Can Individuals Be Re
Relapses are recurrent symptoms that are the result of failure to cure the original infection, whereas re-infection is the recurrence of symptoms as a result of a new exposure to an infected tick, leading to a new infection. Although erythema migrans lesions can relapse if not treated with antibiotics , their recurrence after successful treatment is more likely to be re-infection than relapse .
Re-infection can occur in as many as 2%21% of patients living in endemic areas who have had Lyme disease . On examination, re-infection typically presents with an erythema migrans lesion at a different site than the original lesion more than 12.5 years after the original infection and not within 11 months of the first infection . In one series, 79% of patients with re-infection presented with erythema migrans at a different site than the previous infection, and 21% presented with a febrile illness with myalgias. Re-infection after late Lyme disease characterized by arthritis or neuroborreliosis is very rare .
Other Diagnostic Tests For Lyme Disease
Some laboratories offer Lyme disease testing using urine or other body fluids. These tests are not approved by FDA because they have not been proven to be accurate. For example, one study of urine-based polymerase chain reaction assays for Lyme disease diagnosis showed that with currently available tools, urine cannot be used to accurately diagnose Lyme disease. Another study by NIAID-supported scientists showed that the Lyme Urinary Antigen Test was unreliable and resulted in excessive numbers of false positives. In the same study, researchers confirmed that an ELISA followed by a Western blot test was nearly 100 percent reliable in diagnosing Lyme disease. With the availability of so many Lyme disease tests, including non-commercial tests developed by individual facilities, it is impossible to address the accuracy of each one. The development of new, rapid, clearly validated diagnostic tests continues to be a need.
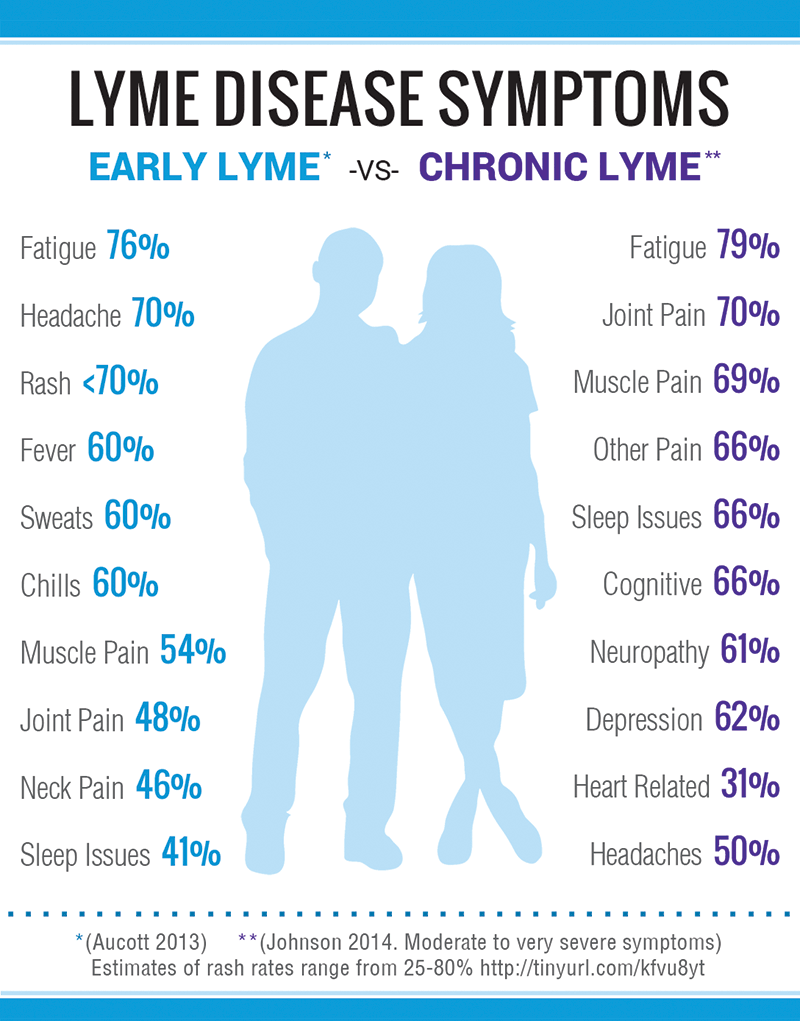
Symptoms Of Lyme Disease
People with Lyme disease may react to it differently, and the symptoms can vary in severity.
Although Lyme disease is commonly divided into three stages early localized, early disseminated, and late disseminated symptoms can overlap. Some people will also present in a later stage of disease without having symptoms of earlier disease.
These are some of the more common symptoms of Lyme disease:
- a flat, circular rash that looks like a red oval or bulls-eye anywhere on your body
- other flu-like symptoms
These symptoms may occur soon after the infection, or months or years later.
Your child may have Lyme disease and not have the bulls-eye rash. According to an early study, results showed roughly 89 percent of children had a rash.
Lyme disease is best treated in the early stages. Treatment for early localized disease is a simple 10- to 14-day course of oral antibiotics to eliminate the infection.
Medications used to treat Lyme disease include:
- doxycycline, amoxicillin, or cefuroxime, which are first-line treatments in adults and children
- cefuroxime and amoxicillin, which are used to treat women who are nursing or breastfeeding
Intravenous antibiotics are used for some forms of Lyme disease, including those with cardiac or central nervous system involvement.
After improvement and to finish the course of treatment, healthcare providers will typically switch to an oral regimen. The complete course of treatment usually takes 1428 days.
Read Also: Will Lyme Disease Go Away
Diagnosis Of Early Disseminated Lyme Disease
In order to diagnose Lyme disease, a doctor will order a blood test that checks for titers, which are the level of antibodies to the bacteria that cause the disease.
The enzyme-linked immunosorbent assay is the most common test for Lyme disease. The Western blot test, another antibody test, was once used to confirm the ELISA results. Current recommendations from the and the Food and Drug Administration state that a second ELISA test may be used to confirm Lyme disease.
The antibodies to B. burgdorferi can take anywhere from 4 to 6 weeks after infection to show up in your blood. As a result, people tested within the first few weeks of infection may test negative for Lyme disease. In this case, your doctor may choose to monitor your symptoms and test again at a later date to confirm the diagnosis.
If youre in an area where Lyme disease is common, your doctor may be able to diagnose Lyme disease in stage 1 based on their clinical experience and your symptoms.
If your doctor suspects you have early disseminated Lyme disease and the infection has spread throughout your body, they may recommend testing potentially affected areas. These tests may include:
Other antibiotics or intravenous medication may be necessary depending on your condition and additional symptoms.
You will likely have a rapid and complete recovery if you receive antibiotics in one of the early stages of Lyme disease.
Does The Time Of Year Matter In The Diagnosis Of Lyme Disease

Since Lyme disease is a tick-borne infection, the seasonality of the disease is linked tightly to the life cycle and behavior of ticks. May, June, July, and early August are the biggest risk months for acquiring first stage Lyme disease in the US. This is the feeding time for nymph and adolescent ticks which are difficult to see. A viral-like illness in those early summer months might be Lyme disease. There is also some transmission of Lyme disease via adult ticks in the fall and winter and throughout the year anytime the temperature is above 40 degrees, but to a lesser degree.
The risk of acute Lyme disease is more of a year-round risk in more temperate regions such as northern California and the pacific northwest. Later stage Lyme disease, however, can manifest at any time.
Also Check: The Best Lyme Disease Doctors
This Research Was Supported By
The Lyme Disease Research Foundation, the Johns Hopkins University Applied Physics Laboratory Research and Development Funds and the Johns Hopkins Institute for Assured Autonomy. We thank Dr. Elizabeth Horn from the Lyme Disease Biobank for the procurement of additional EM images and Cheryl Novak for assistance with annotation of images.
How Should Lyme Disease In Pregnancy Be Managed
While there have been reports of Lyme disease in pregnant women and sporadic case reports of transplacental transmission of B burgdorferi, there is not a clear link between fetal infections and adverse outcomes . Clinical, serological and epidemiological studies of Borrelia infection in pregnancy have failed to demonstrate an association between infection and adverse outcomes . Because doxycycline is contraindicated in pregnancy, treatment and prophylactic options are different than in the non-pregnant adult.
Some data suggest that a 10 day course of ampicillin may be an effective prophylactic strategy, although the risk of a rash developing in reaction to the beta lactam is greater than the risk of Lyme disease, and therefore the Infectious Diseases Society of America guideline does not recommend prophylaxis in the setting of pregnancy . If an Ixodes tick bites a pregnant woman, she should be monitored for 30 days for signs and symptoms of Lyme disease and treated with amoxicillin or cefuroxime if it develops .
Recommended Reading: Signs Of Lyme In Dogs
To Halt The Spread Of Lyme Nantucket Residents Consider Genetically Engineered Mice
Her ordeal is a common one every year, some 300,000 people in the United States are diagnosed with Lyme disease, according to the Centers for Disease Control and Prevention, and that number is on the rise. Some people wait months or years to get a correct Lyme diagnosis. And their cases highlight a problem: Tests for Lyme in the first month of infection are frequently wrong. When diagnosed and treated early the infection is a simple one to get rid of, but left untreated it can cause a myriad of lingering symptoms, from severe arthritis to short-term memory problems.
Now, a number of research groups are working to improve Lyme tests to catch infections in the early stages. One avenue being studied by the CDC aims to create a Lyme signature of small molecules in the blood an approach that, in early testing, catches a dramatically higher share of early infections.
What Are Mast Cells
Think of mast cells as universal alarm cells or guards. When mast cells detect infection, allergic triggers, injury, or toxins, they release specific chemicals which trigger an immune response.
These mediatorswhich include histamine, cytokines, prostaglandin, tryptase, nitric oxide, heparin and many otherscan cause a snowball effect that activates more mast cell reactions, triggering the release of more mediators.
Mast cells also express a substance called angiotensin converting enzyme 2 , now known as the primary cell through which SARS-CoV-2 enters the respiratory tract .
Also Check: East Lyme Homes For Sale
Why Was This Study Done
This study specifically focused on the longer-term outcome of Lyme disease patients and was rigorously designed to determine if persistent patient-reported symptoms following early diagnosis and prompt treatment for Borrelia burgdorferi infection are significant and distinguishable from those found in healthy non-Lyme controls.
High Endemicity Constitutional Symptoms No Erythema Migrans Rash
A patient from an area of high endemicity of Lyme disease presents with fever, headache, and arthralgias that had lasted several weeks, but no erythema migrans rash. After a thorough clinical evaluation, the cause of the symptoms remains unresolved.
The physician should consider serologic testing with the complete two-step approach. For this patient, the pretest probability is moderately low, taking into account the endemicity of the disease and the presence of prolonged , unexplained nonspecific symptoms. In this scenario, if the two-step approach is positive, the probability of Lyme disease is about 90 percent. Although testing probably is beneficial in this type of patient, this has not been proven. There is no clear evidence that treatment is beneficial in patients with Lyme disease who exhibit only nonspecific symptoms.
Read Also: Lyme Disease And Joint Pain
The Problem With Current Lyme Disease Diagnostics Is Clear
The biggest problem is that there is no way to test, unequivocally, for the presence of the bacteria that cause the disease.
There are no accurate diagnostic tests, no vaccines, and whatever treatment is provided is often inadequate.
May 29, 2019
Lyme disease is the most common tick-borne disease in the United States. Each year, approximately 30,000 cases of Lyme disease are reported in the country. However, the Centers for Disease Control and Prevention believes that the actual number of Americans who get Lyme disease each year may be closer to 300,000.
Early Warning: Lab Test Can Detect Acute Lyme Disease From A Single Cell
For those who live in an area blighted by ticks, the threat of Lyme disease can cast a shadow over the joy of spring and summer. These blood-sucking arachnids can transmit bacteria into the bloodstream of their unsuspecting host, causing the disease.
Early treatment is essential, but current tests are not usually sensitive enough to detect the disease in early-stage patients. A recent study in open-access journal Frontiers in Microbiology reveals a new test for Lyme disease, which is the first to reliably distinguish between early- and late-stage patients. The test detects a genetic sequence left by a virus that resides in Lyme-causing bacteria, and can detect just one bacterial cell in a small blood sample.
As the most common tick-borne infection, Lyme disease affects nearly 500,000 people in the U.S. every year. Symptoms include fever, fatigue, joint pain, and a distinctive bulls-eye rash, but if left untreated, the disease can cause paralysis and even death. As such, early diagnosis is important, but difficult.
Read Also: Dr Frank Noonan Lyme Disease
Stage : Early Localized Disease
Symptoms of Lyme disease usually start 1 to 2 weeks after the tick bite. One of the earliest signs of the disease is a bulls-eye rash.
The rash occurs at the site of the tick bite, usually, but not always, as a central red spot surrounded by a clear spot with an area of redness at the edge. It may be warm to the touch, but it isnt painful and doesnt itch. This rash will gradually fade in most people.
The formal name for this rash is erythema migrans. Erythema migrans is said to be characteristic of Lyme disease. However, many people dont have this symptom.
Some people have a rash thats solid red, while people with dark complexions may have a rash that resembles a bruise.
The rash can occur with or without systemic viral or flu-like symptoms.
Other symptoms commonly seen in this stage of Lyme disease include:
How To Prevent Lyme Disease From Progressing
Learn the symptoms of early Lyme disease so that you can seek treatment promptly if you contract the infection. If you get timely treatment, you can avoid the potential complications of early disseminated Lyme disease and later stages.
The symptoms of early Lyme disease can occur between 3 and 30 days after an infected tick bites you. Look for:
- rash, such as:
- a red, expanding bulls-eye rash at the site of the tick bite
- a round or oval rash that can be as wide as 6 to 8 inches
Read Also: Low Dose Naltrexone And Lyme Disease
Current Problems With Lyme Disease Diagnosis & Patient Care
- Diagnostic tests cannot yet accurately identify the earliest stage of Lyme disease when making the diagnosis is crucial.
- The rash is not always present or easily recognized
- Misdiagnosis and delayed diagnosis can make Lyme disease more difficult to treat and lead to prolonged and debilitating illness
- Early symptoms can be mistaken for a summer flu
- Lyme disease can involve several parts of the body, including joints, connective tissue, heart, brain, and nerves, and produce different symptoms at different times.
- Antibody testing done after early treatment may be negative and never turn positive for some cases
- Borrelia burgdorferi can evade our protective immune system and trigger immune system dysfunction.
- No reliable blood test is presently available to measure treatment success, necessitating close clinical follow up and improved physician education.
- Presently there is no vaccine to prevent Lyme disease available to humans.
Risk Factors For Early Disseminated Lyme Disease
Youre at risk for early disseminated Lyme disease if youve been bitten by an infected tick and remain untreated during stage 1 of Lyme disease.
Youre at an increased risk of contracting Lyme disease in the United States if you live in one of the areas where most Lyme disease infections are reported. They are:
- any of the Northeastern states from Maine to Virginia
- the north central states, with the highest incidence in Wisconsin and Minnesota
- parts of the West Coast, primarily northern California
Certain situations also can increase your risk of coming into contact with an infected tick, such as:
- gardening, hunting, hiking, or doing other outside activities in areas where Lyme disease is a potential threat
- walking or hiking in high grass or wooded areas
- having pets that may carry ticks into your home
You May Like: Lyme Vaccine For Dogs Side Effects
A Precise Medical History
Doctors in the Northeast and Northwestern US should ask about the persons hobbies and where they have been recently, such as hiking or camping. They should also ask whether there are pets in the house such as cats or dogs and whether they go out into wooded areas.
They should also be asked if they saw a tick attached to them, and whether or not they tried to remove it. If they tried to remove it, did they do so successfully, or might there still be tick mouth parts embedded in the skin?
If the person lives in an area where Lyme is common, or they have seen a tick, the doctor will likely not wait to start the patient on antibiotics. This is because the bacteria is a spirochete, which looks like a corkscrew or tiny snake. Because of its shape, it can insert itself into tissue and be very difficult to eradicate.
How To Avoid Contracting Lyme Disease
- Use insect repellant on your clothing and all exposed skin when walking in wooded or grassy areas where ticks thrive.
- Treat clothing and footwear with permethrin , an insect repellant that remains active through several washings.
- Walk in the center of trails to avoid high grass when hiking.
- After walking or hiking, change your clothes and perform a thorough check for ticks, focusing on the groin, scalp, and armpits.
- Check your pets for ticks.
Contact a doctor if a tick bites you. You should be observed for 30 days for signs of Lyme disease.
Also Check: My Dog Tested Positive For Lyme Disease
Symptoms Of Early Disseminated Lyme Disease
The onset of early disseminated Lyme disease can begin days, weeks, or months after a person is bitten by an infected tick. The symptoms reflect the fact that the infection has begun to spread from the site of the tick bite to other parts of the body.
At this stage, the infection causes specific symptoms that may be intermittent. They are:
- multiple erythema migrans lesions, which are circular or oval rashes that occur near the bite site and can be solid or resemble a bulls-eye
- Bells palsy, which is paralysis or weakness of muscles on one or both sides of the face
- meningitis, which is inflammation of the protective membranes around the brain and spinal cord
- neck stiffness, severe headaches, or fever
- severe muscle pain or numbness in the arms or legs
- pain or swelling in the knees, shoulders, elbows, and other large joints
Early Vs Later Diagnosis

Lyme disease has been diagnosed long enough, and the infectious bacteria that causes it is easy enough to identify, that most patients with early Lyme disease are able to find a healthcare provider who can accurately diagnose it. Even those patients who are originally told by a healthcare provider that their symptoms are all in their head are often able to find another practitioner to help them get the accurate diagnosis.
But in some cases, patients find great difficulty in getting a Lyme disease diagnosis. And that’s because there is a controversy that surrounds such a diagnosis for patients who don’t suffer symptoms until long after they were possibly bitten by a tick. While some people exhibit symptoms, including the classic “bull’s eye” rash, early after a tick bite, it’s possible that symptoms won’t show up for months or years after being infected.
Furthermore, some patients are treated early with antibiotics, but those antibiotics don’t completely destroy the Lyme Borrelia bacteria, or other symptoms occur even when no sign of any lingering infection remains.
“Chronic” Lyme Disease Diagnosis Controversy
Although no one denies that some people treated appropriately for Lyme disease go on to have persistent symptoms, there is a huge controversy over what it’s called, what causes it, and how it’s best treated. It has been called “chronic Lyme disease” the Centers for Disease Control and Prevention calls it post-treatment Lyme disease syndrome .
Recommended Reading: Lyme Disease Specialist In Delaware