New Cdc/fda Warning Against Unapproved Lyme Culture Test
Concerns about the purported Borrelia burgdorferi culture test marketed by Advanced Laboratory Services resulted this week in a blunt warning published in the Centers for Disease Control and Prevention’s Morbidity and Mortality Weekly Report, advising use only of the 83 FDA-approved tests for diagnosis of Lyme disease.
“The Advanced Laboratory Services example highlights the problem of using tests that are unvalidated and not -approved for diagnosing Lyme disease. We would caution clinicians and patients against the use of any unapproved tests,” lead author Christina Nelson, MD, told Medscape Medical News. Dr. Nelson is from the CDC’s Division of Vector-Borne Diseases, Fort Collins, Colorado. Study coauthors include Sally Hojvat, PhD, director of the FDA’s Division of Microbiology Devices.
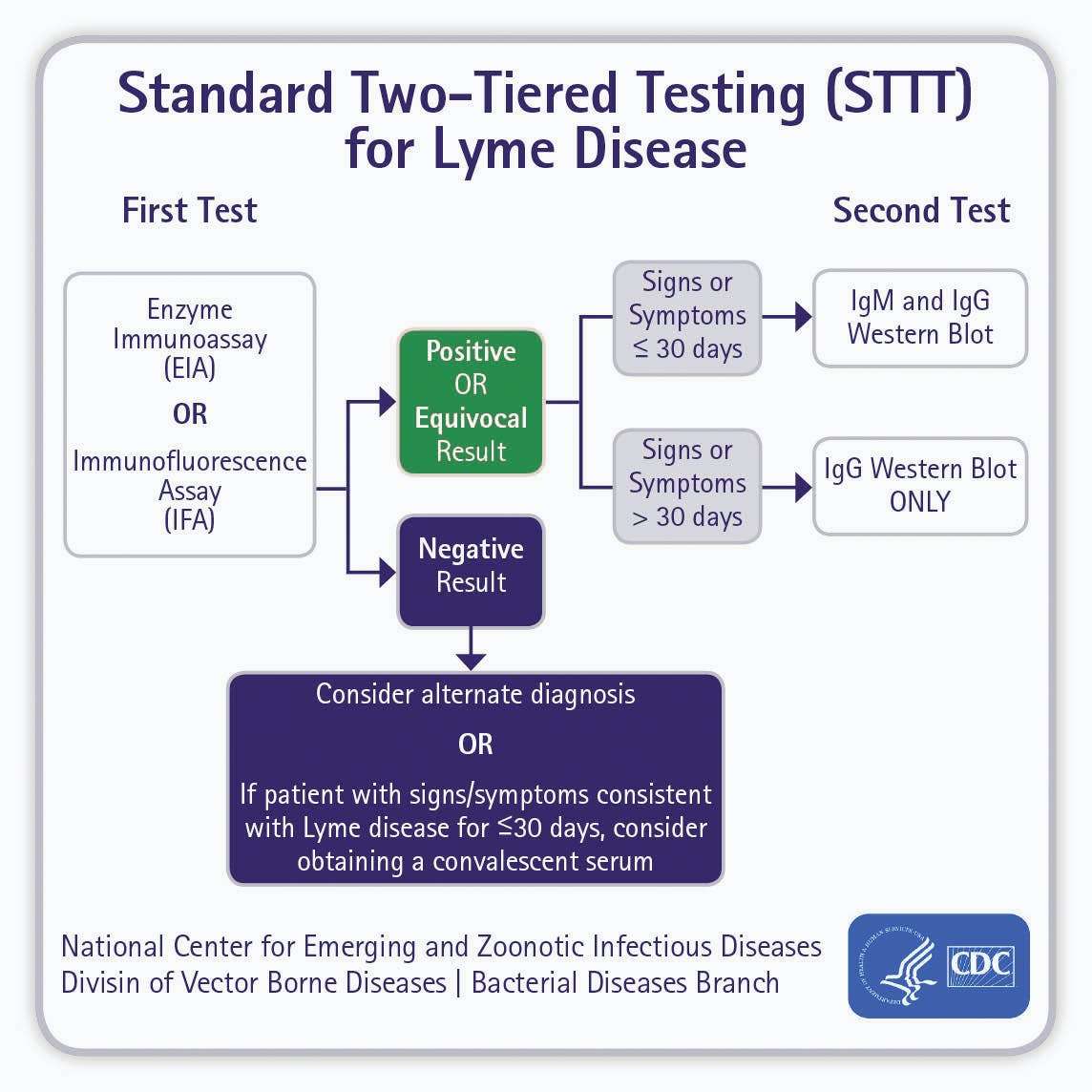
Dr. Nelson emphasized that for Lyme disease diagnosis, the CDC recommends a 2-step process of serologic testing: first, an FDA-cleared enzyme immunoassay, followed in immunoassay-positive or equivocal cases by confirmatory Western blot. Only patients positive on both tests are considered to have Lyme disease. B burgdorferi culture is notoriously difficult and recommended only in rare circumstances, primarily in research settings and for patients with early Lyme borreliosis, atypical rash, and no history of antibiotic treatment, which rapidly aborts culture positivity.
The authors have disclosed no relevant financial relationships.
Morb Mortal Wkly Rep. 2014 63 333. Full text
Cdc Supports The Development Of New Tests
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
When Should I Get A Lyme Disease Test
Lyme disease testing is only recommended under certain circumstances. In general, antibody tests are conducted when you have symptoms of Lyme disease and a confirmed or likely exposure to ticks that are known to carry Borrelia. In these cases, the timing of testing is important. Because antibodies may not form for a few weeks, testing soon after a tick bite or development of a skin rash may cause misleading results.
Antibody testing is not advised if you do not have symptoms of Lyme disease, including for people who live in areas that are confirmed to have the types of ticks that can transmit Borrelia. Testing is also not recommended if you have general symptoms, such as joint pain, but no likely exposure to Borrelia-carrying ticks.
If you have had a tick bite and/or symptoms of Lyme disease, you should talk with your doctor who can address whether Lyme disease antibody testing is appropriate in your situation.
You May Like: Lyme Disease Doctors In Virginia
Other Diagnostic Tests For Lyme Disease
Some laboratories offer Lyme disease testing using urine or other body fluids. These tests are not approved by FDA because they have not been proven to be accurate. For example, one study of urine-based polymerase chain reaction assays for Lyme disease diagnosis showed that with currently available tools, urine cannot be used to accurately diagnose Lyme disease. Another study by NIAID-supported scientists showed that the Lyme Urinary Antigen Test was unreliable and resulted in excessive numbers of false positives. In the same study, researchers confirmed that an ELISA followed by a Western blot test was nearly 100 percent reliable in diagnosing Lyme disease. With the availability of so many Lyme disease tests, including non-commercial tests developed by individual facilities, it is impossible to address the accuracy of each one. The development of new, rapid, clearly validated diagnostic tests continues to be a need.
Is There A Blood Test For Lyme Disease
If your doctor suspects that you have Lyme disease, they may order two blood tests. These will look for signs that your body is trying to fight it off. The results are most precise a few weeks after youâve been infected.
These tests are:
ELISA test. This test canât check for the bacteria that causes Lyme disease. It can only look for your immune systemâs response to it.
Once Borrelia burgdorferi gets into your blood, your body begins to make special proteins called antibodies to fight it off. The ELISA test checks for those antibodies.
Although itâs the most common way to check for Lyme disease, the ELISA test isnât perfect. It can sometimes give false âpositiveâ results. On the other hand, if you have it done too soon after youâve been infected, your body may not have developed enough antibodies for the test to detect them. This will give you a ânegativeâ result even though you do have Lyme disease.
Western blot test. Whether your ELISA test comes back positive or negative, your doctor will need to do this blood test, too.
A Western blot uses electricity to split certain proteins in your blood into patterns. This is then compared to the pattern of people known to have Lyme disease.
At least five band matches means that you have Lyme disease. Still, not all labs have the same standards. Thereâs a chance that you could get a âpositiveâ result from one and a ânegativeâ result from another.
- Alzheimerâs disease
Read Also: Do I Have Ms Or Lyme Disease
Fda Clears New Indications For Lyme Disease Tests
The FDA reviewed data from clinical studies of the Zeus ELISA Borrelia VlsE1/pepC10 IgG/IgM Test System, Zeus ELISA Borrelia burgdorferi IgG/IgM Test System, Zeus ELISA Borrelia burgdorferi IgM Test System, and the Zeus ELISA Borrelia burgdorferi IgG Test System that showed the modified two-tier test is as accurate as current methods for detecting antibodies for assessing exposure to Borrelia burgdorferi.
The FDA granted 510 clearance of the tests to Zeus Scientific.
The Diagnostic Accuracy Of Tests Compared To Clinical Diagnosis
Two-tier serological test vs. clinical diagnosis
Thirteen studies evaluated the two-tier serological test protocol for diagnosis of LD at different stages of disease and after antibiotic therapy. provides the meta-analytic summaries demonstrating low sensitivity, 46.3% , for early LD patients and increasing sensitivity with stage 2, 89.7% , and stage 3, 99.4%H LD. There was relatively high specificity across control groups. Most false positives within the control groups were patients with diseases known to produce antibodies that cross-react in serological tests for B. burgdorferi. Nine studies presented results for two-tier serological testing where at least one of the tests was not FDA licensed , . Heterogeneity analysis of sensitivity and specificity on the impact of using non-commercial tests was not significant. At the early stage of LD the two-tier testing method was good for ruling in LD if the patient tested positive, but had very poor predictive value for ruling out LD, which is why it is recommended to retest after 30 days . However, for convalescent patients treated at stage 1 LD sensitivity remained low even after 30 days.
Also Check: Can You Donate Plasma If You Have Lyme Disease
Diagnostic Test Performance In Early Lyme Disease
Testing for LD in patients exhibiting signs and symptoms of LD for less than 30 days is challenging as the performance of available test protocols is not optimal for making clinical decisions. This is largely due to the time required for the infected individuals immune system to mount a reaction. This is why researchers have explored the use of a variety of targets including VlsE and C6 expressed after infection, Osp C and Fla B expressed by the feeding tick to detect infection sooner . However, cross-reactivity and genetic variability within the targets has limited the diagnostic performance of any single target . Thus the results of expected sensitivities and specificities in emphasize the importance of physician evaluation and informed judgement when deciding to treat rather than rely entirely on imperfect serological test protocols. Notable findings in the table include the higher specificity associated with the two-tier testing method and the poor and highly variable sensitivity of serological tests in the initial stages of disease when an individual is mounting an immune response to B. burgdorferi.
Lymepolicywonk: The Cdc The Fda And Lyme Disease Lab Tests
Yesterday, the CDC officially announced that it recommends that laboratory tests cleared or approved by FDA be used to aid in the routine diagnosis of Lyme disease. This is a shame. Waiting for FDA approval suppresses innovation in Lyme testing and furthers the interests of those who have vested interests in the current flawed lab tests which miss as many cases as they detect. Neither of these is good for patients.
This announcement, while official, is not unexpected. Last year, the CDC amended its website to state that before the CDC will recommend new tests, their performance must be demonstrated to be equal to or better than the results of the existing procedure, and they must be FDA approved.
The CDC does not have jurisdiction over the FDA, of course. And, the FDA permits the marketing of tests that do not have FDA approval. Many tests on the market today fall in this category. What the announcement means is that physicians and insurers will be less likely to accept non-FDA approved tests. This means that patients who want these tests will need to pay for them out of pocket. It also means that the entrenched lab tests that simply do not work will have more of the market to themselves.
This does not help patients. It does not protect patients. It protects vested commercial interests who currently market test that are highly insensitive. It also undermines any incentive they might have to improve their testing by protecting them from competition.
Bibliography:
Also Check: Best Infrared Sauna For Lyme Disease
Notice To Readers: Caution Regarding Testing For Lyme Disease
CDC and the Food and Drug Administration have become aware of commercial laboratories that conduct testing for Lyme disease by using assays whose accuracy and clinical usefulness have not been adequately established. These tests include urine antigen tests, immunofluorescent staining for cell wall–deficient forms of Borrelia burgdorferi, and lymphocyte transformation tests. In addition, some laboratories perform polymerase chain reaction tests for B. burgdorferi DNA on inappropriate specimens such as blood and urine or interpret Western blots using criteria that have not been validated and published in peer-reviewed scientific literature. These inadequately validated tests and criteria also are being used to evaluate patients in Canada and Europe, according to reports from the National Microbiology Laboratory, Public Health Agency of Canada the British Columbia Centres for Disease Control, Canada the German National Reference Center for Borreliae and the Health Protection Agency Lyme Borreliosis Unit of the United Kingdom.
Health-care providers are reminded that a diagnosis of Lyme disease should be made after evaluation of a patient’s clinical presentation and risk for exposure to infected ticks, and, if indicated, after the use of validated laboratory tests. Patients are encouraged to ask their physicians whether their testing for Lyme disease was performed using validated methods and whether results were interpreted using appropriate guidelines.
New Two Step Test For Lyme Claims Improvement Over The Standard Test
SCARBOROUGH, Maine The Centers for Disease Control estimates that up to 300,000 people have Lyme Disease, but only a fraction, 30-thousand cases are actually reported every year.
That highlights a significant problem — some experts report say the standardized test used by the majority of providers and insurance companies is flawed and is accurate less than 50 percent of the time.
But a new Lyme testing method, developed by Zeus Scientific, claims to be far more precise in detecting the disease, especially in the early stages.
In studies, the new two-step test approved by the FDA showed a marked improvement in picking up a person’s immune response against the disease, within the first month of infection. That’s when Lyme can be successfully treated but left untreated can lead to years of lingering symptoms.
For 25 years its the only standardized test for Lyme disease recommended by the CDC. But it is often unreliable in catching the disease early because a patient’s immune response may not be detectable.
Dr. Sean McCloy is a medical doctor who diagnoses and treats patients for Lyme and tick borne illness.
“If clinicians are over-reliant on waiting for that positive result to come along, they may miss the diagnosis,” McCloy said.
The process involves a two-step blood test. The first test is the ‘ELISA’ followed by the ‘Western Blot.’ Both must be positive to indicate a diagnosis of Lyme disease.
NEWS CENTER Maine Tick Cover
Don’t Miss: Sleep Inn East Lyme Ct
Lyme Disease Test Two
Two-tiered Lyme disease testing uses two tests. The first is a screening test that should detect anyone who might have the disease. Tests that do this well have are regarded as having high sensitivity. This test is followed by a second test that is intended to make sure that only people with the disease are diagnosed. Tests that do this well have high specificity.
HIV/AIDS is diagnosed with tests that are both highly sensitive and highly specific. They are accurate more than 99% of the time. In Lyme disease, the second test is highly specific. So there are few false positives. Unfortunately, the screening test is highly insensitive and fails to accurately identify patients who have Lyme disease. The two-tiered test system misses roughly 54% of patients.
Because of this, LDo recommends the patients and physicians skip the ELISA and go straight to the Western blot.
Lyme Disease Diagnostics Research
There is a great need to develop rapid, point-of-care tests to determine whether people are infected with Borrelia burgdorferi, the bacterium that causes Lyme disease. NIAID is committed to improving Lyme disease diagnostics by supporting innovative research projects.
Priorities include finding potential targetssubstances that new diagnostic tools might measure in patient samplesand improving the sensitivity and specificity of currently available diagnostic tests, thereby leading to more accurate results.
Read Also: What Symptoms Does Lyme Disease Cause
Lymepolicywonk: Whose Interests Is The Fda Protecting Not Lyme Patients Apparently
On July 31, the FDA announced it would move forward with regulations to restrict cutting edge laboratory developed tests , which have not required FDA approval before because they are not marketed to consumers. The new regulations would change that. Why should you care?
Because LDTs include the Lyme tests manufactured by IGeneX and Advanced Laboratory Services that many patients rely on for accurate diagnosis.
The FDAs announcement came on the heels of a July 2014 letter sent by five U.S. Senators to the budget office, urging action on the FDAs draft guidance, which has been under review for several years. The letter specifically calls out Lyme disease testing.
Recently, the Centers for Disease Control and Prevention reviewed a frequently utilized LDT to detect Lyme disease and found serious concerns about false-positive results and misdiagnosis. The CDC recommended that the diagnosis of Lyme disease should instead be left to tests approved by the FDA.
I am deeply concerned that Senator Blumenthal D-CT, who supported the Connecticut antitrust action against the IDSA, is one of the five Senators who signed the letter. The other four are Sen. Edward Markey D-MA Sen. Elizabeth Warren D-MA Sen. Sherrod Brown D-OH and Sen. Richard Durbin D-IL.
Whats so bad about requiring FDA approval for Lyme tests?
The public comment period for the proposed regulation will open in October. We hope you have your pen handy. We will keep you informed of on-going developments.
What Precautions Can I Take Against Tick Bites
- Avoid wooded, brushy, and grassy areas, especially in May, June, and July.
- Wear light-colored clothing so that you can see ticks that get on you.
- Wear long pants and long-sleeved shirts, and shoes that cover the entire foot.
- Tuck pant legs into socks or shoes, and tuck shirts into pants.
- Wear a hat for extra protection.
- Spray insect repellent containing DEET on clothes and uncovered skin.
- Walk in the center of trails to avoid brush and grass.
- Remove your clothing, and wash and dry them at high temperatures after being outdoors.
- Do a careful body check for ticks after outdoor activities.
Read Also: Claritin Protocol For Lyme Disease
Lyme Disease Test And Treatment
If you think you may have Lyme disease, contact your physician right away.
Your doctor may do a test for Lyme disease. The FDA regulates diagnostic tests to ensure that they are safe and effective. Its important to know that blood tests that check for antibodies to the bacterium that causes Lyme disease are not useful if done soon after a tick bite. It typically takes 2 to 5 weeks after a tick bite for initial antibodies to develop.
For this reason, your doctor may recommend treatment with antibiotics before the diagnostic tests are complete. According to the CDC, patients treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely.
What Is Lyme Disease
Lyme disease is an illness caused by infection with a bacteria that is spread through the bite of certain kinds of ticks. Symptoms can affect the skin where the bite occurred or elsewhere on the skin and may progress to affect other parts of the body. A family of bacteria, known as Borrelia, causes Lyme disease.
Don’t Miss: How Long Does It Take To Get Lyme Disease
Modified Lyme Disease Testing Process Improves Early Diagnosis
This page was fact checked by our expert Medical Review Board for accuracy and objectivity. Read more about our editorial policy and review process.
The U.S. Food and Drug Administration recently cleared the expanded use of four current Lyme disease tests, allowing these assays to be used in specific combinations for detecting and confirming the illness. The new modified testing protocol eliminates the need to run a specialized test called an immunoblot . Ultimately, this change is anticipated to simplify the interpretation of Lyme disease test results and provide improved detection of Lyme disease earlier on following infection.
Lyme disease is primarily caused by infection with the bacteria Borrelia burgdorferi in the United States and other closely related Borrelia species found throughout Europe and Asia. The disease is spread to humans following a bite from an infected black-legged tick. Transmission of the bacteria from the tick to a human requires at least 36 hours of tick attachment. Signs and symptoms of the illness include fever, headache, and fatigue and may include a bulls-eye rash that develops at the site of the tick bite.
The traditional testing process for Lyme disease has been in place since 1995 and requires two different lab testing methods. Both methods look for the presence of antibodies in the blood that are produced by the immune system in response to the infection.