Natural Remedies For The Chronic Inflammation Of Lyme Disease
Everyone knows that inflammation isnt good, especially when it becomes chronic. But to do something about it, you need to understand whats driving the inflammation in the first place.
Though you cant actually see chronic inflammation, you can certainly feel it. It manifests as joint discomfort, stiffness, general achiness, fatigue, low stamina, brain fog, slow mental activity, depressed mood, and all the other symptoms associated with chronic Lyme disease. Simply put, you feel inflamed.
The root of inflammation is excessive turnover of cells. We all lose cells, and up to a certain point, its perfectly normal. Cells in the body are constantly wearing out, getting injured, or being invaded by microbes. In fact, we typically lose 50-70 billion cells every day. While much of cellular turnover is accounted for by cells that are shed from the body, such as skin and intestinal cells, tissues inside the body are losing cells, too.
When cells die, they break apart and create debris. If enough debris collects in tissues, it obstructs the flow of water, nutrients, and oxygen that cells need to stay healthy. At the same time, metabolic waste produced by cells is trapped around the cell, which, of course, isnt a good thing. If enough debris collects, cells start to choke in their own waste.
Chronic Lyme Disease: Symptoms Causes And Coinfections
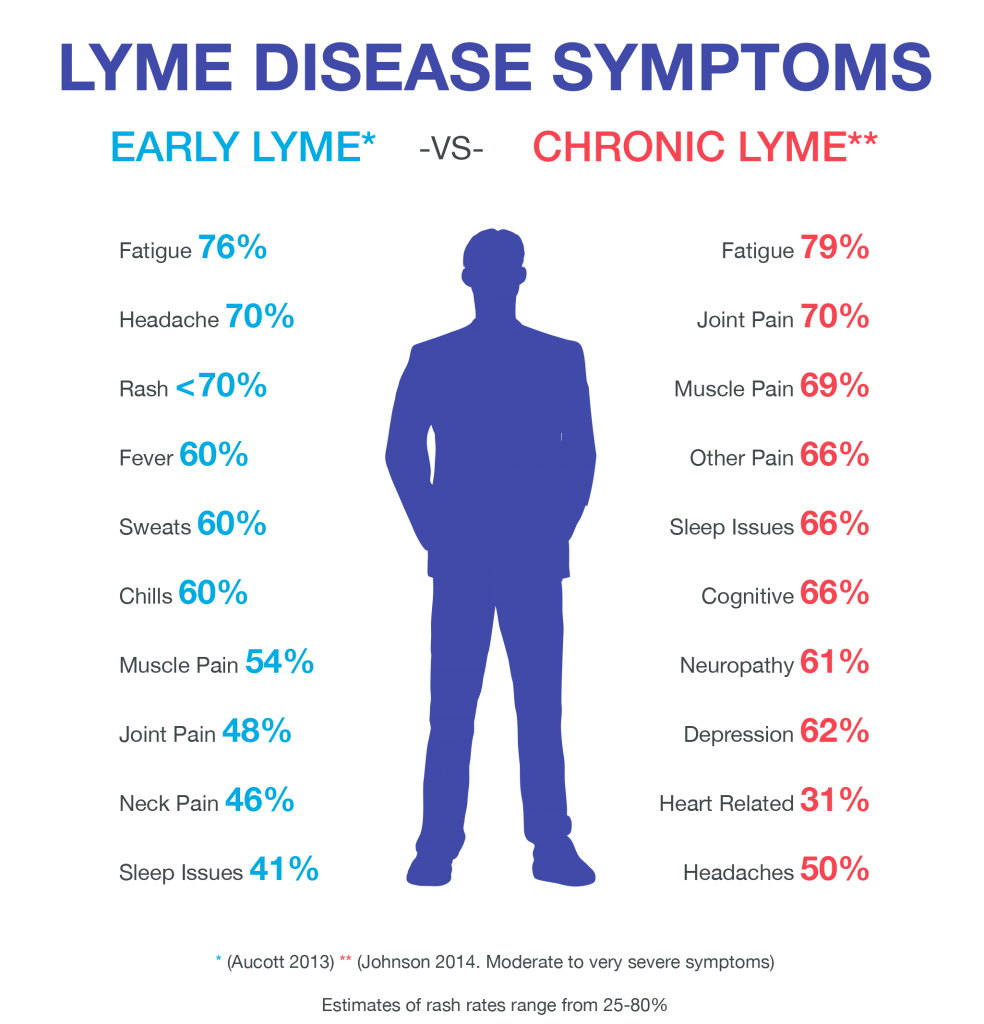
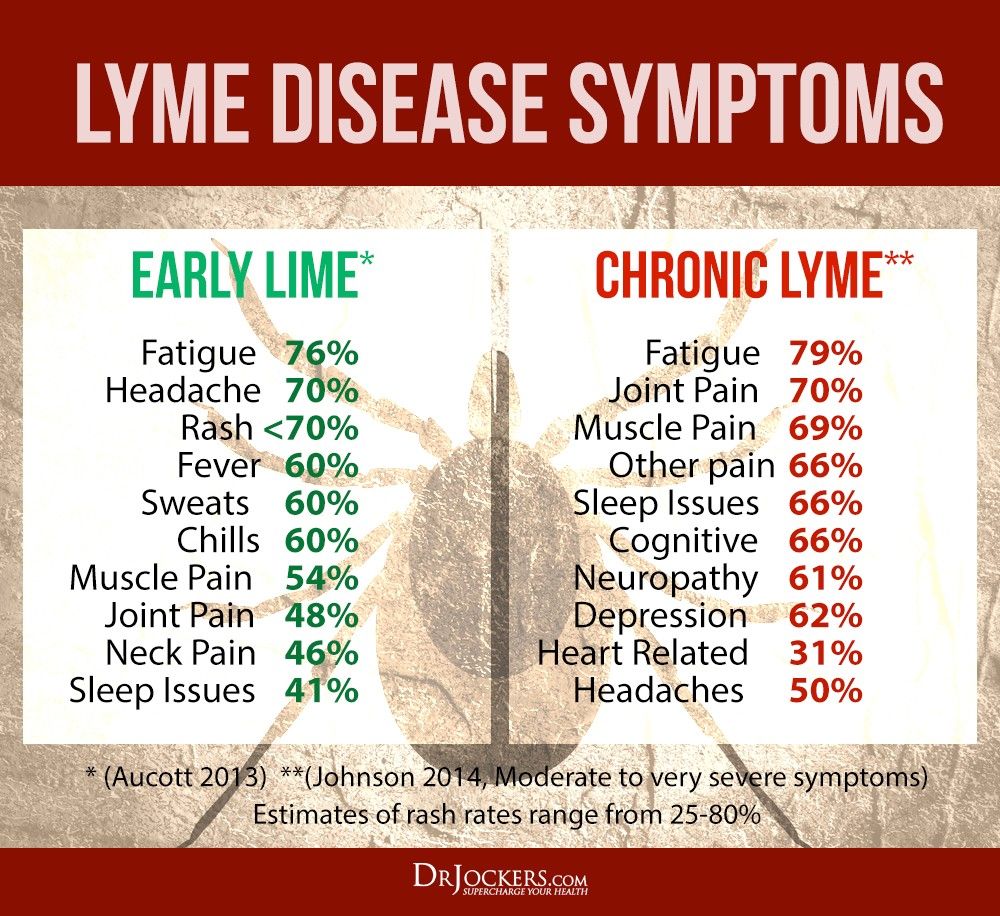
Are you experiencing fatigue, headaches, joint pain, muscle aches, sleep issues, memory and concentration troubles, neurological issues, body pains, or other chronic symptoms without a known explanation? You may have chronic Lyme disease.
Chronic Lyme disease is increasingly prevalent and a very serious health issue. It is caused by Borrelia burgdorferi bacteria transmitted by infected ticks. When Lyme disease is not diagnosed and properly addressed during the acute phase during the first weeks, it can turn chronic leading to countless symptoms and health complications.
Unfortunately, testing is not reliable and the conventional medical community is not equipped to adequately address this rampant health issue. Fortunately, there are Lyme-literate healthcare professionals, like myself, who can help you to get the right diagnosis. You can overcome chronic Lyme disease following some natural supports strategies and using a 6-month protocol.
In this article, you will learn what Lyme disease is and the difference between acute and chronic Lyme disease. You will understand the symptoms of chronic Lyme disease. I will explain what co-infections you may encounter if you have chronic Lyme disease. I will discuss the problems with standard testing methods and offer more reliable testing alternatives. I will offer some natural support strategies to get started with.
When Should I See My Healthcare Provider
If you feel sick after having spent time in areas where ticks might live, you should make an appointment with your healthcare provider.
If you received a Lyme disease diagnosis and you dont feel well after taking all of your antibiotics, contact your provider. This is especially true if you have symptoms like a stiff neck or mental confusion.
Read Also: Lyme Disease In Dogs Cure
Major Symptoms Of Chronic Lyme Disease
Chronic Lyme disease may have a variety of symptoms that can be easily confused with fibromyalgia, autoimmune conditions, chronic fatigue syndrome, psychosomatic illness, or mental health issues. Unfortunately, without proper diagnosis and treatment, chronic Lyme disease gets worse over time and people with chronic Lyme may never recover without adequate treatment.
It is critical that if you experience the following symptoms, you work with a doctor that is well-versed in chronic Lyme disease so you can receive the right diagnosis, get started with proper treatment, relieve your symptoms, and recover from the condition. Major symptoms of chronic Lyme disease that you need to pay attention to may include but not limited to:
- Other chronic health issues
What Are The Stages Of Lyme Infection
There are three stages:
- Early localized Lyme: Flu-like symptoms like fever, chills, headache, swollen lymph nodes, sore throat, and a rash that looks like a bulls-eye or is round and red and at least 2 inches long
- Early disseminated Lyme: Flu-like symptoms like pain, weakness, or numbness in your arms and legs, changes in your vision, heart palpitations and chest pain, a rash , and a type of facial paralysis known as Bellâs palsy
- Late disseminated Lyme: This can happen weeks, months, or years after the tick bite. Symptoms might include arthritis, severe fatigue and headaches, dizziness, trouble sleeping, and confusion.
About 10% of people treated for Lyme infection donât shake the disease. They may go on to have three core symptoms: joint or muscle pain, fatigue, and short-term memory loss or confusion. This is called post-treatment Lyme disease syndrome. It can be hard to diagnose because it has the same symptoms as other diseases. Plus, there isnt a blood test to confirm it.
Experts arenât sure why Lyme symptoms donât always go away. One theory is that your body keeps fighting the infection even after the bacteria are gone, like an autoimmune disorder.
Don’t Miss: Will I Always Have Lyme Disease
Symptoms In Early Disseminated Lyme Disease
Early disseminated Lyme disease occurs days to months after infection, in which the bacteria have begun to spread. There is a wide range of possible symptoms at this stage, including:
- Severe headaches and neck stiffness
- Lyme Arthritis, especially in the knees or other large joints
- Muscle aches and joint pains
- Heart palpitations or shortness of breath
- Facial paralysis on one or both sides
- Numbness or tingling in the hands or feet
- Severe Extreme fatigue
Signs And Symptoms Of Untreated Lyme Disease
Seek medical attention if you observe any of these symptoms and have had a tick bite, live in an area known for Lyme disease, or have recently traveled to an area where Lyme disease occurs.
Untreated Lyme disease can produce a wide range of symptoms, depending on the stage of infection. These include fever, rash, facial paralysis, and arthritis.
The appearance of the erythema migrans rash can vary widely.
- Fever, chills, headache, fatigue, muscle and joint aches, and swollen lymph nodes may occur in the absence of rash
- Erythema migrans rash :
- Occurs in approximately 70 to 80 percent of infected persons
- Begins at the site of a tick bite after a delay of 3 to 30 days
- Expands gradually over several days reaching up to 12 inches or more across
- May feel warm to the touch but is rarely itchy or painful
- Sometimes clears as it enlarges, resulting in a target or bulls-eye appearance
- May appear on any area of the body
- Does not always appear as a classic erythema migrans rash
Swollen Knee
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of the body
- Arthritis with severe joint pain and swelling, particularly the knees and other large joints.
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or an irregular heart beat
- Episodes of dizziness or shortness of breath
- Inflammation of the brain and spinal cord
Links with this icon indicate that you are leaving the CDC website.
Also Check: Elisa Test For Lyme Disease
What Should You Do If You Find A Tick
-
Dont touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Dont squeeze the tick, and dont use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
Symptoms Of Lyme Disease
A circular or oval shape rash around a tick bite can be an early symptom of Lyme disease in some people.
The rash can appear up to 3 months after being bitten by an infected tick, but usually appears within 1 to 4 weeks. It can last for several weeks.
The rash can have a darker or lighter area in the centre and might gradually spread. It’s not usually hot or itchy.
The rash may be flat, or slightly raised, and look pink, red, or purple when it appears on white skin. It can be harder to see the rash on brown and black skin and it may look like a bruise.
LARRY MULVEHILL/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259371/view
Some people also get flu-like symptoms a few days or weeks after they were bitten by an infected tick, such as:
- a high temperature, or feeling hot and shivery
- tiredness and loss of energy
Some people with Lyme disease develop more severe symptoms months or years later.
This is more likely if treatment is delayed.
These more severe symptoms may include:
- pain and swelling in joints
- nerve problems such as pain or numbness
- trouble with memory or concentration
Recommended Reading: Lyme Disease More:for_patients
Which Areas Are More Likely To Have It
The tick that causes Lyme disease has been moving from the Northeast and upper Midwest into the Southern and Western U.S., Mexico, and Canada. Cases in California and Florida are on the rise. After a drop between 2017 and 2018, the numbers jumped a little bit in 2019.
But most Lyme cases in 2019 were in 15 states: Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New
Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, West Virginia, and Wisconsin. Washington, DC, is also a hotspot.
In 2019, Pennsylvania had the most Lyme infections, with 6,763. New York was next, with 2,847 cases.
In the Southern U.S., where itâs hotter, ticks stay under leaves so they dont dry out. This means people donât get Lyme from Southern ticks very often because they dont usually come out to bite.
Even though people only report about 30,000 cases of Lyme infection in the U.S. each year, there are actually around 476,000 a year. The same tick also can spread other diseases, including babesiosis, anaplasmosis, and Powassan virus. Those diseases are also on the rise in the U.S.
Whoâs likeliest to get Lyme disease?
Boys up to age 15 and men between the ages of 40 and 60 are the most likely to get Lyme disease. Thatâs because they tend to play outside and go camping, hunting, and hiking.
Why are there more ticks now than there used to be?
There are several reasons why Lyme is spreading. Some of these are:
Chronic Lyme: What Happens When Lyme Goes Untreated
The Lyme community typically uses the term chronic Lyme disease to describe a range of physical, cognitive, and emotional symptoms that crop up after getting Lyme disease and persist for months to years after infection.
The risk of chronic Lyme increases the longer a Lyme infection goes untreated or undertreated. In other words, patients are more likely to recover fully if their Lyme infection is detected and treated as early as possible after the discovery of a tick bite. This stage is usually marked by symptoms such as fevers, chills, muscle aches, and sometimes rashes.
When left untreated or undertreated, however, Lyme disease can spread throughout the body and affect:
- The central nervous system
- Muscles and joints
As Lymedisease.org points out, these symptoms can evolve, disappear, and reappear at different times.
Also Check: How Many Ozone Treatments For Lyme
Get Regular Light Movement
Moving your body is very important for your health. It strengthens your immune system, supports your lymphatic pathways, aids detoxification, supports your muscles and joints, and enhances your mental health.
However, it is important that you only do light movement and not high-intensity exercise while you are healing to preserve your bodys energy for rest and repair. I recommend stretching, yoga, Tai Chi, pilates, or light walks daily. Listen to your body and be gentle with yourself.
How To Remove Ticks

Tick bites aren’t always painful. You may not notice a tick unless you see it on your skin. Check your skin and your children’s or pets’ skin after being outdoors.
To remove a tick:
The risk of getting ill is low. You don’t need to do anything else unless you become unwell.
You May Like: Lyme’s Disease In Dogs Symptoms
Lyme Disease Rashes And Look
Circular, expanding rash with target-like appearance.
Expanding rash with central crust
Expanding lesion with central crust on chest.
Expanding erythema migrans
Photo Credit: Reprinted from Bhate C, Schwartz RA. Lyme disease: Part I. Advances and perspectivesexternal icon. J Am Acad Dermatol 2011 64:619-36, with permission from Elsevier.
Description:Early, expanding erythema migrans with nodule.
Multiple rashes, disseminated infection
Early disseminated Lyme disease multiple lesions with dusky centers.
Red, oval plaque
Red, expanding oval-shaped plaque on trunk.
Expanding rash with central clearing
Circular, expanding rash with central clearing.
Bluish hued rash, no central clearing
Bluish hued without central clearing.
Expanding lesion, no central clearing
Expanding lesion without central clearing on back of knee.
Red-blue lesion with central clearing
Red-blue lesion with some central clearing on back of knee.
Insect bite hyper-sensitivity
Large itchy rash caused by an allergic reaction to an insect bite.
Fixed drug reaction
Description:A skin condition that occurs up to two weeks after a person takes a medication. The skin condition reappears at the same location every time a person takes that particular medication.
Ringworm
Description:Ringworm is a common skin infection that is caused by a fungus. Its called ringworm because it can cause a ring-shaped rash that is usually red and itchy with raised edges.
Pityriasis rosea rash
Granuloma annulare rash
Can An Animal Get Infected Despite Being Vaccinated
Yes. This has been observed that some animals can still get infected after Lyme vaccination. This can be due to a low immune response of the respective animal and/or a very high exposure rate or Lyme prevalence in the area where the animal lives. A yearly check of the OspA titer is recommended for a vaccinated animal to ensure that the animal responded with high OspA antibodies to vaccination. Please indicate the name of the vaccine and when it has been last applied on the accession form.
Recommended Reading: Orthopedic Partners East Lyme Ct
Does Lyme Disease Treatment With Antibiotics Affect Antibody Levels
Antibiotic treatment affects the pathogen . It does not directly influence antibody titers. However, if the treatment is successful and bacteria are removed from the host, the B-cells are not further triggered to produce new antibodies. As a consequence antibodies levels decrease after treatment. Thus, antibody levels are indicators of treatment success .
When To See Your Gp
You should contact your GP or dial NHS 111 promptly if you feel unwell with any of the symptoms described above after being bitten by a tick or after spending time in areas where ticks may live.
Take this leaflet with you if you are unsure what to say and remember to let your GP know if youve recently had a tick bite or spent time in areas where ticks may live.
Diagnosing Lyme disease can be difficult as many of the symptoms are similar to other conditions. A spreading erythema migrans rash appearing some days after a known tick bite is characteristic and should be treated with antibiotics.
If you dont have this rash but do have other symptoms of Lyme disease, blood tests can be carried out that look for antibodies against the borrelia bacteria.
Blood tests can be negative in the early stages of the infection as the antibodies take some time to reach levels that can be detected.
You may need to be re-tested if Lyme disease is still suspected 4 to 6 weeks after a first negative test result.
If you have long-lasting symptoms, you may be referred to a specialist in microbiology, infectious diseases, rheumatology, or neurology as appropriate for further investigation and management.
You May Like: Natural Antibiotics For Lyme Disease
Antibiotics And Alternative Medicine
Of course, LLMDs would beg to differ. Many maintain that one of the best ways to treat chronic Lyme patients is with a long-term course of antibiotics, claiming the typical month-long course of treatment isnt enough to eradicate the disease in certain individuals.
Londons Lyme Disease Clinic founder and medical director Dr Joshua Berkowitz says: Long-term treatment with antibiotics is necessary to target and kill all the different pleomorphic forms of the bacteria and parasitic infections associated with chronic Lyme disease. Most of these bacteria have the ability to survive based on different mechanisms and they can easily change their shape and surface.
They can hide in other body cells and in intracellular spaces, plus they can invade specific tissues like connected tissue where there is no presence of immune cells which can kill them off. With the support of antibiotics we are able to take care of all these escape mechanisms, but it requires long-term treatment to do so.
Many chronic Lyme patients given a long-term course of antibiotics report feeling better afterwards. But, feeling better on an antibiotic is not a sure fire way to establish that it has actually killed a harmful bacteria, and some argue this approach can actually be dangerous.
A 2015 report in Clinical Infectious Diseases found that the efficacy for these unconventional treatments could not be supported by scientific evidence, and many could potentially be harmful.
For Animals That Have Not Been Vaccinated Can Osp A Values Be Positive How Should This Be Interpreted
Antibodies to OspA have previously been interpreted as markers for vaccination. Non-vaccinated animals usually have low values for antibodies to OspA, while vaccinated animals develop these antibodies. OspA antibodies have been shown to protect from infection with B. burgdorferi.
However, there is accumulating evidence that antibodies to OspA can occur without vaccination. First, residual OspA is present on the bacterial surface at the time of transmission to an animal. This causes a low and transient OspA antibody response early after infection. Second, antibodies to OspA have also been associated with treatment-resistant Lyme arthritis and with development of autoimmunity in human patients. Similarly, OspA antibodies in non-vaccinated dogs or horses can be considered as markers of chronicity and disease severity.
Also Check: What Are The Signs Of Lyme Disease