Can Lyme Disease Be Prevented
To prevent Lyme disease, you should lower your risk of getting a tick bite:
- Avoid areas where ticks live, such as grassy, brushy, or wooded areas. If you are hiking, walk in the center of the trail to avoid brush and grass.
- Use an insect repellent with DEET
- Treat your clothing and gear with a repellant containing 0.5% permethrin
- Wear light-colored protective clothing, so you can easily see any ticks that get on you
- Wear a long-sleeve shirt and long pants. Also tuck your shirt into your pants and your pant legs into your socks.
- Check yourself, your children, and your pets daily for ticks. Carefully remove any ticks you find.
- Take a shower and wash and dry your clothes at high temperatures after being outdoors
Centers for Disease Control and Prevention
Babesia And Lyme Its Worse Than You Think
Babesia, a tick-borne infection that causes malaria-like symptoms, has been making headlines over the past two years as the number of reported cases increases, and concerns grow over the seriousness of the disease and its ability to be transmitted through the blood supply.
Although Lyme disease is the most talked about tick-transmitted disease, Babesia is more common than you might think. In the 2015 issue of Trends in Parasitology, Diuk-Wasser and colleagues report that up to 40% of patients with Lyme disease experienced concurrent Babesiosis.
This means that out of the estimated 300,000 cases of Lyme disease reported annually in the U.S., 120,000 of those individuals may also have Babesia. This is particularly alarming given that the disease can go undetected in asymptomatic individuals and is transmissible through blood transfusions or congenitally. Additionally, Babesia requires different treatment than Lyme disease.
The Babesia microti parasite that leads to Babesia is commonly seen in blacklegged deer ticks. But according to the authors, its also common to find ticks and enzootic hosts carrying both Borrelia burgdorferi and B. microti. In fact, between 12% and 42% of rodents are co-infected with both agents. This would suggest that coinfection provides a survival advantage for both pathogens.
Babesia difficult to diagnose
Treating Babesia
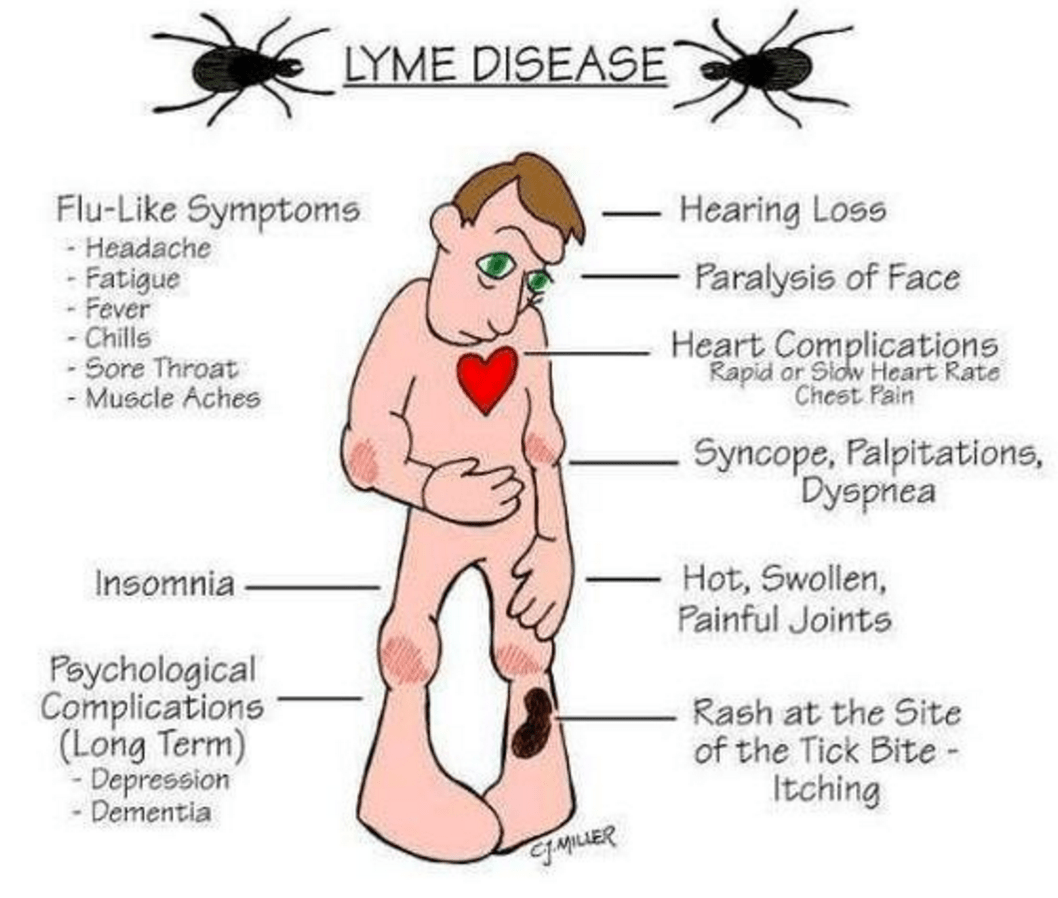
What Are The Signs And Symptoms Of Lyme Disease
Signs and symptoms of Lyme disease depend on how long youve been infected. If youre pregnant and have been bitten by a tick or live in or travelled to an area with Lyme disease, talk to your health care provider.
Early signs and symptoms include:
- A rash called erythema migrans . This rash looks like a bulls eye around where the tick bit you. It may feel warm and may or may not be itchy.
- Fatigue
- Fever and chills
- Headache
- Muscle and joint pain
- Swollen lymph nodes. Lymph nodes are glands throughout the body that help fight infection. You usually cant feel them unless theyre swollen.
Later signs or symptoms include:
- Being short of breath
- Facial paralysis. This is when you cant feel or move parts of your face.
- Joint pain and swelling
Don’t Miss: Lyme Disease And Neurological Problems
What Is Late Lyme Disease
Lyme disease, also known as Lyme borreliosis, is caused by an infection with the bacteria Borrelia burgdorferi. This bacteria is disseminated through tick bites. Infected ticks usually bite small mammals, who do not develop any kind of infection from the bacteria. When humans are exposed to B. Burgdorferi from a tick bite, however, they can develop Lyme disease.
People who work outside or spend time in woodland areas, where there is greater potential for exposure to tick bites, are most at risk of infection.
Lyme disease is a condition which progresses in stages:
How To Prevent Post
While you may not be able to prevent post-treatment Lyme disease syndrome, you can take precautions to prevent coming into direct contact with infected ticks. The following practices can reduce your likelihood of getting Lyme disease and developing persistent symptoms.
If a tick bites you, contact your doctor. You should be observed for 30 days for signs of Lyme disease. You should also learn the signs of early Lyme disease and seek prompt treatment if you think youre infected. Early antibiotic intervention may reduce your risk of developing chronic symptoms.
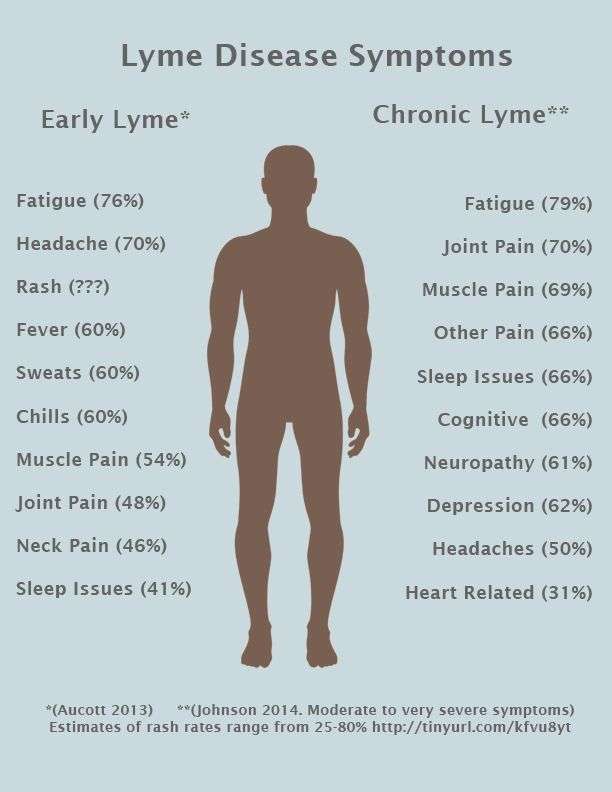
The signs of early Lyme disease can occur from 3 to 30 days after a bite from an infected tick. Look for:
- a red, expanding bulls-eye rash at the site of the tick bite
Recommended Reading: Signs My Dog Has Lyme Disease
Chronic Lyme Disease Patients Profoundly Debilitated
Many patients with chronic Lyme disease are profoundly debilitated. Investigators of the four NIH-sponsored retreatment trials documented that the patients quality of life was consistently worse than that of control populations and equivalent to that of patients with congestive heart failure. Pain levels were similar to those of post-surgical patients, and fatigue was on par with that seen in multiple sclerosis.
An LDo published survey of over 3,000 patients with chronic Lyme disease found that patients suffer a worse quality of life than most other chronic illnesses, including congestive heart failure, diabetes, multiple sclerosis and arthritis. Over 70% of patients with chronic Lyme disease reported fair or poor health. Similar results have been found in other studies. Many of the symptoms associated with Lyme disease are common in other diseases. The CDC surveillance criteria for confirmed cases specifically exclude most of the symptoms that patients report, including fatigue, sleep impairment, joint pain, muscle aches, other pain, depression, cognitive impairment, neuropathy, and headaches. However, these common symptoms can be severe and may seriously affect quality of life.
What Is The Outlook For Someone With Lyme Disease
Most of the people who get Lyme disease and treated early will be fine.
Post-Lyme Syndrome
Even after proper treatment, some patients may experience lingering fatigue, achiness or headaches. This does not signify ongoing infection and will not respond to additional antibiotics. The majority of people in this group will have symptoms resolve over the next 1-6 months.
Chronic Lyme Syndrome
Chronic Lyme syndrome is a term used by some that includes the symptoms of Post-Lyme syndrome outlined above. This is a controversial topic with no accepted etiology and no proven cause or association.
Don’t Miss: How Does Lyme Disease Spread
Has Niaid Looked At Whether Infection Persists After Antibiotic Therapy
Several recent studies suggest that B. burgdorferi may persist in animals after antibiotic therapy. In one study, NIAID-supported scientists found that remnants of B. burgdorferi remained in mice after antibiotic treatment. Another team of NIAID-supported investigators found that intact B. burgdorferi persist in nonhuman primates after antibiotic treatment. It was not possible to culture these bacteria and it is not clear whether they are infectious. More recent work by Hodzic et al. replicated the earlier finding of persisting DNA but non-cultivatable B. burgdorferi after antibiotic treatment using a mouse model. In 2017, scientists at the Tulane National Primate Research Centers, funded in part by an NIH research resources grant, reported evidence of persistent and metabolically active B. burgdorferi after antibiotic treatment in rhesus macaques.
In a first-of-its-kind study for Lyme disease, NIAID-supported researchers have used live, disease-free ticks to see if Lyme disease bacteria can be detected in people who continue to experience symptoms such as fatigue or arthritis after completing antibiotic therapy). This study remains underway.
When Lyme Disease Never Ends: Post Treatment Lyme Disease Syndrome
Summer is officially here!
Do you have your outdoor activities checklist ready yet? Dont forget to add Stay-away-from-ticks to this list.
Lyme disease, caused by the bacteria Borrelia Burgdorferi from tick bites is a chronic condition characterized by an initial bullseye rash. The bacterial invasion hijacks the immune system resulting in susceptibility to co-infections, loss of cognitive function, and repeated reappearance of flu-like symptoms. Over time, many Lyme patients experience a worsening health curve.
An even uglier truth is post-treatment Lyme disease syndrome , a mysterious condition where chronic symptoms persist long after flushing out the pathogen from the body. The reason for recurring Lyme symptoms is not yet fully understood by the medical industry.
Today we are bringing PTLDS into the limelight to look at
- What is post-treatment Lyme disease syndrome ?
- How is it different from acute Lyme infection?
- Why do symptoms persist?
- How can Lyme disease be fully healed?
Lets take a closer look.
Also Check: How Do You Get A Tick Tested For Lyme Disease
What Are The Long Term Effects Of Lyme Disease
The long-term effects of Lyme disease, if untreated or inadequately treated, can vary from arthritis to severe neuropathy. Impaired memory can be seen in some cases and even heart is affected in some others. It is a disease which can cause serious long term effects if untreated or improperly treated.
There are some factors which can increase the risk of getting the Lyme disease. If one spends a lot of time in woods or grasslands, it creates a risk factor for Lyme disease, as ticks dwell more in this type of areas. Also, ticks get attached easily to the bare flesh. Hence, it is advisable to wear full clothing while going to a ticks-infested place. Also, protect your pets from ticks by keeping them away from grass and tall plants. If at all you see a tick on the body, it should be removed promptly and properly. If the tick stays on the body attached for more than 36 hours, it is likely to cause infection. Ticks being attached for less than that period usually do not cause infection.
Lyme disease may affect multiple organs and systems in our body. And hence, it is responsible for producing a wide range of symptoms, which are related to the affected organs. The incubation period for the bacteria may range from one to two weeks, from infection to symptom onset.
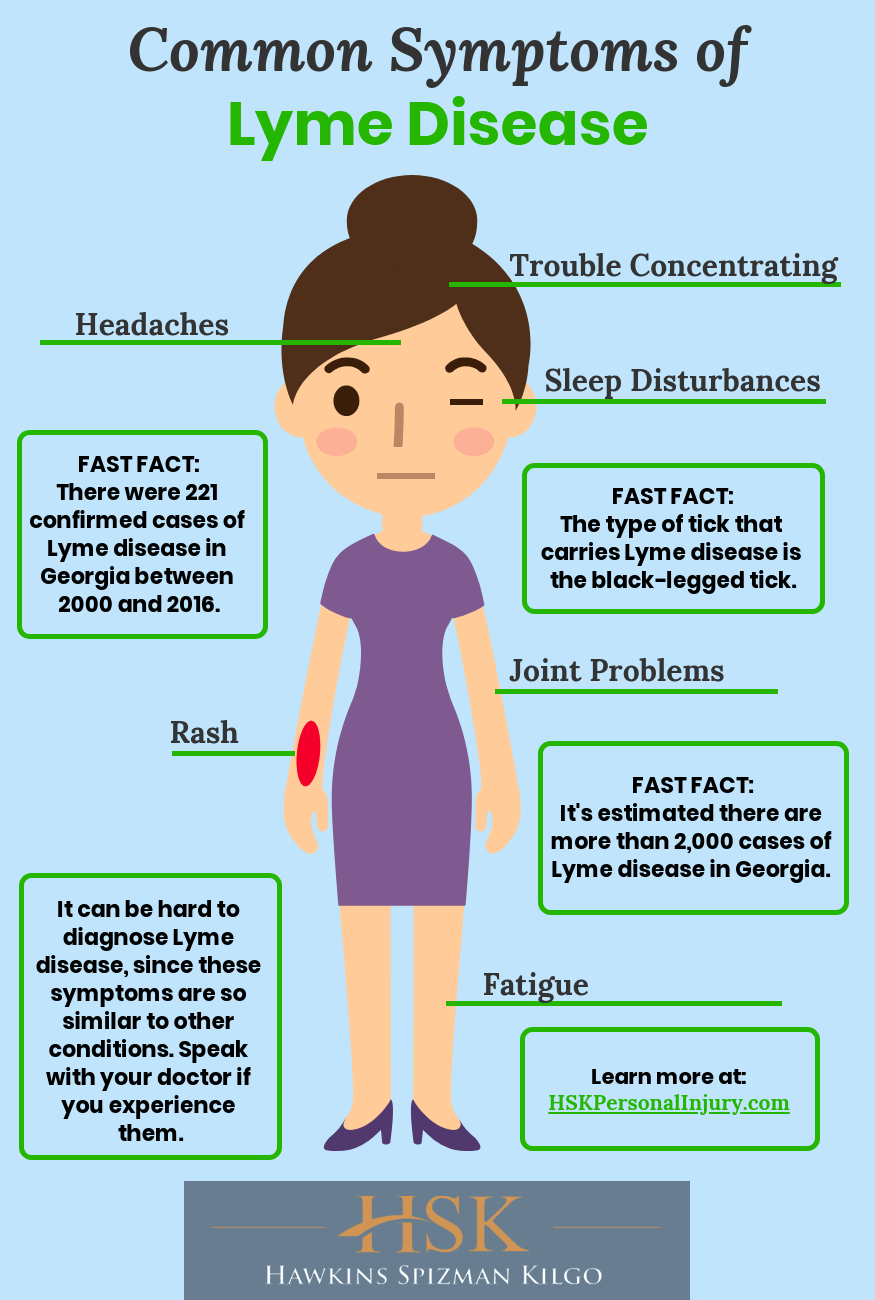
What Are The Symptoms Of Chronic Lyme Disease
Home » Tick Talk » What Are the Symptoms of Chronic Lyme Disease?
Despite some skepticism in the medical community, chronic Lyme disease is a growing epidemic in the U.S. This stems partly from the shortcomings of many of the officially recommended Lyme disease tests, which leave too many patients with untreated infections that then become persistent and debilitating.
The following article will cover what you should know about chronic Lyme and provide an introductory but non-exhaustive chronic Lyme disease symptoms checklist.
You May Like: Best Lyme Disease Doctors In Massachusetts
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
The Cortisol Connection: Are You Addicted To Your Pain
Cortisol, the stress hormone secreted by the adrenal glands, connects the limbic system to the rest of the body via the HPA axis. Chronic stress in the form of Lyme co-infections keeps the HPA axis functioning over time leading to cortisol addiction .
An autopilot cortisol addiction forces the body to remain in an eternal state of survival mode with unceasing PTLDS inflammation and chronic pain.
Also Check: Do You Get A Rash With Lyme Disease
Defining Patient Subgroups: Post
Patients with persistent symptoms related to Lyme disease likely represent a heterogeneous population, which includes previously untreated patients, as well as those treated patients who remain symptomatic. As a result, some will manifest primarily patient-reported symptoms while others will present with symptoms in conjunction with objective, physical findings. This heterogeneity is further complicated by variation in terminology and the definitions used by different groups in the field.
Figure 3. A schematic of clinical- and research-defined patient subgroups among those with persistent symptoms associated with Lyme disease . The size of each patient subgroup is not meant to represent actual population frequency, as prevalence data is extremely limited. IDSA, Infectious Diseases Society of America ILADS, International Lyme and Associated Diseases Society CLD-PT, Chronic Lyme Disease-Previously Treated CLD-U, Chronic Lyme Disease-Untreated IgG, Immunoglobulin G CFS, Chronic Fatigue Syndrome FM, Fibromyalgia.
Post Treatment Lyme Disease Syndrome Why Do Symptoms Persist
Why are symptoms seen, long after bacterial elimination?
Long-term stress combined with an acute infection can cause the limbic system to be hyper-activated. Our ability to detect danger or threats and activate a fight-or-flight reaction is primarily a function of the limbic system. A well-regulated limbic system in a healthy person is selectively triggered but knows when to return to homeostasis.
With chronic illnesses such as Lyme, we often see the limbic system become massively dysregulated. An impaired stress response tricks the mind and body to perpetually be in an ON fight or flight state.
Recommended Reading: What To Do If You Get Lyme Disease
What Do You Do If There’s A Tick Under Your Skin
Use a pair of fine-tipped tweezers to remove it as soon as possible. Pull upward with steady pressure. If parts of the tick are still in your skin, try to get those with the tweezers, too. After everything is out, clean the bite area with rubbing alcohol or soap and water.
You probably wonât get infected if you remove the tick within 36 to 48 hours.
How do you throw away a tick?
Put it in soapy water or alcohol, stick it to a piece of tape, or flush it down the toilet.
The Chance Of Getting Lyme Disease
Not all ticks in England carry the bacteria that causes Lyme disease.
But it’s still important to be aware of ticks and to safely remove them as soon as possible, just in case.
Ticks that may cause Lyme disease are found all over the UK, but high-risk places include grassy and wooded areas in southern and northern England and the Scottish Highlands.
Ticks are tiny spider-like creatures that live in woods, areas with long grass, and sometimes in urban parks and gardens. They’re found all over the UK.
Ticks do not jump or fly. They attach to the skin of animals or humans that brush past them.
Once a tick bites into the skin, it feeds on blood for a few days before dropping off.
Recommended Reading: Pcr Blood Test For Lyme Disease
How We Care For Lyme Disease
The Division of Infectious Diseases at Boston Children’s provides comprehensive care for children and adolescents with Lyme disease and other infections. Our services include consultation, evaluation, treatment, and management of long-term complications of Lyme disease.
The commitment and compassion with which we care for all children and families is matched only by the pioneering spirit of discovery and innovation that drives us to think differently, to find answers, and to build a better tomorrow for children everywhere.
Who Is At Risk For Lyme Disease
Anyone can get a tick bite. But people who spend lots of time outdoors in wooded, grassy areas are at a higher risk. This includes campers, hikers, and people who work in gardens and parks.
Most tick bites happen in the summer months when ticks are most active and people spend more time outdoors. But you can get bitten in the warmer months of early fall, or even late winter if temperatures are unusually high. And if there is a mild winter, ticks may come out earlier than usual.
Read Also: Apartments For Rent In East Lyme Ct
Lyme Light A New Integrative Healing Modality For Lyme Disease
Contrary to the conventional antibiotic-based strategy, Innovative Medicines approach is aimed at restoring complete health by taking into consideration the physical, mental, emotional, and spiritual dysfunction of the patient suffering from Lyme.
Read our article, A new integrative approach to Lyme disease, to see what sets us apart.
Azlocillin Comes Out On Top
The drug, which is not on the market, was tested in mouse models of Lyme disease at seven-day, 14-day and 21-day intervals and found to eliminate the infection. For the first time, azlocillin was also shown to be effective in killing drug-tolerant forms of B. burgdorferi in lab dishes, indicating that it may work as a therapy for lingering symptoms of Lyme disease.
Pothineni and Rajadas have patented the compound for the treatment of Lyme disease and are working with a company to develop an oral form of the drug. Researchers plan to conduct a clinical trial.
Rajadas is also a professor of bioengineering and therapeutic sciences at the University of California-San Francisco.
Other Stanford co-authors are Hari-Hara S. K. Potula, PhD, senior research scientist postdoctoral scholars Aditya Ambati, PhD, and Venkata Mallajosyula, PhD senior research scientist Mohammed Inayathullah, PhD and intern Mohamed Sohail Ahmed.
A researcher at Loyola College in India also contributed to the work.
The study was funded by the Bay Area Lyme Foundation and Laurel STEM Fund.
- Tracie White
Recommended Reading: Rocky Mountain Spotted Fever Vs Lyme Disease