Lyme Disease And Ms Are Often Confused
The symptoms of Lyme disease and MS can be similar. Doctors may confuse one with the other. To diagnose these conditions, your doctor will need to conduct blood and other tests. If your doctor suspects you have MS, you may need:
Its unlikely that you have both Lyme disease and MS, but its possible. Some of Lyme diseases symptoms can mimic those of MS. It can also follow a relapse-remittance course, where symptoms come and go.
If your history and medical results suggest either condition, your doctor may decide to try antibiotic therapy to see if theres an improvement in your symptoms. Once they fully determine your condition, youll begin a treatment and management plan.
If you have Lyme disease or MS, its important to seek medical advice right away. Despite the different outlooks for Lyme and MS, early diagnosis and treatment for either condition is imperative to your overall health.
Also Check: Hyperbaric Chamber Treatment For Lyme Disease
Insights On Neurological Lyme Disease
She rounds out her discussion of these issues by interviewing five professionals who know a lot about neurological Lyme disease. One is psychiatrist Robert Bransfield, MD, a top expert on how Lyme affects the brain . Another is Sandra Berenbaum, LCSW, with whom I co-authored the book When Your Child Has Lyme Disease: A Parents Survival Guide. Others are Leo Shea, Ph.D., who has extensive experience with neuropsychological testing of children and adults with Lyme disease health advocate/blogger Scott Forsgren, founder of BetterHealthGuy.com, who writes extensively on Lyme-related issues and Connie Strasheim, author of many books about Lyme disease. They all offer useful insights on the topic of Lyme disease brain.
Throughout the book, Ducharme offers practical information with a strong helping of optimism. As she writes early on:
I find that the majority of people with Lyme brain can find resolution or, at the very least, significant improvement of their symptoms.Im not saying its quick or easy, but I have seen remarkable improvements in people who started out very, very ill with horrible Lyme brain and are now back at work, running their families and living their lives as productive, happy people.
If you or a loved one has a problem with neurological Lyme disease symptoms, I think youll find this book both helpful and hopeful.
New Scan Technique Reveals Brain Inflammation Associated With Post
A radiotracer shows elevation of the chemical marker in the brain scans of 12 participants with post-treatment Lyme disease syndrome, compared to 19 healthy control participants.Credit: Coughlin et al, Journal of Neuroinflammation, 2018
More than 1 in 10 people successfully treated with antibiotics for Lyme disease go on to develop chronic, sometimes debilitating, and poorly understood symptoms of fatigue and brain fog that may last for years after their initial infection has cleared up. Now, in a small study, Johns Hopkins Medicine researchers report they have used an advanced form of brain scan to show that 12 people with documented post-treatment Lyme disease syndrome all show elevation of a chemical marker of widespread brain inflammation, compared with 19 healthy controls.
Results of the study, in Journal of Neuroinflammation, suggest new avenues for treating the long-term fatigue, pain, sleep disruption and brain fog associated with PTLDS, the researchers say.
Theres been literature suggesting that patients with PTLDS have some chronic inflammation somewhere, but until now we werent able to safely probe the brain itself to verify it, says Jennifer Coughlin, M.D., associate professor of psychiatry and behavioral sciences at the Johns Hopkins University School of Medicine, and one of the first authors of the study report.
Controls and cases were all adult men and women over age 18 and did not differ significantly in age or body mass index .
You May Like: Will Lymes Disease Ever Go Away
How Lyme Disease Affects The Brain
Did you ever wonder how Lyme disease affects the brain, including symptoms of brain fog? The U.S. Centers for Disease Control and Prevention estimates that about 200,000 people are diagnosed every year with Lyme disease.
But many believe the true number of people suffering from Lyme in the United States is actually much higher. Thats because Lyme disease symptoms vary greatly and can impact different people in different ways. Aside from that, the ELISA screening test most doctors use misses up to 35 percent of Lyme cases, making it a horrible first-line detection for the disease.
The problem is likely only going to get worse, too, being that Lyme is among the major health effects of climate change.
Even with many cases missed in the doctors office, Lyme disease is still the most common tickborne disease in the northern hemisphere. Despite being so common, Lyme disease symptoms vary depending on the patient and how the bacteria impacts different systems of the body. In fact, Lyme disease often mimics other diseases or illnesses and be referred to as the new great imitator.
Lyme disease is often misdiagnosed as such diseases, including:
- Chronic fatigue syndrome
- Autism-like syndromes
- Various psychiatric illnesses
Lyme Disease And How It Can Affect The Brain And Nervous System
Patients with neurologic symptoms should discuss with their doctor about having a lumbar puncture to remove and check spinal fluid for antibodies of the Lyme disease causing bacteria. When the spinal fluid is examined, it should be sent for testing of the bacterial PCR , to look at the DNA of the bacteria, along with a blood sample to calculate a ratio index of bacteria and antibodies present within the patient. Please note, the blood should be drawn on the same day as the spinal fluid for an optimal study. The index refers to the ratio of bacterial antibodies in the SF compared to the antibodies present in the blood, to calculate the immune response levels in the whole body. When the index is positive, that indicates that there is a higher production of antibodies in the SF a finding strongly suggestive of central nervous system invasion by the agent of Lyme disease. It is believed that the index may remain positive long after the initial infection has been treated due to immunologic memory. Unfortunately, patients may have neurologic Lyme disease, but test negative on the Lyme index, providing a false negative. When positive however, the clinician can be confident that this particular individual has or has had central nervous system Lyme disease.
MRI
***Because an MRI scan uses a very powerful magnet, patients with pacemakers or other metallic implants should not get an MRI.
You May Like: How Long Does It Take For Lyme Test Results
Post Treatment Lyme Disease
Lyme disease, especially when treated early, often responds to antibiotic therapy, whereas MS does not. Not everyone who is treated for Lyme disease fully recovers. Sometimes there are Post Treatment Lyme Disease symptoms that can be vague and look like other illnesses. The majority of people, however, recover to lead a normal life.
When It Looks Like A Brain Tumor But It Is Lyme Disease
Pseudotumor cerebri, also referred to as idiopathic intracranial hypertension, is a condition caused by elevated cerebrospinal fluid pressure in the brain. Symptoms can mimic a brain tumor, but in actuality there is no tumor. Instead, there is unexplained intracranial pressure in the head. The condition is rare in prepubertal children.
Ezequiel and colleagues report on the case of a 9-year-old boy from Portugal who was diagnosed with pseudotumor cerebri due to Lyme disease. The child was admitted with daily pulsatile frontotemporal headache, pallor, photophobia and phonophobia, without night awakening, vomiting or visual changes, writes Ezequiel in the British Medical Journal Case Reports.
His neurological examination revealed papilloedema but was otherwise normal. Brain images were unremarkable. Serologic, PCR and cultural testing ruled out bacterial and viral agents including Mycoplasma pneumoniae, Epstein-Barr virus,Cytomegalovirus and Enterovirus. So the boy was prescribed acetazolamide .
However, ELISA and Western blot results were positive for B. burgdorferi antibodies, the bacteria causing Lyme disease. The diagnosis of neuroborreliosis was assumed, explains Ezequiel and a 21-day course of intravenous ceftriaxone was started. The boy made a complete recovery.
The authors highlight several key points:
References:
Read Also: My Dog Has Lyme Disease
Also Check: Lyme Disease Doctors In Texas
Could Lyme Disease Have Led To A Spinal Cord Lesion
Doctors considered Lyme disease as a possible cause of a longitudinally extensive spinal cord lesion in a 55-year-old man. The clinicians considered a spinal cord infarction, a malignancy and Lyme disease.
In their article Case report: Dueling etiologies: Longitudinally extensive spinal cord lesion mimicking spinal cord infarct with simultaneous positive Lyme serology and amphiphysin antibody,¹ Kalaszi and colleagues discuss the case of a patient who presented with a Bulls-eye rash 6 months prior to his illness and whose testing was suggestive of Lyme disease as a possible cause of the spinal cord lesion.
The man presented with chest pain, followed by right lower limb weakness, preceded by 2 weeks of constipation and voiding dysfunction, wrote the authors.
The spinal MRI showed extensive disease. Magnetic resonance imaging of the brain and the whole spine with contrast revealed an abnormal, increased T2 signal in the anterior aspect of the spinal cord beginning at the T4 level and extending to the conus without associated edema or contrast enhancement, wrote the authors.
The doctors considered several possibilities. The imaging findings were consistent with a longitudinally extensive transverse myelitis of potential autoimmune, paraneoplastic, or infective etiology.
The patient reported having a Bulls-eye rash 6 months prior to the onset of symptoms. In addition, he complained of autonomic dysfunction 2 weeks before his illness.
Keeping It In Perspective
Its relatively uncommon for Lyme disease to cause brain effects. When Lyme disease does result in brain swelling or problems with thinking and emotions, there are treatments that can help. Its also important to remember that only a very small portion of cognitive or psychiatric conditions are due to Lyme disease. In any case, talk with your doctor about identifying the cause of your problems and the treatment thats right for you.
Also Check: Physical Symptoms Of Lyme Disease
What Gets Stored In A Cookie
This site stores nothing other than an automatically generated session ID in the cookie no other information is captured.
In general, only the information that you provide, or the choices you make while visiting a web site, can be stored in a cookie. For example, the site cannot determine your email name unless you choose to type it. Allowing a website to create a cookie does not give that or any other site access to the rest of your computer, and only the site that created the cookie can read it.
Neurological And Psychiatric Issues Associated With Lyme Disease And Tbrf
Chronic illness often has significant impacts on mental health, and Lyme disease is no different. With the accuracy and sensitivity of todays recommended Lyme testing still so lacking, many Lyme patients have to wait too long to get accurate diagnoses and treatment. To compound this problem, many patients with Lyme-like symptoms are not even tested for the similar, but biologically distinct, Tick-Borne Relapsing Fever . That gives infections time to spread throughout the body and cause neurological and psychiatric symptoms.
This article will outline the direct and indirect effects that Borreliosis both Lyme disease and TBRF can have on mental health, including how and why untreated Lyme can develop into neurological Lyme disease.
Recommended Reading: Symptoms Of Lyme Disease In Humans Mayo Clinic
Why And How Lyme Disease And Tbrf Affect Mental Health
Lyme disease and TBRF can wreak havoc on a patients mental health in the following ways:
- Direct effects As with syphilis, the bacteria that causes Lyme disease and TBRF can invade the central nervous system and cause neurological and psychiatric symptoms that are organic in origin. This is what doctors call neurological Lyme disease or Lyme neuroborreliosis.
- Indirect effects The discomforts and challenges of living with and/or being treated for Lyme disease or TBRF can lead to anxiety, depression, and other mental health conditions that are not necessarily caused by the bacteria, but are indirectly caused or exacerbated .
Of course, these effects are not either/or, but rather can coexist and compound one another. Learn more about each below.
Dont Miss: Lyme Disease Test Kit Cvs
Demographics And Clinical Data
Patient characteristics are shown in Table 1. Cranial nerve palsy and meningitis were the dominant clinical symptoms of LNB. Three patients demonstrated contrast enhancement of cranial nerves, which corresponded to clinical findings. The remaining patients had normal structural MRI.
Table 1 Epidemiological and clinical characteristics among 26 patients with Lyme neuroborreliosis
Recommended Reading: Does Lyme Disease Cause Neurological Problems
Understanding Neurologic Lyme Disease
Lyme disease is a condition that is carried by infected black-legged deer ticks. These ticks are usually found in wooded areas with tall grass. Ticks intended targets are deer and other woodland animals, but will just as easily attach themselves to hikers, hunters, and unsuspecting adventurers. Lyme disease cases are consistently on the rise and the CDC estimates that the current numbers, around 300,000 cases every year, are dramatically underreported.
Dr. Joseph Schneider, DC, DACNB head neurologist at the Hope Brain and Body Recovery Center utilizes state-of-the-art treatment methods and expertise to help patients suffering from Neurologic Lyme Disease. Our team understands how much of a burden Lyme Disease can be and want to help you manage your symptoms and restore your quality of life.
Get Tested And Treated Early
Studies acknowledge that up to 30% of patients go on to suffer further Lyme symptoms even after treatment, sometimes called Post-Treatment Lyme Disease Syndrome . One of the biggest risk factors for this condition is delayed treatment.
Research is finally, if slowly, catching up to the reality that letting Lyme disease slip through the cracks of insufficient diagnostic testing causes real suffering for patients. IGeneX is at the forefront of solving this problem, offering more sensitive and accurate testing for Lyme disease and other tick-borne diseases that can cause mental health problems when left untreated. Learn more today.
Also Check: Western Blot Test For Lyme Disease
Don’t Miss: What Are Some Signs Of Lyme Disease
Lyme Is Not The Only Threat
As mentioned earlier in this article, there is another group of borrelia that causes a disease that is similar to, but biologically distinct from, Lyme. This disease, called Tick-Borne Relapsing Fever or TBRF, is often characterized by fevers that wax and wane every few days. However, many patients never experience relapsing fevers or any fevers at all. Like those of Lyme and other tick-borne diseases, TBRF symptoms can often go undetected or be mistaken for other conditions, which can give the disease time to develop into neurological symptoms.
So, as with Lyme, it is crucial to get an early and accurate diagnosis of TBRF. Be aware that TBRF will not show up on a Lyme test the test must be designed to test for TBRF borrelia in order to show accurate results. If symptoms are Lyme-like but test results are negative, doctors should consider the possibility of TBRF.
Epidemiology And Clinical Presentation
More than 200,000 cases of Lyme disease in the United States have been reported to the Centers for Disease Control, resulting in a national incidence of 9.7 cases per 100 000 population. The prevalence of Lyme disease varies significantly by geography and has a seasonal incidence . More than 93% of Lyme disease cases in the United States have been reported in high endemic Midatlantic states, Michigan, and Minnesota. Lyme disease occurrence peaks during summer months, reflecting the enhanced transmission by the nymphal tick vectors during May and June. Since Lyme disease became nationally notifiable in 1991, the annual number of reported cases has more than doubled.
Fig 2.
A, Summary of reported cases of Lyme disease in the United States. There is 1 dot within the county of residence for each reported case. Note the widespread diversity of cases correlating with the prevalence of infected Ixodes species in different geographic areas. Courtesy of the Centers for Disease Control. B, The beige-shaded areas indicate the geographic distribution of recorded clinical cases of Lyme borreliosis. The colored ellipses indicate the distribution of the various Borrelia subspecies. is reprinted with permission from Nature Publishing Group.
Fig 3.
Erythema migrans rash with the typical target appearance that is virtually diagnostic of Lyme disease.
Comparison of clinical differences between American and European LNB*
Dont Miss: Rocky Mountain Spotted Fever Vs Lyme Disease
Recommended Reading: Dr Jay Davidson Lyme Disease
The Case Study Pathology Is Characteristic Of Dementia With Lewy Bodies
The fresh brain weighed 996 g and appeared atrophic Coronal sections through the left cerebral hemisphere and brain stem revealed mild enlargement of the lateral ventricle, particularly the temporal horn. The substantia nigra was normally pigmented or nearly so. Microscopically, nigral and cortical Lewy bodies, were seen with hematoxylin and eosin stain . Immunohistochemistry for -synuclein showed numerous immunoreactive Lewy bodies and fibers in substantia nigra, hippocampal formation and neocortex, Figures 4CE). IHC for hyperphosphorylated tau revealed intense staining of many limbic neurofibrillary tangles and neuropil threads , and of occasional neurofibrillary tangles in neocortex, but senile plaques were extremely rare, and each contained only a few fibrils . H& E showed prominent thickening of small blood vessels in gray and white matter, extensive mineralization of pallidal vessels, and rare microglial nodules in the hippocampal formation. Immunohistochemistry for Iba-1 , CD68 , and CD163 showed moderate numbers of activated microglia and large numbers of macrophages in hippocampal formation and spinal cord . In summary, we see DLB accompanied by features of Alzheimers disease, a common presentation.
Mri Findings In Lyme Neuroborreliosis
Section
Clinical Cases
Paternain A1, Villino R2, Riverol M2, Malmierca P1, Soriano I1, Calvo-Imirizaldu M1, García-Eulate R1, Domínguez PD1
1. Department of Radiology, Clínica Universidad de Navarra, Spain
2. Department of Neurology, Clínica Universidad de Navarra, Spain
Connected authorsArea of InterestImaging TechniqueProcedureSpecial Focus
A 22-year-old woman was admitted to the emergency room with sudden right peripheral facial palsy. She also referred to progressive and ascending burning pain in the spine for two weeks. After a trip to the mountains one month before, she had developed an erythematous skin lesion that resolved spontaneously.
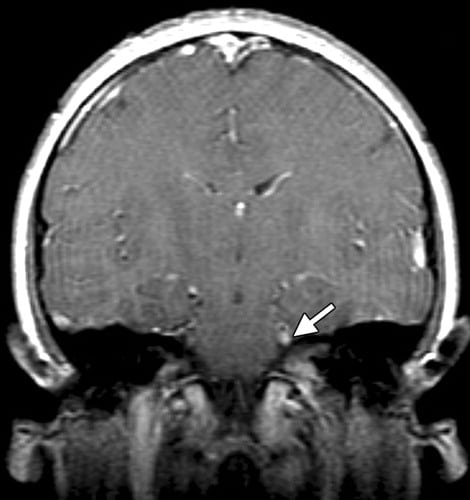
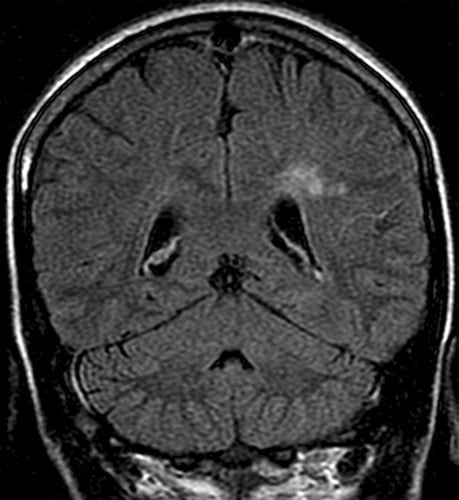
MRI of the spine showed a diffuse enhancement of all nerve roots after contrast administration, without a significant thickening . In the brain, bilateral enhancement of the trigeminal nerves in the posterior cranial fossa was also appreciated. In addition, there was also an abnormally high signal intensity in FLAIR surrounding the cerebral aqueduct of Sylvius .
A lumbar puncture was performed, which showed a positive serology for Lyme disease. The patient was treated with intravenous ceftriaxone for two weeks, followed by oral doxycycline for another 2 weeks, having a complete clinical response afterwards.
Read Also: Can Mosquitoes Carry Lyme Disease