Lyme Disease Test Two
Two-tiered Lyme disease testing uses two tests. The first is a screening test that should detect anyone who might have the disease. Tests that do this well have are regarded as having high sensitivity. This test is followed by a second test that is intended to make sure that only people with the disease are diagnosed. Tests that do this well have high specificity.
HIV/AIDS is diagnosed with tests that are both highly sensitive and highly specific. They are accurate more than 99% of the time. In Lyme disease, the second test is highly specific. So there are few false positives. Unfortunately, the screening test is highly insensitive and fails to accurately identify patients who have Lyme disease. The two-tiered test system misses roughly 54% of patients.
Because of this, LDo recommends the patients and physicians skip the ELISA and go straight to the Western blot.
Severity Of Lyme Disease
Misconception: B. burgdorferi infection is potentially lethal.
Science: Although Lyme disease can cause heart or brain abnormalities, there have been remarkably fewif anydeaths attributable to this infection.
LymeScience note: After this paper was published, the CDC three case studies of deaths associated with Lyme carditis, though two patients had preexisting heart conditions. While its not entirely clear if the infection caused the deaths, the CDC still reiterates, Prompt recognition and early, appropriate therapy for Lyme disease is essential.
What Is The Best Way To Remove A Tick And What If I Did Not Get The Entire Tick Out
The Centers for Disease Control provides this information about removing a tick: Remove a tick from your skin as soon as you notice it. Use fine-tipped tweezers to firmly grasp the tick very close to your skin. With a steady motion, pull the ticks body away from your skin. Then clean your skin with soap and warm water. Throw the dead tick away with your household trash. Avoid crushing the ticks body. Do not be alarmed if the ticks mouthparts remain in the skin. Once the mouthparts are removed from the rest of the tick, it can no longer transmit the Lyme disease bacteria. If you accidentally crush the tick, clean your skin with soap and warm water or alcohol. Dont use petroleum jelly, a hot match, nail polish, or other products to remove a tick. View a diagram of how to remove a tick.
Don’t Miss: Can You Get A Test For Lyme Disease
How Reliable Is A Lyme Disease Blood Test
Although the tests used to diagnose Lyme disease can be highly accurate, the timing with which they are conducted matters a great deal. When a person becomes infected with Lyme, it takes up to six weeks for their body to respond and create the appropriate antibodies to fight it off. In the two-step testing process that looks for these antibodies, detecting Lyme disease before the antibodies have had the chance to develop can be difficult, if not impossible. According to research, over 50% of cases are missed using this two-step process.
The PCR test used to detect Lyme disease bacteria itself is typically highly accurate however, it can also lead to false negatives in people who do have Lyme disease if its distribution is sparse within the body.
Read Also: Does Lyme Disease Go Away
How Accurate Are Lyme Disease Tests
Medically reviewed by Neka Miller, PhD on August 11, 2020. To give you technically accurate, evidence-based information, content published on the Everlywell blog is reviewed by credentialed professionals with expertise in medical and bioscience fields.
Interested in getting tested for Lyme disease and want to learn more about the testing process? Here, weâll cover several aspects of Lyme disease testing, including accuracy in the context of false negatives, different test types, and moreâso continue reading.
Check for Lyme disease from the convenience of home with the Everlywell at-home Lyme Disease Testâwhich includes both screening and confirmatory testing .
Read Also: Academic Rentals Old Lyme Ct
Read Also: How Is Lyme Disease Diagnosed In Humans
Lyme Igg/igm Antibody Serology
The IgG/IgM Antibody Serology test is an ELISA , which indicates the presence of both IgG and IgM antibodies to B. burgdorferi. IgM antibodies are present shortly after infection takes place. IgG antibodies often persist long after symptoms have disappeared. The presence of either IgG/IgM antibodies indicates exposure to Lyme-causing Borrelia, not the active disease. A positive or equivocal test must be confirmed by both IgG and IgM ImmunoBlots Blots.
Reference Range
Lyme Disease Diagnosis And Testing Highlights
- LLMDS consider the specificity of the particular bands that test positive for a patient.
- Although the CDC requires 5 of 10 bands for IgG surveillance purposes, 2 of 5 bands have specificity of 93-96% and a sensitivity of 100%. .
- 56% of patients with Lyme disease test negative using the two-tiered testing system recommended by the CDC.
- The CDC case surveillance definition allows single-tier IgG immunoblot seropositivity using established criteria.
- The CDC states: This surveillance case definition was developed for national reporting of Lyme disease it is not intended to be used in clinical diagnosis.
- The College of American Pathologists found that ELISA tests do not have adequate sensitivity to be used for screening purposes.
- 52% of patients with chronic disease are negative by ELISA but positive by Western blot.
You May Like: Lyme Disease When To See A Doctor
More About Western Blot Testing In North America
The IgG Western Blot test is designed to detect antibodies specific to Borrelia burgdorferi, the bacteria that cause Lyme disease. For Lyme disease in North America, a positive IgG Western Blot test requires at least 5 of 10 measured bands to be positive .
The scored IgG bands are 18 kDa, 24 kDa , 28 kDa, 30 kDa, 39 kDa , 41 kDa flagellin , 45 kDa, 58 kDa , 66 kDa, and 93 kDa.
The Lyme IgM Western Blot test measures 3 different types of antibodies. The North American IgM Western Blot is considered positive only if 2 of 3 IgM bands are positive .
The scored IgM bands are 24 kDa , 39 kDa , and 41 kDa .
According to the CDC, Depending upon the assay, OspC could be indicated by a band of 21, 22, 23, 24 or 25 kDA.
Elisa And Western Blot
The first part of the ELISA test acts as a preliminary investigation to see if further testing is needed. A negative result typically warrants no further testing, but a positive one does. The first test is highly sensitive and the second highly specific. This makes sure that only people with Lyme disease are diagnosed and treated.
The Western blot test is a type of blood test that aims to single out certain proteins known as antigens. It is used to identify an active infection of Lyme disease. Although sometimes accurate, however, this test is inherently flawed because methods and criteria for interpreting results can change from lab to lab.
Recommended Reading: Do You Always Have A Rash With Lyme Disease
Don’t Miss: How To Interpret Lyme Test Results
What Abnormal Results Mean
A positive ELISA result is abnormal. This means antibodies were seen in your blood sample. But, this does not confirm a diagnosis of Lyme disease. A positive ELISA result must be followed up with a Western blot test. Only a positive Western blot test can confirm the diagnosis of Lyme disease.
For many people, the ELISA test remains positive, even after they have been treated for Lyme disease and no longer have symptoms.
A positive ELISA test may also occur with certain diseases not related to Lyme disease, such as rheumatoid arthritis.
How Do I Know Whether I Have Received A Sufficiently Long Course Of Antibiotic Therapy
Taken together, these study results suggest that repeated antibiotic therapy may be beneficial for a subgroup of patients. However all of these studies also reported troubling adverse effects associated with the IV antibiotic therapy. Given these potentially dangerous risks, it is clear that other safer and more durable treatments are needed for patients with persistent symptoms.
Also Check: Treatment For Lyme Disease Years Later
Don’t Miss: What Are The Side Effects Of Lyme Disease In Humans
Is There A Lyme Disease Test Kit
Blood collection kits are available for at-home Lyme disease testing. Lyme disease test kits can cost as less as $20 and as much as $100 or more. Using a Lyme disease test kit is as simple as pricking your finger and smearing or collecting the blood onto the kit for testing.
However, testing for Lyme disease in a more controlled environment such as a lab or clinic is preferable as qualified healthcare professionals are likely to perform a more reliable test.
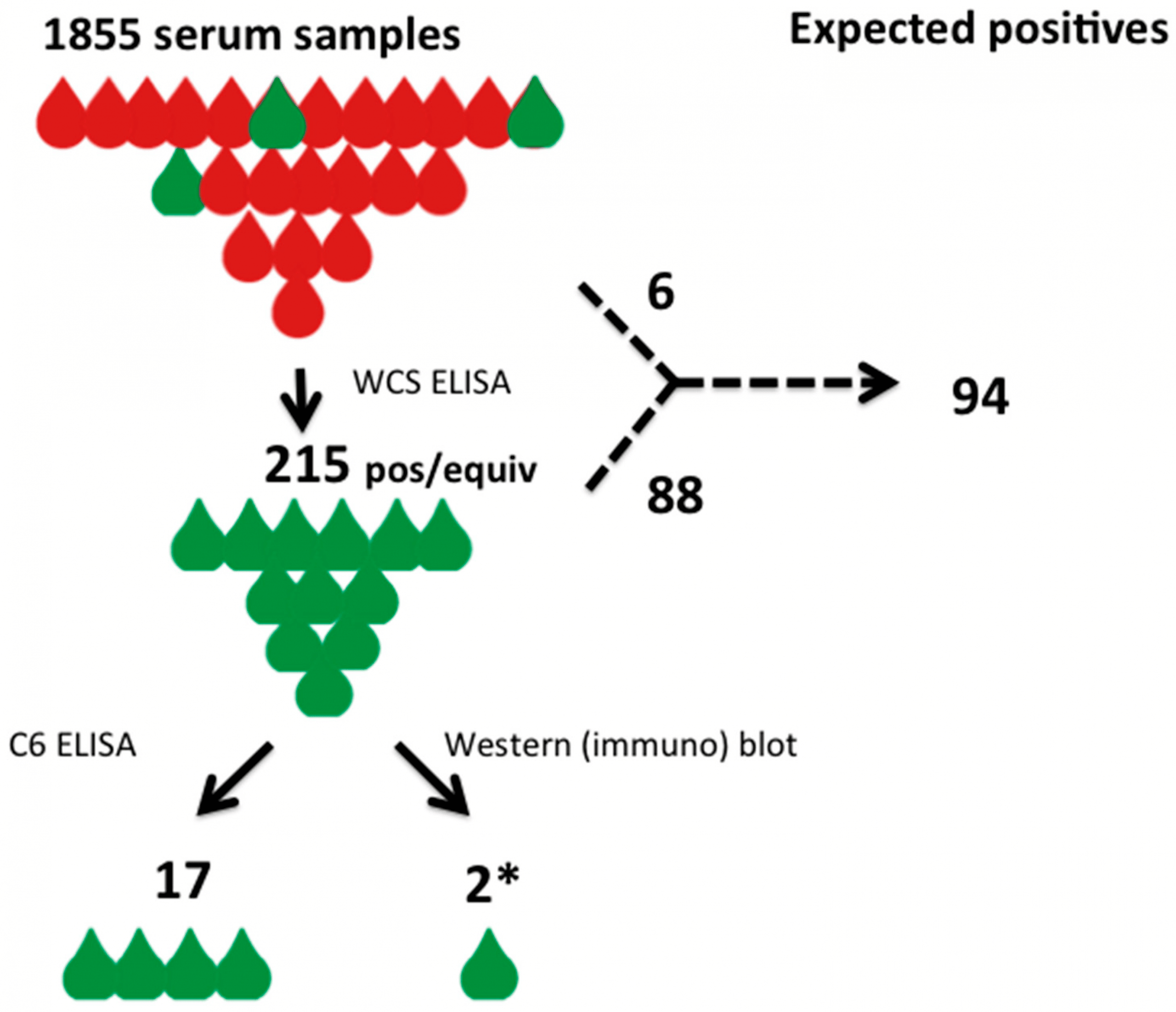
Waddell L. A., et al. . The accuracy of diagnostic tests for Lyme disease in humans, a systematic review and meta-analysis of North American research. PLoS One. 2016 11: e0168613. Retrieved from
Why It Is Done
A Lyme disease test is done to diagnose Lyme disease in people who have symptoms of Lyme disease. Symptoms may include:
- An expanding red rash with a pale center. This is sometimes called a “bull’s-eye” rash.
- Extreme tiredness.
- Headache and stiff neck.
- Muscle and joint pain.
Symptoms of chronic Lyme disease infection include joint pain, stiffness, and problems with the heart, brain, or nerves.
Testing is most accurate when you have risk factors for Lyme disease or symptoms of the disease.
You May Like: Houses For Sale In East Lyme Ct
How Is Lyme Disease Diagnosed
An EM rash is a sure sign of Lyme disease, so your doctor can diagnose and treat you without the need for laboratory tests.
An EM rash, often shaped like a bullseye , is a sure sign of Lyme disease. If you develop an EM rash, you should be diagnosed & treated for Lyme disease without the need for further lab tests. EM rashes are not as obvious on darker skin .
For all other cases, your doctor should consider whether your symptoms and risk factors point to a Lyme disease diagnosis. For example:
-
Were you bitten by a tick?
-
Did you spend time outdoors in an area where Lyme disease is common?
-
Recent travel: Lyme disease may be common where you were, even if it is unusual where you live.
-
Your current symptoms and how long have they been present.
-
Your full medical history, including previous unexplained symptoms that may help lead to an accurate diagnosis whether that ends up being Lyme or another condition.
I Am Wondering If Columbia University Uses Xenodiagnosis For Detection Of Infectious Diseases
This is an interesting question. Xenodiagnosis in this case refers to allowing an uninfected tick to feed on an individual with suspected infection to see whether the tick is able to suck up spirochetes when the spirochetes might not have been detectable otherwise. As strange as this concept appears, it has been used successfully recently by Dr. Steven Barthold at UC Davis. After being unable to identify persistent infection in a treated infected mouse using the standard PCR and culture techniques, he was then able to identify the spirochetes in these mice after treatment using the xenodiagnosis method. We at Columbia are not using this method on humans. This is a very intriguing scientific question that should be studied in humans.
The Centers for Disease Control publishes national statistics and identifies those counties with the highest rates of Lyme disease in the United States. The web sites of many state health departments provide data on Lyme disease by town of residence.
Support groups can be found by calling the Lyme clinics or Lyme disease organizations in your state. You might also call a national organization, such as the Lyme Disease Association for the names of support groups in your area.
Dont Miss: Can Lyme Disease Cause Weight Gain
Don’t Miss: Cost Of Iv Antibiotics For Lyme Disease
How Do Doctors Test For Lyme Disease
Lyme disease is typically assessed based on clinical diagnosis, in combination with laboratory tests. There is much debate over the accuracy and reliability of the laboratory tests and the likelihood of false positives and false negatives. The following tests are FDA-approved for diagnosis:
- The Enzyme-linked immunosorbent assay or ELISA is the first step. This test detects antibodies to B. burgdorferi and, if positive, is followed up by the Western Blot test.
- The western blot is usually run as a second-stage to confirm the diagnosis following a positive ELISA result. The Western blot detects antibodies to several proteins of B. burgdorferi. Together these tests are known as the ELISA/Western Blot.
- Alternatively, the polymerase chain reaction is a highly sensitive test that detects DNA from the Borrelia bacteria in fluid drawn from an infected joint . It is much less commonly used as the bacteria are most likely to bind to joint and nerve tissues and more difficult to detect.
For more on the Lyme testing process as defined by the CDC, check out this flow chart.
The Most Common Lyme Disease Blood Tests
The two most common diagnostic tests for Lyme disease are the enzyme-linked immunosorbent assay and the Western blot. These Lyme disease tests allow physicians to visualize the reaction between antibodies in an infected persons blood to specific antigens or parts of the bacteria that cause Lyme disease.
In the case of the Western blot, for example, antigens are separated by size and then transferred onto a membrane strip. When an antibody reacts with an antigen on the strip, that band will turn dark purple. For test results to be positive, a specific combination of bands on the membrane strip must be present.
Also Check: Is There A Test For Lyme Disease
What The Experts Say
According to the CDC:
- Patients who have had Lyme disease for longer than 4-6 weeks, especially those with later stages of illness involving the brain or the joints, will almost always test positive.
- A patient who has been ill for months or years and has a negative test almost certainly does not have Lyme disease as the cause of their symptoms.
- Serologic testing is generally not useful or recommended for patients with single EM rashes. For this manifestation, a clinical diagnosis is recommended.
Experts around the world agree with the CDC. A 2018 French review of 16 Lyme diagnostic guidelines from 7 countries revealed a global consensus regarding diagnosis at each stage of the infection. The only outlier was the pseudoscience group German Borreliosis Society , a German counterpart to the pseudoscience group ILADS.
Also Check: How To Test For Lyme Disease Years Later
Other Lyme Disease Tests
Three other tests that may be used to diagnose Lyme disease are polymerase chain reaction , antigen detection and culture testing. They are called direct tests because they detect the bacteria, not just your immune response to it.
PCR multiplies a key portion of DNA from the Lyme bacteria so that it can be detected. While PCR is highly accurate when the Lyme DNA is detected, it produces many false negatives. This is because the Lyme bacteria are sparse and may not be in the sample tested.
Antigen detection tests look for a unique Lyme protein in fluid . Sometimes people whose indirect tests are negative are positive on this test.
Culture is the gold standard test for identifying bacteria. The lab takes a sample of blood or other fluid from the patient and attempts to grow Lyme spirochetes in a special medium.
Although culture tests are generally accepted as proof of infection, the CDC has advised caution on the only commercially available culture test developed by Advanced Laboratory Services. LDo recognizes that the test is new and requires further validation in other studies. However, we believe that informed patients should be able to choose the test if they prefer. Choice is particularly important given the low quality of Lyme disease tests generally.
Read Also: What To Do If You Have Lyme Disease
What Is On The Horizon For Lyme Testing
Because Lyme bacteria are not usually present in high enough numbers to be detectable, blood tests to look for Borrelia are not helpful.
Better diagnostic tests are needed that are direct and can detect infection at all stages of Lyme disease. Researchers are studying new diagnostic methods using better antibody tests, direct detection methods, and different ways to measure immune response to Lyme disease.
Lyme Disease Is Remarkably Difficult To Diagnose

The problem with Lyme disease is that the bacteria can create a hard shell around themselves when inactive so that the blood tests are unable to detect them. This is especially true when the disease has reached the chronic stage. The timing of the symptoms is often used by a medical provider to establish a time line to a tick bite or exposure to a high-risk region where the disease is commonly transmitted.
Because the ticks that can spread Lyme disease are often the size of a pinhead, the ticks might not even be notice. A bulls-eye rash at the bite location is a trademark symptom of Lyme disease, but only about half of the people who are infected with the bacteria develop the rash. Once the disease reaches the chronic stage, chronic arthritis, joint pain, and neurological symptoms begin to appear, sometimes several months after the infection.
Read Also: Hyperbaric Treatment For Lyme Disease
You May Like: Can You Die From Lyme Disease
Diagnostic Test Performance In Early Lyme Disease
Testing for LD in patients exhibiting signs and symptoms of LD for less than 30 days is challenging as the performance of available test protocols is not optimal for making clinical decisions. This is largely due to the time required for the infected individuals immune system to mount a reaction. This is why researchers have explored the use of a variety of targets including VlsE and C6 expressed after infection, Osp C and Fla B expressed by the feeding tick to detect infection sooner . However, cross-reactivity and genetic variability within the targets has limited the diagnostic performance of any single target . Thus the results of expected sensitivities and specificities in Table 8 emphasize the importance of physician evaluation and informed judgement when deciding to treat rather than rely entirely on imperfect serological test protocols. Notable findings in the table include the higher specificity associated with the two-tier testing method and the poor and highly variable sensitivity of serological tests in the initial stages of disease when an individual is mounting an immune response to B. burgdorferi.