How Is Lyme Disease Treated
Your healthcare provider will figure out the best treatment for you based on:
-
How old you are
Lyme disease in the earliest stage is usually treated with antibiotics for 2 to 3 weeks.
Treatment will also be considered based on these and other factors:
-
If you are bitten by a tick that tests positive for the bacteria that causes Lyme disease
-
If you are bitten by a tick and have any of the symptoms
-
If you are bitten by a tick and are pregnant
-
If you are bitten by a tick and live in a high-risk area
Contemporary Infection With Anaplasma Phagocitophilum And Babesia Species
Bb sensu lato, Anaplasma phagocytophilum and Babesia share very similar epidemiology and trasmission cycles, having hard ticks as vectors and white-footed mice and white-tailed deer as reservoir hosts .
Since Bb, Anaplasma phagocitophilum and Babesia may be co-transmitted by Ixodes ticks bite, the clinical features of acute and chronic disease can be atypical, complex and variable .
In an original study, Krause et al. analysed clinical and laboratory features as well as short-term complications in 192 people living in New England who experienced infections due to Bb and or Babesia and Ehrlichia. The Authors found that erythema migrans is very peculiar of LD alone, whereas flu-like symptoms are more suggestive of LD concurrent with babesiosis and/or HGA. However, LD itself in small percentage can present with fever, chills and headache. Such an epidemiologic report is confirmed also in Europe: in an Italian study conducted on more than 700 people living in an endemic area for LD, flu-like symptoms as fever, myalgia and headache preceded, accompanied or were the only clinical sign of LD in 16.88% of patients .
In contrast with other reports , Krause et al. found that the presence of a co-infection does not help Bb to spread more rapidly into blood, skin, joint, nervous system and heart .
How Is Lyme Disease Diagnosed
Lyme disease is difficult to diagnose because symptoms are not consistent and may mimic other conditions. The primary symptom is a rash, but it may not be present in up to 20% of cases.
Diagnosis for Lyme disease must be made by a healthcare provider experienced in recognizing Lyme disease. Diagnosis is usually based on symptoms and a history of a tick bite. Testing is generally done to confirm the diagnosis and rule out other conditions. This may need blood and other lab tests.
Research is underway to develop and improve methods for diagnosing Lyme disease.
The symptoms of Lyme disease may look like other medical conditions or problems. Always talk with your healthcare provider for a diagnosis.
Don’t Miss: What Is Chronic Lyme Disease In Humans
Psychiatric Presentations And Other Symptoms
Some patients exhibit a streak-mark rash that resembles stretch marks. Symptoms may include fever, headaches, fatigue, and swollen glands.
Several studies indicate an association between Bartonella and psychiatric symptoms. Investigators describe case studies of patients with new-onset psychiatric symptoms such as sudden agitation, panic attacks, and treatment-resistant depression possibly due to Bartonella.
Another case study highlights a young boy with a Bartonella infection who developed neuropsychiatric symptoms and was later diagnosed with pediatric acute-onset neuropsychiatric syndrome , a type of basal ganglia encephalitis.
Bartonella can be treated with antibiotics such as doxycycline, minocycline, azithromycin, trimethoprim-sulfamethoxazole, clarithromycin, and Rifampin.
STARI is an emerging tick-borne illness related to Lyme disease and was identified in the southeastern and south-central United States.
STARI is believed to be transmitted by the Lone Star tick however, it is not officially confirmed as of yet.
The hallmark sign of STARI is an EM-like rash similar to that seen in Lyme disease. Symptoms may include fevers, headaches, stiff neck, joint pain, and fatigue.
The long term consequences and treatment of the illness have not been established.
It is not known whether antibiotic treatment is necessary or beneficial. Nevertheless, because STARI resembles early Lyme disease, physicians will often treat patients with oral antibiotics.
Transmission Of The Bartonella Bacteria
Bartonella bacteria are known to be carried by fleas, body lice and ticks, and theres high suspicion that ticks transmit it to humans. People with tick bites and no known exposure to cats have acquired the disease. People who recall being bitten by ticks have been co-infected with the Lyme spirochete and bartonella. Scientists have recently established that ticks can transmit Bartonella to mice. More research needs to be done to establish the role of ticks in spreading the disease. In addition, a recent study suggests that bartonella may be passed from mother to unborn child .
Don’t Miss: Town Of East Lyme Jobs
What Can You Do If You Do Get A Tick Bite
If you do get a tick bite, be sure and take care of the wound properly. The CDC gives guidelines on how to properly remove a tick here. To be on the safe side, I recommend placing in in a plastic bag and send it off for testing, you can google in your local area labs that do this type of testing or call your local doctors office. Once your remove the tick you can apply lavender essential oil to the bite every 5 minutes for half an hour. If you notice any flu-like symptoms or a bulls eye rash follow up quickly with your integrative health care team.
What Should You Do If You Find A Tick
-
Don’t touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Don’t squeeze the tick, and don’t use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
You May Like: How Many People Die From Lyme Disease
Nymphal And Adult Ticks Shown To Be Co
Studies have looked at co-infection rates at different points in the ticks life cycle. In a comprehensive review of 61 different published reports, Nieto and Foley found that 2 to 5 percent of young nymphal I. scapularis ticks were reported to be co-infected with more than one microbe. Adult tick co-infection rates with B. burgdorferi varied widely between 1 to 28 percent across the reports analyzed :93-101, 2009). Although humans are more likely to be bitten by the smaller nymphal stage ticks , co-infection rates in adult ticks may provide important information about how tickborne diseases are transmitted.
Co-infection by some or all of these other microbes may make it more difficult to diagnose Lyme disease. Being infected by more than one microbe might also affect how the immune system responds to B. burgdorferi . NIAID-supported studies of mice found that co-infection with human granulocytic ehrlichiosiswhich is now known as anaplasmosisresults in more severe Lyme disease. Another study showed that when mice were co-infected with Babesia microti and B. burgdorferi, the presence of Babesia also enhanced the severity of Lyme disease, while the presence of B. burgdorferi appeared to limit the effects of Babesia.
Babesia And Lyme Disease
Babesia is often present with Lyme disease and can increase the severity of Lyme disease. One study found patients co-infected with Lyme disease and Babesia experienced fatigue, headache, sweats, chills, anorexia, emotional lability, nausea, conjunctivitis, and splenomegaly more frequently than those with Lyme disease alone.
Babesia can also increase the duration of illness with Lyme disease. One study found that 50% of co-infected patients were symptomatic for 3 months or longer, compared to only 4% of patients who had Lyme disease alone.
Also Check: Flower Delivery East Lyme Ct
About This Research Topic
Lyme disease , caused by Borrelia burgdorferi sensu lato , is the most common tick-borne disease in North America and Eurasia. Besides LD, ticks are also capable of transmission of other bacterial pathogens, including those of the genera Anaplasma, Ehrlichia, Babesia, Rickettsia, as well as …
Keywords:coinfections, tick-borne diseases, interaction, Lyme disease, babesiosis
Important Note: All contributions to this Research Topic must be within the scope of the section and journal to which they are submitted, as defined in their mission statements. Frontiers reserves the right to guide an out-of-scope manuscript to a more suitable section or journal at any stage of peer review.
How Can You Repel Ticks
The CDC recommends dousing yourself with the toxin DEET to prevent tick bites, but certain plants have been found to work just as well.1-3 You can mix equal parts of lavender, geranium, juniper and tea tree essential oils and apply to your clothing. Although you can apply to your skin as well, use caution with children as some essential oils are very strong.
You May Like: Can You Fully Recover From Lyme Disease
What Are Lyme Disease Co
A Lyme disease co-infection occurs when you contract more than one infection from the same tick at the same time.
Lyme disease is caused by the bacteria Borrelia burgdorferi, but ticks can carry other strains of bacteria, parasites and viruses that are transmitted when they bite you. According to LymeDisease.org, since the condition was first reported in the 1980s, scientists have identified over 15 tick-related infections or illnesses that are transmitted to humans and they continue to identify more.
Co-infections are common in those diagnosed with Lyme disease. One study found that 53.3 percent of survey participants had at least one co-infection. Nearly 30 percent of the same group were diagnosed with two or more co-infections. The co-infections youre most likely to have depend on where you live and the ticks common in your area.
Is There A Treatment For Lyme Disease

Traditional approaches to Lyme disease include to treat the infection with borrelia with the use of antibiotics. Most experts agree that 2-4 weeks of antibiotic therapy is indicated for acute Lyme disease, or immediately after infection. Many advocate up to 9 months of antibiotic therapy, even though there are no studies supporting long-term antibiotic use.4 This method is based on the germ theory i.e. that if the germ is killed then the host will recover. However antibiotics will wipe out the bad bacteria as well as the good bacteria leaving your microbiome severely unbalanced and most importantly your immune system weak. In addition the initial symptoms of Lyme disease are flu-like so often go undetected until they become chronic. The CDC and IDSA5 , do not recommend antibiotic treatment unless you have an official diagnosis of Lyme disease.
An integrative approach focuses on strengthening the body to allow the bodys innate healing capacities to thrive. Our 5 Step Plan not only is focused on healing Lyme disease but also creating long term wellness and not another disease to deal with down the road potentially from the treatment methods.
Don’t Miss: Early Detection Of Lyme Disease
Ticks Harbor Multiple Pathogens
According to a study in Suffolk County, Long Island, more than half of the ticks collected were harboring at least one pathogen. The causative agent of Lyme disease, Borrelia burgdorferi was the most prevalent , followed by Babesia microti .
Furthermore, researchers found that among infected ticks collected, 45% were co-infected and carried up to 5 different pathogens. The most prevalent co-infections included Bartonella henselae and Rickettsia of the spotted fever group .
Skin Manifestations Of Babesiosis
- Skin manifestations of babesiosis are rare and difficult to separate out from those of Lyme disease. Co-infection with Babesia may alter the skin manifestations of Lyme disease.
- No consistent skin manifestation of babesiosis has been found.
- Rash has been identified as the presenting symptom in around 12% of patients hospitalised with babesiosis.
- Petechiae and bruises may occur, most likely due to thrombocytopenia .
- Jaundice has been reported, most likely due to lysis of red blood cells.
Read Also: Doxycycline Dosage For Lyme Disease
Summary Of The Clinical Symptoms And The Treatment Of Lyme Disease And Chronic Co
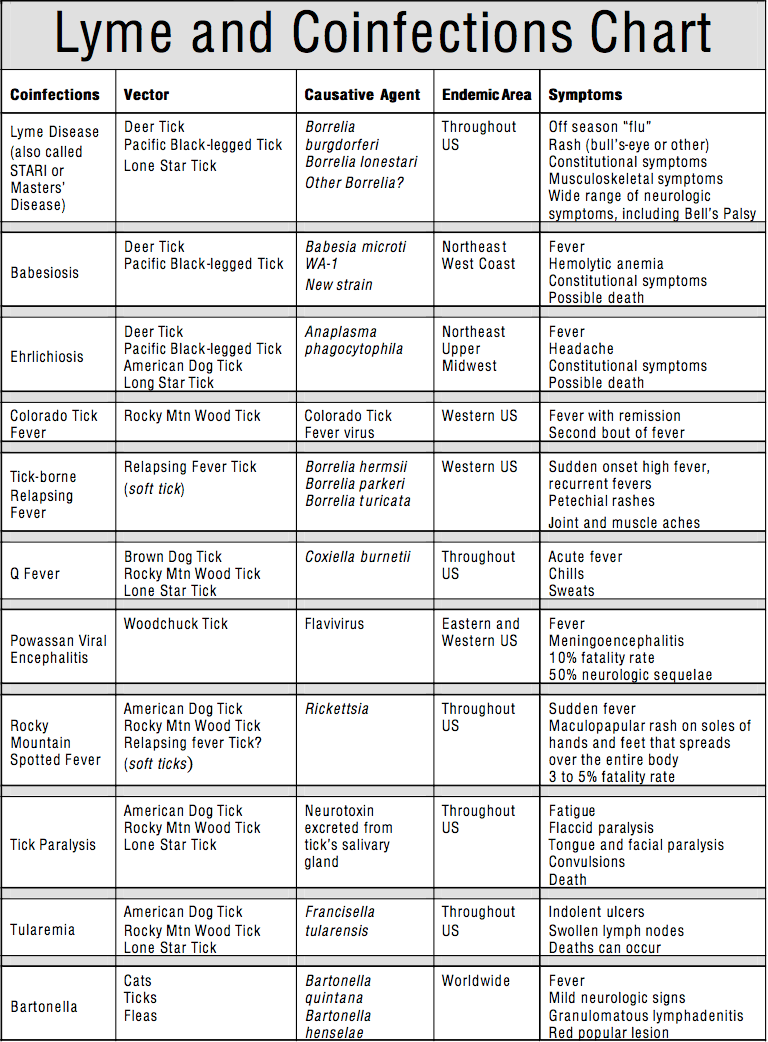
An informative overview of the different disease manifestations of Lyme disease and the significant co-infections is given in Table . The overview shows than there is substantial overlap in symptoms in cases of Lyme disease, bartonellosis, Yersinia enterocolitica and Mycoplasma pneumonia infections. Additionally, Chlamydophila pneumoniae also exhibits some overlap in the symptomatology with Lyme disease. Chlamydia trachomatis and Campylobacter jejuni are primarily characterized by reactive arthritis and rarely by Guillain-Barré syndrome. Only in cases with chronic Lyme disease does the antibiotic treatment involve the use of cephalosporins of the 3rd generation and, if necessary, of carbapenems. Otherwise, the focus is generally on tetracyclines, macrolides, to some extent on quinolones, particularly gemifloxacin, all of which, exhibit an intracellular and extracellular efficacy.
What You Need To Know About Lyme Disease
-
Lyme disease is an infection caused by the spiral-shaped bacteria Borrelia burgdorferi, which is most commonly transmitted by a tick bite.
-
There are over 300,000 estimated new cases of Lyme disease in the United States each year.
-
The symptoms of Lyme disease depend on the how long the infection has been present in the body. The first sign of Lyme disease is often an expanding round or oval red “bullseye” rash.
-
If left untreated, people may develop neurological symptoms and heart problems, and have an approximately 60 percent chance of developing Lyme arthritis.
Read Also: Neurological Disorders From Lyme Disease
Is It Lyme Or A Co
byJennifer Crystalon April 26, 2022
In addition to Lyme disease, ticks can transmit a variety of co-infections that make it more difficult to receive an accurate diagnosis and complicate the healing process.
As tick populations and Lyme disease cases increase, Lyme disease awareness is thankfully growing. Now, when I say I have long-haul Lyme disease, more people understand what that means. But as Lyme literacy has improved, so has the specificity of my vocabulary. Instead of just saying I have Lyme disease, or several chronic illnesses, I make a point to say that I have Lyme and other tick-borne diseases. Sure, its a mouthful, and sure, I sometimes get blank stares, but any awkwardness is worth the opportunity to raise awareness about co-infections. Knowing their signs and symptoms, and how they are similar and different to Lyme disease, can be lifesaving.
Co-infections are other diseases that are transmitted by ticks. Some are transmitted by black-legged ticks, the same ticks that transmit Lyme disease, and some are transmitted by other types of ticks . You can get Lyme disease and one or more co-infections from a tick bite. Or, you can get only a co-infection, but not Lyme disease.
As you head outside this spring and summer, dont just be Lyme awarebe tick aware. Take precautions to prevent tick bites so that you can avoid all tick-borne diseases, and keep all co-infections in mind if you, a family member, or a pet do get a tick bite.
Here’s What You Need To Know About Lyme Disease Co
Most people with Lyme disease respond favorably to proper treatment, especially when their infection is caught early. For some, however, the aftermath of a tick bite can be much worse as those little buggers can transmit more than one infection at a time.
As a result, your Lyme disease symptoms may worsen and you could have symptoms that confuse your doctor because theyre not associated with Lyme disease at all. You feel worse for longer and the usual treatments for Lyme disease dont kick the illness as expected. The cause of your severe case of Lyme disease? It may be a co-infection.
Also Check: Is Joint Pain A Symptom Of Lyme Disease
What Are Some Of These Co
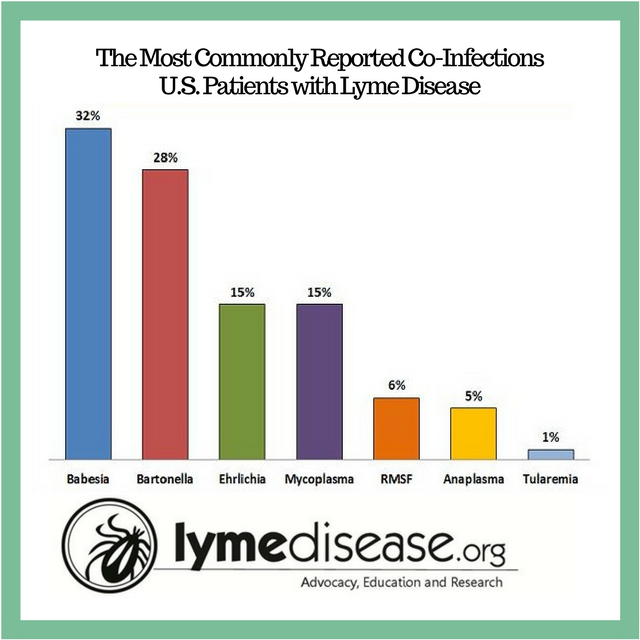
According to LymeDisease.org, the most common Lyme disease co-infections are reported in the following order from most to least common:
Red Cell Invasion And Lysis
After attachment and entry into the erythrocyte, babesia organisms mature into trophozoites that eventually undergo asexual budding to yield two or four daughter cells known as merozoites. Released into the bloodstream, free merozoites quickly invade nearby red blood cells to ensure persistence of the infection in the host.
Erythrocyte lysis is associated with many of the clinical manifestations and complications of babesiosis, including fever, anemia, jaundice, hemoglobinemia, hemoglobinuria, and renal insufficiency. The absence of synchrony in asexual reproduction of the parasite may explain the lack of massive hemolysis associated with babesiosis and therefore the milder clinical presentation of babesiosis when compared with malaria.
You May Like: Early Signs Of Lyme Disease In Adults
How Can Babesiosis Be Prevented
- Those at risk of severe infection with babesiosis should avoid endemic areas between May and October.
- Long-sleeved clothing and pants should be worn when outdoors, to cover as much skin as possible.
- DEET insect repellent should be applied to skin and clothes.
- Ticks must remain attached for at least 24 hours to transmit Babesia. Therefore early removal of ticks from humans and pets should prevent transmission of disease. Careful daily checks for ticks are important as the tick may be as small as a poppy seed.
- McGinley-Smith DE, Tsao SS. Dermatoses from ticks. J Am Acad Dermatol. 2003 49:363-92
Diagnosis Testing And Treatment
You may have heard that the blood test for Lyme disease is correctly positive only 65% of the time or less. This is misleading information. As with serologic tests for other infectious diseases, the accuracy of the test depends upon how long youve been infected. During the first few weeks of infection, such as when a patient has an erythema migrans rash, the test is expected to be negative.
Several weeks after infection, FDA cleared tests have very good sensitivity.
It is possible for someone who was infected with Lyme disease to test negative because:
If you are pregnant and suspect you have contracted Lyme disease, contact your physician immediately.
- Report being bitten by a tick, or
- Live in, or have recently visited, a tick-infested area.
You May Like: What Does Lyme Disease Do To You