Who Gets Lyme Disease
Anyone bitten by an infected deer tick can get Lyme disease. Most U.S. cases of Lyme disease happen in Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. But Lyme disease is found in other parts of the U.S., Europe, Asia, and Australia too.
The Best Test For Lyme Disease
Lyme disease is a tick-borne illness spread by Lyme borreliaebacteria which includes, but is not limited to, Borrelia burgdorferi sensu stricto. The Centers for Disease Control and Prevention estimate that there are 400,000 cases of Lyme disease annually, making Lyme a serious public health concern that only stands to grow as the spread of ticks affects disease endemicity and seasonality.
One of the biggest challenges of fighting Lyme disease is providing patients with accurate diagnostic tests. Without access to the best tests for Lyme disease, its impossible to diagnose this treatable disease in a timely manner. When the disease isnt caught in time, it can spread throughout the body and cause chronic health problems that could otherwise be avoided with earlier detection and treatment.
Which B Burgdorferi Antigens Are Used And How Is The Test Interpreted
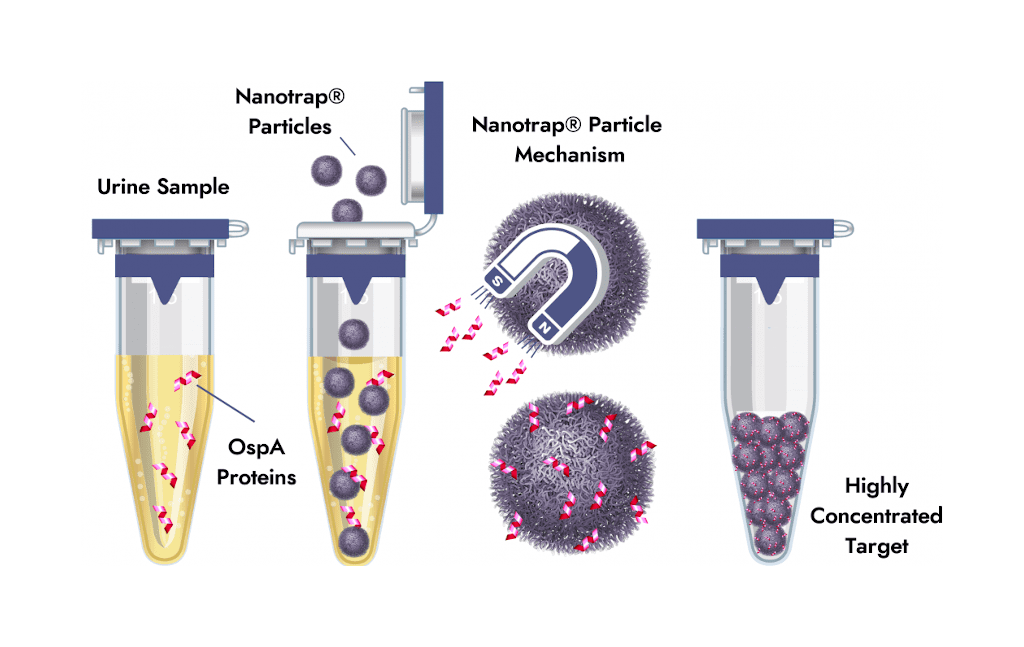
The Equine Lyme Multiplex assay is based on three antigens, called outer surface proteins , of B. burgdorferi. Various research studies have shown that Osp antigen expression changes on the bacterial surface in response to tick feeding and again after infection of a warm-blooded host, such as dogs, horses, or humans . In response to infection, horses develop antibodies to these Osp proteins and testing for antibodies to specific Osp antigens can assist in the diagnosis of infection and Lyme disease.
You May Like: Blot Test For Lyme Disease
Late Lyme Disease Symptoms
Question 10 What Other Infections Can A Tick Transmit To Humans Besides Lyme Disease
I scapularis ticks can also carry other human pathogens that have a high degree of symptom overlap, including Borrelia miyamotoi, Anaplasma phagocytophilum, Ehrlichia chaffeensis, and Babesia microti.2,10-12 Several studies on co-infected ticks indicate as many as 20% of Ixodid ticks can be coinfected with B burgdorferi and one or more of these other tick-borne human pathogens.10-12
Molecular tests can be useful to detect these organisms in early/acute stages of infection, when genetic material from the pathogen can be detected but antibodies remain below the limit of detection of serologic assays.2,10-12 Quest offers molecular and/or serological tests for B burgdorferi, B miyamotoi, A phagocytophilum, E chaffeensis, and B microti, individually and in 2 panels .
Read Also: Can Lyme Disease Cause Chest Pain
Investigation Of Suspected Neurological Lyme Disease
The diagnosis of neurological Lyme disease can only be confirmed by examination of the CSF and a paired serum. A definite diagnosis is based on the presence of a pleocytosis in the CSF, demonstration of intrathecal synthesis of specific antibodies to Borrelia species in CSF by comparison to serum and the presence of neurological symptoms. It is not possible to confirm intrathecal synthesis and hence definite neurological Lyme disease without a paired serum .
In 2018 RIPL is introducing a service for the detection of intrathecal synthesis of Borrelia-specific antibodies which is summarised in this flow diagram.
Clinicians may ask for guidance on laboratory testing of CSF from RIPL if required.
How Does The Equine Lyme Multiplex Assay Work
The Equine Lyme Multiplex Assay was developed at the Animal Health Diagnostic Center at Cornell University. It detects antibodies to three antigens of B. burgdorferi in equine serum . The test is based on fluorescent beads and allows the simultaneous measurement of antibodies to all three B. burgdorferi antigens in a single sample13.
Figure 2:B. burgdorferi
Also Check: Houses In East Lyme Ct
How Can I Tell If Treatment Is Working
If joint lameness is the presenting sign, improvement may be noted after 3-5 days starting antibiotics. A dog’s response to therapy can be assessed by repeating the QC6 test six months after treatment is complete. Dogs that start with a moderate to high QC6 value typically show a 50% reduction or more in the QC6 at six months, indicating that treatment has been successful. Dogs that have a lower initial QC6 value may not show such dramatic reductions in the QC6 at six months, although the value should still be lower than the starting point if treatment has been successful.
A persistently high QC6 suggests treatment may not have been complete or that the dog became reinfected after treatment was stopped.
Is Treatment 100% Effective
Scientists are divided on this topic. Some studies suggest that that even long-term antibiotics may not completely clear infection dogs may get sick again at some point after antibiotic treatment is stopped. Other studies suggest that complete clearance of infection is possible with antibiotic treatment. Further research is required to answer this question.
Also Check: Royall Lyme All Purpose Lotion
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Mis Nooit Meer Een Publicatie
Met een jaarabonnement mis je niets meer! Wil je altijd op de hoogte blijven van de nieuwste ontwikkelingen op het gebied van de biowetenschappen? Neem dan een abonnement! Hiermee ontvang je een korting van 40% ten opzichte van de prijs in de webwinkel. Daarnaast betaal je geen verzendkosten bij een abonnement. Het abonnement gaat in per 1 januari van het nieuwe kalenderjaar. Je kunt te allen tijde opzeggen, waarna je alleen nog de cahiers ontvangt die je hebt betaald.
Also Check: What Are The Symptoms Of Lyme Disease In Cats
Lab Tests Alone Not Conclusive For Diagnosis Of Lyme Disease
Lyme disease can cause a variety of complaints in patients. Laboratory tests for the disease can support medical practitioners in making a diagnosis but are not necessarily conclusive. This was the conclusion of study conducted by a group of more than 20 European experts on the reliability of serological tests in the diagnosis of Lyme disease.
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Also Check: Main Symptoms Of Lyme Disease
How Is It Diagnosed
If youâve been outside in an area where ticks are known to live, you should tell your doctor. Theyâll also want to know about the symptoms youâre having. These details are crucial to making a diagnosis of Lyme disease.
Early symptoms that usually occur within the first month after a tick bite can include:
- Rash at the site of the tick bite that may look like a âbullâs-eyeâ
- Racing heart
- Problems with your short-term memory
Symptoms that come and go are common with Lyme disease. They will also depend on the stage of the disease.
Question 7 What Are Some Prominent Limitations Of Serologic Testing For Lyme Disease
As noted above, serologic tests may yield negative results early during infection, before antibodies have reached detectable levels. In addition, serologic assays may give false-positive results in individuals with other conditions, including 3,5,6
- Pathogenic spirochetal diseases, such as syphilis, yaws, pinta leptospirosis, relapsing fever, and periodontal disease
- Other bacterial and viral infections, such as Rocky Mountain spotted fever, Epstein-Barr virus, and cytomegalovirus
- Connective tissue autoimmune diseases associated with positivity for anti-nuclear antibody, including rheumatoid arthritis and systemic lupus erythematosus
Read Also: How Do You Know If A Tick Has Lyme Disease
Special Considerations For Vaccinated Horses
An approved Lyme vaccine for horses is currently not available. Horses are sometimes vaccinated with one of the three available Lyme vaccines for dogs for attempted protection of horses that are housed in Lyme endemic areas. Efficacy studies of canine vaccines in horses are not yet available, but experimental data suggested that anti-OspA antibodies are protective in horses.
All available vaccines contain OspA antigen as the sole or one of the vaccine components. Antibodies to OspA are identified by the Equine Lyme Multiplex Assay to determine the vaccination status in vaccinated horses. To provide our clients with the best interpretation for each animal, we need information on the vaccine used. This includes the name of the vaccine and the date when the horse was last vaccinated. Please include this information on the submission form when samples of vaccinated horses are submitted for testing.
Recent studies indicate that horses can respond to the canine vaccines, but the responses are typically short-lived17,18. It is therefore recommended to vaccinate horses in close proximity to tick season, approximately four weeks before ticks are typically abundant in the area. Additionally, confirmatory testing is recommended after vaccination of horses since low OspA antibody responses have been observed in individual horses.
How Lyme Disease Testing Works
Lyme disease testing typically involves testing for three strains of bacteria: Borrelia garinii, Borrelia afzelii, and Borrelia burgdorferi. Having antibodies for these bacteria suggests that infection has occurred.
If results are positive for Lyme disease, your healthcare provider will likely advise next steps, including receiving a Western Blot Test, which detects antibodies created in response to specific proteins of B. burgdorferi . Both testing steps can be performed using the same blood sample .
If both tests show positive results, you likely have Lyme disease, and your healthcare provider can help you determine appropriate treatment options. For those still experiencing active Lyme disease despite trying medications for treatment, a PCR test is used to determine the genetic material of the Lyme disease bacteria. This can help identify a current, active infection.
Read Also: What Are The After Effects Of Lyme Disease
How To Remove A Tick
Types Of Lyme Disease Tests
Antibody titer tests for Lyme disease measure antibodies that are specific to the bacteria that can trigger the condition. Antibodies are part of the bodys immune response. Tests look for two types of antibodies, known as immunoglobulin M and immunoglobulin G .
IgM antibodies usually peak within a few weeks after an infection with Borrelia bacteria and start to collapse 4-6 months after infection. IgG antibodies are slower to develop, beginning to show 4-6 weeks after exposure and may peak 4-6 months after exposure. While IgM tends to be associated with an active infection, both IgM and IgG can persist in the blood for many years.
The Centers for Disease Control and Prevention recommends a two-stage or two-tiered test for these antibodies. If the initial blood test is positive for IgM or IgG antibodies associated with the Borrelia bacteria, a second test is done, often using different laboratory methods.
Testing for IgM and IgG can support the finding that you have been exposed to Borrelia, but this on its own does not prove whether or not you have Lyme disease.
Follow-up testing may be necessary if testing is inconclusive. This could involve repeat blood tests or the use of different types of medical tests to rule out other health conditions. In people suspected of bacterial reinfection, imaging tests may be used to detect joint inflammation.
Don’t Miss: New Paradigms In Lyme Disease Treatment
How Is Lyme Disease Treated
Common antibiotics are effective at clearing the infection and early symptoms and in helping to prevent the development of complications. If untreated, the disease will progress to a longer-term form in about half of patients. Antibiotics are generally given for up to three weeks. If complications develop, intravenous antibiotics may need to be used to treat the infection. The bacteria can survive for long periods in the body even if no symptoms develop. If untreated, the bacteria can cause chronic irritation in in a number of the bodys organs. That is why early diagnosis and treatment with antibiotics is important.
Question 8 Is There A Test To Prove Cure For Lyme Disease

There is no test to prove cure for Lyme disease. Antibodies frequently persist in the blood for months or even years after the infection is resolved, despite absence of detectable/viable B burgdorferi.7 Therefore, antibody tests cannot be used to determine a cure. There is no evidence that antibiotics cause Lyme serology blood tests to become negative following treatment.3,5,6
Also Check: Sleep Inn East Lyme Ct
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Read Also: When To Test For Lyme Disease
Completion Of Lyme Disease Test Request Form
Diagnostic samples must be submitted with a completed RIPLLyme disease test request form . Please use a single request form for each patient even when sending several samples.
Please provide details of the sample type, patients symptoms and onset date, tick bite or exposure history and, if relevant, travel and treatment history. Symptom onset date is particularly important for interpretation of laboratory results.
When sending CSF, please provide the cell count and total albumin, IgG and IgM levels for the CSF and serum pair, if available.
Ideally the clinician who sees the patient should print out and complete the appropriate request form . Send the request to the local laboratory with the clinical sample along with a local laboratory request form, whether this is paper or electronic.
The local laboratory should complete the senders information on the request form and then forward the completed form and sample to RIPL. Before sending samples, clinicians are advised to liaise with their local laboratory because local arrangements may vary.
If only immunoblot confirmation is required because the local laboratory has already obtained a positive Lyme screening test result on the serum sample being submitted, tick the Line blot confirmation only box and write the positive screening test result below.
You May Like: Lyme Bell’s Palsy Treatment
What Happens At Your Appointment
The GP will ask about your symptoms and consider any rash or recent tick bites you know about.
Lyme disease can be difficult to diagnose. It has similar symptoms to other conditions and there’s not always an obvious rash.
2 types of blood test are available to help confirm or rule out Lyme disease. But these tests are not always accurate in the early stages of the disease.
You may need to be retested if you still have Lyme disease symptoms after a negative result.
The Blood Tests Can Have False Positives
The blood tests can trigger false positives, suggesting that you have the disease when you really dont. This can happen in up to one out of four tests.
This can lead to unnecessary treatment with antibiotics. These drugs are usually safe, but they sometimes cause side effects, such as nausea, vomiting, diarrhea, and increased sensitivity of the skin to sunlight. In rare cases, they can even cause dangerous allergic reactions.
Using too many antibiotics can also lead to the growth of drug-resistant bacteria. This means that bacteria in your body may get stronger and more difficult to treat with antibiotics in the future.
A false positive can also lead to more unneeded blood tests, urine tests, X-rays, and doctor visits.
If you have a false positive, you may not get treated for the real cause of your pain. For example, rheumatoid arthritis is a disease that causes joint pain. It can lead to permanent and severe joint damage if you do not start taking the right medicines as early as possible.
Don’t Miss: Do You Get A Fever With Lyme Disease