The Role Of Lyme Disease Tests
The purpose of the most common type of Lyme disease testing is to determine whether you have developed antibodies as a result of past exposure to the Borrelia bacteria that cause Lyme disease. Antibodies are proteins created by the immune system that target specific threats like bacteria and viruses.
Blood testing alone cannot determine whether you have Lyme disease. Instead, testing can provide helpful information that your doctor can consider along with other factors, such as any symptoms youve had and whether youve been exposed to ticks that can carry Borrelia, to determine if a diagnosis of Lyme disease is appropriate.
Beyond blood testing, it is possible to analyze fluid from the central nervous system for signs of the Borrelia bacteria.
Lyme Disease Diagnosis And Testing Highlights
- LLMDS consider the specificity of the particular bands that test positive for a patient.
- Although the CDC requires 5 of 10 bands for IgG surveillance purposes, 2 of 5 bands have specificity of 93-96% and a sensitivity of 100%. .
- 56% of patients with Lyme disease test negative using the two-tiered testing system recommended by the CDC.
- The CDC case surveillance definition allows single-tier IgG immunoblot seropositivity using established criteria.
- The CDC states: This surveillance case definition was developed for national reporting of Lyme disease it is not intended to be used in clinical diagnosis.
- The College of American Pathologists found that ELISA tests do not have adequate sensitivity to be used for screening purposes.
- 52% of patients with chronic disease are negative by ELISA but positive by Western blot.
Lyme Disease Test Western Blot
Labs performing a Western blot use electricity to separate proteins called antigens into bands. The read-out from the Western blot looks like a bar code. The lab compares the pattern produced by running the test with your blood to a template pattern representing known cases of Lyme disease. If your blot has bands in the right places, and the right number of bands, it is positive.
The CDC requires 5 out of 10 bands for a positive test result. However, because some bands on the Western blot are more significant than others your doctor may decide you have Lyme disease even if your Western blot does not have the number of bands or specific bands recommended by the CDC. Different laboratories use different methods and criteria for interpreting the test, so you can have a positive test result from one lab and a negative test result from another.
For a comprehensive explanation of the western blot test, download Understanding Western Blot Lyme disease test.
The chart below will help you understand how to interpret the western blot test.
Don’t Miss: How To Treat Post Lyme Disease Syndrome
Reason : The Type Of Test Used
PCR Test: Antibody Test :
| Borrelia Culture Test:This test looks for the actual presence of the Lyme bacteria in a persons blood. It completely skips the middle man, antibodies, of antibody testing, and is considered the closest test to 100% accuracy in detecting an active Lyme infection in a person. The problem with this test is that it relies on a living Lyme bacterium to be cultured , and the nature of the Lyme bacteria is that it does not survive long outside of its host, even in cyst-form. This is why Advanced Laboratory Services, the lab that performs the Borrelia Culture Test, needs your blood sample within 24 hours of being withdrawn. |
Recommended Reading: Test Tick For Lyme Disease Massachusetts
How Accurate Are Blood Tests For Lyme Disease

With about 30,000 people infected each year, Lyme disease causes a range of serious symptoms, including joint pain, chronic fatigue, facial paralysis, and in rare cases, even death. Because of these risks, anyone who is bitten by a deer tick should consider being tested for Lyme disease. Yet while lab tests are crucial for proper and perhaps life-saving treatment, they also have a low accuracy rate, leading many patients to become victims of a medical laboratory misdiagnosis.
Read Also: Rentals In East Lyme Ct
Lyme Disease Testing: How It Works
Two common lab tests for Lyme disease are the enzyme immunoassay test and the Western blot test. These tests measure the antibodies that form when someone is infected with Borrelia burgdorferi .
Enzyme immunoassay test
The EIA test is whatâs typically used to screen for Lyme disease by detecting antibodies for B. burgdorferi.
According to the Centers for Disease Control and Prevention, if the EIA test shows negative for the antibodies, no further testing is needed. However, if this screening test comes back with results that are positive or unclear, a second round of testingâusing the Western blot methodâis recommended. This second test is referred to as a confirmatory test.
Western blot test
When the EIA test is positive, the Western blot test is usually done next. This two-step approach to Lyme disease testing helps reduce the number of false positives. The Western blot test detects antibodies for several proteins belonging to Lyme bacteria.
If My Dog Tests Positive Does He Need To Be Treated
The decision to treat Lyme disease is somewhat controversial since many infected dogs show no signs of illness. Factors that would support treatment include:
a moderate to high value of QC6 signs of illness compatible with Lyme disease at the time of testing a history of illness compatible with Lyme disease within the past year the presence of abnormal levels of protein in the urine.
Don’t Miss: How To Get Energy With Lyme Disease
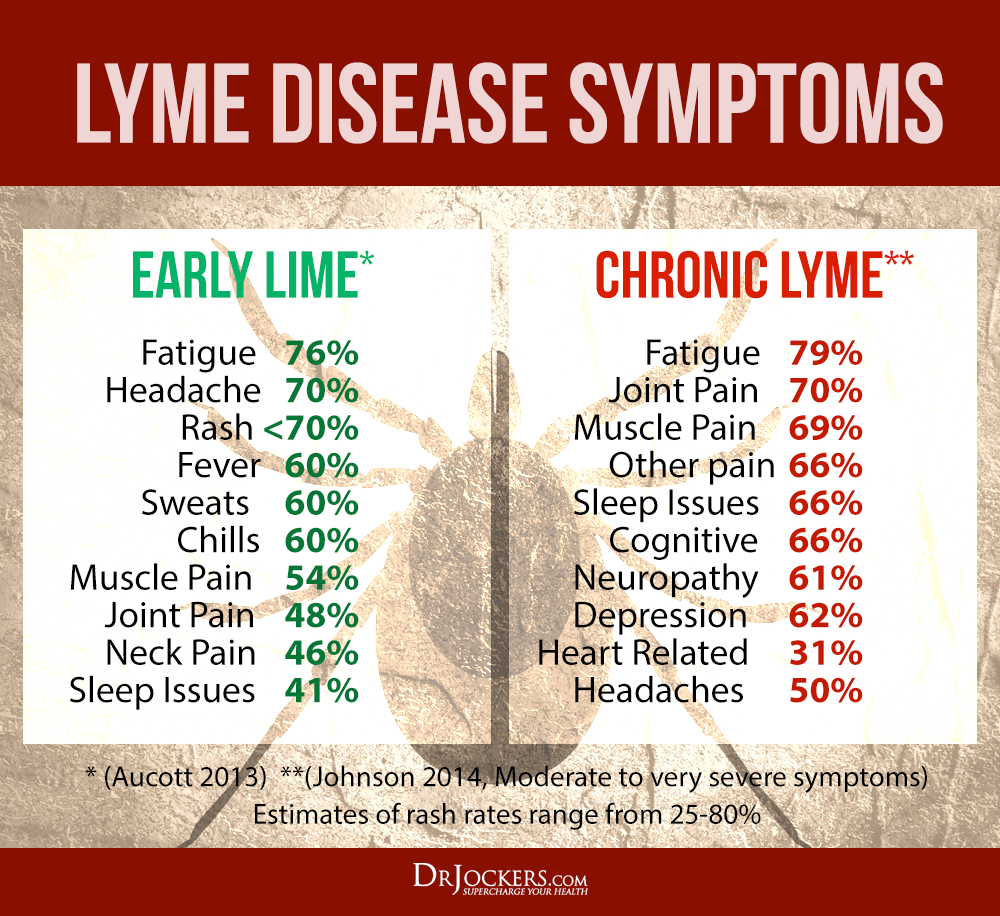
What Are The Symptoms Of Lyme Disease
Lyme Disease is a bacterial infection that results from a tick bite. The symptoms vary, and you can feel sick for months because of it. Some of the most common symptoms of Lyme disease are flu-like symptoms such as fever, chills, and headache. A rash can also occur in 70 to 80 percent of infections. If left untreated, the symptoms can worsen into facial palsy, dizziness, heart palpitations, and more.
What Is The Difference Between This Indirect Blood Diagnostic Test And A Direct Test
Direct diagnostic tests measure the presence of the bacteria directly and are much more reliable than tests looking for indirect measurement of antibodies that measure a persons immune response to an infection. Lyme disease diagnoses and disease management would benefit from validated diagnostic tests that directly measure the infection such as a culture, PCR test, or antigen detection tests. Direct tests are vital to the management of other infectious diseases such as HIV, hepatitis C, strep, and COVID-19, but have not yet become widely available for Lyme disease.
Also Check: Lyme Disease Doctors In Maine
Lyme Disease Diagnostics Research
There is a great need to develop rapid, point-of-care tests to determine whether people are infected with Borrelia burgdorferi, the bacterium that causes Lyme disease. NIAID is committed to improving Lyme disease diagnostics by supporting innovative research projects.
Priorities include finding potential targetssubstances that new diagnostic tools might measure in patient samplesand improving the sensitivity and specificity of currently available diagnostic tests, thereby leading to more accurate results.
Testing For Lyme Disease In Dogs
Lyme disease spread by ticks can be diagnosed with a simple blood tests in your veterinarians clinic. The C6 test is very sensitive and specific at diagnosing cases of Lyme disease and depending on clinical signs and concurrent results, treatment may be started immediately. If treatment has been successful, reductions in the QC6 at six months should be lower than the starting point.
Dont Miss: Beach Houses For Sale In Old Lyme Ct
Recommended Reading: How To Prevent Lyme Disease
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
What Is The Deer Ticks Range Who Is At Risk Of Infection

There are about 900 known species of ticks in the world, but only one Ixodes scapularis, the deer tick carries the bacteria that causes Lyme disease. If you live west of Texas, youre beyond the deer ticks range and probably dont need to worry about Lyme disease. If you live anywhere on the east coast, however, you should take the possibility of infection seriously especially if you live in one of these 14 states, which, according to the CDC, were collectively responsible for 96% of all confirmed U.S. cases in 2014:
- Connecticut
- Virginia
- Wisconsin
While are common, deer ticks generally make their homes in grassy, wooded areas, such as lawns, fields, and forests. Therefore, if you routinely participate in outdoor hobbies like camping, hiking, fishing, or hunting, youre at an increased risk for contracting Lyme disease. Youre also at increased risk if you have an outdoor pet, which can pick up ticks and bring them into your home.
You May Like: Can Lyme Disease Cause Asthma
Ehrlichia Anaplasma And Rickettsia
These microbes have the potential to cause severe illness therapy should not await laboratory diagnosis if acute infection with any of these microbes is suspected. Blood can be drawn when therapy is initiated to confirm the infection.
The most accurate test is serial serology using Indirect Immunofluorescent Assay . Diagnosis relies on a four-fold rise in antibody titer over several weeks. The first sample should be taken as early in the disease process as possible, and the second sample taken two to four weeks later.
PCR is 60-85% effective for diagnosing ehrlichia and 70-90% effective for diagnosing anaplasma, but its less valuable for diagnosing Rocky Mountain spotted fever . Accuracy for diagnosing chronic infection is unknown. There are many new species of these microbes being discovered for which routine testing is not yet available.
Testing And Diagnosing Coinfections And Related Microbes
There are quite a few microbes spread by blood-sucking insects that have stealth characteristics similar to those of Borrelia burgdorferi some we know about, and others still waiting to be discovered.
They all have stealth characteristics and the ability to infect and thrive inside cells. They are masters of evading the immune system, and can be even harder to diagnose than borrelia. Symptoms profiles are similar to borrelia and related mostly to stimulation of cytokine cascades, not concentrations of microbes. Though they each have slightly different strategies, their motive is the same: complete a lifecycle stage within the host and move on.
The primary known players in chronic Lyme include mycoplasma, bartonella, and chlamydia species. The most well-known species of babesia, anaplasma, ehrlichia, and rickettsia are more apt to cause acute illness and less apt to be associated with chronic illness, but research is discovering lesser known and lesser virulent species of these microbes that are associated with chronic Lyme. Reactivation of herpes-type viruses is common in chronic Lyme.
Though testing is possible for some species of these microbes, when a natural route of recovery is chosen, extensive testing is not necessary and can actually be very misleading.
You May Like: How Long Does A Lyme Blood Test Take
Pcr For B Burgdorferi
Short for Polymerase Chain Reaction, a PCR tests directly for borrelia DNA in the hosts blood, tissues, or urine. Historically, PCR has had limited accuracy, but improvements in technique are allowing PCR for microbial DNA to be the future of testing. At some point, it may be possible to define a persons entire microbiome.
For now, testing is available for the most common species of borrelia and many common species of coinfections with other stealth microbes. Testing is most accurate during acute infection, and much less accurate during chronic infection.
Again, the bottom line is that if you have many or most symptoms of chronic Lyme disease, then you are likely harboring at least one species of borrelia and several other species of stealth microbes no matter what the testing shows.
Many companies are offering microbial DNA testing, but a few are taking the lead. DNA Connexions tests DNA in either blood or urine specimens for three species of borrelia and several of the most common coinfections. Testing kits are available online.
Are There Any Risks To Lyme Disease Tests
There is very little risk to having a blood test or a lumbar puncture. If you had a blood test, you may have slight pain or bruising at the spot where the needle was put in, but most symptoms go away quickly. If you had a lumbar puncture, you may have pain or tenderness in your back where the needle was inserted. You may also get a headache after the procedure.
Recommended Reading: What’s The Cure For Lyme Disease
Where Is Lyme Disease Found
In the United States, Lyme disease has been reported in every state, but over 95% of cases are from the Northeastern, Mid-Atlantic, and upper Midwestern states, with a small number of cases reported along the West Coast, especially Northern California. In Canada, Lyme-positive dogs are found mostly in southern Ontario and southern Manitoba, with a small number of cases in southern Quebec and the Maritime provinces.
Read Also: What Is The Best Antibiotic To Treat Lyme Disease
Getting Tested For Lyme Disease
Lyme disease testing is usually ordered by a doctor and is used when there are signs or symptoms consistent with Lyme disease.
A blood sample can be drawn in a doctors office or other medical setting. If a test of cerebrospinal fluid is needed, an outpatient procedure called a lumbar puncture can be done in a hospital. Samples are then analyzed in a credentialed laboratory.
Don’t Miss: Lyme Booster Shot For Dogs
Avoid Unnecessary And Unscientific Testing
As part of the admirable Choosing Wisely campaign to reduce unnecessary tests and treatments, the American College of Rheumatology warns:
Dont test for Lyme disease as a cause of musculoskeletal symptoms without an exposure history and appropriate exam findings.
The CDC , French Society of Internal Medicine, and other experts around the world have expressed similar sentiments to the ACR.
Experts also warn against unvalidated testing . Quackwatch and Science-Based Medicine both provide accessible explanations about the differences between validated and unvalidated tests.
How Is Lyme Disease Diagnosed How Reliable Are These Lab Tests
There are several tests available to diagnose Lyme disease. The CDC recommends using a two-part process. If the first step, called an EIA , yields a positive result or is difficult to interpret, a second step, called a Western Blot test, is used for confirmation.
Unfortunately, these and other diagnostic methods are beset by shortcomings, particularly methods which rely upon blood samples. According to the Lyme Research Alliance, Lyme disease blood testing is fraught with problems and, at best, should only be an adjunct to the clinical diagnosis of the disease a statement which appears to align with observations by medical researchers. For example, consider this excerpt from a 2012 study published in Open Neurology Journal :
In considering the diagnosis of Lyme disease, a major problem is the inability of documenting the existence and location of the bacteria. After the initial transfer of the bacteria from the Ixodes tick into the person, the spirochetes spread locally, but after an initial bacteremic phase, the organisms can no longer be reliably found in body fluids Currently, the use of circulating antibodies directed against specific antigens of the Lyme borrelia are the standard means to diagnose the disease, but specific antibodies are not an adequate means to assess the presence or absence of the organism.
- ADD
Recommended Reading: Lyme Vaccine For Dogs How Often
How We Chose The Best At
When evaluating the companies for the best at-home Lyme disease tests, we looked at several key factors in order to provide you with the best information. For one, accuracy was extremely important, so we looked at testing centers with the best reviews and certifications. Every test mentioned in this article has been evaluated and awarded for their laboratory accuracy when dealing with their at-home tests.
Since Lyme disease is so severe and a misdiagnosis can have awful repercussions, we also considered how others reviewed the at-home tests.
First Comes Igm Then Igg
The pathogenesis and the different stages of infection should inform laboratory testing in Lyme disease.
It is estimated that only 5% of infected ticks that bite people actually transmit their spirochetes to the human host. However, once infected, the patients innate immune system mounts a response that results in the classic erythema migrans rash at the bite site. A rash develops in only about 85% of patients who are infected and can appear at any time between 3 and 30 days, but most commonly after 7 days. Hence, a rash occurring within the first few hours of tick contact is not erythema migrans and does not indicate infection, but rather an early reaction to tick salivary antigens.
Antibody levels remain below the detection limits of currently available serologic tests in the first 7 days after exposure. Immunoglobulin M antibody titers peak between 8 and 14 days after tick contact, but IgM antibodies may never develop if the patient is started on early appropriate antimicrobial therapy.
If the infection is not treated, the spirochete may disseminate through the blood from the bite site to different tissues. Both cell-mediated and antibody-mediated immunity swing into action to kill the spirochetes at this stage. The IgM antibody response occurs in 1 to 2 weeks, followed by a robust IgG response in 2 to 4 weeks.
Because IgM can also cross-react with antigens other than those associated with B burgdorferi, the IgM test is less specific than the IgG test for Lyme disease.
Also Check: How Much Is A Lyme Disease Test