How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Overview Of Lyme Disease Pain Control
Most people with Lyme have pain. In this article I review the causes of Lyme pain and the steps a person can take to control and eliminate pain. I provide a strategy for controlling Lyme disease pain which uses:
- Sleep,
- Anti-cytokine herbs and supplements to lower inflammation,
- Supplements that support repair of mitochondria cell energy factories,
- Low dose naltrexone ,
- Medical marijuana and/or CBD oil,
- Magnesium to relax muscles,
Mitochondria Dysfunction And Chronic Pain
Mitochondria are the energy factories found in every cell. By some estimates there are 300 to 400 mitochondria in a cell. Chronic infection can damage the mitochondria. There is a growing body of science showing damaged mitochondria leads to chronic pain.
Lyme Disease Pain Strategy
It is possible to repair mitochondria. See How to Fix Mitochondria & Get Energy in Lyme Disease for steps to repair the injured mitochondria.
One other strategy is to eat low inflammatory foods which support mitochondria. See The Best Brain, Inflammation, Pain, Energy, and Detox Diet Ever for more information about an effective paleo diet.
Don’t Miss: Lyme Carditis Symptoms In Humans
Defining Patient Subgroups: Post
Patients with persistent symptoms related to Lyme disease likely represent a heterogeneous population, which includes previously untreated patients, as well as those treated patients who remain symptomatic. As a result, some will manifest primarily patient-reported symptoms while others will present with symptoms in conjunction with objective, physical findings. This heterogeneity is further complicated by variation in terminology and the definitions used by different groups in the field.
Figure 3. A schematic of clinical- and research-defined patient subgroups among those with persistent symptoms associated with Lyme disease . The size of each patient subgroup is not meant to represent actual population frequency, as prevalence data is extremely limited. IDSA, Infectious Diseases Society of America ILADS, International Lyme and Associated Diseases Society CLD-PT, Chronic Lyme Disease-Previously Treated CLD-U, Chronic Lyme Disease-Untreated IgG, Immunoglobulin G CFS, Chronic Fatigue Syndrome FM, Fibromyalgia.
What Are The Symptoms Of Post
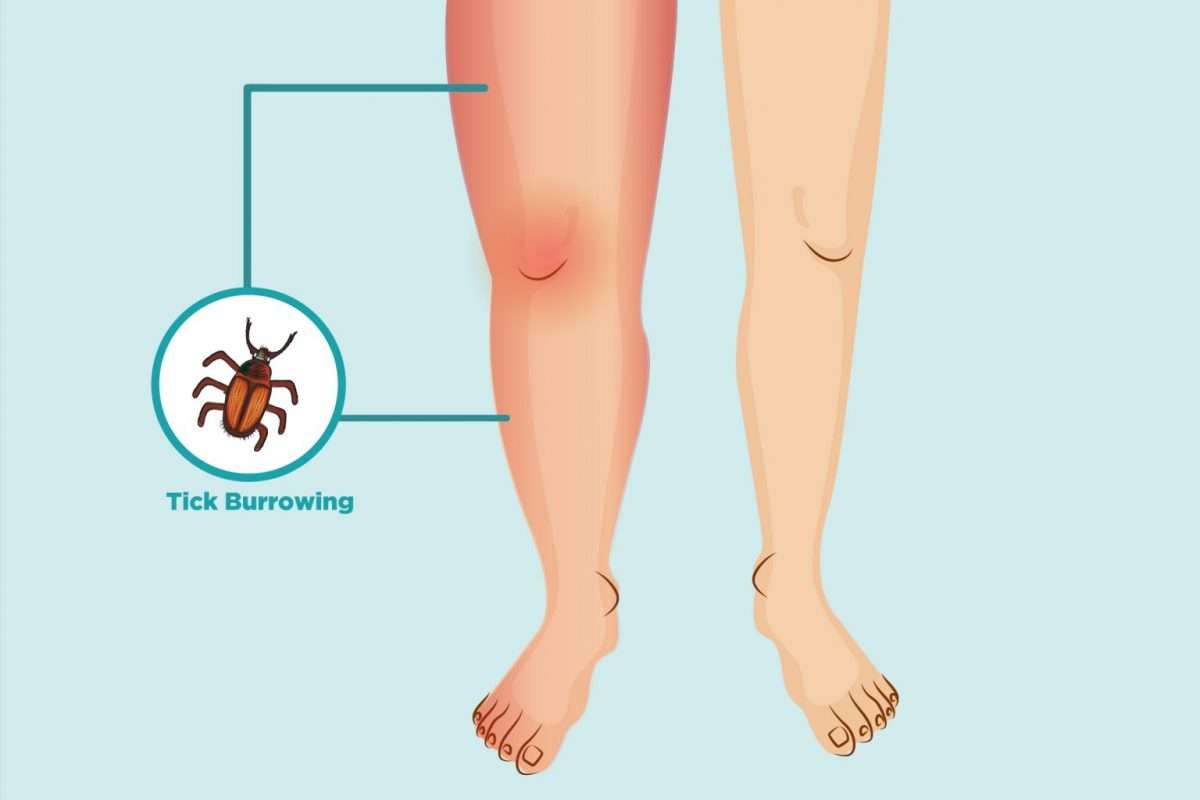
Doctors have known for years that they cannot rely on a physical exam to diagnose early Lyme disease unless they find an erythema migrans rash, Bells palsy, or heart block. Now, Rebman and colleagues from the Johns Hopkins University School of Medicine acknowledge that doctors also cannot count on a physical exam to diagnose Post-treatment Lyme disease syndrome .
In their article published in the journal Frontiers in Medicine, the authors state, Results from the physical exam and laboratory testing our sample of patients with PTLDS did not show a pattern of significant objective abnormalities. However, the most notable exception was the higher rate of diminished vibratory sensation on physical exam among participants with PTLDS.
Following treatment for Lyme disease, it is uncommon to find objective clinical manifestations in patients with PTLDS, according to the researchers. In fact, a much more likely scenario after treatment is the persistence or development of subjective symptoms without any residual or new objective manifestation.
But the authors did discover a collection of symptoms among the Lyme disease patients which, when looked at as a whole, indicated the presence of problems post-treatment. For example, Although only found in a small subset of our sample , two participants met criteria for postural orthostatic tachycardia syndrome, an autonomic condition that has been previously reported following Lyme disease.
References:
You May Like: Breeds Predisposed To Lyme Nephritis
What Is Post Treatment Lyme Disease
Post Treatment Lyme Disease represents a research subset of patients who remain significantly ill 6 months or more following standard antibiotic therapy for Lyme disease. PTLD is characterized by a constellation of symptoms that includes severe fatigue, musculoskeletal pain, sleep disturbance, depression, and cognitive problems such as difficulty with short-term memory, speed of thinking, or multi-tasking. In the absence of a direct diagnostic biomarker blood test, PTLD has been difficult to define by physicians, and its existence has been controversial. However, our clinical research shows that meticulous patient evaluation when used alongside appropriate diagnostic testing can reliably identify patients with a history of previously treated Lyme disease who display the typical symptom patterns of PTLD.
How Is Lyme Disease Diagnosed
As the symptoms and signs of Lyme disease are similar to those found in other conditions and are nonspecific, diagnosis is not easy. In addition to this, the ticks that spread the disease can also transmit other diseases at the same time.
Diagnosis is easier when your doctor can see that you have the characteristic bulls eye rash. However, if you dont, your doctor will ask you about your medical history, whether youve been outdoors in summertime, where you have been outdoors and will give you a medical examination.
Lab tests enable bacteria antibodies to be detected in order to confirm a diagnosis. They are most reliable when youve had the infection for a few weeks, as your body will then have had the time to develop the antibodies.
Tests for Lyme disease include:
- Enzyme-linked immunosorbent assay test. This is the test most commonly used to diagnose Lyme disease, and it detects antibodies to Borrelia burgdorferi bacteria. Sometimes the test brings up a false-positive so its not typically used as the sole test for diagnosis.
Although the test may not show as a positive result during the first stage of Lyme disease, often the accompanying rash is distinctive enough to make the diagnosis, especially if youve been in an area where Lyme disease-transmitting ticks are common.
- Western blot test. If the initial ELISA test comes back positive, the Western blot test will confirm your diagnosis.
Don’t Miss: Is There A Vaccine For Lyme Disease
Symptoms Of Lyme Disease
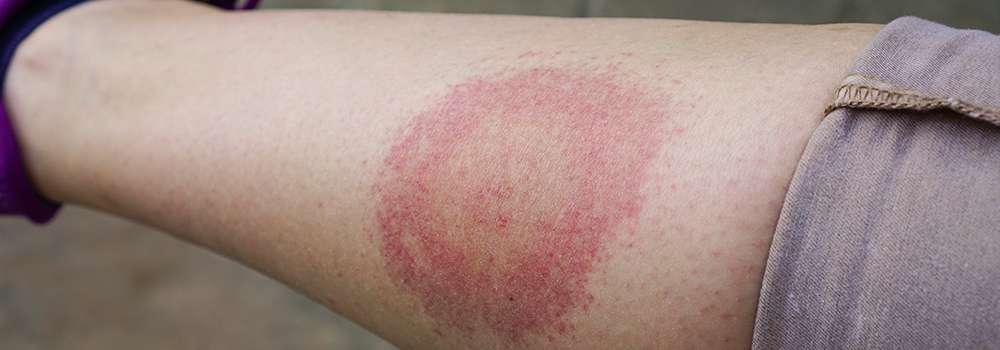
A circular or oval shape rash around a tick bite can be an early symptom of Lyme disease in some people.
The rash can appear up to 3 months after being bitten by an infected tick, but usually appears within 1 to 4 weeks. It can last for several weeks.
The rash can have a darker or lighter area in the centre and might gradually spread. It’s not usually hot or itchy.
The rash may be flat, or slightly raised, and look pink, red, or purple when it appears on white skin. It can be harder to see the rash on brown and black skin and it may look like a bruise.
Some people also get flu-like symptoms a few days or weeks after they were bitten by an infected tick, such as:
- a high temperature, or feeling hot and shivery
- headache
- tiredness and loss of energy
Some people with Lyme disease develop more severe symptoms months or years later.
This is more likely if treatment is delayed.
These more severe symptoms may include:
- pain and swelling in joints
- nerve problems such as pain or numbness
- heart problems
- trouble with memory or concentration
How Is Lyme Arthritis Treated
Most children with Lyme arthritis recover after 28 days of antibiotic treatment. The most common antibiotics prescribed for Lyme disease are:
- Doxycycline for children eight years of age or older
- Amoxicillin for children under eight years of age
If the symptoms persist after a course of antibiotics, a second course of antibiotics may be prescribed.
In persistent cases of Lyme arthritis, your rheumatologist may prescribe non-steroidal anti-inflammatory drugs , disease-modifying antirheumatic drugs , or intra-articular corticosteroids.
Don’t Miss: Cure Lyme Disease Without Antibiotics
When To See A Healthcare Provider
Since Lyme disease can take different forms, and since its often confused with other conditions, its important to be proactive if you suspect the condition. What signs prompt medical help? Call the healthcare provider if:
- You have a bullseye rashor any kind of rashfollowing a tick bite.
- You experience flu-like symptoms after a tick bite.
- You experience symptoms of more advanced Lyme disease: arthritis, heart palpitations, facial paralysis, dizziness, and others.
How Does Lyme Disease Affect The Joints
Lyme disease is an infection caused by Borrelia burgdorferi bacteria transmitted from the bite of an infected blacklegged tick . A bulls-eye shaped rash is an easily recognizable sign of this tick borne disease however, if the rash doesnt appear or goes unnoticed, Lyme disease is often confused with other conditions due to the common nature of its flu-like symptoms.
Lyme disease can typically be treated with a course of antibiotics however, if left untreated, the infection can develop into a chronic disorder affecting the heart, joints, and nervous system. Once the disease reaches this stage, the infection may be managed, but the damage it has caused can be irreversible. .
Also Check: Biomagnetic Therapy For Lyme Disease
Chronic Lyme Arthritis: A Mystery Solved
- By John Ross, MD, FIDSA, Contributor
In 1975, researchers from Yale investigated an epidemic of 51 patients with arthritis who lived near the woodsy town of Lyme, Connecticut. The most common symptom was recurrent attacks of knee swelling. A few had pain in other joints, such as the wrist or ankle. Many had fever, fatigue, and headache. Some remembered a round skin rash before the onset of knee swelling.
We now know that Lyme disease is an infection acquired from tick bites, caused by a spiral bacterium named Borrelia burgdorferi. After a tick bite, Borrelia bacteria wriggle through the skin away from the bite site. This leads to a circular red rash, known as erythema migrans. In its more advanced stages, erythema migrans may take on a bullseye appearance. Many people are unaware of the rash, as it is usually painless, and ticks may bite in less visible locations, such as a buttock or shoulder blade.
Lyme disease is diagnosed with blood tests that detect antibodies to B. burgdorferi. Two-step testing is traditionally performed. A rapid enzyme immunoassay is performed first. If this is positive, a more time-consuming Western blot test is sent for confirmation. The FDA recently approved two rapid tests for Lyme disease that are performed simultaneously, reducing the turnaround time.
Can Lyme Disease Come Back After Being Treated
Lyme disease is one of the most common vector-borne diseases occurring in approximately 300,000 people in United States of America. The disease is caused by the bacteria, but transmitted by the ticks. Mice and deer acts as reservoir of the bacteria. When ticks feed on these reservoirs, the bacterium gets transmitted in ticks and from ticks they infect humans. The symptoms may be fatigue, joint pain, inflammation and rashes. The bacteria can be completely removed from the body by taking the recommended therapy of antibiotics. Certain preventive measures should also be taken to stay away from the disease causing ticks. The prevalence of disease is growing to other parts of the world due to migration of people. In India, the disease is rare but recently cases have of Lyme infections have been reported in India.
Read Also: Post Treatment Lyme Disease Syndrome Mayo Clinic
Sign Up For Our Newsletter
Disclaimer: The above material is provided for information purposes only. The material is not nor should be considered, or used as a substitute for, medical advice, diagnosis, or treatment, nor does it necessarily represent endorsement by or an official position of Global Lyme Alliance, Inc. or any of its directors, officers, advisors or volunteers. Advice on the testing, treatment or care of an individual patient should be obtained through consultation with a physician who has examined that patient or is familiar with that patients medical history. Global Lyme Alliance, Inc. makes no warranties of any kind regarding this Website, including as to the accuracy, completeness, currency or reliability of any information contained herein, and all such warranties are expressly disclaimed.
Early Symptoms And Signs Of Lyme Disease
You can expect a small, red bump on the site of your bite, or where you removed the tick from, and this will resolve within a day or two. This is to be expected after being bitten by any insect, and it in itself is not an indicator that you have Lyme disease.
However, if you have been infected, you can expect the following within a month or so:
- Flu-like symptoms. Early-stage Lyme disease can present as chills, fever, fatigue body aches, stiff neck, headache and other flu-like symptoms.
- Rash development. Between three and 30 days after an infected tick bites you, you may see a rash that looks like a bulls eye. This will expand over days, and it can grow to as many as 11 to 12 inches across. It is usually not painful or itchy.
Also Check: How Long Does It Take For Lyme Test Results
Strategies For Managing Nerve Pain
1. Reduce Your Microbial Burden
When youre dealing with Lyme disease and co-infections, its not always easy to pinpoint which stealth pathogen is affecting your nervous system. In fact, its most reasonable to recognize that all sneaky microbes are capable of disrupting immune function and causing it to go awry.
When your bodys microbial burden becomes too great, your microbiome becomes imbalanced, driving inflammation and aggravating neuropathy. Thus, at the top of the priority list is decreasing the infectious load to normalize and calm the immune system.
When youre looking for natural solutions to lessen the impact of stealth pathogens, herbal therapy can play a critical role. Not only do herbs have antimicrobial properties, but they are anti-inflammatory and contain antioxidants as well.
Moreover, herbs dont disrupt the delicate balance of the microbiome like synthetics medications do. Some of my favorite herbs with antimicrobial and immunomodulating properties to keep in mind include:
2. Use Medications Cautiously
When it comes to neuropathy, the reality is that sometimes you need some extra support to get your pain levels to a tolerable level. There are a variety of over-the-counter and prescription medications that may be useful from time to time.
However, the value of medications is limited to short term management of symptoms because of cumulative side effects. The list of medications commonly recommended by healthcare providers includes:
Lyme Disease Vs Rheumatoid Arthritis
Lyme disease can sometimes be confused for other conditions, and its not uncommon for patients presenting with Lyme disease-related joint pain to be misdiagnosed with . Both Lyme and RA cause joint pain and can be debilitating when left untreated, but there are differences.
-
Lyme arthritis tends to manifest in larger joints , on one side of the body. Lyme joint pain tends to come and go.
-
Rheumatoid arthritis occurs more often in the hands, feet, fingers, and toes, and shows up on both sides of the body. RA joint pain and stiffness occurs every day, and is usually chronic.
-
Lyme disease usually goes away when treated, and most patients make a full recovery.
-
can manage symptoms and show the progression of the disease, but there is no cure.
Lyme pain can often migrate throughout the body, and patients may have pain in their knee one week, and in their wrists the following week, says Chicago-based integrative medicine specialist Casey Kelley, MD. With rheumatoid arthritis, the pain often stays where it begins and does not migrate.
Getting Lyme puts you at greater risk for later developing RA and other types of inflammatory arthritis. One study found that nearly one-third of participants who had Lyme-arthritis later developed an inflammatory arthritis.
Don’t Miss: How To Find A Lyme Literate Doctor
When Lyme Disease Isnt Caught And Treated Early It Can Cause Late
If youre from a certain area, you know at least a little about Lyme disease. Its the reason your parents made you cover up any time youd be remotely close to a wooded area and checked you religiously for ticks upon your return home.
Lyme disease is an infectious disease spread by certain ticks in certain parts of the United States and Europe. Early on, it can cause flu-like symptoms and a telltale bulls-eye rash. But if Lyme disease isnt caught and treated with antibiotics promptly, the infection can eventually spread through the body. The most common late-stage symptoms include joint swelling and pain, a condition known as Lyme arthritis.
Historically, about 60 percent of people with undiagnosed, untreated Lyme disease would develop Lyme arthritis, according to a study in the journal Arthritis & Rheumatology.
Lyme arthritis, however, shouldnt be confused with chronic Lyme. As its name implies, chronic Lyme is a condition that doesnt go away with one course of antibiotics. Its controversial in the medical world, partly because some patients are diagnosed with chronic Lyme when lab tests dont show evidence of an infection. Some doctors insist that chronic Lyme patients symptoms fade when they stay on antibiotics others argue that its a different disease entirely and that long-term antibiotics will only create more side effects.
Late-stage Lyme, on the other hand, is curable Lyme disease thats progressed and lead to complications such as arthritis.
Treating What You Dont Know
The other big question is how to treat something with a cause that cant be identified.
Antibiotics are sometimes prescribed on the theory that B. burgdorferi might still be hiding out in the body somewhere. However, although there have been anecdotal short-term successes, Marques said no studies have shown sustained benefits from antibiotics to people with chronic Lyme disease or those with post-Lyme disease syndrome.
The majority of people who contract Lyme and are treated for it with a course of antibiotics do get better with time.
But those who dont 10 to 20 percent, according to Marques review of the research fall into the post-Lyme disease syndrome category.
Those people continue to experience persistent or intermittent symptoms a year after completing the antibiotics therapy.
Children appear less likely to develop long-term symptoms as are those who dont delay antibiotics or have less severe cases of Lyme in the first place.
In cases of chronic Lyme, people who test negative for the disease despite symptoms could be infected with another tick-borne illness or have an autoimmune disorder or other problem.
How to treat these long-term symptoms is still a mystery.
For now, Marques and her team are working on identifying biomarkers and other ways to find out definitively whether Lyme disease is to blame for the symptoms.
That additional research is becoming more critical.
Researchers have predicted higher tick numbers in some parts of the country this summer.
Read Also: Lyme Disease Specialist Long Island New York