How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Stage : Early Disseminated Lyme Disease
Timing: Weeks to months after a tick bite
In early disseminated Lyme disease, the infection has started to move beyond the site of your tick bite to other parts of your body such as your heart, brain, or spinal cord. Lyme disease that has moved to the brain is sometimes referred to as Lyme neuroborreliosis, or neurological Lyme disease.
Common symptoms of early disseminated Lyme disease include:
-
More than one EM rash
-
Pain that may come and go and move around the body, in joints, tendons, muscles, and bones
-
Inflammation of the brain and spinal cord , which can cause severe headache, neck stiffness, and sensitivity to light and sound
-
Numbness, weakness, or tingling in the arms and legs
-
Weakness or drooping on one or both sides of the face difficulty closing an eyelid
-
Inflammation of the heart that can cause heart palpitations, irregular heartbeat, dizziness, shortness of breath, or fainting. If you are experiencing any of these heart symptoms, seek immediate medical care.
You may also experience a worsening of earlier Lyme disease symptoms.
Lyme disease can cause joint pain , a stiff neck , or weakness or drooping on one or both sides of the face, known as facial palsy .
Recommended Reading: Lyme Disease And Urinary Problems
How A Pathogen May Be Helping Ticks
Couret and her research partners hypothesize that the Lyme bacteria and blacklegged ticks maintain a mutually beneficial relationship. The idea is that if ticks with the pathogen are stronger or more resilient, then the chances of the bacteria spreading go up.
In pilot studies, Couret has seen changes in ticks after they pick up the bacteria, ranging from the behavioral to the metabolic.
So how could the bacteria be helping ticks? Its still early in the study, which started in September, and hard to say, but one promising avenue may lie in the ticks tolerance of drought conditions.
Ticks are generally sensitive to heat, spending time in the leaf litter when its hot and dry. But one characteristic of ticks in the Northeast, versus those in the South, appears to be a tendency to climb higher in the vegetation, up on to plant stalks or branches even as the temperature rises. From these elevated vantage points, its easier for them to latch on to a passing deer or person.
If somehow the Lyme bacteria is influencing this behavior, it may offer an advantage to the ticks in finding their meals.
Of course, there are other organisms that make up the ticks microbiome, so isolating the specific interactions with the Lyme bacteria will be difficult. But the researchers are taking a comprehensive view, hoping to look at the many ecological relationships that affect the tick life cycle and tease out some answers.
Recommended Reading: Does Lyme Disease Cause Kidney Failure
How To Remove A Tick
Ticks have 24 hours to sink in their evil magic. According to the CDC, to remove a tick you simply take a pair of fine-tipped tweezers, like these, grasp the tick as close to the surface of the skin as possible and pull upward. Flush the tick down the toilet as soon as possible. Do NOT crush it with your fingers. Wash the skin area with rubbing alcohol, iodine scrub or soap and water. Monitor your childs health for a rash or fever over the next few weeks.
Call Ahead And Ask Questions
Even if you find a doctor who specializes in treating tick-borne diseases, you will want to ask some questions before making an appointment and committing your time and money. A few basic questions to consider asking upfront include the following:
- What is your experience in treating patients with tick-borne diseases?
- How do you diagnose diseases? Do you use any specific labs or lab tests to confirm diagnosis?
- Do you test for coinfections?
- Do you use traditional antibiotics and/or herbals?
- Do you have any patient success stories you can share?
- Do you strictly adhere to CDC test interpretation criteria or are you open to alternative criteria?
If youd like to find a LLMD and want to know more about how to vet them, read the Tick Talk blog, What Makes a Doctor Lyme Literate?
Don’t Miss: Medicine For Lyme Disease In Dogs
What Are The Symptoms Of Lyme Disease
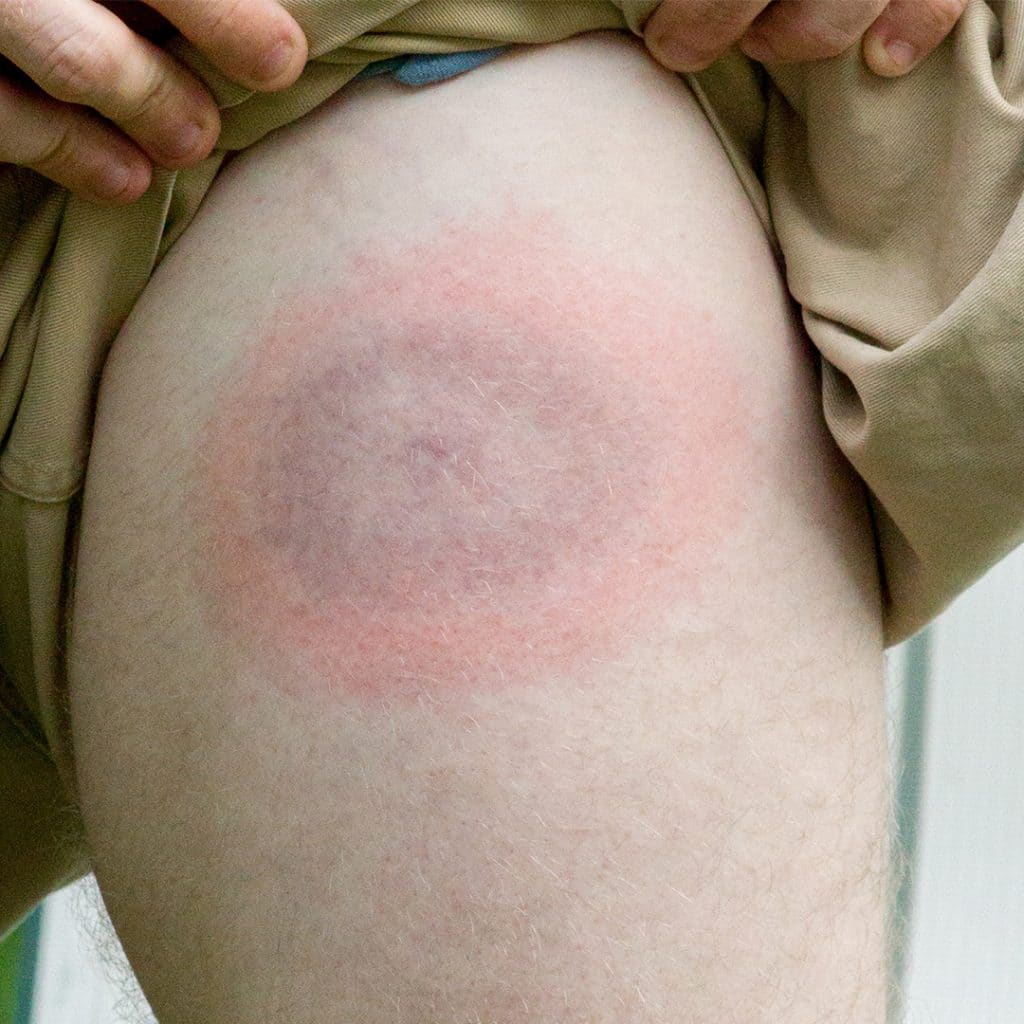
Symptoms of Lyme disease have a wide range and depend on how far the disease progresses. Symptoms can occur anywhere from three to thirty days post infected tick bite. Early symptoms of Lyme disease include a rash that develops on the area surrounding a tick bite. This rash can spread over the course of a few days and may have a noticeable bullseye pattern in its center. In some cases, a rash never develops. Not all tick bites carry infection.
Early signs of Lyme disease include:
If left untreated, Lyme disease can progress to more serious complications. Later stage symptoms include:
- Severe headache and neck stiffness
- Arthritis with severe joint pain and swelling
- Inflammation of the brain or spinal cord
- Heart-related complications
If you think youre experiencing some of the symptoms of Lyme disease, schedule a consultation at Advanced Infectious Disease Medical.
Read Also: Common Treatment For Lyme Disease
Check For Ticks After Being Outside
Anyone who comes in contact with a deer tick can be at risk of a bite. Ticks cannot fly or jump. They wait for a possible host to brush against them and then use their legs to attach themselves. There are steps you can take to reduce the number of ticks in your yard:
-
Clear tall grass and brush
-
Mow the lawn frequently and rake leaves
-
Keep wood stacked in dry areas
-
Create a barrier of woodchips or gravel around recreational areas
-
Treat pets with anti-tick medication
Reducing your time in areas known for ticks is the best way to avoid bites and Lyme disease. Always check yourself after spending time outside.
You May Like: Lyme Disease Ab Quant Igm
Why You Might Need To See A Llmd:
- Your Lyme disease test results were negative, but you still have symptoms of Lyme disease.
- Youve been treated for Lyme disease in the past but still have symptoms, which could indicate chronic Lyme disease.
- Youve been treated or are being treated for common misdiagnoses of Lyme disease, such as Rheumatoid Arthritis or Chronic Fatigue Syndrome, but your symptoms havent gone away.
- Your physician doesnt believe in Lyme disease, chronic Lyme disease, or Post-Treatment Lyme Disease Syndrome.
Even patients who dont fall into the above categories may simply feel safer in the hands of a LLMD who is familiar with the various ways Lyme and other tick-borne diseases present themselves.
How Is Lyme Disease Diagnosed
An EM rash is a sure sign of Lyme disease, so your doctor can diagnose and treat you without the need for laboratory tests.
An EM rash, often shaped like a bullseye , is a sure sign of Lyme disease. If you develop an EM rash, you should be diagnosed & treated for Lyme disease without the need for further lab tests. EM rashes are not as obvious on darker skin .
For all other cases, your doctor should consider whether your symptoms and risk factors point to a Lyme disease diagnosis. For example:
-
Were you bitten by a tick?
-
Did you spend time outdoors in an area where Lyme disease is common?
-
Recent travel: Lyme disease may be common where you were, even if it is unusual where you live.
-
Your current symptoms and how long have they been present.
-
Your full medical history, including previous unexplained symptoms that may help lead to an accurate diagnosis whether that ends up being Lyme or another condition.
Don’t Miss: What Medicine Is Used To Treat Lyme Disease
How Will My Doctor Test Me For Lyme Disease
The CDC recommends two-step testing, sometimes referred to as a two-tiered test, for Lyme disease. You will need to go to a lab to have blood drawn. It takes a few days to get results.
If the first test comes back positive or unclear, the lab will do the second blood test. If the first test comes back negative, the CDC does not recommend the second test. However, according to the CDC the second test must be positive for you to be diagnosed with Lyme disease.
The first test: ELISA
This blood test is for antibodies against the Lyme disease bacteria. Because it can take some time for your body to produce antibodies, this test isnt always accurate soon after a person is infected.
The second test: Western Blot or a second ELISA
There are two options for the second test. One is called a Western blot, which looks at how your antibodies react to specific parts of the Lyme disease bacteria. The Western blot test has been part of the two-step testing system since 1994 and is more commonly used.
The other option is to do a second ELISA test, which measures antibodies to a specific protein found on Lyme disease bacteria. Because these tests are newer, not all doctors have experience with them and not all labs have access to them.
These tests can be run on the blood sample used for the first test. You should not need to go back to the lab.
A possible drawback of the two-step testing system
Which second test is best: ELISA or Western blot?
Are Llmds Infectious Disease Specialists
No. While it is possible for a LLMD to be an infectious disease specialist, LLMDs can come from any field or background. Many LLMDs are general practitioners or family doctors, while others may specialize in a specific type of medicine, such as naturopathic medicine.
For more information on finding a LLMD, read IGeneXs blog How to Find Doctors Who Can Help with Your Tick-Borne Disease.
Read Also: What Are The Side Effects Of Lyme Disease In Humans
What Is On The Horizon For Lyme Testing
Because Lyme bacteria are not usually present in high enough numbers to be detectable, blood tests to look for Borrelia are not helpful.
Better diagnostic tests are needed that are direct and can detect infection at all stages of Lyme disease. Researchers are studying new diagnostic methods using better antibody tests, direct detection methods, and different ways to measure immune response to Lyme disease.
Myth: Lyme Disease Doesnt Cause Chronic Illness

The biggest Lyme disease controversy centers on post-treatment Lyme disease syndrome , a chronic illness often called âChronic Lyme Diseaseâ . A paper published in the Journal of Pharmacy and Pharmaceutical Sciences states that 10-20% of patients who get infected with Lyme disease will have long-term symptoms after initial treatment. However, the difficulties with diagnosing and treating Lyme disease have led to a deep divide within the medical community. Some believe that the lingering symptoms are caused by an active, persistent Lyme disease infection. Others believe that they are the manifestation of a post-infection autoimmune condition. Still others believe that the symptoms are unrelated to Lyme disease and that PTLDS/CLD doesnât exist at all. The Centers for Disease Control and Prevention recognizes PTLDS as a chronic illness, but acknowledges that a lot doctors, scientists, and researchers donât know about it.
Regardless of the medical communityâs views on PTLDS/CLD, thousands of people in the United States are struggling with the chronic illness, per a study published in BioMed Central Public Health. And it has a major impact on their well-being. One study found that people diagnosed with PTLDS experience a poorer quality of life and greater symptom severity than people with other chronic illnesses.
Read Also: Where To Go To Get Tested For Lyme Disease
You May Like: Dr David Jernigan Lyme Disease
What Are Symptoms Of Chronic Lyme Disease In Dogs
Symptoms of ChronicLymeDisease in Dogs. The symptoms of Lymedisease occur some time after the tick bite, usually 2 to 5 months. Most common symptoms are: Fever. Sudden lameness the lameness episodes can last 3 to 4 days and then disappear for weeks. Swelling of the joints. Swollen lymph nodes. Myositis
You May Like: Lyme Disease And Peripheral Neuropathy
When To Go To The Doctor For An Infected Bug Bite Or Sting
You may be able to treat minor infections at home with over-the-counter antibiotic ointments. But in many cases, youll need to go to the doctor for an infected bug bite or sting. You should see a doctor if:
- you have signs of a systemic infection, such as chills or a fever, especially if the fever is above 100°F
- your child has any signs of an infected bug bite
- you have signs of lymphangitis, such as red streaks extending from the bite
- you develop sores or abscesses on or around the bite
- the pain on or around the bite gets worse over a few days after youve been bitten
- the infection doesnt get better after using an antibiotic ointment for 48 hours
- redness spreads from the bite and gets bigger after 48 hours
In the beginning of an infection, you may be able to treat it at home. But if the infection gets worse, you may need medical treatment. Call a doctor if youre not sure.
Also Check: How To Rule Out Lyme Disease
The Different Types Of Doctors Who Can Test For Lyme Disease
Lyme disease is a tick-borne infectious disease caused by a group of spiral-shaped bacteria we now refer to as Lyme borreliae. This includes, but is not limited to, Borrelia burgdorferi. It is treatable with antibiotics, but in order to have the best chance at full recovery, its crucial to get your disease diagnosed and treated as soon as possible. That means finding the right doctor.
But what kind of doctor tests for Lyme disease? You may be wondering if you need to see a specific kind of physician to get the right test and treatment. The answer can depend on your particular situation.
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040 rel=nofollow> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Also Check: Can You Donate Blood With Lyme Disease
What Does The Future Hold
But how long can a lone septuagenarian keep his finger in the dike? Can he do moreaffect true changeby transmitting his knowledge to the world?
Jones decades of clinical experience have never been committed to writing or taught outside his small circle. And while he has the monopoly on a burgeoning marketLyme disease in the U.S. is at an all-time highhe cannot find a young physician to work by his side full-time and commit to assuming his practice when hes gone. With his colleagues under investigation, their careers in peril, an heir may be hard to find.
One ray of hope comes from the newly established Charles Ray Jones Endowed Student Fellowship at Columbia University, which allows him to train one medical intern in his practice each summer.
In 2001, it was Megan Peimer, a second-year medical student at Columbia College of Physicians and Surgeons, who worked alongside Dr. Jones. Peimer, who also spent her time absorbing the peer-reviewed literature on Lyme disease and writing up Jones classic cases, says her hope is to foster a more rational attitude about tick-borne disease.
Will Peimer specialize in Lyme disease? Im devoted to international medicine, she says, but when a child with Lyme disease comes to my practice, thanks to Dr. Jones, I will know how to recognize it, and I will know how to treat.
Also Check: How To Know If I Have Lyme Disease
In General Tick Borne Disease Or Lyme Disease Should Be Treated With Antibiotics Usually These Antibiotics Should Be Pharmaceuticals Although Augmentation With Botanical Antibiotics Can Be Even More Effective Than Pharmaceutical Therapies Alone
Unfortunately in late Lyme, antibiotics alone are often not sufficient. Some patients are genetically or epigenetically predisposed to chronic Lyme disease. Often the underlying conditions must be addressed along with the infection.
Borrelia burgdorferi has been called the second great pretender, after syphilis. Like syphilis it is a spirochete , and the spirochete goes to the brain and spinal cord as fast as it can get there. In addition like syphilis it grows very slowly. Unlike syphilis it is relatively smart in the bacterial world, having the largest genome of any other bacteria. Borrelia burgdorferi is able to crawl inside of cells, thus avoiding immune detection, hide in the brain and spinal cord, where our immune system is careful not to cause too much inflammation. More recent data suggests it may, like many of its co infecting microbes be able to fool the immune system and manipulate the immune response so that the immune system thinks that there is not an infection. In 3 animal models dog, mouse and monkey, chronic persistent infectious borrelia infection has been proven after short course antibiotic. This provides evidence that the cure of chronic Lyme disease in many patients will take more than 1-3 months of antibiotics.
Read Also: How Do You Treat Lyme Disease In Dogs
Also Check: Intravenous Treatment For Lyme Disease