Current Challenges And Future Priorities
Patients with PTLD represent a substantial burden to the United States health care system. In a large, health insurance claims analysis of 47 million members, estimated total direct medical costs from Lyme disease were between $712 million and $1.3 billion per year, with a significant portion of these specifically due to PTLD-related costs . The same study found that the adjusted odds of any PTLD-related symptom diagnosis following Lyme disease was 4.77 higher than age-, sex-, enrollment year-, region- and payer type-matched controls without Lyme disease, and that those patients with Lyme disease who went on to have at least one PTLD symptom had over twice the average total health care costs as those who did not . These cost estimates do not reflect additional indirect, non-medical, and lost productivity costs to patients, which may be substantial in a population with a chronic and significant illness impact on quality of life . Novel preventative approaches to reduce incidence of new Lyme disease cases, as well as physician and community educational interventions to increase awareness and reduce diagnostic delays and misdiagnosis, are needed to reduce costs and improve patient outcomes.
Fragments From Lyme Bacteria Persist In Joints Even After The Bacteria Are Killed Off
A new study published in Proceedings of the National Academy of Sciences sheds light on this medical mystery. To keep from spilling open, bacteria have rigid cell walls made of a matrix of protein and sugars, called peptidoglycan. Most bacteria recycle their peptidoglycan when they grow and divide, but the peptidoglycan of B. burgdorferi has a peculiar structure, and the bacteria is unable to reuse it. Instead, it dumps it into its immediate surroundings, like a microbial litterbug.
This peptidoglycan collects in the joints where B. burgdorferi is found. Almost all patients in the PNAS study with Lyme arthritis had peptidoglycan in their joint fluid. Most of them also had specific antibodies to peptidoglycan in the joint fluid, suggesting that the peptidoglycan was driving the inflammatory process. These antibodies were not found in fluid from people with other joint conditions, such as rheumatoid arthritis, osteoarthritis, or gout.
Patients with Lyme arthritis who did not get better with antibiotics still had peptidoglycan in their joint fluid. However, their joint fluid did not contain detectable B. burgdorferi DNA. This suggests that even after the bacteria were killed off, the peptidoglycan stayed behind, and stimulated further inflammation. This may explain why people with Lyme arthritis who do not respond to antibiotics may improve with medications that damp down the immune system, such as methotrexate or TNF inhibitors.
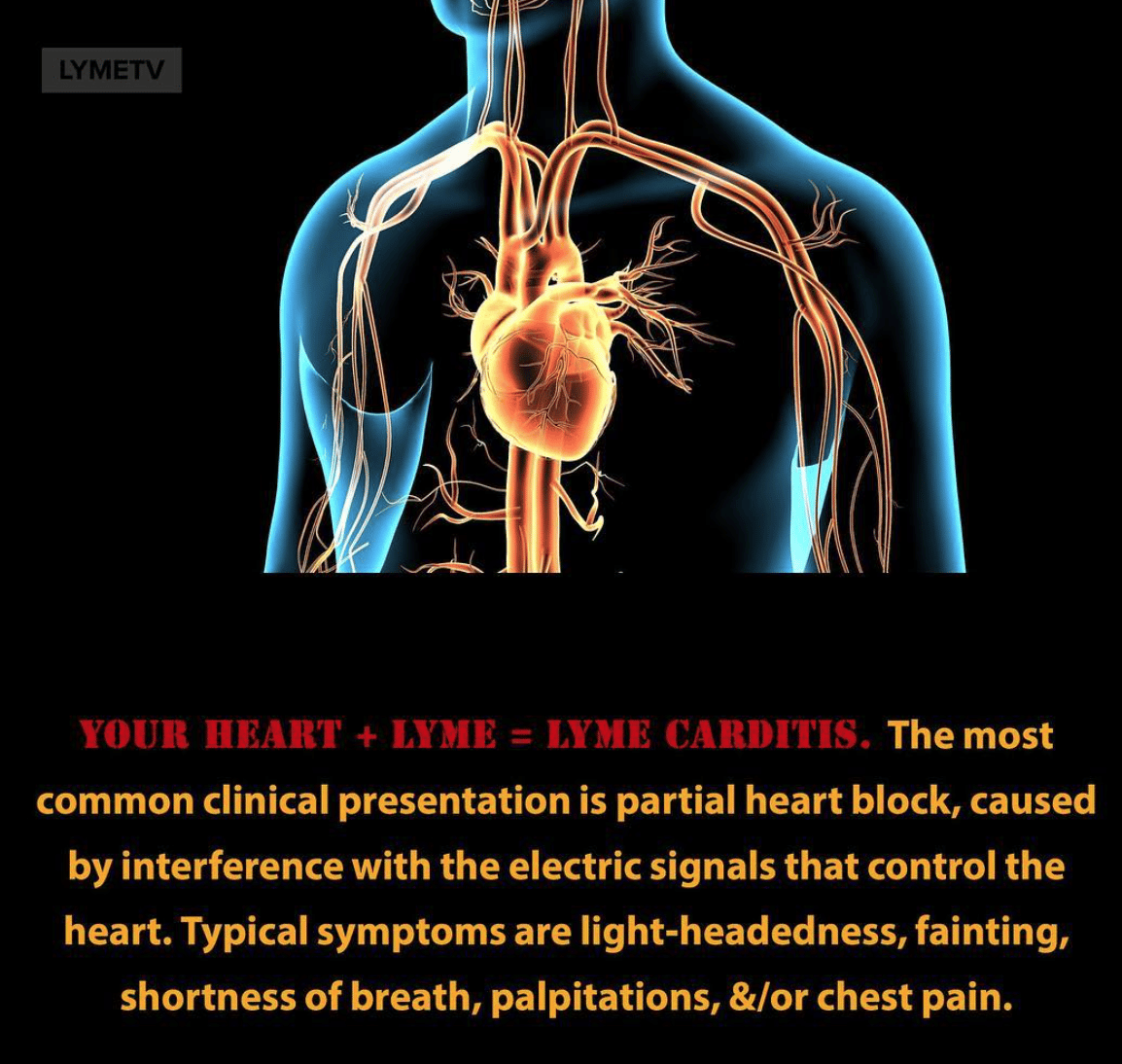
What Is Lyme Carditis
Lyme carditis occurs when Lyme disease bacteria enter the tissues of the heart. This can interfere with the normal movement of electrical signals from the hearts upper to lower chambers, a process that coordinates the beating of the heart. The result is something physicians call heart block, which can vary in degree and change rapidly. Lyme carditis occurs in approximately one out of every hundred Lyme disease cases reported to CDC.
You May Like: Medical Treatment For Lyme Disease
Lyme Disease Joint Pain And Arthritis
Lyme disease and joint pain unfortunately go hand in hand, as Lyme-related arthritis is commonly found in Lyme disease sufferers. If you have Lyme arthritis, you have swollen, painful and aching joints that cause stiffness and pain. It is found in people who are in the late stages of Lyme disease. According to an article in Science Daily, approximately 60 percent of patients with untreated Lyme disease will develop related arthritis.
Lyme arthritis is caused by the bacteria that causes Lyme disease getting into your joints and causing inflammation of your tissues. Over time, this can cause damage to your cartilage. Most cases of Lyme arthritis are short-lasting and affect only one large joint.
Lyme arthritis can affect your:
In the U.S., its estimated that about 60 percent of untreated Lyme disease patients will experience intermittent episodes of swelling and lyme disease joint pain for months to years after they are infected by a tick bite.
Thankfully, most Lyme arthritis cases can be treated with antibiotics and NSAIDs, although some people may require surgery to remove some diseased tissue. Around ten percent of untreated patients may go on to develop chronic arthritis, reports Johns Hopkins Arthritis Center.
Cause #: Untreated Infections
Lyme disease and Lyme coinfections like babesia, bartonella, and mycoplasmacontribute to metabolic and immune changes in the body because the microbes can be low-grade and persist for long periods of time. While no system of the body is off-limits, the central nervous system and the endocrine system are particularly vulnerable.
When pathogens invade the nervous system, white blood cells immune cells like lymphocytes and plasmocytes flood into the white matter of the brain and the spinal cord, says Dr. Bill Rawls, Medical Director of RawlsMD and Vital Plan. This causes a cascade of inflammatory immune messengers, called cytokines, in cerebrospinal fluid.
This influx of proinflammatory cytokines causes neuroinflammation in the brain, which can contribute to a range of neurological symptoms, including those associated with Lyme brain. Because most Lyme patients have a compromised immune system, the body struggles to keep the offending pathogens in check.
The outcome? You continue to experience a prolonged inflammatory response and resulting symptoms until youre able to suppress the harmful, stealth infections.
Recommended Reading: How Much Does Igenex Lyme Test Cost
Later Symptoms And Signs Of Lyme Disease
If you dont seek treatment, other symptoms and signs of infection may appear over the following weeks and months, including:
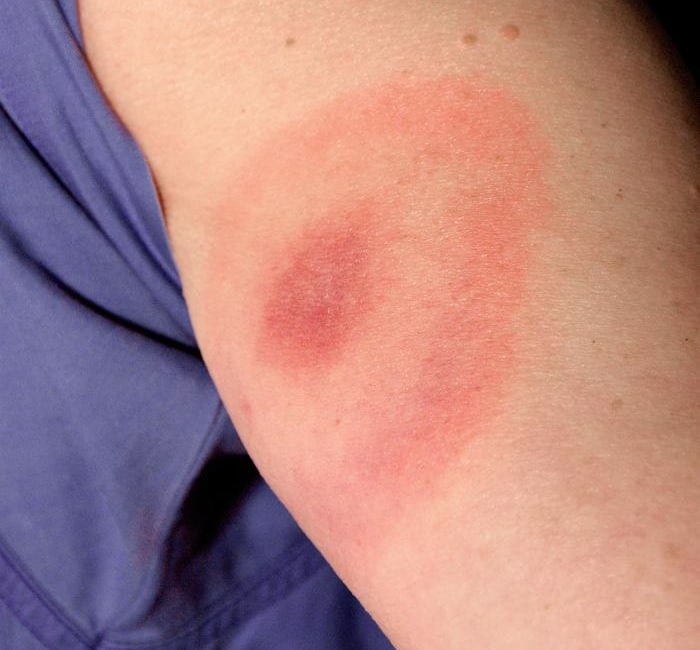
- The bulls eye rash. It is also called erythema migrans, and it may appear on other areas of your body.
- Neurological problems. At any time after the initial Lyme disease infection, even years later, you could develop meningitis, Bells palsy , weakness or numbness in your limbs and impaired muscle movement.
You may also suffer from:
Many weeks after infection, some people develop:
Swap The Sad Diet For Anti
When it comes to managing inflammation, diet is the perfect place to start. The foods you choose to eat can either help or hinder your recovery from Lyme disease by impacting your bodys inflammatory burden. The Standard American Diet, rich in refined carbohydrates and industrial seed oils, increases the expression of pro-inflammatory cytokines, immune molecules that trigger an inflammatory response. Many of the same pro-inflammatory cytokines triggered by the SAD diet are also triggered by Lyme disease and other tick borne infections.1 The SAD diet is also associated with an impaired immune response, which is the last thing you want when youre battling an infection.2 Other food groups, such as gluten and dairy, can also trigger inflammation and are best avoided by people with Lyme disease.
Conversely, eating an anti-inflammatory, nutrient-dense diet can accelerate your recovery process and create a foundation for long-term health. At CCFM, we recommend that most patients begin a Paleo Reset Diet. This diet is designed to reduce inflammation and improve digestion, energy, blood sugar control, and body weight. The Paleo Reset Diet is centered around the following foods:
- Non-starchy vegetables ideally 6-8 cups of vegetables across the color spectrum
- Gluten free diet
- Elimination and reintroduction diet
Incorporate Anti-Inflammatory Foods
Also Check: Do Antibiotics Cure Lyme Disease
Chronic Lyme Arthritis: A Mystery Solved
- By John Ross, MD, FIDSA, Contributor
In 1975, researchers from Yale investigated an epidemic of 51 patients with arthritis who lived near the woodsy town of Lyme, Connecticut. The most common symptom was recurrent attacks of knee swelling. A few had pain in other joints, such as the wrist or ankle. Many had fever, fatigue, and headache. Some remembered a round skin rash before the onset of knee swelling.
We now know that Lyme disease is an infection acquired from tick bites, caused by a spiral bacterium named Borrelia burgdorferi. After a tick bite, Borrelia bacteria wriggle through the skin away from the bite site. This leads to a circular red rash, known as erythema migrans. In its more advanced stages, erythema migrans may take on a bullseye appearance. Many people are unaware of the rash, as it is usually painless, and ticks may bite in less visible locations, such as a buttock or shoulder blade.
Lyme disease is diagnosed with blood tests that detect antibodies to B. burgdorferi. Two-step testing is traditionally performed. A rapid enzyme immunoassay is performed first. If this is positive, a more time-consuming Western blot test is sent for confirmation. The FDA recently approved two rapid tests for Lyme disease that are performed simultaneously, reducing the turnaround time.
The Lyme Disease And Digestive Symptom Connection
Since Lyme disease is a systemic infection, the bacteria can affect any organ or tissue in the body. The gastrointestinal symptoms of Lyme disease and its associated infections are related to inflammation, nerve damage, and mitochondrial dysfunction. These digestive symptoms or conditions may occur in isolation, but if systemic symptoms are present or the digestive disorders are challenging to treat, Lyme disease should be considered as the underlying culprit. In addition, treating digestive disorders improves the outcome of treating Lyme disease by reducing intestinal-mediated immune dysregulation.
Also Check: How To Know You Have Lyme Disease
Lyme Disease Leg Pain At Night
There are many possible causes of leg pain at night, and Lyme disease is one of them. Lyme disease is a bacterial infection that is transmitted by ticks. Lyme disease can cause a wide range of symptoms, including leg pain. Leg pain from Lyme disease is often worse at night, and it can be accompanied by other symptoms such as fatigue, fever, and headache. If you think you may have Lyme disease, it is important to see a doctor for diagnosis and treatment.
Chronic aching muscles can be caused by Lyme disease. Aside from fatigue, headaches, dizziness, light and sound sensitivity, memory and concentration issues, stiff neck, tingling, and joint and muscle pain, a few other symptoms may occur. Before you begin to investigate the source of your muscle pain, you should first figure out what is causing it. Understanding why you feel sore when you have Lyme will help you understand how the immune system functions in this context. Musculoskeletal issues, particularly arthritis, are common in people who have this disease. The increased sensitivity to Lyme that occurs when you take medication for it is caused by the elimination of Lyme bacteria. For several years prior to Lyme, there is a marked cellular and humoral immune response that starts to affect the large joints, particularly the knee.
How To Prevent Tick
High-risk regions for infection include the Atlantic coast from Maine to Virginia, as well as Minnesota, Wisconsin, and Michigan. Lyme disease was once rare in Canada, but has been steadily ratcheting its range northward as a result of climate change.
If you live in an area where Lyme disease is common, some simple steps can minimize the risk of tick bites:
About the Author
John Ross, MD, FIDSA, Contributor
You May Like: How To Find A Lyme Literate Doctor
How Do You Treat Lyme & Tick
Access to proper tick bite treatment can often be hindered because there the medical community disagrees about how to identify those with Lyme Disease. Moreover, no perfect measures of identification exist. Lacking good measures for Lyme Disease, which has been readily accepted for decades, is compounded by lacking measures for the dozens of co-infections.
Diagnosis guidelines do not require positive blood work, yet many physicians erroneously use the CDC epidemiology study submission guidelines for diagnosis. Thus, patients are often forced to pay out of pocket for the best diagnostic tools available, which are through private lab companies.
Relying on incorrect guidelines means patients are told they must have 5 out of 10 bands to be diagnosed with Lyme. This creates a major barrier to quick and necessary tick bite treatment. Only clinical opinion after a physical exam is required to make a diagnosis of Lyme.
Read Also: Can Lyme Disease Cause Lower Back Pain
Key Points For Healthcare Providers
You May Like: Type Of Doctor For Lyme Disease
Did You Know That Lyme Disease Can Affect Your Eyes
May 16, 2022 By Johns Hopkins Lyme Disease Research Center
Lyme disease is a tick borne infectious disease caused by the bacterium, Borrelia burgdorferi . It is well known that Bb can disseminate from a tick bite throughout the body to the joints, heart, and nervous system. Less well known, is the impact that Lyme disease can have on the eyes.
Research at our Center has identified impairments in eye functioning and eye inflammation in patients with Lyme disease:
- Visual contrast sensitivity impairment occurs in post treatment Lyme disease patients and is linked to signs of cognitive and neurologic impairment and may be a marker of illness severity.
- Horner Syndrome with Negative Serology is an unusual presentation of Lyme disease.
- Lyme disease can also be an uncommon cause of Scleritis in endemic areas.
Potential eye or neuro-ophthalmologic symptoms that could be associated with Lyme disease include:
- Cranial nerve damage resulting in double vision
- Optic nerve inflammation
- being very sensitive to bright light
- having blurry vision
- seeing eye floaters
- redness and swelling of the white part of the eye
How Is It Treated
An initial episode of Lyme arthritis should be treated with a 4-week course of oral antibiotics. Patients with persistent joint inflammation and pain after the first course of antibiotics may require a second course . In some cases, joint swelling and pain can persist or recur after two courses of antibiotics. The cause of persistent arthritis is unknown but is thought to be driven by immunologic factors. Additional antibiotics have not been shown to improve these symptoms, and patient referral to a rheumatologist should be considered.
Don’t Miss: Urgent Care Lyme Disease Test
Chronic Inflammation: Why Its Time To Talk About Lyme Disease
Your body can experience chronic inflammation in response to fighting off an attack for a long period of time. Some level of inflammation is normal and a completely healthy immune response to a short-term injury, like a cut, broken bone, or the flu. Acute inflammation is a short-lived process that aids in healing by releasing antibodies, blood flow, and proteins to any damaged cells.
However, when dealing with an injury or infection your immune system cant fix right away, like Lyme disease, inflammation can last for years and go into overdrive. This puts constant stress and wear on your body and can cause your immune system to attack other organs and tissues.
There are several different factors that can contribute to chronic inflammation, including autoimmune disorders, long-term irritant exposure, or untreated infections and injuries. Additionally, your lifestyle and certain habits can increase your bodys inflammatory reaction, such as chronic stress, obesity, smoking, and drinking alcohol.
If you notice signs of chronic inflammation, this is often a strong indicator that something isnt right. If you have been bitten by a tick or have been in an area where ticks commonly live, Lyme disease could be to blame. When left untreated for months or longer, Lyme disease can progress and cause a range of chronic, debilitating symptoms, including inflammation.
Ready to heal your body? Make anappointment with Dr. Ridinger today.
Facts About Lyme Disease In Pa
Ticks thrive in the countryside of Pennsylvania in particular, and according to a study published in the Proceeding of the National Academy of Sciences of the United States of America , Lyme has a greater likelihood of occurring where suburban developments encroach on existing forest. This is thought to be because the white-footed mouse that is the most important animal in the Lyme disease transmission cycle can live without too many predators under these circumstances.
Notable statistics of Lyme disease in PA include:
- Swollen lymph nodes
For some people, a telltale sign of the disease is the red bulls eye-shaped skin rash that presents in some, but not all sufferers, within three to 30 days after being bitten by a tick.
Often, these first signs are missed when youre infected with Lyme disease and are dismissed as the flu or some other virus. This is very worrying because if antibiotic treatment isnt begun when the first signs of the disease present, your condition can become more serious.
Joint pain is another issue that can occur with Lyme disease. In the worst cases, over several weeks, nervous system and heart issues can develop. If left untreated, you may suffer from arthritis and neurological issues. In fact, according to the Arthritis Foundation, when Lyme disease is untreated, more than half of all sufferers will develop sporadic arthritis bouts.
Also Check: How To Cope With Lyme Disease
Constipation In Lyme Disease
It is estimated that up to 25% of the worlds population struggles with constipation. Not only is constipation uncomfortable and can affect daily activities, but it can also predispose individuals to develop more severe health issues. What about people who are doing all the right things to prevent constipation drinking plenty of water, eating plenty of fiber, and exercising regularly but still experience constipation?
Constipation in Lyme has been referred to as Bells palsy of the gut. Just like facial paralysis that can occur in Lyme disease, the nerves that innervate the intestines can be affected causing a decrease in the muscular wave of contractions that usually move the contents of the intestines downstream. Chronic constipation ensues, and people end up taking magnesium, Dulcolax, or other laxative medications for long periods because the underlying cause of their constipation was never identified. Nerve dysfunction can occur elsewhere in the gastrointestinal tract, including the esophagus, which leads to difficulty swallowing.
When constipation or difficulty swallowing is related to nervous system dysfunction from Lyme disease, treating the infection also helps to improve nerve signaling. Prokinetic medications help with bowel movements but also serve as physical therapy for the large intestine by increasing the activity of intestinal muscular contraction.