Why Lyme Is Tough To Diagnose
- Lyme symptoms are similar to other illnesses, so misdiagnosis is common.
- Many Canadian doctors are unfamiliar with Lyme, so they dont test for it or administer the wrong tests.
- Only a handful of blood tests effectively detect Lyme bacteria, so the infection is often missed.
Dont get discouraged if you get a negative diagnosis. Seek out second, and even third, opinions if you must!
Other Infections Associated With Tick Bites
Ticks can carry a number of other bacterial and viral infectious agents, sometimes at the same time as the Lyme disease organisms. In the eastern part of the United States, babesiosis and ehrlichiosis may occur independently or with Lyme disease after tick bites.
Transmission of more than one agent in Europe and the UK is rare, with only a handful of cases reported with definite evidence of co-infection.
In other parts of the world, viruses such as tick borne encephalitis virus can cause infections that may be mistaken for Lyme disease. Depending on where the patient was exposed, other infections may also give rise to symptoms similar to Lyme disease.
Persistence Of The Clinical Manifestations After Treatment
The persistence of symptoms related to LB can be observed in untreated patients as well as in patients who have undergone treatment but continue to present symptoms. Untreated patients can develop persistent signs and symptoms, which usually involve the joints and less commonly the nervous system . Patients who instead have been treated mainly report a worsening of subjective symptoms. After 6 months, 36% of patients experienced an increase in fatigue, 20% complained of widespread pain, and 45% of neurocognitive impairment . Long-term persistent illness following antibiotic treatment is not uncommon, especially when treatment is delayed. About 1020% of patients treated for early or late LB experience persistent symptoms, which may last for months or years . Symptoms consist of fatigue, joint and muscle pains, recent cognitive disorders, root pain, paresthesia, or dysesthesia. If we analyze the group of patients treated for Neuroborreliosis, this percentage increases significantly. Eikeland found that in Europe only 56% of patients treated with antibiotics for neuroborreliosis were symptom-free 30 months after treatment .
Some published authors of medical research recognize mainly two clinical scenarios: the first characterized by typical symptoms of post-Lyme disease when symptoms persist for < 6 months, and post-treatment Lyme disease syndrome or chronic Lyme disease if symptoms are debilitating and persist after treatment .
Don’t Miss: Foods That Kill Lyme Disease
How You Get Lyme Disease
If a tick bites an animal carrying the bacteria that cause Lyme disease, the tick can become infected. The tick can then transfer the bacteria to a human by biting them.
Ticks can be found in any areas with deep or overgrown plants where they have access to animals to feed on.
They’re common in woodland and moorland areas, but can also be found in gardens or parks.
Ticks don’t jump or fly. They climb on to your clothes or skin if you brush against something they’re on. They then bite into the skin and start to feed on your blood.
Generally, you’re more likely to become infected if the tick is attached to your skin for more than 24 hours. Ticks are very small and their bites are not painful, so you may not realise you have one attached to your skin.
How Is It Diagnosed
If youâve been outside in an area where ticks are known to live, you should tell your doctor. Theyâll also want to know about the symptoms youâre having. These details are crucial to making a diagnosis of Lyme disease.
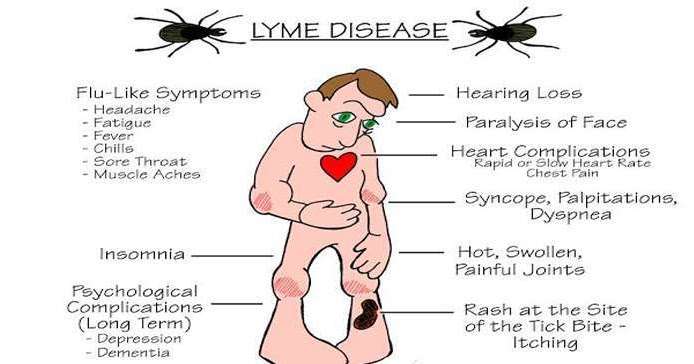
Early symptoms that usually occur within the first month after a tick bite can include:
- Rash at the site of the tick bite that may look like a âbullâs-eyeâ
- Racing heart
- Problems with your short-term memory
Symptoms that come and go are common with Lyme disease. They will also depend on the stage of the disease.
Recommended Reading: Do Ticks In Florida Carry Lyme Disease
Late Lyme Disease Symptoms
What Are The Stages Of Lyme Infection
There are three stages:
- Early localized Lyme: Flu-like symptoms like fever, chills, headache, swollen lymph nodes, sore throat, and a rash that looks like a bull’s-eye or is round and red and at least 2 inches long
- Early disseminated Lyme: Flu-like symptoms like pain, weakness, or numbness in your arms and legs, changes in your vision, heart palpitations and chest pain, a rash , and a type of facial paralysis known as Bellâs palsy
- Late disseminated Lyme: This can happen weeks, months, or years after the tick bite. Symptoms might include arthritis, severe fatigue and headaches, dizziness, trouble sleeping, and confusion.
About 10% of people treated for Lyme infection donât shake the disease. They may go on to have three core symptoms: joint or muscle pain, fatigue, and short-term memory loss or confusion. This is called post-treatment Lyme disease syndrome. It can be hard to diagnose because it has the same symptoms as other diseases. Plus, there isn’t a blood test to confirm it.
Experts arenât sure why Lyme symptoms donât always go away. One theory is that your body keeps fighting the infection even after the bacteria are gone, like an autoimmune disorder.
You May Like: Lyme Disease Specialist San Francisco Bay Area
Managing Lyme Symptoms From Home
Heather Lowery is a physician assistant at NYCIM and a former Lyme disease patient. Drawing from her own journey with neurological Lyme disease, Heather shares some tips and treatments to address the physical, mental, emotional, and spiritual trials that arise when battling Lyme disease.
According to Heather, Lyme disease is characterized by two steps forward and one step back. And as symptoms subside and then return, it is important to not dwell on them or view them as a defeat. Participating in activities that spark joy and passion can help deal with the emotional roller coaster that is Lyme disease.
Antibiotics Cant Kill Parasites
Lyme bacteria love to hide inside parasites. Just like you, parasites have a microbiota. You may have a mix of good and bad microbes in your gut. But parasites are a Pandoras box of terrible microbes one being Lyme.
Even if you get rid of Lyme in the rest of your body, the bacteria hiding in parasites can reinfect you. This is why the disease may come back, despite long and intense antibiotic treatment. But the Lyme inside the parasites is protected and will reinfect the host. It may be impossible to conquer Lyme without getting rid of the Lyme carrying parasites because it’s addressing the infection in the wrong order.
Antibiotics also do not always travel past the blood/brain barrier. If the Lyme disease bacteria have settled there, they may not be affected at all.
You May Like: Testing For Lyme Disease In Humans
Autoimmune Symptoms And Conditions
Its one thing for Borrelia burgdorferi to attack you. Its a whole new ball game if your own immune system attacks your tissues because of them. Thats an autoimmune disease. Examples are rheumatoid arthritis and multiple sclerosis .
The bacteria do whatever they can to protect themselves from your immune system. They have learned to hide in your cells. This makes your immune system soldiers suspicious. They think, This isnt right. I need to get rid of this cell.
This happens because some of the proteins in the bacteria look like your own. Your immune system starts to view healthy cells as foreign invaders. It attacks them to get rid of the Lyme.
This problem can escalate to rheumatoid arthritis. In this condition, your body attempts to stomp out joint cells where the bacteria live. You may be told you have RA, but chronic Lyme disease is at the root of it.
Heres another problem. Proteins in the tail of the bacteria look like the cells of your myelin sheath. These are the cells that cover and insulate your nerves. So, the bacteria can trick your immune system into attacking your healthy myelin cells.
The microbes also release enzymes that block your bodys ability to regenerate the myelin. Without this protective nerve covering, you may get inflammation and intense pain.
This process looks exactly like multiple sclerosis. Chronic Lyme disease may sneak under the radar once again, and your doctor may diagnose you with MS.
Notice To Readersrecommendations For Test Performance And Interpretation From Thesecond National Conference On Serologic Diagnosis Of Lyme Disease
The Association of State and Territorial Public HealthLaboratory Directors, CDC, the Food and Drug Administration, theNational Institutes of Health, the Council of State and TerritorialEpidemiologists, and the National Committee for Clinical LaboratoryStandards cosponsored the Second National Conference on SerologicDiagnosis of Lyme Disease held October 27-29, 1994. Conferencerecommendations were grouped into four categories: 1) serologictest performance and interpretation, 2) quality-assurancepractices, 3) new test evaluation and clearance, and 4)communication of developments in Lyme disease testing. Thisreport presents recommendations for serologic test performance andinterpretation, which included substantial changes in therecommended tests and their interpretation for the serodiagnosis ofLD.
It was recommended that an IgM immunoblot be consideredpositive if two of the following three bands are present: 24 kDa * , 39 kDa , and 41 kDa . It was furtherrecommended that an that IgG immunoblot be considered positive iffive of the following 10 bands are present: 18 kDa, 21 kDa *,28 kDa, 30 kDa, 39 kDa , 41 kDa , 45 kDa, 58 kDa , 66 kDa, and 93 kDa .
The details of both plenary sessions and the work groupdeliberations are included in the publication of the proceedings,which is available from the Association of State and TerritorialPublic Health Laboratory Directors telephone 822-5227.
Don’t Miss: What To Do If You Have Lyme Disease
How To Avoid Wasting Time & Money With 6 Steps
1. Add Certainty
Lyme MSIDS Questionnaire
2. Play An Active Role In Your Healing ASAP
as proactive as possible
3. Find the Right Doctor
There are not many reliable tests out there to truly confirm that one has Lyme. It doesnt show up on most standard tests like other diseases do. Lyme disease is also known as the “great imitator.” This is because its symptoms can be so diverse that it can mimic 200 different illnesses. Theres a really tragic amount of people who get misdiagnosed as having “Atypical MS,” “Atypical ALS,” “Atypical Lupus,” Fibromyalgia, or some other symptom-based diagnosis, and so they get the wrong treatments and waste a lot of time and money for nothing. In addition, many doctors have believed that it can only be Lyme disease if there is or was a bulls-eye rash, but we now know that only about 30% of people bitten by a Lyme-infected tick even develop a bulls-eye rash. Combine these with the testing difficulties and it’s easy to see how misdiagnoses could be far too common. That doesn’t have to be your story though! When searching for a doctor, use Lyme-literate as a keyword and find someone who specializes in this tricky illness instead of just your standard general practitioners. A good place to start could be seeing if one of the many clinics that carry the Jernigan Nutraceuticals product line is near you. Find out here.
4. Create a Well-Rounded Healing Strategy
5. DETOX. Yes, It Really Is Important.
6. Support Yourself Emotionally & Mentally
Canadian Public Health Laboratory Network Recommendations
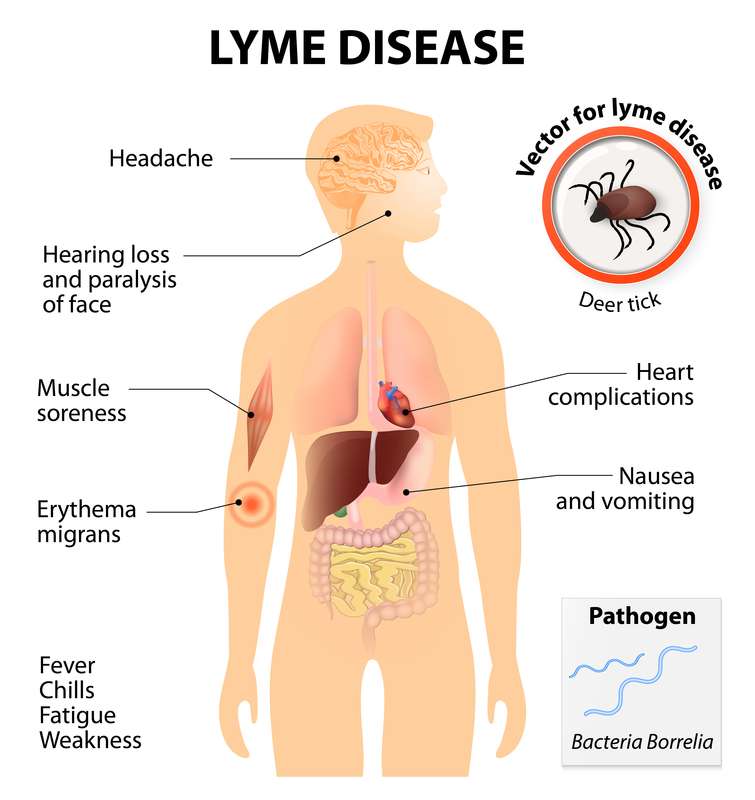
The appearance of a typical EM rash occurring in season and with a history of exposure to ticks should be considered an indication for antibiotic treatment, irrespective of the results of serological testing.
An EM-like rash occurring out of season and/or after exposition in a Lyme nonendemic area where ticks are not known to be established should be investigated with antibody testing.
Initial negative serological tests in patients with skin lesions suggestive of EM should have testing repeated after four weeks.
Patients with symptoms and signs suggestive of early disseminated or late Lyme disease should be tested for antibodies to B burgdorferi.
Initial testing should include an EIA commercially available and approved for use in Canada.
Sera that are positive or indeterminate by an EIA should be subjected to Western blot confirmatory testing.
Sera that are screened negative for antibodies using an EIA should not be subjected to Western blot testing.
Western blot tests should be interpreted using criteria set forth by the CDC Working Group.
Western blot tests that fail to meet all of the criteria set out by the CDC Working Group should be reported as negative testing may be repeated when it is appropriate to do so.
The specific banding patterns seen on Western blots should not be reported.
Culturing for B burgdorferi is a low-yield procedure and is not encouraged if performed, it should be done only on biopsies from EM lesions and synovial or spinal fluid.
Read Also: Fda Approved Lyme Disease Test
How Do You Get Lyme Disease From Ticks
How do you get lyme disease from ticksAdult ticks can also transmit Lyme disease bacteria. They are much larger and are more likely to be discovered and removed. Adult ticks most commonly bite during the fall. There is no evidence that Lyme disease is transmitted from person-to-person through touching, kissing, or having sex with a person who has Lyme disease. Lyme disease acquired .
The signs and symptoms of Lyme disease vary. They usually appear in stages, but the stages can overlap. Early signs and symptoms. A small, red bump, similar to the bump of a mosquito bite, often appears at the site of a tick bite.
In the South, lone star ticks can also transmit Lyme disease or a closely related illness. Ticks have four life stages: egg, larva, nymph and adult. In each stage after hatching, they suck blood from animals like mice, squirrels, birds and deer.
If you think you may have Lyme disease, contact your physician right away. Your doctor may do a test for Lyme disease. The FDA regulates diagnostic.
DISCLAIMER: The Lyme Disease Association, Inc. provides referrals to health care providers who treat Lyme disease, and often other TBD, as a courtesy to those seeking Lyme Literate Physicians . However, some of the providers included do not specifically treat Lyme and TBD but see patients who have symptoms associated with Lyme and TBD to.
Can I Catch Lyme Disease From My Dog
Dogs are not a direct source of infection for people. Lyme disease cant be transmitted from one pet to another, nor from pets to humans, except through tick bites. However, a carrier tick could come into your house on your dogs fur and get on you.
If your dog is diagnosed with Lyme disease, you and any other pets have probably been in the same outdoor environment and may also be at risk, so it is a good idea to consult with your physician and veterinarian to see whether you should test other pets or family members.
Read Also: Best Lyme Disease Doctors In Massachusetts
Racial Differences In Incidence
Lyme disease is reported primarily in whites, although it occurs in individuals of all races. No genetic explanation is known for this the disparity most likely stems from social or environmental factors and possibly to the fact that erythema migrans is more difficult to diagnose in dark-skinned individuals.
Can You Get Lyme Disease From Other People Or Animals
Theres no evidence that Lyme disease can be transmitted sexually or by touching or kissing a person who has it, says Dr. Kuritzkes. One widely reported study from 2014 found that the bacterium that transmits Lyme disease could be present in semen and vaginal secretions, which sparked fears that the disease could be passed between sexual partners. But theres never been a reported case of sexual transmission, says Dr. Kuritzkes, and most experts dont believe you can catch Lyme disease in this way.
In rare cases, Lyme disease has been transmitted from a pregnant woman to her fetus or placenta. Fortunately, according to the CDC, treating an infected woman with antibiotics seems to protect the fetus from any negative effects. Theres also no evidence that Lyme disease can be passed through breastfeeding.
And while there have been no reports of Lyme disease being transmitted through a blood transfusion, scientists say it could potentially happenso people who are being treated for Lyme disease should not donate blood.
Dogs are less likely to be bitten by deer and western blacklegged ticks, although it does happenso its still important to check your pets after time spent outdoors and to remove any ticks you find. You can also talk to your veterinarian about preventive treatments that can reduce the risk of your pets being bitten by ticks or about a vaccine that can protect dogs from the disease.
Also Check: What To Do If I Have Lyme Disease
Brain Fog And Cognitive Issues
Chronic Lyme disease knows no boundaries. This includes your blood-brain barrier. Borrelia burgdorferi can cross this protective border and create new problems. These may mimic other diseases.
Your body makes an enzyme called plasmin that dissolves the membrane of the bacteria. But the sneaky microbe can counteract this enzyme and protect itself. This gives it a free pass through your blood-brain barrier.
Lyme bacteria can also change their size and shape so they can migrate to other parts of your body. When they get into your brain, they inhabit glial cells and neurons. They cause these brain cells to become dysfunctional. This can lead to anxiety and depression.
The bacteria can also interfere with your neurotransmitters or nerve messengers. For example, they may disrupt your production and use of dopamine. The result can look like Parkinson’s disease.
Whats more, the microbe can increase a neurotransmitter called octopamine. When this accumulates in your brain, it can raise your blood pressure and cause headaches. You may incorrectly blame these headaches on environmental allergies, stress, or other factors.
When this insidious microorganism is killed, it sheds parts of itself as endotoxins. These may interfere with your brain chemistry. A buildup of toxins can give you intense brain fog and memory issues. %20%5B231%5D.” rel=”nofollow”> 31)