The Case Study Pathology Is Characteristic Of Dementia With Lewy Bodies
The fresh brain weighed 996 g and appeared atrophic Coronal sections through the left cerebral hemisphere and brain stem revealed mild enlargement of the lateral ventricle, particularly the temporal horn. The substantia nigra was normally pigmented or nearly so. Microscopically, nigral and cortical Lewy bodies, were seen with hematoxylin and eosin stain . Immunohistochemistry for -synuclein showed numerous immunoreactive Lewy bodies and fibers in substantia nigra, hippocampal formation and neocortex, Figures 4CE). IHC for hyperphosphorylated tau revealed intense staining of many limbic neurofibrillary tangles and neuropil threads , and of occasional neurofibrillary tangles in neocortex, but senile plaques were extremely rare, and each contained only a few fibrils . H& E showed prominent thickening of small blood vessels in gray and white matter, extensive mineralization of pallidal vessels, and rare microglial nodules in the hippocampal formation. Immunohistochemistry for Iba-1 , CD68 , and CD163 showed moderate numbers of activated microglia and large numbers of macrophages in hippocampal formation and spinal cord . In summary, we see DLB accompanied by features of Alzheimer’s disease, a common presentation.
Post Treatment Lyme Disease
Lyme disease, especially when treated early, often responds to antibiotic therapy, whereas MS does not. Not everyone who is treated for Lyme disease fully recovers. Sometimes there are Post Treatment Lyme Disease symptoms that can be vague and look like other illnesses. The majority of people, however, recover to lead a normal life.
How Lyme Disease Affects The Brain
Did you ever wonder how Lyme disease affects the brain, including symptoms of brain fog? The U.S. Centers for Disease Control and Prevention estimates that about 200,000 people are diagnosed every year with Lyme disease.
But many believe the true number of people suffering from Lyme in the United States is actually much higher. Thats because Lyme disease symptoms vary greatly and can impact different people in different ways. Aside from that, the ELISA screening test most doctors use misses up to 35 percent of Lyme cases, making it a horrible first-line detection for the disease.
The problem is likely only going to get worse, too, being that Lyme is among the major health effects of climate change.
Even with many cases missed in the doctors office, Lyme disease is still the most common tickborne disease in the northern hemisphere. Despite being so common, Lyme disease symptoms vary depending on the patient and how the bacteria impacts different systems of the body. In fact, Lyme disease often mimics other diseases or illnesses and be referred to as the new great imitator.
Lyme disease is often misdiagnosed as such diseases, including:
- Chronic fatigue syndrome
- Autism-like syndromes
- Various psychiatric illnesses
Recommended Reading: What Are The Lasting Effects Of Lyme Disease
Lyme Sci: When Brain Inflammation Persists After Lyme Disease Treatment
In a new study, researchers from the Johns Hopkins School of Medicine have found evidence of chemical changes and widespread inflammation in the brains of patients with chronic symptoms following treatment for Lyme disease.
This Johns Hopkins study, in Journal of Neuroinflammation, supports the experience of hundreds of thousands of patients who have tried for years to have their chronic symptoms of pain, sleep disturbance, fatigue, and cognitive impairment validated.
What this study does is provide evidence that the brain fog in patients with post-treatment Lyme disease syndrome has a physiological basis and isnt just psychosomatic or related to depression or anxiety, says John Aucott, M.D., a senior author of the new paper and director of the Johns Hopkins Lyme Disease Research Center.
The fact is, too many patients with Lyme disease are left with chronic, debilitating symptoms following treatment for Lyme disease. In the nearly 40 years since the discovery of Lyme, no one has been able to determine why some patients get better with treatment and others remain ill.
Rnascope Is A Sensitive Technique For Finding Viable Pathogen But Requires Freshly Prepared Tissue
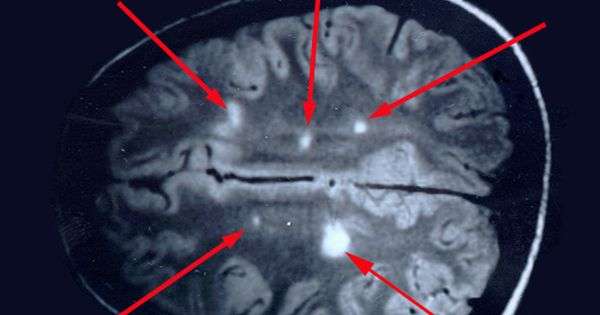
Figure 8. Validation of RNA integrity on Fresh frozen NHP frontal cortex brain tissue using RNAscope assay. NHP tissue was stained with a 3-plex positive control probe POLR2A targeting DNA-directed RNA polymerase II RPB1, PPIB targeting cyclophilin B, and UBC that targets Ubiquitin C. In terms of relative expression levels, UBC is highest, PPIB is considered a moderate-high, POLR2A is moderate-to low expressor target. Successful staining has 49 dots per cell of PPIB/POLR2A and UBC of 1015 dots per cell. PPIB is considered a standard to determine the RNA quality of brain samples. Represents red fluorescence, indicating the specificity of PPIB, whereas, displays a far-red puncta targeting UBC gene. Absence of POLR2A signal in represents, quality of RNA being partially compromised. A merge image of all the channels can be seen in . White arrows were pointing toward the fluorescence puncta and orange arrows toward autofluorescence of the tissue.
The Patient Harbored Borrelia in the Amygdala and Spinal Cord
Tissue slices adjacent to the autopsy tissue specimens that were positive for DNA were stained for the presence of persisters. For this, slides were stained with the primary rabbit polyclonal antiB. burgdorferi antibody and a goat anti-rabbit IgG-Alexa Fluor 488 secondary antibody. An intact Borrelia spirochete with the expected morphology was identified within fixed tissue of the spinal cord . The spirochete appeared to be adjacent to vasculature.
Don’t Miss: What To Do If You Have Lyme Disease
Immunofluorescent Detection Is The Most Reliable Method To Detect Spirochetes In Fixed Tissues
To strengthen the results of our PCR, we next explored immunofluorescence assay to see if these tissue specimens contain morphologically intact spirochetes. Initially, we tested our rabbit polyclonal antibody on NHP frontal cortex tissue that was incubated with borrelial spirochetes to see the specificity of the antibody . The image cleanliness was increased after incubating the tissue with the lipofuscin quencher that quenches the fluorescence of lipofuscin aggregates, which are formed during normal aging process . Secondary antibodies were tested with isotype controls for specificity on human and macaque . Optimal fixation time is very crucial for the success of the IFA. Tissues must be properly fixed under-fixation leads to tissue deformation, shrinkage and autolysis , whereas over-fixation may permanently mask the antigen, abolishing its detection even after antigen-retrieval steps .
When It Looks Like A Brain Tumor But It Is Lyme Disease
Pseudotumor cerebri, also referred to as idiopathic intracranial hypertension, is a condition caused by elevated cerebrospinal fluid pressure in the brain. Symptoms can mimic a brain tumor, but in actuality there is no tumor. Instead, there is unexplained intracranial pressure in the head. The condition is rare in prepubertal children.
Ezequiel and colleagues report on the case of a 9-year-old boy from Portugal who was diagnosed with pseudotumor cerebri due to Lyme disease. The child was admitted with daily pulsatile frontotemporal headache, pallor, photophobia and phonophobia, without night awakening, vomiting or visual changes, writes Ezequiel in the British Medical Journal Case Reports.
His neurological examination revealed papilloedema but was otherwise normal. Brain images were unremarkable. Serologic, PCR and cultural testing ruled out bacterial and viral agents including Mycoplasma pneumoniae, Epstein-Barr virus,Cytomegalovirus and Enterovirus. So the boy was prescribed acetazolamide .
However, ELISA and Western blot results were positive for B. burgdorferi antibodies, the bacteria causing Lyme disease. The diagnosis of neuroborreliosis was assumed, explains Ezequiel and a 21-day course of intravenous ceftriaxone was started. The boy made a complete recovery.
The authors highlight several key points:
References:
Read Also: My Dog Has Lyme Disease
Lyme Disease Effects On The Brain
The first section of Lyme Brain discusses the fundamentals. What actually causes this condition? Research has shown that Lyme spirochetes can invade the brain and wreak all kinds of havoc. They damage nerve cells, trigger inflammation, release neurotoxins, and disrupt the balance of brain chemicals.
Ducharme lays all this out in plain language. She also explains how co-infections contribute to Lyme disease brain:
One of the reasons I believe that the actual brain fog, memory issues and difficulty with focus and concentration is Borrelia driven is because when I treat my patients with medications that primarily impact Borrelia and cross the blood-brain barrier, I see these symptoms improve, whereas the insomnia and wacky dreams tend to respond more to Babesia treatment. Really extreme psychiatric symptoms such as rages, and suicidal thoughts and behaviors, respond mostly to Bartonella treatment.
Insights On Neurological Lyme Disease
She rounds out her discussion of these issues by interviewing five professionals who know a lot about neurological Lyme disease. One is psychiatrist Robert Bransfield, MD, a top expert on how Lyme affects the brain . Another is Sandra Berenbaum, LCSW, with whom I co-authored the book When Your Child Has Lyme Disease: A Parents Survival Guide. Others are Leo Shea, Ph.D., who has extensive experience with neuropsychological testing of children and adults with Lyme disease health advocate/blogger Scott Forsgren, founder of BetterHealthGuy.com, who writes extensively on Lyme-related issues and Connie Strasheim, author of many books about Lyme disease. They all offer useful insights on the topic of Lyme disease brain.
Throughout the book, Ducharme offers practical information with a strong helping of optimism. As she writes early on:
I find that the majority of people with Lyme brain can find resolution or, at the very least, significant improvement of their symptoms.Im not saying its quick or easy, but I have seen remarkable improvements in people who started out very, very ill with horrible Lyme brain and are now back at work, running their families and living their lives as productive, happy people.
If you or a loved one has a problem with neurological Lyme disease symptoms, I think youll find this book both helpful and hopeful.
Also Check: What Happens When You Have Lyme Disease
Why Accurate Ms Diagnoses Are Challenging
There is no single test for MS, so an accurate MS diagnosis can be challenging. Results of a recently study published in the Journal Multiple Sclerosis and Related Disorders suggested that nearly 1 in 5 people with other neurologic conditions are mistakenly diagnosed with MS.1 The confusion also means that many people also live with symptoms for months or years before an official MS diagnosis can be confirmed.
Visualizing Brain Fog In Post
More than one in 10 people successfully treated with antibiotics for Lyme disease go on to develop chronic, sometimes debilitating and poorly understood symptoms of fatigue and brain fog that may last for years after their initial infection has cleared up.
Now, a Johns Hopkins team has used an advanced form of brain scan to show that 12 people with documented post-treatment Lyme disease syndrome all show elevation of a chemical marker of widespread brain inflammation, compared with 19 healthy controls.
Results of the study, published in Journal of Neuroinflammation, suggest new avenues for treating the long-term fatigue, pain, sleep disruption and brain fog associated with PTLDS. Theres been literature suggesting that patients with PTLDS have some chronic inflammation somewhere, but until now we werent able to safely probe the brain itself to verify it, says Jennifer Coughlin, a senior author and associate professor of psychiatry and behavioral sciences.
What this study does is provide evidence that the brain fog in patients with post-treatment Lyme disease syndrome has a physiological basis and isnt just psychosomatic or related to depression or anxiety, says John Aucott, director of the Johns Hopkins Lyme Disease Research Center.
In addition, the results suggest that drugs designed to curb neuroinflammation may be able to treat PTLDS, although clinical trials are needed first to determine the safety and benefit of such therapy, Aucott says.
You May Like: Can Lyme Disease Cause Jaw Pain
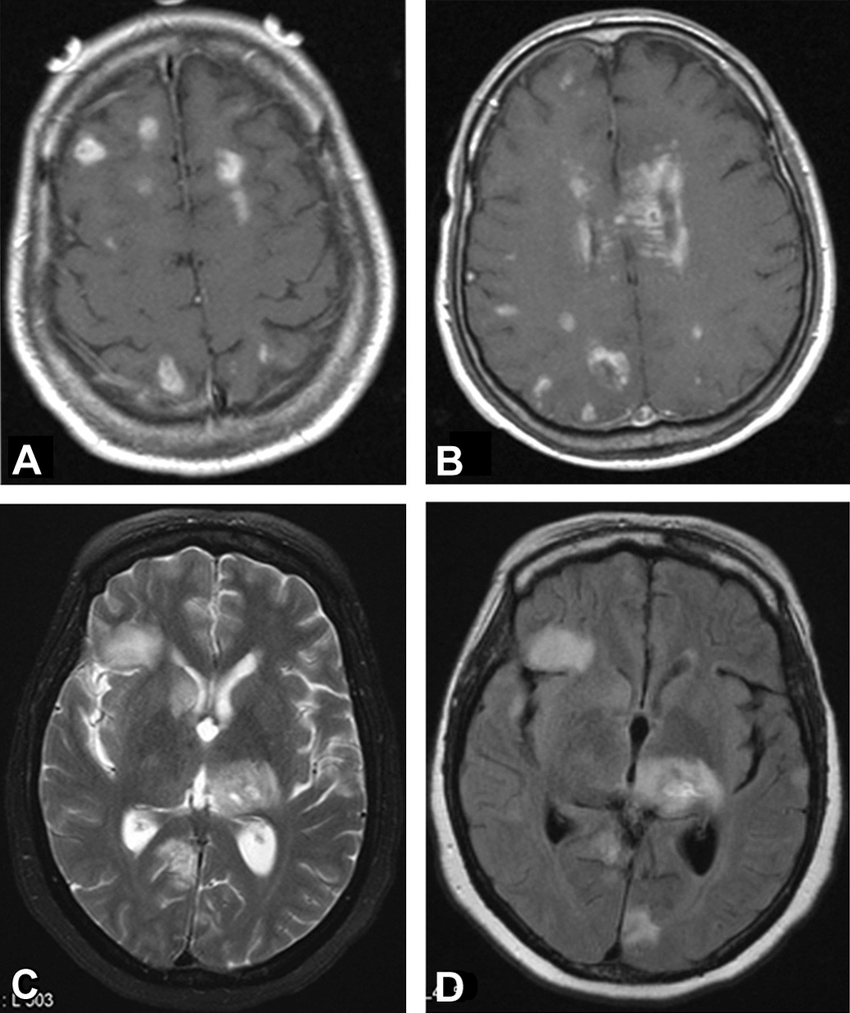
Mri Findings In Lyme Neuroborreliosis
Section
Clinical Cases
Paternain A1, Villino R2, Riverol M2, Malmierca P1, Soriano I1, Calvo-Imirizaldu M1, García-Eulate R1, Domínguez PD1
1. Department of Radiology, Clínica Universidad de Navarra, Spain
2. Department of Neurology, Clínica Universidad de Navarra, Spain
Connected authorsArea of InterestImaging TechniqueProcedureSpecial Focus
A 22-year-old woman was admitted to the emergency room with sudden right peripheral facial palsy. She also referred to progressive and ascending burning pain in the spine for two weeks. After a trip to the mountains one month before, she had developed an erythematous skin lesion that resolved spontaneously.
MRI of the spine showed a diffuse enhancement of all nerve roots after contrast administration, without a significant thickening . In the brain, bilateral enhancement of the trigeminal nerves in the posterior cranial fossa was also appreciated. In addition, there was also an abnormally high signal intensity in FLAIR surrounding the cerebral aqueduct of Sylvius .
A lumbar puncture was performed, which showed a positive serology for Lyme disease. The patient was treated with intravenous ceftriaxone for two weeks, followed by oral doxycycline for another 2 weeks, having a complete clinical response afterwards.
Epidemiology And Clinical Presentation
More than 200,000 cases of Lyme disease in the United States have been reported to the Centers for Disease Control, resulting in a national incidence of 9.7 cases per 100 000 population. The prevalence of Lyme disease varies significantly by geography and has a seasonal incidence . More than 93% of Lyme disease cases in the United States have been reported in high endemic Midatlantic states, Michigan, and Minnesota. Lyme disease occurrence peaks during summer months, reflecting the enhanced transmission by the nymphal tick vectors during May and June. Since Lyme disease became nationally notifiable in 1991, the annual number of reported cases has more than doubled.
Fig 2.
A, Summary of reported cases of Lyme disease in the United States. There is 1 dot within the county of residence for each reported case. Note the widespread diversity of cases correlating with the prevalence of infected Ixodes species in different geographic areas. Courtesy of the Centers for Disease Control. B, The beige-shaded areas indicate the geographic distribution of recorded clinical cases of Lyme borreliosis. The colored ellipses indicate the distribution of the various Borrelia subspecies. is reprinted with permission from Nature Publishing Group.
Fig 3.
Erythema migrans rash with the typical target appearance that is virtually diagnostic of Lyme disease.
Comparison of clinical differences between American and European LNB*
Don’t Miss: Rocky Mountain Spotted Fever Vs Lyme Disease
How Does The Brain Work
The brain controls thoughts, memory, speech, movements of the limbs, and organ function. There are many parts to the brain, and each section has a specific role to play in the human body.
Four lobes make up the brain:
Frontal lobe – the largest of the four lobes, is responsible for the bodys motor skills, such as voluntary movement, language, and intellectual and behavioral functions. This area controls memory, intelligence, concentration, temper and personality.
Temporal lobe – located on each side of the brain at ear level, is important for hearing, memory and speech.
Parietal lobe – at the center of the brain, is where sensory information like heat, pressure and pain is received and interpreted.
Occipital lobe – found at the back of the brain, is primarily responsible for vision.
Lyme Disease And Ms Are Often Confused
The symptoms of Lyme disease and MS can be similar. Doctors may confuse one with the other. To diagnose these conditions, your doctor will need to conduct blood and other tests. If your doctor suspects you have MS, you may need:
Its unlikely that you have both Lyme disease and MS, but its possible. Some of Lyme diseases symptoms can mimic those of MS. It can also follow a relapse-remittance course, where symptoms come and go.
If your history and medical results suggest either condition, your doctor may decide to try antibiotic therapy to see if theres an improvement in your symptoms. Once they fully determine your condition, youll begin a treatment and management plan.
If you have Lyme disease or MS, its important to seek medical advice right away. Despite the different outlooks for Lyme and MS, early diagnosis and treatment for either condition is imperative to your overall health.
Also Check: Hyperbaric Chamber Treatment For Lyme Disease
Acute Vs Chronic Lymedisease
There are some importantdifferences between acute and chronic Lyme disease. When infection occurs andthe bacteria enter the body, the immune system recognizes the microbes asharmful and begins fighting them. If the immune system is strong and robust,the initial symptoms may be very mild, and sometimes there wont be anysymptoms at all. This is why people often dont even realize theyve beeninfected.
In its early stages, Lymedisease is usually treated successfully with antibiotics. But if the infectionremains undiagnosed, the bacteria can go on living inside the cells withoutcausing any trouble for a long time. As they travel to other tissues andorgans, including the brain, they eventually disperse throughout the body. Theonly time symptoms might present is when the immune system weakens due toillness, extreme stress, or some other reason. This is when the bacteria startto flourish, causing a chronic infection.
Chronic Lyme disease occurswhen the entire microbiome is disrupted. After this has happened, the immune system continues todysfunction, which can lead to many different types of symptoms. This chronicphase can even last a lifetime.
Kaitlin: Brain Cancer Survivor
In the summer of 2014, during her last months of pregnancy, Kaitlin Eppinger began experiencing severe headaches and migraines. Her OBGYN prescribed medication and the headaches gradually went away, but returned soon after the birth of her daughter. Again, she attributed them to the pregnancy and hormonal changes. When the headaches persisted, she had blood work done that revealed she had Lyme disease. She received treatment and started to feel better, but was still not 100%. Usually a very active person, especially in the summer months, she noticed a lack of energy along with some new symptoms body tingling and blurred vision that would come and go. She thought these symptoms might be related to the Lyme disease, but in autumn of that year, her doctor suggested an MRI of her brain just to be safe, which was performed at her local hospital.
Kaitlin had started teaching a new school year in her kindergarten classroom, and was feeling overwhelmed and stressed, when normally a new year brought excitement. The day after the MRI, she received a phone call at school with her results she was instructed to call her husband to drive her to the Emergency Department immediately, as a mass the size of an orange had been found in her brain.
You May Like: Is There A Human Vaccine For Lyme Disease