Coinfection With Other Tick
Ixodes ticks have a broad host range, therefore increasing the chance of acquiring multiple pathogens from reservoir hosts. This suggests that patients with one documented tick-transmitted disease may be at increased risk for infection with other tick-transmitted microorganisms. In Wisconsin, a study of 96 patients with a primary diagnosis of LD demonstrated immunoserologic evidence of coinfection with Babesia microti and/or Ehrlichia phagocytophila in 9.4% . In addition to ehrlichiosis and babesiosis, coinfection with tick-borne encephalitis virus is a possible consideration for LD patients in Europe. Infection with multiple agents could explain, at least in part, the variable manifestations and clinical responses reported in some patients with LD and may have confounded our understanding of the true clinical spectrum of the disease. As a practical consideration, laboratory testing for coinfection should be considered in some clinical situations to ensure that appropriate antimicrobial therapy is prescribed.
When Is Lyme Disease Blood Test Ordered
Lyme disease testing is ordered when a person has signs and symptoms suggestive of an infection with B. burgdorferi and lives in or has visited a region where deer ticks, also known as black-legged ticks, are common, especially when the person has recently been bitten by a tick.
Some early signs and symptoms of Lyme disease may include:
- A characteristic “bulls-eye” rash that spreads from the site of the bite
What Are The Symptoms Of Lyme Disease
Symptoms of Lyme disease change as it progresses in the body, but a rash can occur between three days to several weeks after the tick bite. The rash is the most identifiable symptom of Lyme disease and happens in about 70-80% of diagnosed cases.
Common Lyme disease symptoms include:
- A characteristic bullseye shaped rash
Less common Lyme disease symptoms include:
- Temporary paralysis of the muscles in the face
- Irregular heartbeat
Don’t Miss: Lyme Literate Doctor Los Angeles
What Are The Complications With Lyme Disease
Lyme disease is often misdiagnosed as arthritis, fibromyalgia, multiple sclerosis, and other illnesses like chronic fatigue syndrome, so it is important to get tested if you are experiencing any symptoms so you can be prescribed the right treatment.
If you dont get tested and it remains untreated, long-term damage to the heart, joints, and nervous system can occur.
The Role Of Lyme Disease Tests
The purpose of the most common type of Lyme disease testing is to determine whether you have developed antibodies as a result of past exposure to the Borrelia bacteria that cause Lyme disease. Antibodies are proteins created by the immune system that target specific threats like bacteria and viruses.
Blood testing alone cannot determine whether you have Lyme disease. Instead, testing can provide helpful information that your doctor can consider along with other factors, such as any symptoms youve had and whether youve been exposed to ticks that can carry Borrelia, to determine if a diagnosis of Lyme disease is appropriate.
Beyond blood testing, it is possible to analyze fluid from the central nervous system for signs of the Borrelia bacteria.
Recommended Reading: Can You Get Lyme Disease More Than Once
Why Do I Need A Lyme Disease Test
You may need a test if you have symptoms of infection and were exposed or possibly exposed to ticks that carry the bacteria that causes Lyme disease. The first symptoms of Lyme disease usually show up between 3 and 30 days after the tick bite.
Early signs and symptoms may include:
- A reddish round skin rash that slowly gets bigger over several days. It usually doesn’t itch or hurt, but it may be warm. As it gets better, it may look like a bull’s-eye , but not always.
- Muscle and joint aches
- Swollen lymph nodes
Later signs and symptoms of Lyme disease usually affect your joints and nervous system. They include:
- Severe headaches and neck stiffness
- Rashes on other parts of your body
- Arthritis with severe joint pain and swelling, especially in the knees
- Pain that comes and goes in your muscles, joints, bones, and tendons
- Shooting pains, numbness, or tingling in your hands or feet
Molecular Testing For Detection Of Borrelia Species Bacterial Dna
PCR is available for Borrelia species DNA detection but is of limited value in routine testing for Lyme disease because the organism is only present in blood during the early stages of the disease and is predominantly restricted to the affected tissues.
Diagnostic molecular testing for Borrelia species DNA is available on request for relevant specimen types. Please call RIPL to discuss individual cases.
Also Check: Do You Get A Fever With Lyme Disease
Key Points To Remember
- Most Lyme disease tests are designed to detect antibodies made by the body in response to infection.
- Antibodies can take several weeks to develop, so patients may test negative if infected only recently.
- Antibodies normally persist in the blood for months or even years after the infection is gone therefore, the test cannot be used to determine cure.
- Infection with other diseases, including some tickborne diseases, or some viral, bacterial, or autoimmune diseases, can result in false positive test results.
- Some tests give results for two types of antibody, IgM and IgG. Positive IgM results should be disregarded if the patient has been ill for more than 30 days.
What Is A Lyme Disease Blood Test
A Lyme disease blood test is used to determine if you have contracted Borrelia burgdorferi , the bacterium that causes Lyme disease. Lyme disease tests are conducted with a routine blood draw.
While there are other species of Borrelia that cause Lyme disease, B. burgdorferi is the most common cause in the United States. Most antibody tests in the United States only test for B. burgdorferi, but other species-specific tests are available depending on a persons travel history.
Lyme disease is transmitted to humans through ticks that are infected with Borrelia.
- shortness of breath
Lyme disease can be difficult to diagnose. Ticks are very small, and the bites are not always noticeable. Symptoms of the disease can vary from person to person. Not everyone experiences the classic bulls-eye rash pattern around a tick bite.
It should be noted that testing is not always required to make a diagnosis. For people with a classic bulls-eye rash living in a high risk area, testing is not recommended for diagnosis.
Your doctor will use the results of a Lyme disease antibody test, along with the report of your symptoms, to confirm a diagnosis.
Antibodies are proteins your body makes in response to foreign or harmful substances called antigens. Common antigens include:
Your body produces antibodies if you have contracted B. burgdorferi. These Lyme disease-specific antibodies will be present in your blood, and your test will be positive if you have the bacterial infection.
Don’t Miss: Lyme Disease And Joint Pain
Lyme Disease Antibody Test Procedure
The Lyme disease antibody test requires no advance preparation. A lab technician will swab the inside of your elbow with an antiseptic before drawing your blood. Your blood will be drawn from a vein in your arm using a small needle.
The blood draw should not be painful, though you might feel a slight prick when the needle is inserted into your vein.
The blood sample will be collected in a vial. The puncture site will be bandaged, if needed, after the needle is removed. After the blood draw, you are free to go home.
There are very few risks associated with the Lyme disease antibody test. Excessive bleeding is possible, but there may be an increased risk if you take blood thinning medications or certain anti-inflammatory drugs like:
Culture Isolation And Direct Detection Of Organisms In Tissue
Culture isolation of B. burgdorferi sensu lato from clinical specimens remains the gold standard for diagnosis and is most commonly attempted with skin biopsy or cutaneous lavage specimens from EM lesions and blood from patients with early-disseminated disease. Positive culture rates of nearly 90% for secondary EM lesions, 50% for primary EM lesions, and 48% for large-volume blood or plasma specimens from patients with early LD have been reported . Isolation of B. burgdorferi sensu lato from other sites, such as cerebrospinal fluid and synovial fluid, is uncommon the low recovery rate probably reflects the small number of viable organisms present in those anatomic locations.
Culture of B. burgdorferi sensu lato involves incubating a specimen in Barbour-Stoenner-Kelly medium and detecting the presence of characteristic spirochetes by dark-field microscopy or by fluorescent microscopy with acridine orange or a specific fluorescent antibody . Some microbiologists consider Borrelia culture to be too expensive and tedious to be practical for many clinical laboratories. In reality, isolation of B. burgdorferi sensu lato is no more difficult and is probably easier than recovering and identifying other fastidious microorganisms such as Legionella or Mycobacteria spp. from clinical specimens. BSK is commercially available, and the only specialized equipment required is a fluorescent microscope or a light microscope equipped with a dark-field condenser.
Also Check: Cvs Minute Clinic Lyme Disease Test
What Is Lyme Disease
Lyme disease is an illness caused by infection with a bacteria that is spread through the bite of certain kinds of ticks. Symptoms can affect the skin where the bite occurred or elsewhere on the skin and may progress to affect other parts of the body. A family of bacteria, known as Borrelia, causes Lyme disease.
Alternative Diagnostic Tests Not Available At Ripl
Tests used by the NHS and UKHSA to identify Lyme disease are well characterised, standardised, and are highly reproducible between laboratories. They are the methods of choice recommended in the 2018 NICE Lyme disease guidelines, following an extensive review of the evidence and literature. International external quality assurance schemes are in place to ensure consistency between different centres offering these tests.
Several private laboratories in Europe and the US offer an alternative type of test called an ELISpot to diagnose Lyme disease. This looks for different markers in blood samples compared to conventional validated Lyme disease serology tests. The laboratories using these tests in the diagnosis of Lyme disease do not publish their methods, and have not produced peer reviewed publications on their clinical value.
This makes it very difficult to verify their results, especially as there are no national or international EQA schemes for Lyme disease ELISpot tests and therefore no independent verification of performance between laboratories. Without independent evidence it is impossible to determine the validity of results produced using these alternative tests.
RIPL cannot interpret the results of alternative diagnostic tests.
You May Like: How Many Ticks Carry Lyme Disease
Who Should Get Testing
Testing is usually indicated if a person has symptoms of Lyme disease and a known or possible exposure to ticks that can carry the Borrelia bacteria. However, because it takes time for antibodies to develop, the timing of testing is important to consider.
Lyme disease symptoms depend on the extent of the bacterial infection. Three phases are used to describe the infection:
It is important to understand these phases because testing is not equally valuable in each stage. With early localized disease and erythema migrans, blood testing is generally not helpful because antibodies have not had enough time to develop.
Because of similar concerns about potential false positive results, random screening for Lyme disease in people without symptoms is not recommended even in areas that are known to have ticks that can carry the Borrelia bacteria.
Laboratory Testing In Vaccinated Individuals
In 1998 the Food and Drug Administration approved a recombinant OspA vaccine for use in patients at risk of acquiring LD . Since the efficacy of the vaccine is reported to be in the range of 76% after three doses, there will be instances where vaccinated individuals acquire natural infection with B. burgdorferi sensu lato. ELISAs and IFA assays utilizing OspA-producing strains of B. burgdorferi sensu lato will not discriminate between vaccinated and naturally infected individuals. Therefore, the CDC two-step algorithm is not applicable to vaccinated patients and immunoblotting must be relied on for serologic confirmation of infection. In addition to increasing costs, the issue is complicated further by reports that some vaccinated patients produce antibodies that bind to various borrelial proteins, making interpretation of immunoblots more difficult . This will continue to be problematic until ELISAs and other first-line assays based on non-OspA-producing strains or recombinant borrelial proteins are in widespread use and physicians become aware of the specific limitations of the testing methods provided by their laboratories .
Recommended Reading: Diagnosed With Lyme Disease Now What
Types Of Lyme Disease Tests
Antibody titer tests for Lyme disease measure antibodies that are specific to the bacteria that can trigger the condition. Antibodies are part of the bodys immune response. Tests look for two types of antibodies, known as immunoglobulin M and immunoglobulin G .
IgM antibodies usually peak within a few weeks after an infection with Borrelia bacteria and start to collapse 4-6 months after infection. IgG antibodies are slower to develop, beginning to show 4-6 weeks after exposure and may peak 4-6 months after exposure. While IgM tends to be associated with an active infection, both IgM and IgG can persist in the blood for many years.
The Centers for Disease Control and Prevention recommends a two-stage or two-tiered test for these antibodies. If the initial blood test is positive for IgM or IgG antibodies associated with the Borrelia bacteria, a second test is done, often using different laboratory methods.
Testing for IgM and IgG can support the finding that you have been exposed to Borrelia, but this on its own does not prove whether or not you have Lyme disease.
Follow-up testing may be necessary if testing is inconclusive. This could involve repeat blood tests or the use of different types of medical tests to rule out other health conditions. In people suspected of bacterial reinfection, imaging tests may be used to detect joint inflammation.
Lyme Disease Antibody W/ Reflex To Blot
Test Code: 6646
CPT Code: 86618
Includes: If Lyme Disease Antibody Screen is Equivocal or Positive, Lyme Disease Antibodies , Immunoblot will be performed at an additional charge : 86617 x2).
Methodology: Immunoassay
Clinical Significance: Lyme disease is caused by a bacterium borrelia burgdorferi and is transmitted by ticks. EIA is the screening test with high sensitivity for antibody detection. Immunoblot testing qualitatively examines with high specificity antibodies in a patientâs specimen. Immunoblot testing is appropriate for confirming a detected EIA test result.
Alternative Name: Borrelia burgdorferi, Lyme Screening, Lyme Antibody Screen
Collection Guide:
Also Check: Treatment For Chronic Lyme Disease In Humans
How Lyme Disease Tests Work
Early and accurate diagnosis is the most important factor in a persons ability to overcome Lyme and other tick-borne diseases. This means access to high quality Lyme disease tests is crucial something all too many patients unfortunately struggle to find. The CDCs Lyme disease test recommendations are limited and flawed, leaving many patients understandably in search of better options.
However, without a medical background, it can be tough to understand the differences between the many types of Lyme disease tests. In this article, learn about the most common tests for Lyme and their various advantages and limitations.
Igg Vs Igm Antibodies
Getting accurate test results is the first step in getting treatment for Lyme disease. Still, it can be difficult to navigate the world of testing and understand how different tests work. Were here to help clear up some of the confusion, specifically when it comes to different types of cells and antibodies.
Read Also: Tick Bite Lyme Disease Symptoms Pictures
Finding The Right Lyme Disease Test
Symptoms of Lyme disease can mimic a wide range of illnesses, which can cause tick-borne infections to go misdiagnosed for long periods of time. Laboratory testing is vital for confirming a diagnosis so that people can get the treatment that they need.
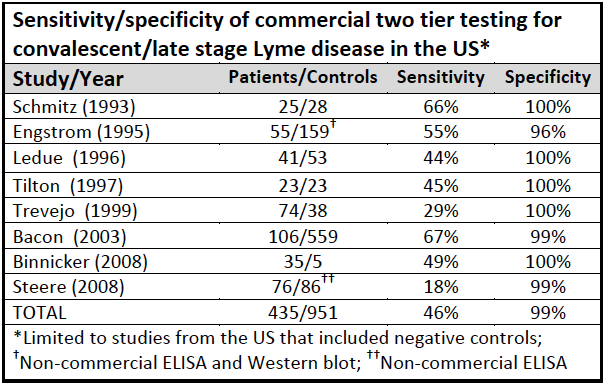
However, it can be difficult to find the testing and care you need after potential infection of Lyme disease. Not all Lyme testing is created equal. For example, the CDC-recommended two-tiered testing is notoriously unreliable, as many commercially available tests are not always sensitive enough to detect active infections.
IGeneX tests, on the other hand, provide higher sensitivity testing to detect the bacteria that causes Lyme and other tick-borne diseases. IGeneX test panels contain tests designed to detect IgM or IgG antibodies, meaning they can detect disease at multiple stages.
Access To Lyme Disease Testing Services

This guidance on the laboratory diagnosis of Lyme disease is intended for healthcare professionals in the UK. Patients concerned about possible Lyme infection should consult an appropriate healthcare professional, for example their GP, in the first instance.
Health professionals wishing to discuss a possible case or ascertain local arrangements for testing should contact a local Infection specialist .
NHS testing for Lyme disease is available through local service providers and the Rare and Imported Pathogens Laboratory at UK Health Security Agency Porton where ISO15189 accredited confirmatory testing is also provided. RIPL also provides a testing service for neurological Lyme disease.
RIPL provides medical and laboratory specialist services to the NHS and other healthcare providers, covering advice and diagnosis of a wide range of unusual bacterial and viral infections, including Lyme disease.
RIPL continuously updates its methods and will make further information on Lyme disease diagnostic testing available as it arises.
Recommended Reading: Eye Doctor East Lyme Ct
Also Check: Antibiotics For Lyme Disease In Humans