What Are The Treatments For Lyme Disease
Lyme disease is treated with antibiotics. The earlier you are treated, the better it gives you the best chance of fully recovering quickly.
After treatment, some patients may still have pain, fatigue, or difficulty thinking that lasts more than 6 months. This is called post-treatment Lyme disease syndrome . Researchers don’t know why some people have PTLDS. There is no proven treatment for PTLDS long-term antibiotics have not been shown to help. However, there are ways to help with the symptoms of PTLDS. If you have been treated for Lyme disease and still feel unwell, contact your health care provider about how to manage your symptoms. Most people do get better with time. But it can take several months before you feel all better.
Treatment For Erythema Migrans
People treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely. Early diagnosis and proper antibiotic treatment of Lyme disease can help prevent late Lyme disease.
Treatment regimens listed in the following table are for the erythema migrans rash, the most common manifestation of early Lyme disease. These regimens may need to be adjusted depending on a persons age, medical history, underlying health conditions, pregnancy status, or allergies. Consult an infectious disease specialist regarding individual patient treatment decisions.
| Age Category | |
|---|---|
| 100 mg, twice per day orally | N/A |
| 500 mg, three times per day orally | N/A |
| 500 mg, twice per day orally | N/A |
| 4.4 mg/kg per day orally, divided into 2 doses | 100 mg per dose |
| 50 mg/kg per day orally, divided into 3 doses | 500 mg per dose |
| 30 mg/kg per day orally, divided into 2 doses | 500 mg per dose |
*When different durations of antibiotics are shown to be effective for the treatment of Lyme disease, the shorter duration is preferred to minimize unnecessary antibiotics that might result in adverse effects, including infectious diarrhea and antimicrobial resistance.
NOTE: For people intolerant of amoxicillin, doxycycline, and cefuroxime, the macrolide azithromycin may be used, although it is less effective. People treated with azithromycin should be closely monitored to ensure that symptoms resolve.
Clinical Signs Of Lyme Disease In Dogs
It has been suggested that in dogs, neurologic manifestations and myocarditis may be associated with Lyme disease, but these manifestations are uncommon and poorly understood. In dogs co-infected with other tick-borne pathogens , overall clinical signs can be worse and treatment complicated. Although cats in Lyme disease-endemic areas are commonly seropositive for B. burgdorferi, findings of associated clinical disease are rare or unclear. In cats experimentally infected with B. burgdorferi, no signs of clinical disease were observed 14 however, some practitioners in highly Lyme diseaseendemic areas report having seen cats displaying clinical signs of Lyme disease.15,16
Also Check: Natural Ways To Get Rid Of Lyme Disease
Second Stage: Early Disseminated Lyme Disease
If not detected and treated during the first stage of Lyme disease, it can develop into an early disseminated infection. This stage takes place about one to four months after the initial infection. At this point, the Lyme disease is no longer localized and has spread throughout other parts of the body.
Youll likely still have flu-like symptoms that make you feel tired, achy, and feverish. You may also still have a rash, which can even multiply and spread to other areas of your skin. You will likely also start to experience some of the following symptoms:
· Conjunctiva
· Dizziness, which may be accompanied by fainting
· Heart palpitations and other heart issues
· Brain fog
· Joint pain and swelling
· Pain and numbness in the arms and legs
· Multiple rashes throughout the body
· Sleep issues and extreme fatigue
· Paralysis of facial muscles
Complications Of Untreated Lyme Disease
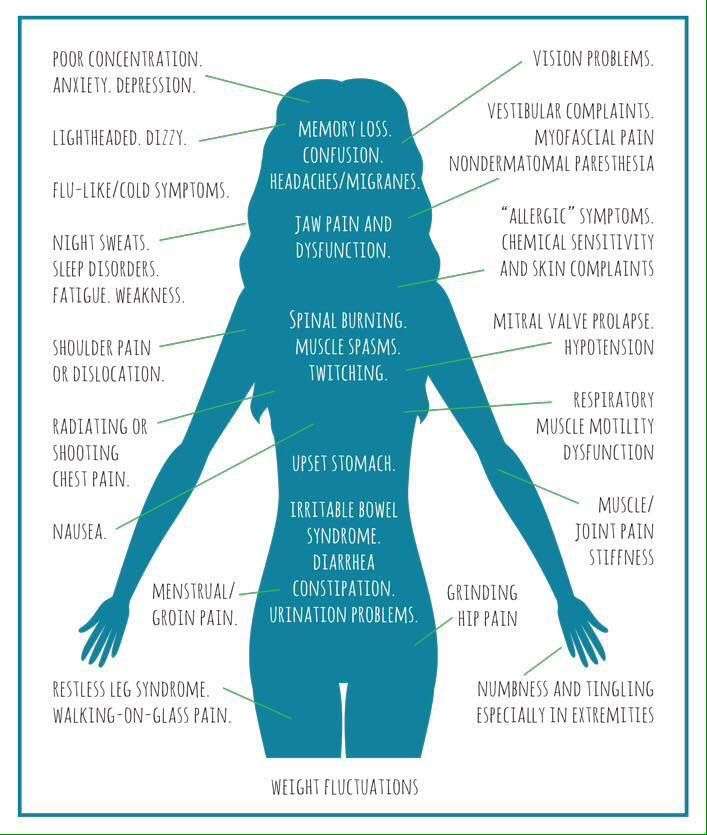
If unchecked, the Lyme disease infection can spread to other bodily systems, causing significant damage. Untreated, complications of this condition can be very severe:
- Arthritis:Prolonged infection with Lyme disease leads to chronic joint inflammation and swelling, usually in the knees . These symptoms tend to arise within two years of infection, with periods of flare-ups and remissions. This arthritis is relatively difficult to manage, though antibiotics and steroids may be attempted.
- Lyme carditis:If the bacteria reach the heart tissues, they can cause inflammation and lead to heart block. The electrical signals being sent between the upper and lower chambers of the heart are interrupted, impairing the coordination of the heartbeat. Though disruptive, this is rarely fatal.
- Lyme neuroborreliosis:Inflammation of multiple nerves, including those in the spine and brain, is the chief characteristic of this condition. This can also affect the meningesthe layer of tissue surrounding the brain and spineleading to meningitis, among other conditions. Antibiotic therapy, if applied promptly, tends to be effective as a treatment.
Even in cases where Lyme disease has progressed, antibiotic regimensespecially drugs like doxycyclineare generally successful in resolving problems.
Recommended Reading: What Is The Best Antibiotic To Treat Lyme Disease
Transmission Of Lyme Disease In Dogs
B. burgdorferi is transmitted through the bite of an infected Ixodes tick. In the United States, the primary tick vector of B. burgdorferi is I. scapularis, the blacklegged or deer tick . Over the past 20 years, the geographic distribution of I. scapularis ticks has more than doubled, and ticks of this species are now found throughout the eastern half of the United States .1 Expansive white-tailed deer populations in this area provide an ample supply of hosts favored by adultI. scapularis ticks. However, although white-tailed deer support local I. scapularis tick populations, they do not serve as a transmission reservoir for B. burgdorferi. Lyme disease also occurs in the western United States, where the primary vector of B. burgdorferi is the I. pacificus tick.
Figure 1. Adult female Ixodes scapularis tick. Photo courtesy Dr. Michael Dryden.
Figure 2. Estimated distribution of Ixodes scapularis tick populations, United States.3
B. burgdorferi is rarely transmitted from an adult female tick to her offspring. Ticks most commonly become infected as juveniles after a bloodmeal on an infected wildlife host . Because ticks typically feed only one time per life stage, the next opportunity for B. burgdorferi transmission is during the next bloodmeal in the ticks next life stage.
Lyme Disease In Horses: Symptoms Treatment And Prevention
Grooming your horse every day and checking for ticks is one of the best preventative measures against Lyme disease. PHOTO: Andrea Caudill
May 20, 2021 | Showing , Timed Events , Trail Riding , Ranching | Ranching , Healthcare and medication , Ranching , Showing , Horse Health and care
The signs can be vague and mysterious. A thumbnail-size lump on the body, general lethargy and sore joints could point to anything or nothing at all, which is exactly the problem posed by Lyme disease in horses, which can present as a number of rather generic symptoms.
If you live in an area where ticks are common, Lyme disease is a possibility for humans and horses alike. While it is usually a treatable disease, it is one where an ounce of prevention is the best option.
Don’t Miss: What Is The Effects Of Lyme Disease
Third Stage: Late Disseminated Lyme Disease
The final, and most severe, stage of Lyme disease is the late disseminated stage. At this point, the infection is now considered chronic and the harmful bacteria has made its way throughout the rest of your body.
People may reach this stage if no proper treatment is successfully administered within four months of being infected. When Lyme disease has reached this point, it can greatly affect your quality of life and make everyday activities and movements very painful and difficult. Stage-three Lyme disease can affect almost every aspect of your life, from your gut health and hormone levels to your immune system and heart condition.
Many of the symptoms listed in stage two progress to a more serious state. For instance, joint pain can develop into chronic arthritis, most often in the knees. Numbness and tingling sensations can spread to other parts of your body, like your back, hands, and feet.
Brain fog symptoms are likely to worsen, making it increasingly difficult to recall certain events or to remain concentrated on one task. You may even experience problems speaking and continue to struggle getting decent sleep at night. Some people with experience mood issues with Lyme disease that can make you feel like you have depression or anxiety which may not be connected to a psychiatric disorder and can lead to a misdiagnosis from a mental health professional.
Should I Get Tested By The Nhs Or A Privately Funded Laboratory Is There A Difference
If patients have a recent tick exposure but no bulls eye rash, guidance to NHS doctors in England is to take a blood sample and send it for testing at an NHS or UKHSA laboratory.
The tests work by looking for antibodies that a person infected with Lyme disease would produce.
The antibodies take some time to reach levels that can be detected,therefore, tests carried out within the first 4 weeks of infection may be negative and may need to be repeated on a fresh blood sample taken 4 to 6 weeks after the first test.
We recommend people exercise caution with private tests and speak to their NHS doctor for advice before spending money on private tests or treatments, as some private laboratories and clinics offer tests and treatments for Lyme disease which may not be supported by scientific evidence.
Diagnostic tests done outside the NHS may also produce false positives where the test shows positive for Lyme disease when the patient doesnt actually have it. Our advice is to seek help through the NHS.
Also Check: How Many Hbot Sessions For Lyme
What Are The Symptoms Of Chronic Lyme Disease
Home » Tick Talk » What Are the Symptoms of Chronic Lyme Disease?
Despite some skepticism in the medical community, chronic Lyme disease is a growing epidemic in the U.S. This stems partly from the shortcomings of many of the officially recommended Lyme disease tests, which leave too many patients with untreated infections that then become persistent and debilitating.
The following article will cover what you should know about chronic Lyme and provide an introductory but non-exhaustive chronic Lyme disease symptoms checklist.
How Lyme Disease Is Identified In Horses
The identification and treatment of the most common form of Lyme disease starts with diagnostics.
When we have a horse that has signs that we think could be compatible with Lyme disease, the next step is actually to rule out all the other causes that could be causing it, Dr. DeNotta says.
A veterinarian typically starts with a complete physical exam, blood work, lameness exam and diagnostic workup.
Its what we call a diagnosis of exclusion, Dr. DeNotta says. The reason for that is most of the time, its something else .
The veterinarian first must rule out the most common reasons causing whatever abnormality the horses owner is reporting.
An additional difficulty is that the bacteria doesnt show in high concentrations in easily sampled fluids, such as blood, which would allow for a direct test. This is why the blood work is checked for, among other things, the antibody levels.
However, if all those reasons have not proven compatible, and the horse has antibody levels indicating a past or ongoing borrelia infection, the veterinarian at that point might look to Lyme disease and recommend treatment.
Recommended Reading: Hyperbaric Chamber Treatment For Lyme Disease
Better Treatment Starts With Better Testing
If these celebrity Lyme stories tell us anything, its that Lyme can strike anyone, anywhere, any time. As a premier testing lab dedicated to better diagnostic outcomes, IGeneX appreciates these candid discussions of Lyme, chronic Lyme, and other tick-borne diseases. These famous Lyme cases remind us that with the right treatment, there is a light at the end of the tunnel when it comes to Lyme.
The key to getting the right treatment is getting the right diagnosis and that requires highly accurate, sensitive testing technology. Learn about the Lyme disease tests available at IGeneX today.
Chronic Lyme: What Happens When Lyme Goes Untreated
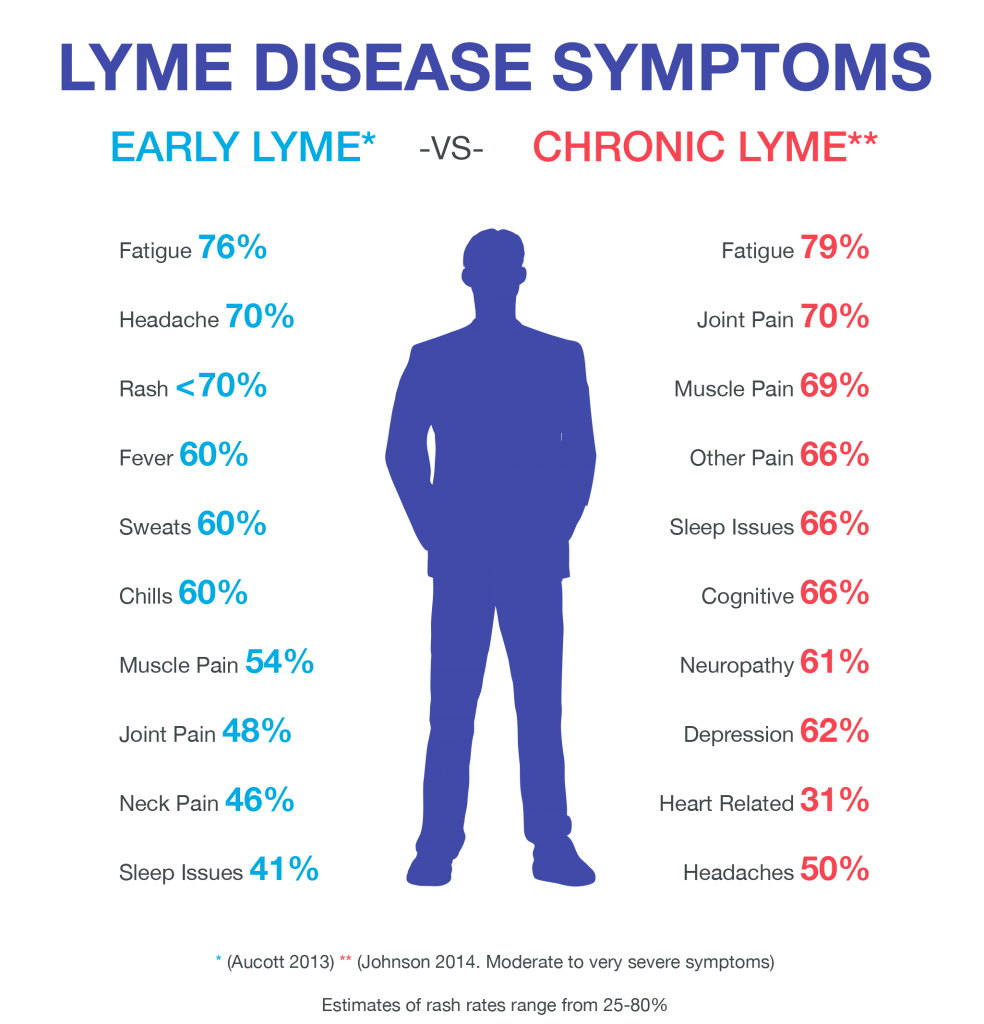
The Lyme community typically uses the term chronic Lyme disease to describe a range of physical, cognitive, and emotional symptoms that crop up after getting Lyme disease and persist for months to years after infection.
The risk of chronic Lyme increases the longer a Lyme infection goes untreated or undertreated. In other words, patients are more likely to recover fully if their Lyme infection is detected and treated as early as possible after the discovery of a tick bite. This stage is usually marked by symptoms such as fevers, chills, muscle aches, and sometimes rashes.
When left untreated or undertreated, however, Lyme disease can spread throughout the body and affect:
- The central nervous system
- Muscles and joints
As Lymedisease.org points out, these symptoms can evolve, disappear, and reappear at different times.
Read Also: Does Lyme Disease Always Have A Rash
What Are The Second Stage Signs And Symptoms Of Lyme Disease
The symptoms of second stage, early disseminated, Lyme disease can be difficult to attribute. Symptoms include severe fatigue, fever, pain, intermittent weakness and achiness of the muscles and joints, numbness in arms and legs, vision changes, and cognitive dysfunction such as short-term memory difficulties and problems multitasking. These symptoms are not specific for Lyme disease and can make the diagnosis of second stage Lyme disease very challenging.
More recognizable Lyme disease nervous system manifestations include facial paralysis , or meningitis with severe headache and stiff neck. Notable cardiac manifestations include passing out or feeling faint from an abnormally slow heart rate, irregular heart palpitations, or unexplained difficulty tolerating exercise. Meningitis and carditis are both potentially serious Lyme disease conditions and warrant immediate medical attention.
The Stages Of Lyme Disease And Their Accompanying Symptoms And How You May Still Miss Them
Lyme Disease comes in three stages, each of which has their own distinct symptoms .
Localized Lyme Disease or Stage 1: Days to weeks after the tick bite, Borrelia Burgdorferi haven’t yet spread through your body, and you are likely to experience flu-like symptoms. A fever, muscle and joint pain, a stiff neck, headaches, and a feeling of general malaise may plague you. The much talked-about “bull’s eye rash” can act as a tell-tale sign to get yourself to a doctor, but make no mistake it doesn’t show up in everyone.
Alaine didn’t have a bull’s eye rash, and never saw the tick who gave her Lyme Disease. This is more common than you may think. Like her, you may dismiss these symptoms as a flu, some random virus, an integral part of getting older, or having an overly busy life things you wouldn’t ordinarily seek medical help for.
Early disseminated Lyme Disease or Stage 2: Borrelia Burgdorferi are making their way through your system, and weeks to months after your unwanted encounter with a tick, you may experience pain and numbness, Bells palsy , heart palpitations, shortness of breath, and chest pain. You’ll begin to catch on that something is wrong, but by this time, a tick bite may not be anywhere on your mind even if you knew you were bitten, and you may get lost in the battery of diagnostic tests.
Don’t Miss: Best Medication For Lyme Disease
Is Chronic Lyme Disease Real
- Post author:Dr. John Dempster, ND
As long as we wish to be surrounded by nature and trees, we have to accept the possibility of tick bites and tickborne diseases. And even though many are harmless and cause no noticeable symptoms, there are bacteria, like Borrelia burgdorferi that transmit serious diseases like Lyme disease.
Lyme disease the most commonly transmitted tick-borne infection in North America wasnt recognized as a medical condition until very recently, just some 40-45 years ago! This is even more surprising considering that the bacteria causing Lyme disease has been lurking around for thousands of years. Excavation of a 5,300 year-old mummy, called an Iceman, confirmed that our ancestors also suffered from B. burgdorferi and possibly even Lyme disease.
But it wasnt until the 1960-70s when Lyme disease gained public attention after children in Lyme, Connecticut started having unexplainable symptoms like fatigue, skin rashes, fever, arthritis, etc. If it wasnt for two persistent mothers who pushed the Connecticut State Department of Health to look into this outbreak, we might have still been oblivious to this serious medical condition.
Warning Signs Of Lyme Disease To Be Aware Of
Ever come back home from a pleasant trip out to the fields or woods on a nice, summer day only to discover youve brought along an unwelcome visitor? Ticks can be quite a nuisance. They grab hold of the flesh with their little mouths, latching on with a strong bite. Then, the blood-sucking begins. Worse than the fear of a little vampire-like insect feasting on your blood, though, is the potential threat they carry within their own bodies.
Lyme disease.
This disease is an infection caused by the bacterium Borrelia burgdorferi found in black-legged ticks. At first, the symptoms start off simple and largely unnoticeable. Left untreated, however, and the effects can be painful and long-lasting.
Read on to learn the symptoms and how to treat Lyme disease.
Read Also: What To Do If I Have Lyme Disease
Target Areas Of Lyme Disease
The Center for Disease Control has reported that 95% of cases in 2015 for Lyme disease took place in the following 14 states:
- Connecticut
- Virginia
- Wisconsin
If you reside in or plan to visit one of these states, its vital for your health to always be cautious of black-legged ticks. As a precaution, its best to wear long socks, pants, and long-sleeved shirts.
After every outing, be sure to check any exposed areas of your body for ticks. If you discover a tick on your body, follow these steps for removal and disposal as quickly as possible:
Be on the lookout for any of the symptoms described below, and contact your doctor should you experience any of them. Your doctor will know best how to treat Lyme disease.