a patients health and quality of life. Late Lyme arthritis is a third stage Lyme disease manifestation that involves fluid accumulation and pain in joints, particularly in the knee joints. Late neurologic disease is a 3rd stage condition that can also be debilitating and difficult to diagnose. Late disseminated Lyme disease symptoms include a variety of symptoms that are often neurologic in origin including: numbness in extremities, mental fogginess and concentration problems, and difficulty following conversations or processing information.
Also Check: What Does Lyme Disease Do To You
Synovial Fluid Analysis Imaging And Other Tests
On presentation, joint aspiration is usually done for diagnostic purposes to rule out the presence of other arthritides such as crystalline arthropathy or staphylococcal septic arthritis. Joint fluid white cell counts are usually inflammatory in the range , but cell counts as low as 500 or as high as 100,000 cells/mm3 have been reported. Although tests for rheumatoid factor or antinuclear antibodies typically yield negative results, antinuclear antibodies in low titer may be detected. Peripheral white blood cell counts are usually within the normal range, but inflammatory markers, such as ESR and CRP, may be elevated. Imaging studies are not required for diagnosis or are not typically performed. The major reason for imaging studies in Lyme arthritis is when there are concerns for alternative diagnoses.
In patients with Lyme arthritis, plain films, MRI scanning or ultrasound typically show non-specific joint effusions, while MRI studies utilizing contrast dye, may display synovial thickening or enhancement. In adult patients, imaging studies may show co-incidental degenerative changes or chronic mechanical injuries, but these abnormalities would not be expected to cause significant synovitis or inflammation. Lyme arthritis is not rapidly erosive, but with longer arthritis durations, joint damage can be seen on radiographic studies. Finally, MRI scanning may be useful in the planning of synovectomies by determining the extent of synovitis within the joint.
How Is Lyme Arthritis Treated
Most children with Lyme arthritis recover after 28 days of antibiotic treatment. The most common antibiotics prescribed for Lyme disease are:
- Doxycycline for children eight years of age or older
- Amoxicillin for children under eight years of age
If the symptoms persist after a course of antibiotics, a second course of antibiotics may be prescribed.
In persistent cases of Lyme arthritis, your rheumatologist may prescribe non-steroidal anti-inflammatory drugs , disease-modifying antirheumatic drugs , or intra-articular corticosteroids.
Don’t Miss: At Home Lyme Disease Test
Facts About Lyme Disease In Pa
Ticks thrive in the countryside of Pennsylvania in particular, and according to a study published in the Proceeding of the National Academy of Sciences of the United States of America , Lyme has a greater likelihood of occurring where suburban developments encroach on existing forest. This is thought to be because the white-footed mouse that is the most important animal in the Lyme disease transmission cycle can live without too many predators under these circumstances.
Notable statistics of Lyme disease in PA include:
- Fatigue
- Swollen lymph nodes
For some people, a telltale sign of the disease is the red bulls eye-shaped skin rash that presents in some, but not all sufferers, within three to 30 days after being bitten by a tick.
Often, these first signs are missed when youre infected with Lyme disease and are dismissed as the flu or some other virus. This is very worrying because if antibiotic treatment isnt begun when the first signs of the disease present, your condition can become more serious.
Joint pain is another issue that can occur with Lyme disease. In the worst cases, over several weeks, nervous system and heart issues can develop. If left untreated, you may suffer from arthritis and neurological issues. In fact, according to the Arthritis Foundation, when Lyme disease is untreated, more than half of all sufferers will develop sporadic arthritis bouts.
Joint Pain Or Arthritis
If you start experiencing joint pain or symptoms of arthritis after you’ve completed treatment for Lyme disease, it could be PTLDS. While it’s rare for people in their 20s and 30s to develop suddenly arthritis, WebMD reported that at least half of people with Lyme disease get some form of arthritis. “Often the pain and joint stiffness can be felt all over, but sometimes itâs just in certain joints, like the knees. It usually goes away, but in some people, the arthritis may continue.”
Read Also: Where Can You Get A Lyme Disease Test
How Is Morphea Diagnosed
If you have unexplained hard or discolored patches of skin, your doctor may refer you to a dermatologist or a rheumatologist .
Your doctor is likely to ask you questions about your symptoms, such as when you first started noticing changes in your skin, if youve done anything to treat yourself, and if you have any other symptoms. Theyll ask for a family health history and about any recent illnesses youve had and any medications youre taking.
There is no test for diagnosing morphea. Your doctor will examine your skin and, though not usually necessary, might take a small sample to have analyzed by a lab. This is called a skin biopsy.
They may also order some tests to help distinguish morphea from something called systemic scleroderma. This type of scleroderma is similar to morphea at first. But it can later affect internal organs and requires more aggressive treatment.
Morphea with deep lesions, lesions on your face or neck, or widespread lesions can lead to:
- restricted joint mobility
- permanent eye damage in children
- hair loss
Often people with morphea also have genital lichen sclerosis, which can cause itching and burning and changes to your skin. Its important to tell your doctor about these symptoms if you have morphea.
Fragments From Lyme Bacteria Persist In Joints Even After The Bacteria Are Killed Off
A new study published in Proceedings of the National Academy of Sciences sheds light on this medical mystery. To keep from spilling open, bacteria have rigid cell walls made of a matrix of protein and sugars, called peptidoglycan. Most bacteria recycle their peptidoglycan when they grow and divide, but the peptidoglycan of B. burgdorferi has a peculiar structure, and the bacteria is unable to reuse it. Instead, it dumps it into its immediate surroundings, like a microbial litterbug.
This peptidoglycan collects in the joints where B. burgdorferi is found. Almost all patients in the PNAS study with Lyme arthritis had peptidoglycan in their joint fluid. Most of them also had specific antibodies to peptidoglycan in the joint fluid, suggesting that the peptidoglycan was driving the inflammatory process. These antibodies were not found in fluid from people with other joint conditions, such as rheumatoid arthritis, osteoarthritis, or gout.
Patients with Lyme arthritis who did not get better with antibiotics still had peptidoglycan in their joint fluid. However, their joint fluid did not contain detectable B. burgdorferi DNA. This suggests that even after the bacteria were killed off, the peptidoglycan stayed behind, and stimulated further inflammation. This may explain why people with Lyme arthritis who do not respond to antibiotics may improve with medications that damp down the immune system, such as methotrexate or TNF inhibitors.
Don’t Miss: How To Know If I Have Lyme Disease
Older Adults Vulnerable To Lyme Disease
For most people, Lyme disease will result in no lasting illness after some initial flu-like symptoms. But for others, it can become debilitating if left untreated. Older adults can be particularly vulnerable, and they may brush off the effects. Symptoms of Lyme disease that has progressed include short-term memory loss, joint pain or swelling, and fatigue signs often attributed to aging.
You might start thinking, I’m just beginning to lose my memory a bit. And everybody does that as they get older, said Dr. Brian Fallon, a psychiatrist and director of the Lyme and Tick-Borne Diseases Research Center at Columbia University.
Other long-term effects include chronic pain, irregular heartbeat, brain fog, shooting pains or numbness in the arms or legs, and severe headaches.
Early Detection Is Key
Stephen Morse, PhD, an epidemiologist at the Columbia University Mailman School of Public Health, said that the findings were reassuring.
The general wisdom about it was even if you didnt find the tick immediately it would take about 48 hours, to contract Lyme disease, said Morse. This seems to be true here, too.
Morse said the data can help to inform people on how to enjoy the outdoors safely.
He pointed out that in areas with high numbers of ticks, people may need to take precautions even if they just go into their own backyards.
If youve got a nice backyard, use that mosquito repellent or bug repellent, he said.
In addition, there are obviously the usual precautions of dont leave a lot of exposed skin, and be careful if youre climbing the underbrush.
Recommended Reading: Is Lyme Disease Curable In Humans
Lyme Disease Vs Rheumatoid Arthritis
Lyme disease can sometimes be confused for other conditions, and its not uncommon for patients presenting with Lyme disease-related joint pain to be misdiagnosed with rheumatoid arthritis . Both Lyme and RA cause joint pain and can be debilitating when left untreated, but there are differences.
- Lyme arthritis tends to manifest in larger joints , on one side of the body. Lyme joint pain tends to come and go.
- Rheumatoid arthritis occurs more often in the hands, feet, fingers, and toes, and shows up on both sides of the body. RA joint pain and stiffness occurs every day, and is usually chronic.
- Lyme disease usually goes away when treated, and most patients make a full recovery.
- Rheumatoid arthritis treatment can manage symptoms and show the progression of the disease, but there is no cure.
Lyme pain can often migrate throughout the body, and patients may have pain in their knee one week, and in their wrists the following week, says Chicago-based integrative medicine specialist Casey Kelley, MD. With rheumatoid arthritis, the pain often stays where it begins and does not migrate.
Getting Lyme puts you at greater risk for later developing RA and other types of inflammatory arthritis. One study found that nearly one-third of participants who had Lyme-arthritis later developed an inflammatory arthritis.
Lyme disease symptoms typically begin 3-30 days after youve been bitten by a tick. Early symptoms of Lyme disease include:
- Bulls eye rash
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040″ rel=”nofollow”> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Recommended Reading: Costco Pharmacy East Lyme Ct
Diet & Targeted Exercise Can Help Lyme
If you have Lyme disease, discuss a protocol for killing the bacteria with your doctor. Of course, this is imperative for eliminating symptoms.
That said, most Lyme protocols take time, and there is much more you can do during treatment to mitigate symptoms of pain.
For instance, Dr. Farshchians clinic advises people with Lyme arthritis to decrease any environmental factors that may contribute to inflammation, such as mold exposure or mast cell activation . Addressing common comorbidities often makes a significant improvement in symptoms, she says. In addition, her clinic aims to help patients reduce inflammation organically through diet, lifestyle, anti-inflammatory herbal supplements, medications, light therapy, Epsom-salt baths, and exercise.
In my experience and that of my clients, all these approaches can be helpful. Below are a few of my favorite strategies.
1. Rolling with a foam roller
One thing you can easily do at home is to roll tight tissue in your body with a foam roller. This helps to lengthen and release tension in your fascia, or connective tissue.
Rollers are inexpensive and available online. Just play with gently rolling the muscles surrounding painful joints, or really any sore muscles at all, with the roller. If you need ideas for how to experiment with this, this video demonstrates my favorite ways to roll.
2. Gentle strengthening