How Is Lyme Disease Diagnosed
Lyme disease is difficult to diagnose because symptoms are not consistent and may mimic other conditions. The primary symptom is a rash, but it may not be present in up to 20% of cases.
Diagnosis for Lyme disease must be made by a healthcare provider experienced in recognizing Lyme disease. Diagnosis is usually based on symptoms and a history of a tick bite. Testing is generally done to confirm the diagnosis and rule out other conditions. This may need blood and other lab tests.
Research is underway to develop and improve methods for diagnosing Lyme disease.
The symptoms of Lyme disease may look like other medical conditions or problems. Always talk with your healthcare provider for a diagnosis.
What Can Be Done To Prevent Lyme Disease
The best prevention of Lyme disease is through awareness. Generally, ticks cannot jump or fly onto a person. They wait in vegetation and cling to animals and humans when they brush by. When in a potentially tick-infested habitat take special care to prevent tick bites, such as wearing light-colored clothing and tucking pants into socks and shirt into pants. Check after every 2 to 3 hours of outdoor activity for ticks on clothing or skin. Brush off any ticks on clothing or skin before skin attachment occurs. A thorough check of body surfaces for attached ticks should be done at the end of the day. If removal of attached ticks occurs within 36 hours, the risk of tick-borne infection is minimal. For proper tick removal, please watch the video at Tick removal. A vaccine for Lyme disease is not currently available.
Insect repellents can be effective at reducing bites from ticks that can spread disease. If you decide to use a repellent, use only what and how much you need for your situation. More information on repellents can be found at Environmental Protection Agency – insect-repellents.
In addition:
Domestic animals can carry ticks into areas where you live so it is important to check pets for ticks before they enter the home.
Diagnosis Of The Disease
New-onset Lyme disease is usually diagnosed based on symptoms, the presence of erythema migrans and possible exposure to infected ticks.
In addition, a blood test known as the two-step process is recommended.
The US CDC describes this testing process in its guidelines: Recommendations for Performing and Interpreting the Test from the Second National Conference on Serological Diagnosis of Lyme Disease.
Specifically, the two phases include:
- Stage 1: the EIA test or, less commonly, the immunofluorescence assay is performed.
- Stage 2: if the EIA or IFA are positive or inconclusive, the second test performed is an immunoblot test, also known as a Western blot. If the symptoms are new onset , the IgM Western blot is performed.
If symptoms have been present for more than 30 days, a positive or inconclusive EIA or IFA test is followed by the Western Blot IgG test.
Recommended Reading: What Is A Lyme Flare Up
What To Do If You Have A Blacklegged Tick Bite
Remove the tick by pulling it directly out with fine-tipped tweezers. Lift upward with slow and even pressure. Dont twist when removing it. Dont crush it or put soap or other substances on it. Dont apply heat to it.
Place the tick in a resealable container. See if you can identify what kind of a tick it is.
Immediately after removing the tick, wash your skin well with soap and water or with rubbing alcohol.
Not all ticks carry Lyme. The Lyme bacteria is transmitted only by blacklegged ticks in their nymph or adult stage.
Save the tick to show your doctor. The doctor will want to determine if its a blacklegged tick and if theres evidence of feeding. Ticks enlarge as they feed. Your risk of getting Lyme from an infected tick increases with the length of time that the tick fed on your blood.
Summary:
Pull the tick out with tweezers and save it in a resealable container for identification.
Lyme Disease Is An Illness Caused By The Bacterium Borrelia Burgdorferi These Bacteria Are Carried By The Black
About Lyme Disease
While Lyme disease was named for the town in Connecticut where it was first identified, Lyme disease-carrying ticks are found throughout the United States . The highest concentrations of black-legged ticks are found in the northeast, mid-Atlantic, and upper Midwest regions of the US. In recent years, confirmed cases of Lyme disease have been reported in every state. Most recent estimates are of 476,000 new cases of Lyme in the US every year. Scientists estimate that two million people could suffer from post-treatment Lyme disease at the end of 2020. Lyme disease has also been found in 80 countries.
How Do You Get Lyme Disease?
Lyme disease is transmitted through the bite of an infected black-legged tick. Ticks look for hosts to feedhosts can include pets, deer, mice, birds, squirrels, some reptiles, and yes, people.
to see a chart of most common ticks found in the U.S. and the associated diseases they may carry.
Who Is Most At Risk for Lyme Disease?
Ticks are not just a suburban problem they are everywhere including urban areas and cities. Many people get bitten by a tick in their own yards and local parks. While you are most likely to be bitten by a tick during the warmer months, ticks can be active year-round and are active at any temperature above 34 degrees Fahrenheit.
How is Lyme Disease Diagnosed?
Cases of Lyme Disease Are on the Rise
Also Check: What If My Dog Has Lyme Disease
There Is A Right Way To Remove A Tick
So, for now, the best way to prevent Lyme right now is to keep an eye out for ticks and make sure you remove them correctly.
According to the CDC, you want to take a tweezer and get close to the skin, and then pull the tick upward. Thats because you want to make sure to remove the whole tick, without leaving any of its mouth parts where bacteria may linger in the skin.
After removing the tick, wash the bite area and your hands with rubbing alcohol or soap, and then take care to dispose of the tick by submersing it in alcohol, placing it in a sealed bag/container, wrapping it tightly in tape, or flushing it down the toilet, the CDC advises.
Here are a few other things the CDC recommends doing to avoid tick bites and Lyme:
- When youre spending time outdoors, especially in wooded areas, wear insect repellent and clothes that protect your skin.
- Bathe after youve been outdoors, and check your body for ticks including the back of your legs and your scalp.
- If youre worried ticks have embedded themselves in your clothes, throw them in your clothes dryer on high heat for 10 minutes.
- Check your gear and pets for ticks .
- Walk in the center of trails, avoiding brushing up against tall grass.
- Keep the space around your home clean and minimize the areas where ticks can lurk cut your grass, pick up your leaves, and make sure there are no rodents around.
For more about Lyme Disease, tune in to the June 15, 2018 episode of Today Explained: Little summer vampires.
Limitations Of Surveillance Data
You May Like: What Happens When You Have Lyme Disease
Lyme Disease Heightens Risk Of Mental Disorders Suicidality: Study
Washington, January 7: In a new study, US and Danish researchers report that patients hospitalised with Lyme disease had a 28 per cent higher rate of mental disorders and were twice as likely to have attempted suicide post-infection, compared to individuals without the diagnosis.
Lyme disease heightens risk of mental disorders, suicidality: Study
Unexplained Pain And Other Sensations
Some people with Lyme may have sharp rib and chest pains that send them to the emergency room, suspecting a heart problem 00090-7/abstract%20″ rel=”nofollow”> 27).
When no problem is found, after the usual testing, the ER diagnosis is noted as an unidentified musculoskeletal cause.
You can also have strange sensations like skin tingling or crawling, or numbness or itchiness 00090-7/abstract%20″ rel=”nofollow”> 27).
Other symptoms have to do with cranial nerves.
- Ear-ringing . Tinnitus can be a nuisance, especially at bedtime when it seems to get louder as youre trying to fall asleep. About 10 percent of people with Lyme experience this (
- Hearing loss. One study reported that 15 percent of Lyme patients experienced loss of hearing .
- Jaw pain or toothaches that are not related to actual tooth decay or infection.
Summary:
You May Like: Can Lyme Disease Cause Immune Deficiency
Publicly Available Surveillance Data
Links with this icon indicate that you are leaving the CDC website.
We take your privacy seriously. You can review and change the way we collect information below.
Cookies used to make website functionality more relevant to you. These cookies perform functions like remembering presentation options or choices and, in some cases, delivery of web content that based on self-identified area of interests.
Each Year Nearly Half A Million People In The United States Are Diagnosed And Treated For Lyme Disease Also Known As Lyme Borreliosis Caused By A Bacterium Carried By Deer Ticks And Transmitted To Humans Through Their Bite
In a new study, US and Danish researchers report that patients hospitalised with Lyme disease had a 28 per cent higher rate of mental disorders and were twice as likely to have attempted suicide post-infection, compared to individuals without the diagnosis.
The study, a collaboration of Columbia University and the Copenhagen Research Centre for Mental Health, is believed to be the first large, population-based study examining the relationship between Lyme disease and psychiatric outcomes.
The research appears in the July 28 online edition of the American Journal of Psychiatry.
ALSO READ: Everything you need to know about Lyme disease and how to prevent it
“It is time to move beyond thinking of Lyme disease as a simple illness that only causes a rash,” said Brian Fallon, MD, MPH, a psychiatrist with the New York State Psychiatric Institute and Columbia University who is the lead author of the paper, adding, “In addition to the risk of severe cardiac, rheumatologic, and neurologic problems, Lyme disease can cause severe mental health problems as well.”
Dr. Fallon, one of the foremost researchers of the neuropsychiatric effects of Lyme disease, is director of the Lyme and Tick-borne Diseases Research Center at Columbia. The team of investigators on the study includes Michael Benros MD, PhD, principal investigator Trine Madsen, PhD, co-first author and Annette Erlangsen, PhD, all psychiatric epidemiologists at the Research Centre for Mental Health.
Also Check: Alternative Therapies For Lyme Disease
It May Not Just Be Lyme Thats Infecting People
At the same time, theres a lot were still learning about Lyme and all the other infections ticks may simultaneously transmit to people. A third of all the known tick-borne pathogens were discovered in the past two decades, including:
- Borrelia miyamotoi
- Heartland virus
- Rickettsia parkeri
So researchers and doctors have a lot to learn about how ticks can sicken people and how the diseases they can spread interact with one another.
We know new organisms are being discovered every one or two years … in ticks, said Fallon. This is a time of continuous discovery in terms of whats going on with tick-borne diseases. So some of what we now think are symptoms of Lyme may be infections caused by other viruses and bacteria, or co-infections that may be interacting with the B. burgdorferi that causes Lyme.
Too few health care practitioners and patients are aware of that, wrote Richard Horowitz, a doctor specializing in internal medicine, at the New York Times:
The existence of these co-infections so-called because they are often transmitted along with Lyme disease explain why some people with Lyme remain chronically ill even after treatment. While the Lyme is identified and treated, these other infections are not. In addition, testing for co-infections is often unreliable, as it is for Lyme disease, so co-infections often go undiagnosed.
The Rise And Fall Of A Lyme Disease Vaccine
The best way to avoid a tick bite is simply to stay out of places where they are prevalent: wooded, bushy areas with tall grass. If you do visit this type of environment, Krause said, apply insect repellant and wear long sleeves with long pants tucked into socks.
“If you go into a wooded area, you have to do tick checks later,” he said.
People who get a tick bite can seek antibiotics, but Krause said they don’t always eliminate the symptoms.
“What appears to be the case at least there’s some reasonable evidence for this is that although the Lyme organism is killed with antibiotics, the organism itself doesn’t break down very well. It sort of hangs around in a dead form,” he said.
He added: “We really do need a vaccine. Thats probably the best hope for us to really get control of it.”
The Food and Drug Administration approved a vaccine called LYMErix in 1998 that was shown to prevent Lyme disease in clinical trials. ButGlaxoSmithKline, the developer of that vaccine, pulled it off the market in 2002.
“It worked, but the company stopped using it because it took three injections and there was a group of people who claimed, falsely, that it was causing arthritis,” Krause said.
Krause said another Lyme vaccine could become available in a couple of years. A candidate from Pfizer has shown early promise in trials.
You May Like: How To Get Checked For Lyme Disease
Blood Tests For Antibodies
Blood tests for detecting antibodies to B. burgdorferi are most reliable several weeks after infection has occurred and are rarely of value during the first 7 to 10 days of illness. During these initial days of infection, these tests can give false negative results .
Most authorities, including the CDC, recommend a 2-step testing process for Lyme disease:
- EIA Test. The first test used is an enzyme immunoassay . The EIA measures IgM and IgG antibodies to the B. burgdorferi spirochete. Positive results from this test still require confirmation with a Western blot test, since the EIA test is often positive even when there has been no infection. Negative results do not require further testing.
- Western Blot or second EIA test. If the EIA test is positive or uncertain, it is followed by the Western blot test. This test is more accurate and is very helpful in confirming the diagnosis but is more expensive and takes longer to complete. The Western blot creates a visual graph showing bands of IgM or IgG antibodies that laboratories use to interpret the immune response. More recently, recommendations have changed to allow for a second EIA in place of the confirmatory Western blot .
- V1sE . This newer FDA-approved test detects a specific component within the EIA IgG antibodies and is being increasingly used instead of the Western Blot to confirm a positive EIA test. Since it is less expensive and more rapidly completed, it may ultimately replace the Western Blot test.
What You Need To Know About Lyme Disease
-
Lyme disease is an infection caused by the spiral-shaped bacteria Borrelia burgdorferi, which is most commonly transmitted by a tick bite.
-
There are over 300,000 estimated new cases of Lyme disease in the United States each year.
-
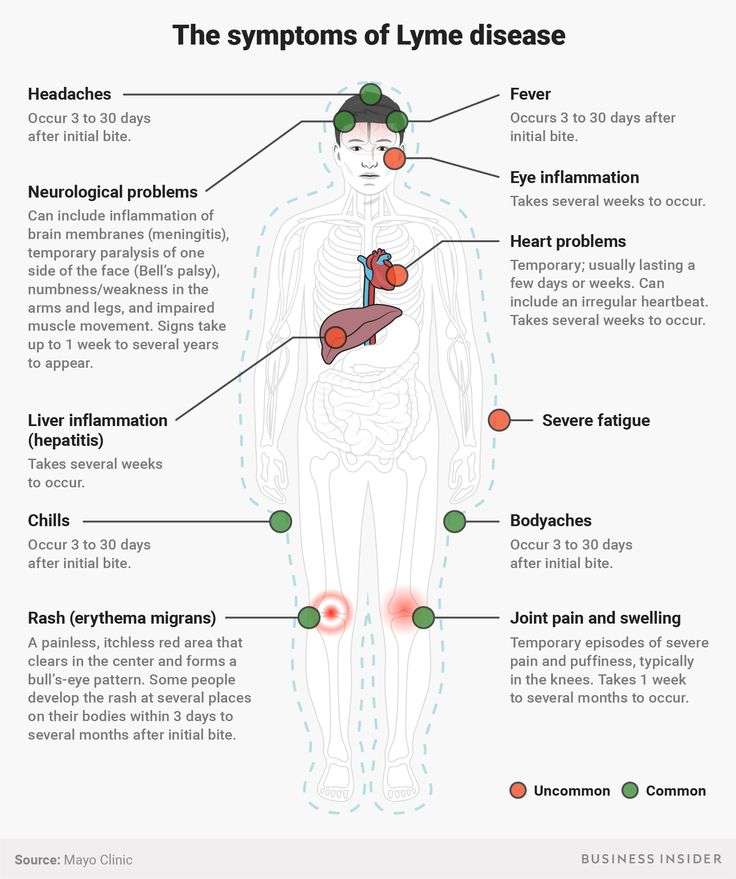
The symptoms of Lyme disease depend on the how long the infection has been present in the body. The first sign of Lyme disease is often an expanding round or oval red “bullseye” rash.
-
If left untreated, people may develop neurological symptoms and heart problems, and have an approximately 60 percent chance of developing Lyme arthritis.
Read Also: Fasting To Cure Lyme Disease