What To Do If You Have A Blacklegged Tick Bite
Remove the tick by pulling it directly out with fine-tipped tweezers. Lift upward with slow and even pressure. Dont twist when removing it. Dont crush it or put soap or other substances on it. Dont apply heat to it.
Place the tick in a resealable container. See if you can identify what kind of a tick it is.
Immediately after removing the tick, wash your skin well with soap and water or with rubbing alcohol.
Not all ticks carry Lyme. The Lyme bacteria is transmitted only by blacklegged ticks in their nymph or adult stage.
Save the tick to show your doctor. The doctor will want to determine if its a blacklegged tick and if theres evidence of feeding. Ticks enlarge as they feed. Your risk of getting Lyme from an infected tick increases with the length of time that the tick fed on your blood.
Summary:
Pull the tick out with tweezers and save it in a resealable container for identification.
Tickborne Triggered Seizure Disorder: Case Study Of A Teenager With New Onset Seizure Disorder And The Neurological Impact Of Tickborne Diseases
The Neurological impact of Bartonella and Rickettsia
This next case study is of an 18-year-old female who was adopted at the age of 5. Her adoptive mother described her as a malnourished premature baby who eventually received good foster care. This young lady was diagnosed with a growth hormone deficiency that was left untreated in her country of origin at the age of two. By the age of five, she was adopted and moved to the US with her American family. She was fully immunized twice, diagnosed with hypothyroidism and inadequate growth. By this time, an Endocrinologist was onboard and treating her thyroid and growth deficiencies. She seemed to rebound, reaching puberty by the age of 13. Life was stable for some time until January of 2016. She was nearly sixteen years old and developed sudden neuropsychiatric symptoms with acute confusion, severe obsessive-compulsive disorder, frequent urination, insomnia, auditory hallucinations, severe sensory issues, leg tremors and eventually catatonia. Given her acute changes, her mother rushed her to the Emergency Room for evaluation. EEG was negative and she was hospitalized for apparent acute psychosis treated with Risperdal and Ativan.
After her hospitalization she followed up with a well-known Neurologist who identified positive Mycoplasma and initiated a course of Azithromycin. By the fourth dose she began to return to her normal state and began sleeping again. She was treated for over a month with antibiotics and seemed stable.
Regression And Other Symptoms In Children
Children are the largest population of Lyme patients.
The CDC study of reported Lyme cases from 19922006 found that the incidence of new cases was highest among 5- to 14-year-olds . About one quarter of reported Lyme cases in the United States involve children under 14 years old .
Children can have all the signs and symptoms of Lyme that adults have, but they may have trouble telling you exactly what they feel or where it hurts.
You may notice a decline in school performance, or your childs mood swings may become problematic.
Your childs social and speech skills or motor coordination may regress. Or your child may lose their appetite.
Children are more likely than adults to have arthritis as an initial symptom 01267-2/fulltext#sec0040″ rel=”nofollow”> 25).
In a 2012 Nova Scotian study of children with Lyme, 65 percent developed Lyme arthritis . The knee was the most commonly affected joint.
Summary:
Also Check: Can All Ticks Carry Lyme Disease
Common Abnormalities Found In People With Lyme Disease
Many of the more severe or chronic cases of Lyme disease seem to have a lot of similar physiological abnormalities. I remember having some of the blood work forms in hand, thinking, why the hell is Dr. S testing for that? What a weirdo. I thought to myself, I have Lyme, and thats that! End of story. Fix me please. But now, I can see why he as well as DC have chosen some of the tests that would not necessarily be on the normal blood test and would have to be sent out to LabCorp, Quest, or whatever company your hospital sends special tests to. Some were normal blood tests but I had no idea why they were important to test for. Well that is usually not the case. So, not a weirdo just good doctors who can see the whole picture.
Another term for having several abnormalities, given by one of the worlds most renowned Lyme doctors is called Multiple Chronic Infectious Disease Syndrome, or MCIDS. I prefer to tell people instead of using this fancy term, I have a laundry list of shit wrong with me. You say potato, I say potato. Tomatoes, tomatoes.
So, there are some abnormalities that people should consider when having Lyme disease. These abnormalities are important to look into because they could be hindering your path to getting well:
Toxicity Toxicity is an important issue among many Lymies. People who arent sick are able to get rid of the toxins more easily and people with Lyme tend to struggle at eliminating these toxins from their body.
*****
Chronic Lyme Disease Patients Profoundly Debilitated

Many patients with chronic Lyme disease are profoundly debilitated. Investigators of the four NIH-sponsored retreatment trials documented that the patients quality of life was consistently worse than that of control populations and equivalent to that of patients with congestive heart failure. Pain levels were similar to those of post-surgical patients, and fatigue was on par with that seen in multiple sclerosis.
An LDo published survey of over 3,000 patients with chronic Lyme disease found that patients suffer a worse quality of life than most other chronic illnesses, including congestive heart failure, diabetes, multiple sclerosis and arthritis. Over 70% of patients with chronic Lyme disease reported fair or poor health. Similar results have been found in other studies. Many of the symptoms associated with Lyme disease are common in other diseases. The CDC surveillance criteria for confirmed cases specifically exclude most of the symptoms that patients report, including fatigue, sleep impairment, joint pain, muscle aches, other pain, depression, cognitive impairment, neuropathy, and headaches. However, these common symptoms can be severe and may seriously affect quality of life.
You May Like: Beach House Rentals Old Lyme Ct
Treating Neurological Lyme Disease
Though neurological and psychiatric symptoms can be reduced with antibiotic treatment, emotional and cognitive problems arising from late-stage or chronic Lyme often call for a broader range of interventions. This includes lifestyle changes in such areas as diet, exercise, and environment.
Again, its worth reiterating that the longer an infection goes undetected, the harder it is to treat, and the more likely it is that symptoms will require multi-pronged, multi-system interventions besides antibiotics alone.
What Are The Signs And Symptoms Of Stage 3 Lyme Disease
Late or chronic Lyme disease refers to manifestations that occur months to years after the initial infection, sometimes after a period of latency. Signs and symptoms of chronic Lyme disease are primarily rheumatologic and neurologic. Acrodermatitis chronica atrophicans, the cutaneous feature of late-stage Lyme disease, is found almost exclusively in European patients.
Most patients presenting with late disease do not have a history of erythema migrans, because the rash typically leads to earlier treatment, which prevents the development of late disease. However, other manifestations of the disease may coexist or may have occurred in the past. Thus, a history of Bell palsy, aseptic meningitis, arthritis, acral paresthesias or dysesthesias , or cognitive dysfunction may be diagnostically useful.
Maladaptive host responses can lead to a variety of syndromes in stage 3, as follows :
- Postinfectious Lyme arthritis Massive inflammatory synovial proliferation, usually in a knee
- Posttreatment Lyme disease syndrome Pain, neurocognitive impairment, fatigue
- Autoimmune joint disease Rheumatoid arthritis, psoriatic arthritis, or peripheral spondyloarthropathy
- Autoimmune neurologic disease Chronic idiopathic demyelinating polyneuropathy
Lyme arthritis is the hallmark of stage 3 Lyme disease. It tends to involve large joints . Arthritis must be differentiated from arthralgia, which is common in early disease.
References
Read Also: What Antibiotics Treat Lyme Disease In Humans
Lyme Disease Symptoms In Dogs
One of the main symptoms of Lyme disease is limping in dogs, which can be alarming when first spotted. With Lyme disease, lameness is ongoing and can last anywhere from three to four days but sometimes, even goes on for weeks on end. It can worsen in the same leg or move on to other legs. If it jumps to other legs, then its often called shifting-leg lameness.
This lameness causes extreme discomfort, because lameness often causes a dogs legs to feel swollen, warm, and painful. If you see your dog suddenly limping, dont assume that they injured their paw or got tired from running too much at the park. It might be something more serious, like Lyme disease.
How can you tell whether they injured themselves or if its Lyme disease? If your dog is consistently lifting the same leg, then hes probably just injured it. But if the leg pain is shifting around and shifts from one leg to the next, it could be a sign of shifting-leg-lameness and actually a result from Lyme disease.
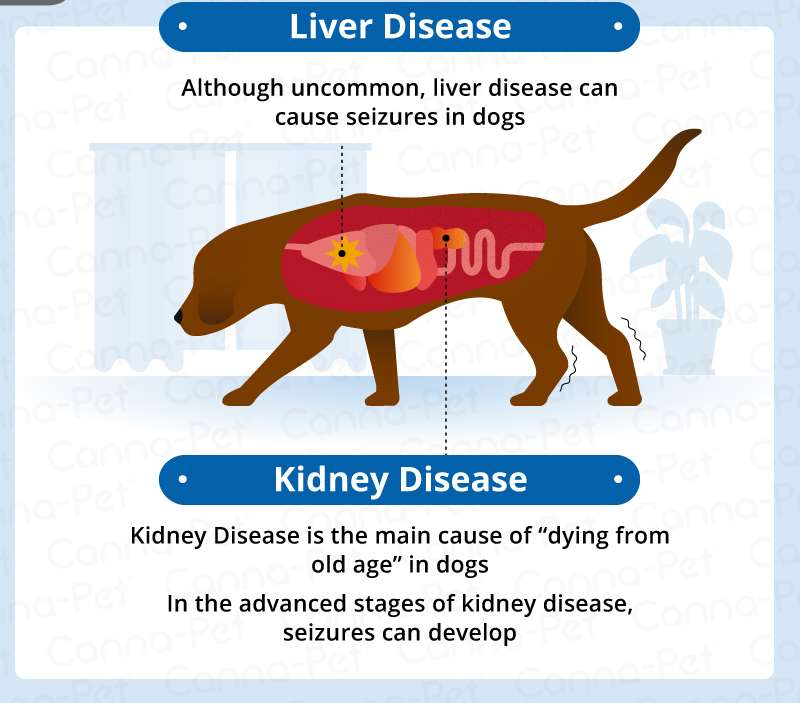
Lyme disease can also cause kidney problems in dogs. Dog kidney disease comes with a host of other problems like diarrhea, lack of appetite, weight loss, increased urination and thirst, and fluid build-ups.
Some general symptoms of Lyme Disease in dogs include:
- Stiff walking with an arched back
- Sensitivity to touch
- Nervous system complications
Does Lyme Disease Affect The Brain And Nervous System
Lyme disease affects the nervous system. This statement is both accurate and terrifying since, for many of us, damage to the brain is the most feared consequence of disease. However, when it comes to Lyme disease, much of this fear is misplaced. Lyme disease can affect the lining of the brain, a disorder known as meningitis. Other than causing fever and bad headaches, this form of meningitis is remarkably benign nobody has ever died of it, and it has rarely if ever caused significant damage to any patients brain. On extremely rare occasions, the infection can involve the brain or spinal cord, disorders that are now extraordinarily rare. Other patients can develop inflammation of various nerves, e.g., the nerves that control the muscles on one side of the face this might occur in about 5% of untreated individuals. Other nerves can be affected, but even less frequently.
When considering these disorders, it is essential to recognize some key facts. First, the infection is highly responsive to antibiotics. Second, if the facial nerve has been severely damaged, there may be some residual weakness after treatment. However it is extraordinarily rare for there to be any permanent damage to the brain itself.
Recommended Reading: Walk In Clinic East Lyme Ct
Lyme Is Not The Only Threat
As mentioned earlier in this article, there is another group of borrelia that causes a disease that is similar to, but biologically distinct from, Lyme. This disease, called Tick-Borne Relapsing Fever or TBRF, is often characterized by fevers that wax and wane every few days. However, many patients never experience relapsing fevers or any fevers at all. Like those of Lyme and other tick-borne diseases, TBRF symptoms can often go undetected or be mistaken for other conditions, which can give the disease time to develop into neurological symptoms.
So, as with Lyme, it is crucial to get an early and accurate diagnosis of TBRF. Be aware that TBRF will not show up on a Lyme test the test must be designed to test for TBRF borrelia in order to show accurate results. If symptoms are Lyme-like but test results are negative, doctors should consider the possibility of TBRF.
The New Tick Diseases You Need To Know Aboutone Of Them Is Way Worse Than Lyme
byAdmin at Global Lyme Allianceon March 24, 2017
Lyme disease is the most common tick-borne disease, but it’s not the only one we need to be aware of this summer.
Read Also: Foods To Avoid With Lyme Disease
Chronic Lyme Disease Symptom Severity
In LDos chronic Lyme disease survey, over 75% of patients reported at least one symptom as severe or very severe and 63% reported two or more such symptoms. Find out more about LDo peer-reviewed published surveys. The chart below shows the severity of ten common chronic Lyme symptoms.
The survey also found that patients with chronic Lyme disease have high disability and unemployment rates. Over 40% of patients with chronic Lyme disease reported that they currently are unable to work because of Lyme disease and 24% report that they have received disability at some point in their illness.
Get Tested And Treated Early
Studies acknowledge that up to 30% of patients go on to suffer further Lyme symptoms even after treatment, sometimes called Post-Treatment Lyme Disease Syndrome . One of the biggest risk factors for this condition is delayed treatment.
Research is finally, if slowly, catching up to the reality that letting Lyme disease slip through the cracks of insufficient diagnostic testing causes real suffering for patients. IGeneX is at the forefront of solving this problem, offering more sensitive and accurate testing for Lyme disease and other tick-borne diseases that can cause mental health problems when left untreated. Learn more today.
Recommended Reading: Can Lyme Disease Cause Leg Weakness
Neurological Complications Of Rheumatologic Conditions
Systemic lupus erythematosis , rheumatoid arthritis, Sjogren syndrome, and mixed connective tissue disease are a few of the rheumatologic conditions that can affect the nervous system, and they can do so in a variety of ways. Additionally, many parts of the nervous system can be involved, from the muscle to the peripheral nerve all the way to the cerebral cortex. For instance, some patients can have abnormal blood clotting as a complication of SLE, which can affect the brain. Additionally, these conditions may place patients at risk for opportunistic infections, as mentioned above, usually due to the longstanding immune therapy required to treat these diseases.
Chronic Lyme And Mental Health
The CDC lists having a chronic disease as a risk factor for developing mental illness. This underscores the reality that even for patients who do not develop neurological Lyme disease, the experience of Lyme disease alone can cause or exacerbate mental health problems like depression, anxiety, and others listed above.
Getting diagnosed and treated for Lyme disease can be stressful and exhausting, especially the longer this process takes which, for many, can be several years. Patients often must deal with conflicting or inaccurate diagnoses, lack of support from health care professionals, and exorbitant medical bills, all while battling physically and mentally debilitating symptoms with no end in sight. This experience can lead to a drastic reduction in quality of life that creates the perfect conditions for mental illness.
Also Check: Is There A Rash With Lyme Disease
The Role Of Coinfections
Ticks carry more diseases than just Lyme and TBRF, and its not uncommon for patients to be infected with more than one type of disease-causing bacteria.
Common coinfections such as Babesiosis and Bartonellosis can not only cause neurological and psychiatric symptoms of their own, but they can also complicate the diagnostic process, delaying proper diagnosis and treatment all of which increase the risk of developing emotional, behavioral, or cognitive problems from the infection.
What Are The Symptoms Of Lyme Disease
Most children who develop Lyme disease do not recall having been bitten by a tick. Symptoms can appear a few days to many months after the bite, and can include:
- a rash in the form of a bulls-eye
- facial palsy, or weakness of the facial muscles
- headache/meningitis, or swelling of tissues around the brain and spinal cord
- fainting
- arthritis
- carditis
Children with a bulls-eye rash may also have systemic symptoms such as fever, fatigue, and joint aches. The rash may not have a classic bull-eye appearance, especially on people with darkly pigmented skin, and can be mistaken for cellulitis, ringworm, or other skin conditions. Children who develop a disseminated infection often have not had a preceding skin rash.
The most common late stage symptom of Lyme disease is arthritis, particularly in the large joints and especially the knee. Typically, the joints will be more swollen and tender than painful, and anti-inflammatory medicine can help.
Read Also: Post Treatment Lyme Disease Syndrome Mayo Clinic
Neurological Infections In Travelers/immigrants
Many infectious diseases that affect the nervous system can be acquired from other parts of the United States or other parts of the world. In the United States, several regional viruses and fungi can cause encephalitis and/or meningitis that individuals coming from endemic regions may have been exposed to. Worldwide, neurocysticercosis, poliomyelitis, malaria, schistosomiasis, rabies, chikungunya virus, dengue fever, leptospirosis, Tick-Borne encephalitis virus, cycloviruses, and melioidosis are some of the infections that can be acquired which affect the nervous system.
Diagnosing Lyme Disease In Dogs
In order to properly diagnose Lyme disease, vets will perform two types of blood tests that can indicate whether or not your dog is infected.
The antibody test will detect the presence of not just bacterium, but also specific antibodies that are formed in the dogs body in reaction of the bacterium. If the test comes back positive, then your dog has in fact been exposed to the bacterium. There is a possibility of it coming back as a false positive, though. This occurs when the dog doesnt have a high enough level of antibodies in their system. Therefore, the test is unable to pick up on them.
Another test that vets conduct is a polymerase chain reaction test, a specific DNA test that confirms the presence of the disease-causing bacteria. Unlike the first test, this test looks directly for the presence of disease-causing bacteria rather than just looking for antibodies.
Read Also: Lyme Disease And Lower Back Pain