What Do I Do If I Find A Tick On My Skin
Dont panic. Use fine-tipped tweezers to grasp the tick as close to the skins surface as possible. Pull up with steady, even pressure. Be careful not to squeeze or twist the tick body. Sometimes parts of the tick remain in the skin. You can leave them alone or carefully remove them the same way you would a splinter. Do not use heat , petroleum jelly, or other methods to try to make the tick back out on its own. These methods are not effective.
Wash the area where the tick was attached thoroughly with soap and water. Keep an eye on the area for a few weeks and note any changes. Call your doctor if you develop a rash around the area where the tick was attached. Be sure to tell your doctor that you were bitten by a tick and when it happened.
Who Gets Lyme Disease
Anyone bitten by an infected deer tick can get Lyme disease. Most U.S. cases of Lyme disease happen in Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. But Lyme disease is found in other parts of the U.S., Europe, Asia, and Australia too.
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
You May Like: Best Lyme Disease Doctors In Massachusetts
What Is The Treatment For Lyme Disease
The first-line standard of care treatment for adults with Lyme disease is doxycycline, a tetracycline antibiotic. Other antibiotics that have activity against borrelia include the penicillin-like antibiotic, amoxicillin, and the second generation cephalosporin, Ceftin. The mainstay of treatment is with oral antibiotics, but intravenous antibiotics are sometimes indicated for more difficult to treat cases of neurologic-Lyme disease, such as meningitis, and cases of late Lyme arthritis.
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Don’t Miss: At Home Lyme Disease Test
Risk Communication And Policy Implications
Risk communication represents the process of informing individual and collective decision-making by describing benefits as well as risks. As illustrated by the case of Lyme vaccine, the issues involved often become very complex and require an in-depth understanding to accurately access risk. However, the public attention span is typically short. The media often serve as the only channel through which the general public obtains its health information.
In the aftermath of the LYMErix market withdrawal, we must look for lessons learned. The vaccine developers believed they developed a safe and effective vaccine to prevent the most common tick-borne infection in the United States. Even available post-market surveillance failed to demonstrate convincing harm from the LYMErix vaccine. After review of available data, the FDA found insufficient evidence to support a causal relationship between the reported adverse effects and the vaccine and continued to permit use of the vaccine. However, the public’s perception of potential risks, heavily influenced by the negative press coverage and limited awareness of the benefits of the vaccine, decreased consumer demand for the vaccine.
Who Is At Risk For Lyme Disease
Anyone can get a tick bite. But people who spend lots of time outdoors in wooded, grassy areas are at a higher risk. This includes campers, hikers, and people who work in gardens and parks.
Most tick bites happen in the summer months when ticks are most active and people spend more time outdoors. But you can get bitten in the warmer months of early fall, or even late winter if temperatures are unusually high. And if there is a mild winter, ticks may come out earlier than usual.
Read Also: What Tick Has Lyme Disease
When To See A Doctor
If you have been bitten by a tick and start to display symptoms, especially if you think the tick has been on you for longer than 24 hours, you should consult with your doctor. The treatment will be far more effective if it is started earlier.
Even if your signs and symptoms disappear, the disease might still be present in your body. If left untreated the infection can spread to other parts of your body.
Questions To Ask Your Doctor
- I found a tick embedded in my skin, but I cant get it out. What should I do?
- Ive been bitten by a tick. Do I need to be seen?
- Do I need a blood test to confirm Lyme disease?
- Which antibiotic is best for me?
- How long will I have to take the antibiotic?
- What tick or insect repellent should I use for me or my child?
- How long will the symptoms last?
- What should I do if I still dont feel well a long time after I was bitten?
Don’t Miss: Can You Get A Test For Lyme Disease
Does Treatment Immediately After A Tick Bite Negate Signs Of Early Infection
Not every tick carries B. burgdorferi. The infection rate of ticks also varies with geographic region. Therefore, treatment should not be performed based on a tick bite alone. If the tick was found on the animal it can be sent in for B. burgdorferi PCR. PCR for Anaplasma can be performed simultaneously if requested. If the tick was infected, early treatment can be considered. However, a tick must feed for at least 24 hours on an animal or human for B. burgdorferi transmission to occur. Only a serological test will confirm whether transmission of B. burgdorferi occurred and the animal was infected. Antibodies can be detected in infected animals as early as 3-4 weeks after infection. Lyme Multiplex testing is recommended after that time. Treatment can be initiated immediately afterwards if antibody levels are positive. Treatment during this early infection phase is generally very effective.
Can Lyme Disease Be Prevented
To prevent Lyme disease, you should lower your risk of getting a tick bite:
- Avoid areas where ticks live, such as grassy, brushy, or wooded areas. If you are hiking, walk in the center of the trail to avoid brush and grass.
- Use an insect repellent with DEET
- Treat your clothing and gear with a repellant containing 0.5% permethrin
- Wear light-colored protective clothing, so you can easily see any ticks that get on you
- Wear a long-sleeve shirt and long pants. Also tuck your shirt into your pants and your pant legs into your socks.
- Check yourself, your children, and your pets daily for ticks. Carefully remove any ticks you find.
- Take a shower and wash and dry your clothes at high temperatures after being outdoors
Centers for Disease Control and Prevention
Recommended Reading: Best Rife Machine For Lyme
How Can Lyme Disease Be Prevented
Tick control and prevention methods significantly reduce the likelihood of infection. Maintaining antibodies against B. burgdorferi through vaccination can further protect your animal. Antibody amounts and duration of vaccine antibodies can vary in individuals. Verifying your animals antibody response to vaccination helps to assure durable protection.
What’s The Best Way To Prevent A Tick Bite
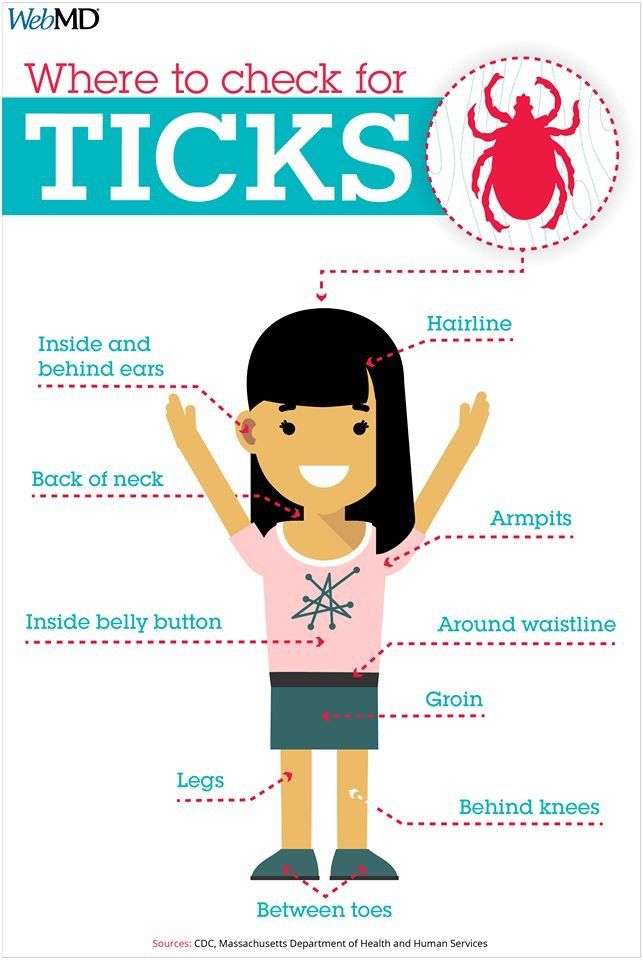
Ticks can’t fly or jump. But they live in shrubs and bushes and can grab onto you when you pass by. To avoid getting bitten:
- Wear pants and socks in areas with lots of trees and when you touch fallen leaves.
- Wear a tick repellent on your skin and clothing that has DEET, lemon oil, or eucalyptus.
- For even more protection, use the chemical permethrin on clothing and camping gear.
- Shower within 2 hours after coming inside. Look for ticks on your skin, and wash ticks out of your hair.
- Put your clothing and any exposed gear into a hot dryer to kill whatever pests might be on them.
How do you know if you’ve been bitten?
Since ticks are so small, you’ve got to have pretty good eyes to see them.
If you have a small, red bump on your skin that looks like a mosquito bite, it could be a tick bite. If it goes away in a few days, itâs not a problem. Remember, a tick bite doesnât necessarily mean you have Lyme disease.
If you notice a rash in the shape of a bull’s-eye, you might have a tick bite. Talk to your doctor about treatment.
If you have an allergic reaction to ticks, you’ll notice a bite right away.
You May Like: How To Cure Lyme Disease Naturally
Key Points To Remember
- Most Lyme disease tests are designed to detect antibodies made by the body in response to infection.
- Antibodies can take several weeks to develop, so patients may test negative if infected only recently.
- Antibodies normally persist in the blood for months or even years after the infection is gone therefore, the test cannot be used to determine cure.
- Infection with other diseases, including some tickborne diseases, or some viral, bacterial, or autoimmune diseases, can result in false positive test results.
- Some tests give results for two types of antibody, IgM and IgG. Positive IgM results should be disregarded if the patient has been ill for more than 30 days.
What Do You Do If There’s A Tick Under Your Skin
Use a pair of fine-tipped tweezers to remove it as soon as possible. Pull upward with steady pressure. If parts of the tick are still in your skin, try to get those with the tweezers, too. After everything is out, clean the bite area with rubbing alcohol or soap and water.
You probably wonât get infected if you remove the tick within 36 to 48 hours.
How do you throw away a tick?
Put it in soapy water or alcohol, stick it to a piece of tape, or flush it down the toilet.
Recommended Reading: My Dog Tested Positive For Lyme
Stage : Early Localised Lyme Disease
The symptoms for this stage normally begin within a few days to weeks after infection from the tick bite. In some cases of Lyme disease, you may not notice signs of infection during this stage.
The bacteria begin to multiply in the bloodstream, with the first sign being that of a red, circular rash. It might look a lot like a bulls eye.
This rash will develop at the site of the tick bite. It is not painful or itchy, just warm to touch. It is known as erythema migrans and will most likely disappear within four weeks.
With or without the rash, you may develop flu-like symptoms. These can include:
- A loss of energy
- Vision changes
For Animals That Have Not Been Vaccinated Can Osp A Values Be Positive How Should This Be Interpreted
Antibodies to OspA have previously been interpreted as markers for vaccination. Non-vaccinated animals usually have low values for antibodies to OspA, while vaccinated animals develop these antibodies. OspA antibodies have been shown to protect from infection with B. burgdorferi.
However, there is accumulating evidence that antibodies to OspA can occur without vaccination. First, residual OspA is present on the bacterial surface at the time of transmission to an animal. This causes a low and transient OspA antibody response early after infection. Second, antibodies to OspA have also been associated with treatment-resistant Lyme arthritis and with development of autoimmunity in human patients. Similarly, OspA antibodies in non-vaccinated dogs or horses can be considered as markers of chronicity and disease severity.
Recommended Reading: What Type Of Doctor Treats Lyme Disease
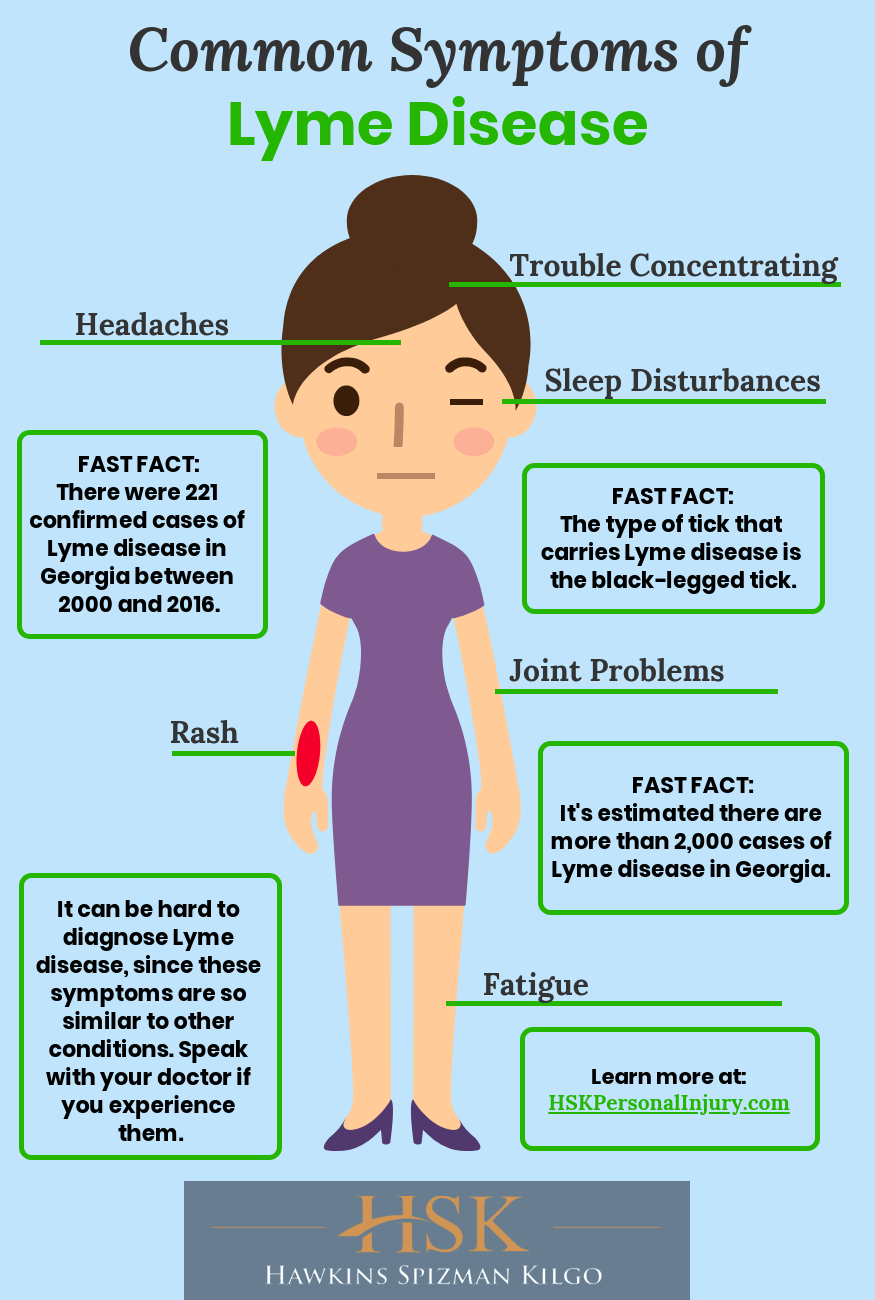
Signs And Symptoms Of Lyme Disease
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
Overview
Lyme disease is an underreported, under-researched, and often debilitating disease transmitted by spirochete bacteria. The spiral-shaped bacteria, Borrelia burgdorferi, are transmitted by blacklegged deer ticks. Lymes wide range of symptoms mimic those of many other ailments, making it difficult to diagnose .
The blacklegged ticks can also transmit other disease-causing bacteria, viruses, and parasites. These are known as coinfections . These ticks that transmit Lyme are increasing their geographical spread. As of 2016, they were found in about half the counties in 43 of 50 states in the United States .
Lyme is the fifth most reported of notifiable diseases in the United States, with an estimated 329,000 new cases found annually . Some studies estimate that there are as many as 1 million cases of Lyme in the United States every year .
Most people with Lyme who are treated right away with three weeks of antibiotics have a good prognosis.
But if youre not treated for weeks, months, or even years after infection, Lyme becomes more difficult to treat. Within days of the bite, the bacteria can move to your central nervous system, muscles and joints, eyes, and heart .
Here is a list of 13 common signs and symptoms of Lyme disease.
Which Antibodies Does The Vaccine From Merial Induce
It is a recombinant vaccine based on Osp A. Vaccinated animals should develop high antibody levels to OspA and maintain negative antibody levels to the remaining two antigens. Infected/non-infected animals can be identified based on OspC and OspF antibody values. Detection of the early Lyme infection stage is possible after using this vaccine.
Also Check: What Can I Give My Dog For Lyme Disease
What If A Tick Bites My Dog
The more ticks in your region, the likelier it is that your furry pal will bring them home.
Your dog is much more likely to be bitten by a tick than you are. And where Lyme disease is common, up to 25% of dogs have had it at some point.
About 10% of dogs with Lyme disease will get sick. 7-21 days after a tick bite, your dog might seem like theyâre walking on eggshells. They also might have a fever and enlarged lymph nodes. Plus, they might seem tired. Dogs also get antibiotics for Lyme.
What if my dog brings ticks into my home?
Use a tick control product on your pet to prevent Lyme disease. Also, have your dog vaccinated against Lyme.
Check your dogâs whole body each day for bumps. If you notice a swollen area, see if thereâs a tick there. If you find a tick, wear gloves while you use tweezers to separate it from your dog. Then, put it in soapy water or alcohol, or flush it down the toilet.
Use alcohol to clean the spot on your dog where the tick was attached. Keep an eye on that spot, and also on your dog to make sure theyâre behaving normally. If you notice any changes, check with your vet.
Show Sources
John Aucott, MD, assistant professor of medicine, Johns Hopkins University School of Medicine director, Johns Hopkins Lyme Disease Clinical Research Center.
CDC.
Morbidity and Mortality Weekly Report: âVital Signs: Trends in Reported Vectorborne Disease Cases — United States and Territories, 2004-2016.â
American College of Rheumatology.
Lyme Disease: Symptoms & Side Effects
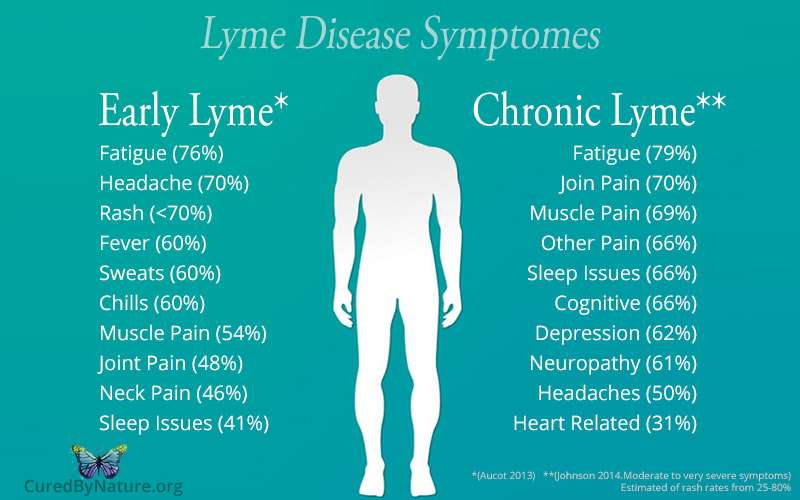
Lyme disease is a tick-born illness with over 150 symptoms, usually involving multiple systems. There are three stages of Lyme disease: early localized, early disseminated, and late persistent. If left untreated, it may progress into long-term disabilities. However, it is important to note that Lyme disease can lie dormant in your body for a prolonged period of time, and will invade when your immune system is compromised.
- Irritable bladder
- Upset stomach
- Pain in eyes, or swelling around eyes
- Oversensitivity to light
- Buzzing in ears
- Pain in ears, oversensitivity to sound
- Ringing in one or both ears
- Unexplained weight gain or loss
- Extreme fatigue
- Unexplained fevers
- Continual infections
- Symptoms seem to change, come and go
- Pain migrates to different body parts
- Early on, experienced a flu-like illness, after which you have not since felt well
- Twitching of facial or other muscles
- Facial paralysis
- Tingling of nose, cheek, or face
- Stiff or painful neck, creaks and cracks
- Jaw pain or stiffness
- Memory loss
- Confusion, difficulty in thinking
- Difficulty with concentration or reading
- Going to the wrong place
- Speech difficulty
- Stammering speech
- Any joint pain or swelling
- Stiffness of joints, back, neck
- Muscle pain or cramps
- Burning or stabbing sensations in the body
- Weakness or partial paralysis
- Numbness in body, tingling, pinpricks
- Poor balance, dizziness, difficulty walking
- Increased motion sickness
Read Also: What Are The Lasting Effects Of Lyme Disease
Babesia And Lyme Its Worse Than You Think
Babesia, a tick-borne infection that causes malaria-like symptoms, has been making headlines over the past two years as the number of reported cases increases, and concerns grow over the seriousness of the disease and its ability to be transmitted through the blood supply.
Although Lyme disease is the most talked about tick-transmitted disease, Babesia is more common than you might think. In the 2015 issue of Trends in Parasitology, Diuk-Wasser and colleagues report that up to 40% of patients with Lyme disease experienced concurrent Babesiosis.
This means that out of the estimated 300,000 cases of Lyme disease reported annually in the U.S., 120,000 of those individuals may also have Babesia. This is particularly alarming given that the disease can go undetected in asymptomatic individuals and is transmissible through blood transfusions or congenitally. Additionally, Babesia requires different treatment than Lyme disease.
The Babesia microti parasite that leads to Babesia is commonly seen in blacklegged deer ticks. But according to the authors, its also common to find ticks and enzootic hosts carrying both Borrelia burgdorferi and B. microti. In fact, between 12% and 42% of rodents are co-infected with both agents. This would suggest that coinfection provides a survival advantage for both pathogens.
Babesia difficult to diagnose
Treating Babesia