Lyme Disease Often Leads To Lyme Arthritis
Although Lyme disease may affect many organs, such as the heart and nervous system, joint involvement tends to be the most common and persistent manifestation, resulting in joint swelling and pain. About 60% of people who are infected with Lyme develop arthritis unless they receive antibiotics.
In most, Lyme arthritis resolves after 30 days of treatment with an oral antibiotic, such as doxycycline or amoxicillin. Individuals with persistent symptoms despite an oral antibiotic usually respond to treatment with an intravenous antibiotic for 30 days. However, about 10% of those with Lyme arthritis fail to respond to antibiotic treatment, for reasons that have long been unclear.
Older Adults Vulnerable To Lyme Disease
For most people, Lyme disease will result in no lasting illness after some initial flu-like symptoms. But for others, it can become debilitating if left untreated. Older adults can be particularly vulnerable, and they may brush off the effects. Symptoms of Lyme disease that has progressed include short-term memory loss, joint pain or swelling, and fatigue signs often attributed to aging.
You might start thinking, Im just beginning to lose my memory a bit. And everybody does that as they get older, said Dr. Brian Fallon, a psychiatrist and director of the Lyme and Tick-Borne Diseases Research Center at Columbia University.
Other long-term effects include chronic pain, irregular heartbeat, brain fog, shooting pains or numbness in the arms or legs, and severe headaches.
Is Lyme Disease Contagious
There is no evidence that Lyme disease is contagious. You can’t get infected from touching, kissing, or having sex with a person who has Lyme disease, or from receiving a transfusion of their blood. Untreated Lyme disease during pregnancy can lead to infection of the placenta, but new mothers cannot transmit the disease to their baby through breast milk.
Recommended Reading: Early Signs Of Lyme Disease In Adults
Gastrointestinal Symptoms Of Lyme Disease
The spirochete that causes Lyme disease Borrelia burgdorferi and the associated tickborne infections such as Bartonella and Babesia can directly affect any organ system in the body, including the gastrointestinal tract. About 80% of the immune system is located around the digestive tract, so digestive health influences the immune response. Gastrointestinal symptoms of Lyme disease range from food intolerances to constipation.
Rarely does acute Lyme disease cause gastrointestinal symptoms, but occasionally nausea, vomiting, heartburn, and abdominal pain can occur. More commonly, digestive symptoms such as constipation, gas/bloating, and abdominal discomfort occur in chronic or late-stage Lyme disease. Lyme bacteria can directly infect the gastrointestinal tract causing inflammation that creates digestive symptoms. In turn, digestive issues can cause immune dysregulation increasing susceptibility to chronic infections. Whether digestive problems are a result of Lyme disease or increase the susceptibility to chronic infections, it is essential to address the underlying issues to restore health more quickly and effectively.
Chronic Lyme Arthritis: A Mystery Solved
- By John Ross, MD, FIDSA, Contributing Editor
In 1975, researchers from Yale investigated an epidemic of 51 patients with arthritis who lived near the woodsy town of Lyme, Connecticut. The most common symptom was recurrent attacks of knee swelling. A few had pain in other joints, such as the wrist or ankle. Many had fever, fatigue, and headache. Some remembered a round skin rash before the onset of knee swelling.
We now know that Lyme disease is an infection acquired from tick bites, caused by a spiral bacterium named Borrelia burgdorferi. After a tick bite, Borrelia bacteria wriggle through the skin away from the bite site. This leads to a circular red rash, known as erythema migrans. In its more advanced stages, erythema migrans may take on a bullseye appearance. Many people are unaware of the rash, as it is usually painless, and ticks may bite in less visible locations, such as a buttock or shoulder blade.
Lyme disease is diagnosed with blood tests that detect antibodies to B. burgdorferi. Two-step testing is traditionally performed. A rapid enzyme immunoassay is performed first. If this is positive, a more time-consuming Western blot test is sent for confirmation. The FDA recently approved two rapid tests for Lyme disease that are performed simultaneously, reducing the turnaround time.
Don’t Miss: Antibiotics Given For Lyme Disease
The Patient Who Suspects Chronic Lyme Infection
LD is so prevalent and well known that the public is well aware of its symptoms. Many patients, particularly those who have been diagnosed with fibromyalgia, degenerative arthritis, or neuropathies of unknown origin, believe they may have had unrecognized and undiagnosed LD. They may request recurrent LD testing and even antibiotic therapy, despite negative Lyme serologic tests.
In reality, some of these patients may be correct. The authors have encountered several patients who presented with a chronic pain syndrome such as fibromyalgia who were later found to have disseminated LD or PTLDS. At this juncture, we are not prepared to set out any specific diagnostic or treatment protocols. We do, however, believe that pain practitioners must consider LD as an underlying cause of pain in patients who present without a clear event or cause of chronic muscle, nerve, or joint pain. In addition to diffuse musculoskeletal and joint pathologies, cranial neuropathy , and radiculoneuritis are 2 of the most common presentations of acute, early neurologic LD. Given what appears to be an epidemic of LD, we will carefully monitor the situation and bring you updates through Practical Pain Management.
The Aches And Pains Of Tick
byJennifer Crystalon July 23, 2019
The first time I saw the award-winning Lyme documentary Under Our Skin, I was seated in the theater. In the film, a doctor who doesnt believe in chronic Lyme was asked what might otherwise be causing the symptoms of the more than 427,000 people afflicted by tick-borne illness every year. He suggested it could just be the normal aches and pains of getting older.
With that bit of ignorance so baldly stated, everyone in the theater let out a collective groan.
There is a big difference between the aches and pains that come with tick-borne illnesses and those associated with every day life.
To be fair, those who havent wrestled with tick-borne illnesses might be confused by the generic descriptor aches and pains. Thats because its like so many other nebulous descriptions,like fatiguethat could be the result of any number of illnesses. Let me explain.
In my former athletic life, I was a hard-core skier. In college I skied almost every winter day, and after I graduated and moved to Colorado, I skied every Saturday and Sunday from November to April. Often my muscles were sore after these workouts. Sometimes Id even wake up with an aching back, but only because Id worked my arms too hard the day before. These aches and pains were akin to those anyone might feel after working out at the gym, going for a run, or weeding the garden. The muscles get overworked, and you feel residual soreness.
You May Like: Lyme Arthritis Synovial Fluid Analysis
Vision Auditory And Other Sensory Symptoms
In addition to aches and pains, many tick-borne diseases can cause vision and auditory issues such as those listed below:
- Light sensitivity has been linked to Bartonellosis .
- Retinal inflammation, which can cause blurred or distorted vision, has also been linked to Bartonellosis.
- Red eyes, clinically referred to as conjunctival injection, can be a sign of Ehrlichiosis and Anaplasmosis , both of which can be hard to detect because of the variation in symptoms across patients.
- Sound sensitivity can be associated with Bartonellosis.
- Ringing in the ears can be a symptom of Babesiosis.
- Burning sensation on the skin and numb skin patches can both be signs of Bartonellosis.
How To Treat Thrombocytopenia
The treatment you will receive for thrombocytopenia ultimately depends on the severity and cause of the condition.
If there is no excessive bleeding and platelet counts are not dangerously lowor are still within a safe realmtreatment may consist of little more than monitoring the situation.
Your doctor may schedule some follow-up tests and ask you to pay attention to new bruises or markings. You will be asked to alert them if you notice changes prior to your follow up.
In more severe cases where bleeding is heavier and platelet counts are lower, thrombocytopenia is treated with medicine.
Read Also: Mayo Clinic Low Back Pain Exercises
Also Check: How Do I Get Tested For Lyme Disease
Determining The Source Of Your Symptoms
Again, its important to note that symptoms of tick-borne diseases in humans can vary greatly from person to person and can change over time if diseases are not diagnosed and treated in a timely manner.
The presence of any one of the symptoms above does not alone guarantee that you have a tick-borne disease, but if you do experience them alongside any other potential symptoms, its important to talk to a trusted doctor and get tested immediately.
IGeneX is proud to offer highly accurate, highly sensitive diagnostic testing for all major tick-borne diseases in the U.S., including Lyme disease, Tick-Borne Relapsing Fever, Rocky Mountain Spotted Fever, Bartonellosis, Babesiosis, and Ehrlichiosis and Anaplasmosis. Learn more about IGeneX testing today.
Celiac Disease And Autoimmune Disorders
The human body has an immune system which helps to fight off infections. It is a sophisticated system comprising of several type of cells that play a variety of important roles in killing an organism when it invades the body. The immune system gets activated when an organism such as a virus or bacteria enters the body but goes back to the resting phase once the organism is killed. It is smart enough to recognize what is part of its own body and what is foreign coming from outside. However, in some instances the immune system becomes abnormal and starts to recognize part of the body as foreign. It then goes and attacks those parts of the body causing damage with serious health consequences. These are called autoimmune disorders.
There are numerous autoimmune disorders known. One example is type-1 diabetes, where the immune system attacks and permanently destroys the cells in the body that make the hormone called insulin. Once this happens, the patient now has to take insulin by injections for the rest of their lives. Another common example is thyroid disease, where the immune system destroys the thyroid . This leads to low thyroid function and one now has to take the thyroid hormone in the form of a pill every day. Some other examples of autoimmune disorders include lupus, multiple sclerosis, rheumatoid arthritis, etc.
Don’t Miss: What Are The First Symptoms Of Lyme Disease
How Is Lyme Disease Treated
Generally speaking, the earlier and more quickly Lyme disease is treated, the quicker and more complete your recovery will be.
Antibiotics are used to treat Lyme disease, and they include:
- Oral antibiotics. Oral antibiotics are the standard treatment for Lyme disease when its in its early stages. Cefuroxime or amoxicillin is prescribed for younger children, breastfeeding or pregnant women and some adults. Doxycycline is given to children and adults over the age of eight years.
The usual length of a course of antibiotics for Lyme disease is between 14 and 21 days.
- Intravenous antibiotics. If you are suffering from complications affecting your central nervous system, you may be prescribed treatment via intravenous antibiotics for between 14 and 28 days. This course of action gets rid of any infection, although it may still take you a long time to recover entirely from your symptoms.
Intravenous antibiotic treatment often causes a range of side effects, including:
- Mild to severe diarrhea
- Lower white blood cell count
- Infection or colonization with other antibiotic-resistant organisms
Even though there is a risk of experiencing these side effects, its imperative to undergo the course of treatment your doctor prescribes to avoid the serious complications Lyme disease can have.
Early Symptoms And Signs Of Lyme Disease
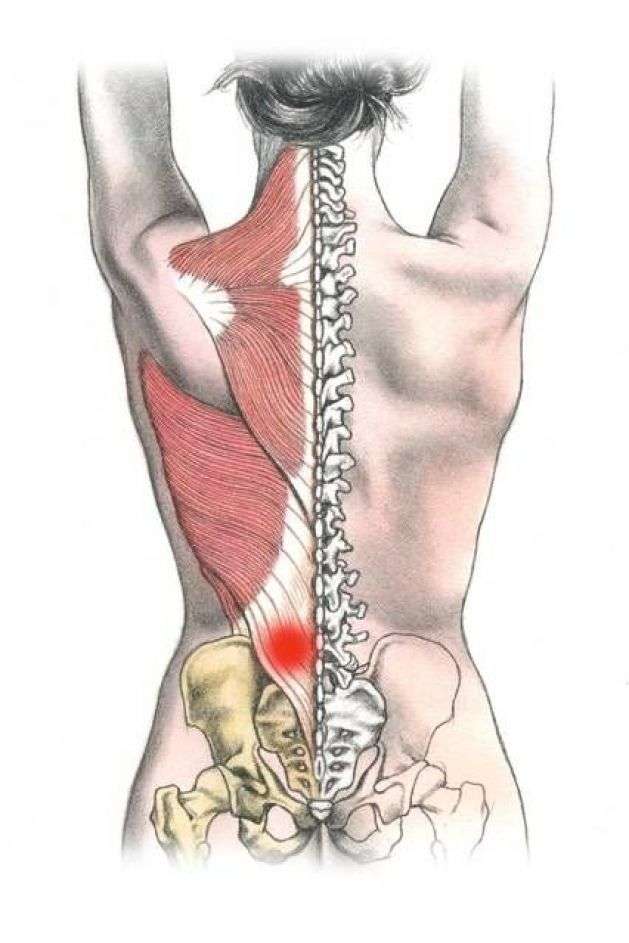
You can expect a small, red bump on the site of your bite, or where you removed the tick from, and this will resolve within a day or two. This is to be expected after being bitten by any insect, and it in itself is not an indicator that you have Lyme disease.
However, if you have been infected, you can expect the following within a month or so:
- Flu-like symptoms. Early-stage Lyme disease can present as chills, fever, fatigue body aches, stiff neck, headache and other flu-like symptoms.
- Rash development. Between three and 30 days after an infected tick bites you, you may see a rash that looks like a bulls eye. This will expand over days, and it can grow to as many as 11 to 12 inches across. It is usually not painful or itchy.
You May Like: New Treatments For Chronic Lyme Disease
Treatment For Lyme Disease
People suffering from Candida overgrowth related to Lyme disease infection or treatment should avoid the inflammatory foods listed above but also consider making the following adjustments to their dietary habits:
- Consider a low-carbohydrate diet for a while. This will deprive Candida of the simple sugars it thrives on. Next, consider eating a completely grain-free and legume-free diet with carbohydrates derived exclusively from root vegetables, sweet potatoes, winter squash, non-starchy vegetables, and small amounts of low-sugar fruits, such as wild blueberries and avocado. It is possible to take anti-Candida diets to extremes, so I strongly recommend working with a qualified nutritionist or dietitian if youre struggling with Candida overgrowth and trying to eat to support healing.
- Incorporate functional foods with antifungal properties. Unrefined coconut oil contains lauric acid and caprylic acid, unique fatty acids that exert anti-Candida properties. Garlic, thyme, and rosemary are common kitchen herbs with antifungal properties that can assist with Candida management.
Diet alone often isnt enough to address significant Candida overgrowth. In the case of stubborn Candida overgrowth, it is essential to work with a practitioner who can order testing and implement treatments for Candida overgrowth. I regularly work with clients to address Candida overgrowth using strategic herbal formulas, probiotics, therapeutic fatty acids, and dietary changes.
Symptoms Of An Enlarged Spleen
An enlarged spleen usually does not cause many symptoms, and the symptoms that it does cause may be mistaken for many other medical conditions. Because the enlarged spleen lies next to the stomach and sometimes presses against it, people may feel full after eating a small snack or even without eating. People may also have abdominal or back pain in the area of the spleen in the upper left part of the abdomen or the left side of the back. The pain may spread to the left shoulder, especially if parts of the spleen do not get enough blood and start to die.
If hypersplenism causes severe anemia, people may be tired and short of breath. People may also have frequent infections as a result of too few white blood cells, and the tendency to bleed as a result of too few platelets.
Also Check: Lyme Disease Symptoms Rash Pictures
Lyme Disease Manifesting As Acute Transverse Myelitis
Acute transverse myelitis is a neurologic disorder caused by inflammation of the spinal cord. This inflammation can damage or destroy the fatty substance protecting the nerve cell fibers along the spine and disrupt the communication between the nerves in the spinal cord and the rest of the body.
Clinical signs and symptoms depend on the affected region of the spinal cord, explains Kaiser and colleagues in a recently published case report, Lyme myelopathy: Case report and literature review of a rare but treatable disorder.
The causes of ATM include demyelinating processes, infections, autoimmune disorders, malignancies, vascular insults, and nutritional deficiencies, writes Kaiser.
There have been documented cases of Lyme-associated ATM, but they are rare. Only 25 cases have been reported in the literature. Three of those cases reported an erythema migrans or another rash and only 5 individuals reported a recent tick bite.
In the journal Multiple Sclerosis and Related Disorders, Kaiser describes the case of a 56-year-old man who developed transverse myelitis as a complication of Lyme disease.
The man, who was an avid gardener living in Pennsylvania, developed right back and flank pain , as well as numbness and tingling that eventually spread over the abdomen, writes Kaiser, from the University of Pittsburgh.
The mans signs and symptoms included:
There was some relief of pain with steroids and an antiviral medication.
Related Articles:
When Should I Go See My Doctor
Anyone who has been bitten by a black-legged deer tick is at risk for Lyme disease. The highest risk groups include those living in or visiting endemic areas, especially people who spend significant time outdoors such as gardeners, hikers, or outdoor workers.
Patients should seek advice from their doctor if they have a suspicious round expanding red skin lesion, and/or show signs of summer-flu, particularly during Lyme disease season, which is highest-risk late spring through July/August. If those circumstances apply or symptoms persist it is very important to go to a physician.
For the west coast and other more temperate regions Lyme disease can be a year-round concern.
In the later disseminated stages, Lyme disease can be a much more insidious and complex illness. An individual should seek medical care if experiencing symptoms such as prolonged fevers, unexplained fatigue, painful joints, new or unusual headache, or heart or neurologic symptoms. If unexplained viral-like symptoms last for more than 1-2 weeks, please seek the advice of a physician.
Read Also: How To Avoid Lyme Disease
Later Symptoms And Signs Of Lyme Disease
If you dont seek treatment, other symptoms and signs of infection may appear over the following weeks and months, including:
- The bulls eye rash. It is also called erythema migrans, and it may appear on other areas of your body.
- Neurological problems. At any time after the initial Lyme disease infection, even years later, you could develop meningitis, Bells palsy , weakness or numbness in your limbs and impaired muscle movement.
You may also suffer from:
- Other rashes
Many weeks after infection, some people develop:
- Severe fatigue