What Are The First Signs And Symptoms Of Lyme Disease
In the first early localized stage of Lyme disease the skin at the site of the tick bite becomes infected with Borrelia burgdorferi bacteria which can cause an expanding round or oval red skin lesion called erythema migrans. This may or may not be associated with flu-like symptoms within days to a month after the tick bite such as achiness, chills, fever, sweats, fatigue, malaise, headache, stiff neck, muscle soreness, joint pain, swollen lymph nodes, and sore throat. The combination of the skin lesion and flu-like symptoms are the primary manifestations of acute stage Lyme disease. Acute Lyme disease is not associated with typical cold-like symptoms of runny nose, prominent cough, or prominent diarrhea.
Lyme Sci: 12 Ways You Can Help Yourself Manage Chronic Pain
Chronic paindefined as ongoing pain that continues for longer than six monthsis a common complaint of patients with persistent Lyme disease.
The CDC estimates that 20% of Americanscurrently live with chronic pain. Estimates range from 10% to 36% of Lyme patients who are diagnosed and treated early are left with chronic symptoms.
For the past 40 years, the medical definition of chronic pain was more narrowly defined, including only those patients with actual or potential tissue damage.
Recently, with the help of researchers at Johns Hopkins Medicine, the International Association for the Study of Pain has made a subtle but important change to the medical definition of pain.
The new definition, An unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damages, is important as it includes the pain caused by an overstimulated nervous system, commonly associated with chronic pain.
This new more inclusive definition, if adopted by insurance providers, could have a positive impact on access to health care for disempowered and neglected populations.
You’ve Gotten A Positive Blood Test
The fourth and final point to determine if your symptoms are due to Lyme disease is to ask your healthcare provider to run a blood test. Although there are several different laboratory tests to diagnose Lyme disease, these tests each have their pros and cons, and can miss establishing the diagnosis because they are not sensitive enough to always pick up the presence of the bacteria.
A bullseye rash is a classic manifestation of Lyme disease, and does not require a positive blood test, but less than 50% of people may get the rash, and it may be located in a part of the body where the rash cannot easily be seen.
If you suffer from chronic unexplained symptoms, including fatigue and musculoskeletal pain, follow this four-step approach and ask your doctor for a professional opinion.
Also Check: Neurologist Specializing In Lyme Disease
How Is Lyme Disease Treated
Generally speaking, the earlier and more quickly Lyme disease is treated, the quicker and more complete your recovery will be.
Antibiotics are used to treat Lyme disease, and they include:
- Oral antibiotics. Oral antibiotics are the standard treatment for Lyme disease when its in its early stages. Cefuroxime or amoxicillin is prescribed for younger children, breastfeeding or pregnant women and some adults. Doxycycline is given to children and adults over the age of eight years.
The usual length of a course of antibiotics for Lyme disease is between 14 and 21 days.
- Intravenous antibiotics. If you are suffering from complications affecting your central nervous system, you may be prescribed treatment via intravenous antibiotics for between 14 and 28 days. This course of action gets rid of any infection, although it may still take you a long time to recover entirely from your symptoms.
Intravenous antibiotic treatment often causes a range of side effects, including:
- Mild to severe diarrhea
- Lower white blood cell count
- Infection or colonization with other antibiotic-resistant organisms
Even though there is a risk of experiencing these side effects, its imperative to undergo the course of treatment your doctor prescribes to avoid the serious complications Lyme disease can have.
Victims And Doctors May Overlook Signs
We often hear that a bulls-eye rash is the classic Lyme marker. But the more common rash if you have one at all is a round or oval-shaped reddish or pinkish area that starts small and expands in size, said Fallon, author with Dr. Jennifer Sotsky of Conquering Lyme Disease.
Black-legged ticks, or deer ticks, are in the nymph stage when they spread Lyme disease. The size of a poppy seed, they can easily be overlooked. Many people dont realize theyve been bitten.
That uncertainty can lead doctors to discount the possibility of Lyme disease in their patients, although symptoms may point in that direction. Fallon said. And even when doctors test for the disease, the results can be inconclusive. For example, in the first four to six weeks after a tick bite, people with Lyme disease will likely test negative because antibodies have not yet had time to develop, according to the CDC.
If you feel your doctor is not taking your concerns seriously, Fallon said, you should seek someone else, and perhaps someone who has more knowledge of tick-borne diseases.
Also Check: Will Lyme Disease Go Away
Achy Stiff Or Swollen Joints
Joint pain and stiffness, often intermittent, are early Lyme symptoms. Your joints may be inflamed, warm to the touch, painful, and swollen. You may have stiffness and limited range of motion in some joints .
Pain may move around. Sometimes your knees may hurt, whereas other times its your neck or your heels. You may also have bursitis . Bursae are the thin cushions between bone and surrounding tissue.
The pain may be severe, and it may be transitory. More than one joint may be affected. Most often the large joints are involved .
People often attribute joint problems to age, genetics, or sports. Lyme should be added to that list, as these statistics indicate:
- One study estimates that 80 percent of people with untreated Lyme have muscle and joint symptoms .
- Fifty percent of people with untreated Lyme have intermittent episodes of arthritis .
- Two-thirds of people have their first episode of joint pain within six months of the infection .
- Use of anti-inflammatory drugs may mask the actual number of people with joint swelling .
Summary:
Joint pain that comes and goes, or moves from joint to joint, could be a sign of Lyme.
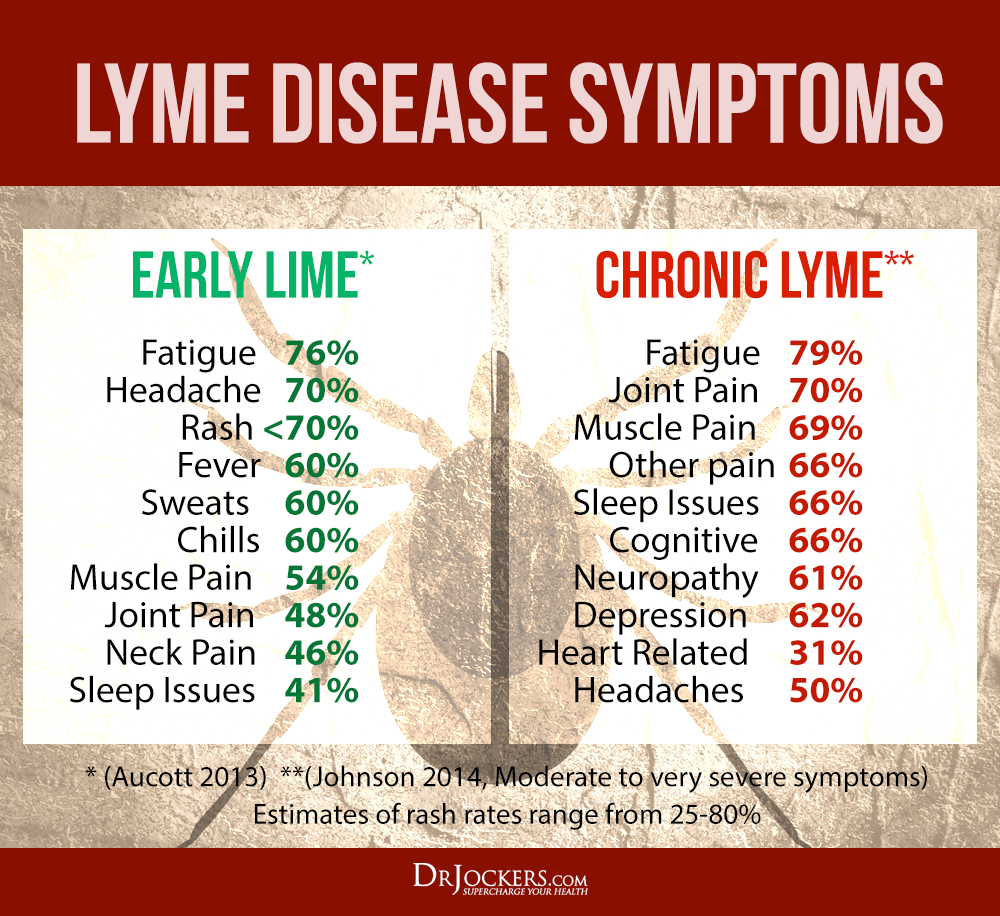
What Are The Symptoms Of Lyme Disease
Symptoms of Lyme disease can be different from person to person.
Early signs and symptoms of Lyme disease usually start 3 to 30 days after you have been bitten by an infected blacklegged tick. Most people experience mild flu-like symptoms soon after being bitten, while a small number may have more serious symptoms, sometimes weeks after the bite.
Early signs and symptoms of Lyme disease may include:
- Rash, sometimes shaped like a bull’s eye )
- Fever
- Muscle and joint aches
- Swollen lymph nodes
If left untreated, more severe symptoms may occur and can last from months to years. Severe symptoms may include:
- Severe headaches
- Facial paralysis
- Intermittent muscle, joint, tendon and bone aches
- Heart disorders , known as Lyme carditis
- Neurological disorders
- Arthritis with severe joint pain and swelling, particularly the knees and less commonly in other joints such as the ankle, elbow and wrists.
In rare cases, Lyme disease can lead to death usually because of complications involving infection of the heart.
Don’t Miss: Pcr Blood Test For Lyme Disease
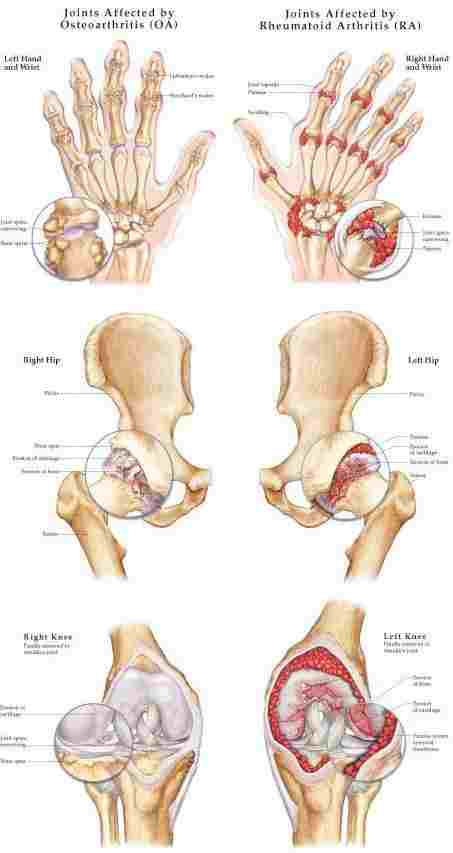
What Are The Symptoms Of Lyme Arthritis
Lyme arthritis usually occurs during a later stage of Lyme disease that has not been treated. For many children, arthritis is the first symptom of Lyme disease they experience, and most do not remember being bitten by a tick.
Symptoms of Lyme arthritis include:
- Joint pain, usually in the knees
- Joint swelling, usually in the knees
- Limping or inability to put weight on a limb
Early symptoms of Lyme disease may include:
- Enlarging, warm rash at the site of the bite that can last days to weeks, often with a partial central clearing so that it looks like a bulls eye
- Fever
If left untreated, later stage symptoms of Lyme disease can include:
- Rash on other parts of the body
- Bells palsy
- Severe headache and neck stiffness
- Pain and swelling in the large joints
- Heart palpitations
How Do You Get Lyme Disease
In the U.S., Lyme disease is carried primarily by deer or blacklegged ticks, and it is caused by the Borrelia mayonii and Borrelia burgdorferi bacteria. Its easy to be bitten by ticks in high-risk areas such as Central PA. The creatures are often no bigger than a poppy seed, so they are very difficult to see before they latch on.
However, not all ticks are Lyme disease carriers. To contract the disease, an infected tick needs to bite you. Bacteria from the tick will eventually make its way from the bite through to your bloodstream, usually taking between 36 to 48 hours. For this reason, whenever youve been in the outdoors, particularly in a known tick-heavy area, you should always check your body for parasites before you come back inside.
In the two primary stages of life, U.S. deer ticks feed on rodents, which are a prime source of the bacteria that causes Lyme disease. Ticks move onto feeding primarily on white-tailed deer when they reach adulthood.
If you find a swollen tick attached to you, it could have fed for long enough to transmit bacteria and should be removed with tick tweezers as soon as possible to prevent infection.
Don’t Miss: Do Ticks In Florida Carry Lyme Disease
Fragments From Lyme Bacteria Persist In Joints Even After The Bacteria Are Killed Off
A new study published in Proceedings of the National Academy of Sciences sheds light on this medical mystery. To keep from spilling open, bacteria have rigid cell walls made of a matrix of protein and sugars, called peptidoglycan. Most bacteria recycle their peptidoglycan when they grow and divide, but the peptidoglycan of B. burgdorferi has a peculiar structure, and the bacteria is unable to reuse it. Instead, it dumps it into its immediate surroundings, like a microbial litterbug.
This peptidoglycan collects in the joints where B. burgdorferi is found. Almost all patients in the PNAS study with Lyme arthritis had peptidoglycan in their joint fluid. Most of them also had specific antibodies to peptidoglycan in the joint fluid, suggesting that the peptidoglycan was driving the inflammatory process. These antibodies were not found in fluid from people with other joint conditions, such as rheumatoid arthritis, osteoarthritis, or gout.
Patients with Lyme arthritis who did not get better with antibiotics still had peptidoglycan in their joint fluid. However, their joint fluid did not contain detectable B. burgdorferi DNA. This suggests that even after the bacteria were killed off, the peptidoglycan stayed behind, and stimulated further inflammation. This may explain why people with Lyme arthritis who do not respond to antibiotics may improve with medications that damp down the immune system, such as methotrexate or TNF inhibitors.
What To Do If You Have A Blacklegged Tick Bite
Remove the tick by pulling it directly out with fine-tipped tweezers. Lift upward with slow and even pressure. Dont twist when removing it. Dont crush it or put soap or other substances on it. Dont apply heat to it.
Place the tick in a resealable container. See if you can identify what kind of a tick it is.
Immediately after removing the tick, wash your skin well with soap and water or with rubbing alcohol.
Not all ticks carry Lyme. The Lyme bacteria is transmitted only by blacklegged ticks in their nymph or adult stage.
Save the tick to show your doctor. The doctor will want to determine if its a blacklegged tick and if theres evidence of feeding. Ticks enlarge as they feed. Your risk of getting Lyme from an infected tick increases with the length of time that the tick fed on your blood.
Summary:
Pull the tick out with tweezers and save it in a resealable container for identification.
Also Check: Can Lyme Disease Cause Rheumatoid Arthritis
How Is Lyme Disease Diagnosed
As the symptoms and signs of Lyme disease are similar to those found in other conditions and are nonspecific, diagnosis is not easy. In addition to this, the ticks that spread the disease can also transmit other diseases at the same time.
Diagnosis is easier when your doctor can see that you have the characteristic bulls eye rash. However, if you dont, your doctor will ask you about your medical history, whether youve been outdoors in summertime, where you have been outdoors and will give you a medical examination.
Lab tests enable bacteria antibodies to be detected in order to confirm a diagnosis. They are most reliable when youve had the infection for a few weeks, as your body will then have had the time to develop the antibodies.
Tests for Lyme disease include:
- Enzyme-linked immunosorbent assay test. This is the test most commonly used to diagnose Lyme disease, and it detects antibodies to Borrelia burgdorferi bacteria. Sometimes the test brings up a false-positive so its not typically used as the sole test for diagnosis.
Although the test may not show as a positive result during the first stage of Lyme disease, often the accompanying rash is distinctive enough to make the diagnosis, especially if youve been in an area where Lyme disease-transmitting ticks are common.
- Western blot test. If the initial ELISA test comes back positive, the Western blot test will confirm your diagnosis.
What Happens At Your Appointment
The GP will ask about your symptoms and consider any rash or recent tick bites you know about.
Lyme disease can be difficult to diagnose. It has similar symptoms to other conditions and there’s not always an obvious rash.
2 types of blood test are available to help confirm or rule out Lyme disease. But these tests are not always accurate in the early stages of the disease.
You may need to be retested if you still have Lyme disease symptoms after a negative result.
Don’t Miss: Unusual Symptoms Of Lyme Disease
Lyme Disease And Joint Pain: Its Complicated
For starters, Lyme is complicated and every patient responds to the disease differently.
Approximately 30,000 new cases of Lyme are diagnosed each year, according to the CDC, and just over one-third of them develop arthritis as a symptom. The most common symptoms beyond the bullseye rash are chills, fatigue, headache/neck stiffness, fever. Painful and swollen jointsespecially in large joints such as the kneeare often considered a late-stage symptom of Lyme, but can appear even days after the tick bite.1-3 Some individuals may find out they have Lyme as a result of chronic joint painwithout ever knowing they had a tick bite.
Ticks rarely carry just one strain of bacteria. They usually deliver several different species of bacteria and parasites in one bite these are called co-infections. Co-infections are one reason Lyme disease diagnosis and treatment can be so complex and difficult.
To investigate why joint pain is a common symptom of Lyme disease, I spoke to Thalia Farshchian, ND, a naturopathic doctor practicing at Medical Options for Wellness, a clinic in Foster City, California. She specializes in treating patients affected by chronic and complex diseases, including Lyme disease.
It is estimated that about 70% of individuals presenting with bullseye rash do not recall a tick bite,” she said. “It is important to note that the absence of a rash does not rule out Lyme Disease as diagnosis, but may be supportive of the diagnosis.”
Lyme Disease: Why Does Joint Pain Persist
Researchers have found clues that might lead to a treatment for Lyme arthritis. The secret may lie in the walls of the bacterium that causes the condition.
Lyme disease occurs when a person becomes infected with a tick-borne bacterium called Borrelia burgdorferi.
Initial symptoms typically include general fatigue, fever, skin rashes, and headaches.
Although doctors can often treat Lyme disease with antibiotics, if they do not catch it early, the bacteria can cause long-term issues with the individuals joints.
In fact, following infection with B. burgdorferi, about 60% of people develop a condition called Lyme arthritis, the hallmarks of which are inflamed and painful joints.
Lyme arthritis can persist for months or even years in some cases.
Researchers are still unsure why joint symptoms can continue long after antibiotics have destroyed the bacteria.
30,000 cases of Lyme disease among the United States population.
However, the true number of cases is likely to be much higher. In fact, the CDC estimate that there might be up to 300,000 cases each year.
According to the CDC, reports of Lyme disease have tripled since the late 1990s, and overall, tick-borne diseases are becoming more prevalent. This increase is due, at least in part, to rising global temperatures.
Due to the steady growth in the number of cases, scientists are keen to uncover more effective ways of treating the long-term symptoms.
Read Also: Antibiotics For Lyme Disease In Humans
When Should I Go See My Doctor
Anyone who has been bitten by a black-legged deer tick is at risk for Lyme disease. The highest risk groups include those living in or visiting endemic areas, especially people who spend significant time outdoors such as gardeners, hikers, or outdoor workers.
Patients should seek advice from their doctor if they have a suspicious round expanding red skin lesion, and/or show signs of summer-flu, particularly during Lyme disease season, which is highest-risk late spring through July/August. If those circumstances apply or symptoms persist it is very important to go to a physician.
For the west coast and other more temperate regions Lyme disease can be a year-round concern.
In the later disseminated stages, Lyme disease can be a much more insidious and complex illness. An individual should seek medical care if experiencing symptoms such as prolonged fevers, unexplained fatigue, painful joints, new or unusual headache, or heart or neurologic symptoms. If unexplained viral-like symptoms last for more than 1-2 weeks, please seek the advice of a physician.