To Remove A Tick That Is Attached To Your Skin
- Gently grip the tick as close to the point of attachment to the skin as possible. Do this preferably using fine-toothed tweezers or forceps, or a tick removal device.
- Pull steadily upwards, away from the skin. Take care not to crush the tick.
Inexpensive tick removal devices may be available at veterinary surgeries and pet supply shops and are useful for people who are frequently exposed to ticks. These should be used in accordance with manufacturers’ instructions.
Do NOT do any of the following:
- Burn the tick off .
- Apply petroleum jelly, alcohol, nail varnish remover, or other substances .
- Use your fingers to pull the tick off.
- Squeeze the tick.
After removal, DO clean the skin with soap and water, or skin disinfectant, and wash hands.
Who Is At Risk For Lyme Disease
Anyone can get a tick bite. But people who spend lots of time outdoors in wooded, grassy areas are at a higher risk. This includes campers, hikers, and people who work in gardens and parks.
Most tick bites happen in the summer months when ticks are most active and people spend more time outdoors. But you can get bitten in the warmer months of early fall, or even late winter if temperatures are unusually high. And if there is a mild winter, ticks may come out earlier than usual.
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
You May Like: What Type Of Doctors Treat Lyme Disease
Who Is At Risk For Complications Of Lyme Disease
People who do not know they have been infected. So its important to check for deer ticks after outdoor activitiesespecially in the northeast or midwest parts of the country.
Ticks sometimes bite in such inconspicuous places as the hairline or back. Lyme disease is treated with antibiotics at any stage of illness to eradicate the bacterial infection. However, some people might still be at risk for lingering neurological complications if the bacteria has traveled to the tissue of the central nervous system.
Also Check: Whats Lyme Disease Look Like
Does Lyme Disease Stay With You Forever
Once treated, Lyme disease does not stay for years. However, some people may still experience the after-effects of the disease for months and even years. There are clinical trials that involve participants who are suspected to have Post Treatment Lyme Disease Syndrome to help in understanding the disease even further and develop new treatment plans. If you are interested in joining a clinical trial, go to Power to quickly find one that also matches your current condition. Anonymous Online Contributor
Early Lyme disease is treated with antibiotics such as doxycycline, amoxicillin, or cefuroxime axetil. When treated early, Lyme disease can be cured and most patients will recover completely.
Even when treated in later stages, most patients will respond well to antibiotics, though there may be some chronic damage to the nervous system or joints.
Lyme disease is an illness transmitted to humans via tick bites, from infected ticks of the genus Ixodes . The tick bite spreads the germ that causes Lyme disease to humans .
The type of tick that carries Lyme disease feeds on deer and mice, and can only infect a human if it remains attached to a person for at least a day and a half.
You May Like: Chances Of Lyme Disease After Tick Bite
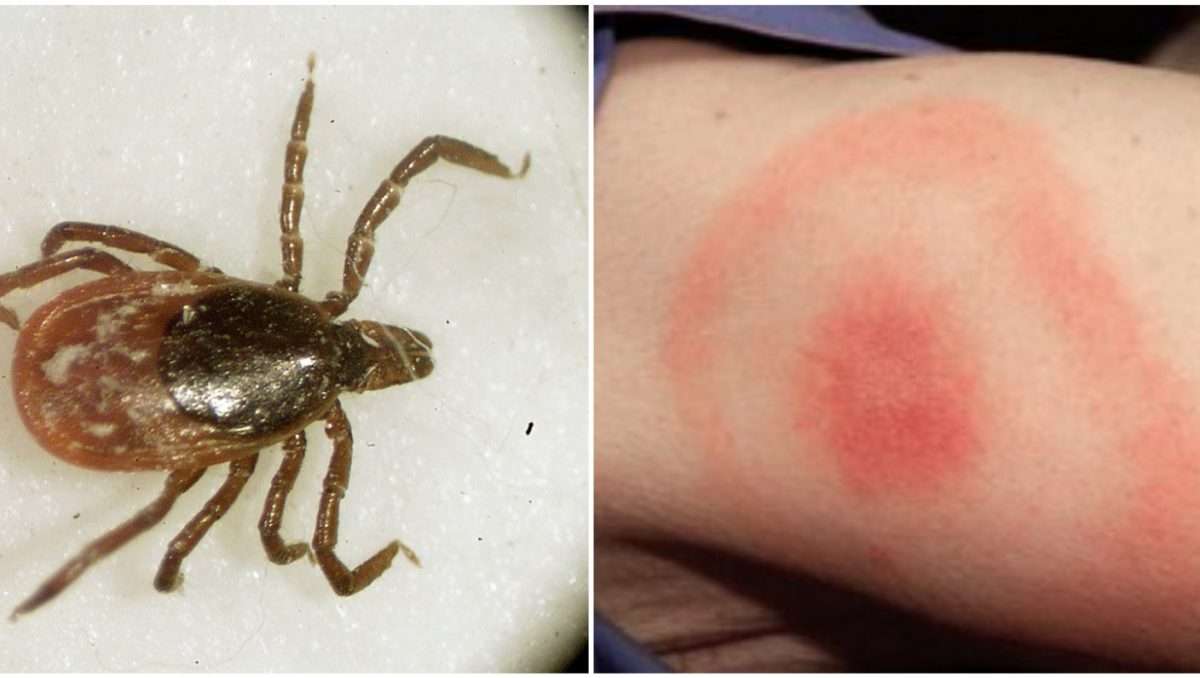
Erythema Migrans ‘bullseye Rash Of Lyme Disease
Rash – the classical symptom of Lyme disease is a typical rash called erythema migrans. However, this does not always occur. It may depend on which species of borrelia is involved. In the UK, most people with Lyme disease have or have had this rash.
The rash is usually a single circular red mark that spreads outwards slowly over several days. The circle becomes bigger and bigger with the centre of the circle being where the tick bite occurred. As it spreads outwards, a paler area of skin emerges on the inner part of the circle. Therefore, the rash is often called a ‘bullseye’ rash. Some types of the germ do not cause a rash, or the rash is different. For example, in the USA, the rash is less likely to have the ‘bullseye’ appearance.
The rash usually spreads over at least 5 cm but may be much bigger.
The rash is not usually painful or particularly itchy. You may not even notice it if it is on your back. Without treatment, erythema migrans typically fades within 3-4 weeks. However, just because the rash fades it does not necessarily mean the infection has cleared from the body.
Note: many insect bites cause a small red blotchy ‘allergic’ rash to appear soon after the skin is bitten. These soon go away. The rash of erythema migrans is different in that it usually develops several days after the bite, lasts for longer and has a typical spreading circular appearance.
Unraveling The Mystery Of Lyme Disease
Vol. 53 No. 4
Monitor on Psychology53
Long before the SARS-CoV-2 virus was linked to a syndrome we now call long COVID, researchers and clinicians were already debating over how to best assist patients experiencing lingering symptoms from Lyme disease. For reasons that are unclear, 10% to 20% of people who contract Lyme disease report ongoing or intermittent symptoms at least a year after completing antibiotic treatment, including fatigue, muscle aches, difficulties with memory, irritability, and other symptoms, according to a review of the research .
For patients, these ongoing and sometimes debilitating symptoms can erode their quality of life, potentially leading to depression, anxiety, and other mental health issues. But over the past few decades, researchers have also determined that the tick-borne infection itself, along with related inflammatory and other physiological effects, may directly cause mental health disorders.
One recent study, conducted by researchers from the Columbia University Irving Medical Center and the Copenhagen Research Centre for Mental Health, found that patients who received a hospital diagnosis of Lyme disease had a 28% higher rate of mental disorders and were twice as likely to have attempted suicide postinfection than individuals without a Lyme diagnosis .
Read Also: Best Lyme Treatment In The World
Lyme Disease Patients Covid
Patients surveyed expressed concern about being exposed to COVID-19 . Some patients have avoided or cancelled a Lyme disease appointment due to fear of being exposed in medical office. Most patients reported taking actions to reduce their risk by washing their hands and/or using hand sanitizer often , wearing a mask in public , sheltering in place , or wearing gloves .
Many expressed concerns about the availability of treatment or obtaining medications for Lyme disease. Approximately 53% report that their clinician has cancelled an in-office appointment due to COVID-19. However, 82% reported that their clinician offered virtual appointments. Obtaining medications was not a problem for 74% of those who responded.
Financial concerns and concerns about insurance availability were common. 64 percent of people report not having a financial hardship, while 36% say that they or someone in their household has been laid off, furloughed, or has temporarily or permanently closed a business. 90 percent reported no impact on their insurance. This again is another figure that may change if patients lose their coverage due to job loss as the pandemic continues.
We are grateful to all who have participated thus far and encourage others to take part as well. If you are already part of MyLymeData, you simply have to log in to your account and click on the survey. Otherwise, please enroll in MyLymeData here, take the initial survey and proceed to the COVID-19 survey.
What Should You Do If You Find A Tick
-
Don’t touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Don’t squeeze the tick, and don’t use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
Recommended Reading: How Does Lyme Disease Affect Humans
Some Vaccinated For Covid While Actively On Antibiotics
16% of patients who report having been vaccinated were actively on antibiotic treatment for Lyme disease when they received their shots. Nearly 93% of those vaccinated recommend that their friends and family receive the vaccination when able.
Of those who have not been vaccinated, 35% intend to get the vaccine when it is available to them and 39% do not intend to receive the vaccine. The remainder are unsure. For patients who do not intend to get vaccinated, 49% cited safety concerns and worries about potential COVID vaccination side effects.
A large majority of patients report that they take precautions to reduce their risk of exposure by wearing a mask in public , washing their hands and/or using hand sanitizer often , sheltering in place , or limiting contact to a small group of people with low risk .
What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.
Read Also: What Are The Signs Of Lyme Disease In A Dog
Gulf Coasts Ticks Infected With Rickettsia Parkerii Established In Nyc
Monica WhiteHome Page Featured, Information for Doctors, Lyme-TBD, New York, News, Other Tick-Borne Diseases, Resources for Patients, Rickettsiosis, States, Tick Vectors
In a recent New York City study, researchers investigated habitat associations and pathogen status of Gulf coast ticks . NYC is a newly expanded distribution range for this species. Investigators collected 88 ticks from two parks on Staten Island and compared findings of ticks collected from similar habitats in Brooklyn from April
The Chance Of Getting Lyme Disease

Not all ticks in England carry the bacteria that causes Lyme disease.
But it’s still important to be aware of ticks and to safely remove them as soon as possible, just in case.
Ticks that may cause Lyme disease are found all over the UK, but high-risk places include grassy and wooded areas in southern and northern England and the Scottish Highlands.
Ticks are tiny spider-like creatures that live in woods, areas with long grass, and sometimes in urban parks and gardens. They’re found all over the UK.
Ticks do not jump or fly. They attach to the skin of animals or humans that brush past them.
Once a tick bites into the skin, it feeds on blood for a few days before dropping off.
Read Also: Lyme Carditis Symptoms In Humans
Transmission Of Bb Via Ixodes Spp Vectors
The black-legged ticks, Ixodes scapularis and Ixodes pacificus on the West Coast, are the primary vectors of Bb in the USA. In endemic areas, the proportion of Ixodes spp. ticks infected withBb can be remarkably high. One recent survey of the pathogen burden of 197 Ixodes scapularis ticks collected from New York and Connecticut where LD is endemic, revealed 111 ticks were infected with Bb and 37 were co-infected with more than one human pathogen . The high pathogen burden is consistent with previous tick surveys in the same region . In contrast, the percent of infected ticks in other regions of the USA is much lower. In recently published surveys across California, for example, fewer than 5% of Ixodes spp. ticks were infected . Ixodes ticks sometimes carry multiple strains of Bb that may impact the course of disease in people that are co-infected. One tick survey showed that 39% of Ixodes ticks in North America are infected with multiple genotypes of Bb .
Recommended Reading: Lyme Literate Doctors In Colorado
Enhancing Healthcare Team Outcomes
The key to Lyme disease is prevention and this requires an interprofessional team approach. All healthcare workers including the nurse practitioner, pharmacist, and primary care provider should provide patient education on measures to prevent tick bites while hiking or working outdoors. In areas where ticks are common, cleaning up of the environment by removing the underbrush and spraying an insecticide may reduce the tick burden in the area. The outdoors person should be told to wear appropriate garments and be familiar with the skin features of the tick bite. The nurse should educate the patient on how to remove the tick from the skin and when to seek medical assistance. The pharmacist should educate the patient on medication compliance for those who have been confirmed to have acquired Lyme disease.
Nurses should educate parents how to inspect their children for ticks at the end of an outdoor event, in an endemic area. While there are many repellants on the market, it is best to avoid them as the risk of harm is greater than any benefit. If one is going to use a repellant, DEET is the one product that is safe, however, it is not 100% effective. finally, the pharmacist should educate the patient about the harms of taking prophylactic doxycycline a better strategy is to remove the tick as soon as it is visualized.
Outcomes
Recommended Reading: What Does A Lyme Flare Up Feel Like
Does Having Lyme Disease Increase The Risk For Severe Covid
According to the CDC, nearly one in five American adults who have had COVID-19 currently have chronic symptoms. With the U.S. approaching 100 million cases of confirmed COVID-19, that would mean nearly 20 million adults have long COVID.
Ive heard from many Lyme disease patients who say their Lyme symptoms flared after they contracted COVID-19.
The symptoms I hear about most are fatigue, migrating joint pain, difficulty concentrating , fibromyalgia-like muscle pain and sleep disturbance. Several patients I know have been placed back on treatment for Lyme disease and have seen significant improvement in their symptoms.
Babesiosis: A Global Review
Monica WhiteBabesiosis, Home Page Featured, Information for Doctors, Lyme-TBD, News, Other Tick-Borne Diseases, Peer Reviewed Articles, Research Articles, Resources for Patients
This review summarizes the health burden of human babesiosis emerging on a global scale. Authors discuss tools used to monitor the frequency and location of disease as well as demographics, modes of transmission and the location of human babesiosis. Authors further describe the causative Babesia spp. in North and South America, Europe, Asia, Africa, and
Monica WhiteHome Page Featured, Information for Doctors, Lyme & TBD Prevention, Lyme-TBD, News, Resources, Resources for Patients
A recent article published by The Wilderness Medical Society describes evidence-based guidelines for the prevention and management of tick-borne illness. These guidelines were developed on a grade system by an expert panel designated by The Wilderness Medical Society. Panelists were selected based on level of clinical interest or research experience. Evidence for each recommendation was
Recommended Reading: New York Times Lyme Disease
Who Gets Lyme Disease
Anyone bitten by an infected deer tick can get Lyme disease. Most U.S. cases of Lyme disease happen in Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin. But Lyme disease is also found in other parts of the U.S., Europe, and Asia.
Other things that might increase a person’s risk include:
- spending a lot of time outdoors in tall grass, brush, shrubs, or wooded areas
- having pets that may carry ticks indoors
- activities such as yardwork, hiking, camping, fishing, or hunting in tick-infested areas
Racial Differences In Incidence
Lyme disease is reported primarily in whites, although it occurs in individuals of all races. No genetic explanation is known for this the disparity most likely stems from social or environmental factors and possibly to the fact that erythema migrans is more difficult to diagnose in dark-skinned individuals.
Also Check: Snow Plowing East Lyme Ct
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Can You Get Lyme Disease Without A Tick Bite

Lyme disease can only be transmitted when an infected tick bites you. It means that you cannot be infected even by close contact with a person who currently has the infection. Clinical trials aim to develop a new drug or vaccine for Lyme disease. These trials require participants subject to some requirements to help with the studies. If you are interested in participating in one of the clinical trials, visit Power to help you match with a clinical trial according to your condition and location. Anonymous Online Contributor
Read Also: How To Control Lyme Disease
Recommended Reading: Can You Get Disability For Lyme Disease