How Accurate Are Blood Tests For Lyme Disease
With about 30,000 people infected each year, Lyme disease causes a range of serious symptoms, including joint pain, chronic fatigue, facial paralysis, and in rare cases, even death. Because of these risks, anyone who is bitten by a deer tick should consider being tested for Lyme disease. Yet while lab tests are crucial for proper and perhaps life-saving treatment, they also have a low accuracy rate, leading many patients to become victims of a medical laboratory misdiagnosis.
Testing And Diagnosing For Lyme Disease
The most common testing used for diagnosing Lyme disease is the two-tiered CDC recommended tests. These include the ELISA and the Western Blot. Both are indirect tests in that they merely measure the immune systems response to an infectious agent instead of looking for evidence or components of the agent itself. Many physicians falsely yield to the CDC definition case of Lyme disease to make a diagnosis. However, these tests were originally designed for surveillance of one single species of Borrelia. The tests were never intended to be used in making clinical diagnosis. These standard Lyme tests can give false negatives between 50% and 80% of the time, depending on which study you are looking at. Even on the CDC website, they state, Lyme disease is diagnosed based on symptoms, physical findings and the possibility of exposure to ticks. Yet, despite this information, doctors are still relying on laboratory tests to definitively determine whether a patient has the disease or not. This current method of diagnosing has serious and sometimes deadly consequences for patients who indeed have Lyme disease and/or co-infections, but do not receive treatment due to a negative lab result.
There are several private labs that offer Lyme disease and other vector borne testing.
We are not medical professionals and cannot recommend any specific testing. Please consult your doctor to find the right test for you and your family.
When Is The Lyme Disease Blood Test Ordered
When someone has the signs and symptoms of Lyme disease or they live in a region that has deer ticks or black-legged ticks, then this blood test will be ordered. It will also be ordered when these symptoms occur without improvement over the course of 7-14 days by most medical providers.
- A bulls-eye rash that grows from the bite site.
- Fevers, chills, and a persistent headache that does not go away.
- Unusual and persistent fatigue that does not immediately improve.
The IgM and IgG tests are generally ordered first when Lyme disease is suspected. This is because people who have never been exposed to the bacteria that causes the disease will not have any antibodies present. If these tests are positive and followed up by a positive Western Blot test, then the chances are very good that Lyme disease is present. This is especially true if antibody levels continue to rise over time.
Recommended Reading: How Does Lyme Disease Affect The Brain
How To Remove A Tick
Testing Beyond The Lab
Certain types of symptoms require evaluation by diagnostic procedures conducted by specialists in their respective fields. These symptoms include:
- Neurological symptoms: Severe neurological symptoms are evaluated with a nerve conduction test and MRI of the brain to assess the nervous system. The purpose is ruling out multiple sclerosis.
- Cardiac symptoms: Heart symptoms like chest pain and irregular heartbeat are evaluated by EKG and Holter monitor . Findings may lead to cardiac catheterization.
- GI symptoms: Stomach pain and symptoms are often evaluated by an upper endoscopy. Lower intestinal and colon symptoms are evaluated by colonoscopy. Routine colon cancer screening with colonoscopy is recommended every 10 years for everyone over 50.
Read Also: East Lyme High School Lacrosse
Indirect Testing Can Be More Limited Than Direct Testing
Both tests used in the CDC recommended two-step process are indirect methods of diagnosismeaning they do not detect the actual Lyme disease bacteria itself but, instead, measure the bodys immune system response to the presence of disease-causing bacteria. However, a number of factors can prevent the body from producing antibodies, including the following:
- Timing: If conducted in the early stages of Lyme disease, a patients body may not have developed a sufficient enough number of antibodies to detect. This issue can be compounded by the lack of sensitivity of the ELISA test.
- Immunity Suppression: The saliva of infected ticks contains specific immune-suppressing components that can delay or prevent the activation of a persons immune response. These components are designed to prevent the body from effectively fighting off the Lyme disease-causing bacteria, so it has a chance to take hold.
- Antibiotics: If patients are taking antibiotics at the time of the Lyme disease test, they may not produce enough antibodies to be detected by the test.
- Modified Form of Borrelia: In some patients, the Borrelia bacteria will transform into a cyst, which will prevent the bodys immune system from producing antibodies.
- Weakened Immune System: False negatives can also result in patients in whom the immune system is weakened or compromised due to coinfection with another illness.
- Seronegative patients: These patients do not produce antibodies.
Investigation Of Suspected Neurological Lyme Disease
The diagnosis of neurological Lyme disease can only be confirmed by examination of the CSF and a paired serum. A definite diagnosis is based on the presence of a pleocytosis in the CSF, demonstration of intrathecal synthesis of specific antibodies to Borrelia species in CSF by comparison to serum and the presence of neurological symptoms. It is not possible to confirm intrathecal synthesis and hence definite neurological Lyme disease without a paired serum .
In 2018 RIPL is introducing a service for the detection of intrathecal synthesis of Borrelia-specific antibodies which is summarised in this flow diagram.
Clinicians may ask for guidance on laboratory testing of CSF from RIPL if required.
Also Check: How Long To Treat Lyme Disease
How To Test For Lyme Disease
There is more than one way to test for Lyme disease. The tests that are most used today include the ELISA and the Western blot test. They are designed to look for evidence that the body has responded to a Lyme disease infection rather than looking for the actual infection itself. The ELISA is typically part one of a two-step process, but it only requires one blood sample to be taken. According to the CDC, the ELISA should be ordered first prior to the Western blot.
Image by on : How do you test for Lyme disease?
Lyme Disease Diagnostics Research
There is a great need to develop rapid, point-of-care tests to determine whether people are infected with Borrelia burgdorferi, the bacterium that causes Lyme disease. NIAID is committed to improving Lyme disease diagnostics by supporting innovative research projects.
Priorities include finding potential targetssubstances that new diagnostic tools might measure in patient samplesand improving the sensitivity and specificity of currently available diagnostic tests, thereby leading to more accurate results.
Read Also: Breeds Predisposed To Lyme Nephritis
We Implement Proven Measures To Keep Your Data Safe
At HealthMatters, we’re committed to maintaining the security and confidentiality of your personal information. We’ve put industry-leading security standards in place to help protect against the loss, misuse, or alteration of the information under our control. We use procedural, physical, and electronic security methods designed to prevent unauthorized people from getting access to this information. Our internal code of conduct adds additional privacy protection. All data is backed up multiple times a day and encrypted using SSL certificates. See our Privacy Policy for more details.
Popular search
An Introduction To Lab Testing
Lyme disease tests can serve as valuable resources for the diagnosis and treatment of tick-borne disease. But its important not to get too hung up on the results.
The problem of chronic Lyme disease, cant be solved exclusively by looking at lab results, which is something I know from personal experience. In fact, becoming overly obsessed with lab results can hinder the recovery process.
Lab work provides a snapshot of whats going on inside your body. But multiple other factors including your symptoms, the length of time youve had them, and clinical presentation, as well as the environments in which you live, work, and travel all factor into making an accurate diagnosis.
Furthermore, the human body is an immensely complex biological machine, with millions of different biochemical functions happening simultaneously. Lab tests provide an ever-so-small glimpse at certain key functions of different systems in the body. From those indicators, determinations can be made about how well the body is functioning and whether illness is present.
Laboratory assessment, however, is far from absolute. Because the human body is so complex, the ability of lab testing to predict a specific chronic illness, such as one from a tick-borne disease, is often limited. All labs are subject to variability and different interpretations.
You May Like: Lyme Literate Doctor Los Angeles
Lyme Disease Is On The Rise An Expert Explains Why
May marks the beginning of the summer season when black-legged ticks that spread Lyme disease are more prevalent even in California.
Earlier this month, the U.S. Centers for Disease Control and Prevention reported that cases of tickborne diseases had more than doubled from 2004 to 2016, from 22,000 to 48,000, and that Lyme disease accounted for 82 percent of tickborne diseases.
Moreover, due to underreporting, the actual number of Lyme disease cases is estimated to be significantly higher likely more than 350,000 in 2016.
We talked to infectious disease expert Charles Chiu, MD, PhD, about the rise in Lyme disease cases, better diagnostic tests on the horizon and what you need to know to protect yourself from infection. Chiu is an associate professor of laboratory medicine and medicine and director of the UCSF-Abbott Viral Diagnostics and Discovery Center.How common is Lyme disease in California? And why have rates been increasing?
In terms of reported cases, there are about 80 to 100 a year in the state. Residents in or travelers to the northwestern coastal counties Trinity, Humboldt, and Mendocino are at highest risk. But because of underreporting, the actual number of Lyme disease cases likely exceeds 1,000 cases a year, simply because most cases of Lyme disease are not reported.
How is Lyme disease transmitted, and is it contagious between humans?
Compared to other infections, is Lyme disease more difficult to detect and diagnose?
Borrelia burgdorferi,
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
Itâs not clear why this happens to some people and not others. This means thereâs also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and familiesâ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
Read Also: Lyme Disease Tick Testing Kit
Also Check: How Do You Know If You Got Lyme Disease
Stony Brook University Medical Center
Administered in conjunction with the Clinical Immunology Laboratory in the Department of Pathology at the Renaissance School of Medicine at Stony Brook University, the IgM and IgG Western Blot Lyme disease test is often covered by insurance. This is considered a more sensitive test if the ordering healthcare provider checks the box to include CDC non-specific bands on the Western Blot report.
How Is Lyme Disease Diagnosed How Reliable Are These Lab Tests
There are several tests available to diagnose Lyme disease. The CDC recommends using a two-part process. If the first step, called an EIA , yields a positive result or is difficult to interpret, a second step, called a Western Blot test, is used for confirmation.
Unfortunately, these and other diagnostic methods are beset by shortcomings, particularly methods which rely upon blood samples. According to the Lyme Research Alliance, Lyme disease blood testing is fraught with problems and, at best, should only be an adjunct to the clinical diagnosis of the disease a statement which appears to align with observations by medical researchers. For example, consider this excerpt from a 2012 study published in Open Neurology Journal :
In considering the diagnosis of Lyme disease, a major problem is the inability of documenting the existence and location of the bacteria. After the initial transfer of the bacteria from the Ixodes tick into the person, the spirochetes spread locally, but after an initial bacteremic phase, the organisms can no longer be reliably found in body fluids Currently, the use of circulating antibodies directed against specific antigens of the Lyme borrelia are the standard means to diagnose the disease, but specific antibodies are not an adequate means to assess the presence or absence of the organism.
- ADD
Also Check: How Long Does It Take To Transmit Lyme Disease
What Is The Most Reliable Lyme Disease Test
There is no one answer when it comes to determining which Lyme disease test is the most reliable. This is because each test looks for a different thing at a different stage of the infection. When investigating a long-term infection, tests that look for the bodys response to the infection are the most reliable, whereas for an active infection, a test that identifies the bacteria itself will be the most effective. Some tests only show up on an active infection and fail to indicate chronic Lyme, so the most reliable test option depends on which stage a persons infection is currently at.
Featured image by Emin Baycan on Unsplash
Not All Ticks Are The Same
Different species of ticks carry different types of bacteria, viruses and protozoa. However, new tick-borne infections are emerging as tick habitats change over time. For example, the deer tick is now reported in 50% of US counties by the CDC. The Lone Star tick is also on the move and expanding into the Northeastern states.TICKNOLOGY has one comprehensive tick testing panel for all ticks that threaten US residents.
Read Also: What Is It Like To Have Lyme Disease
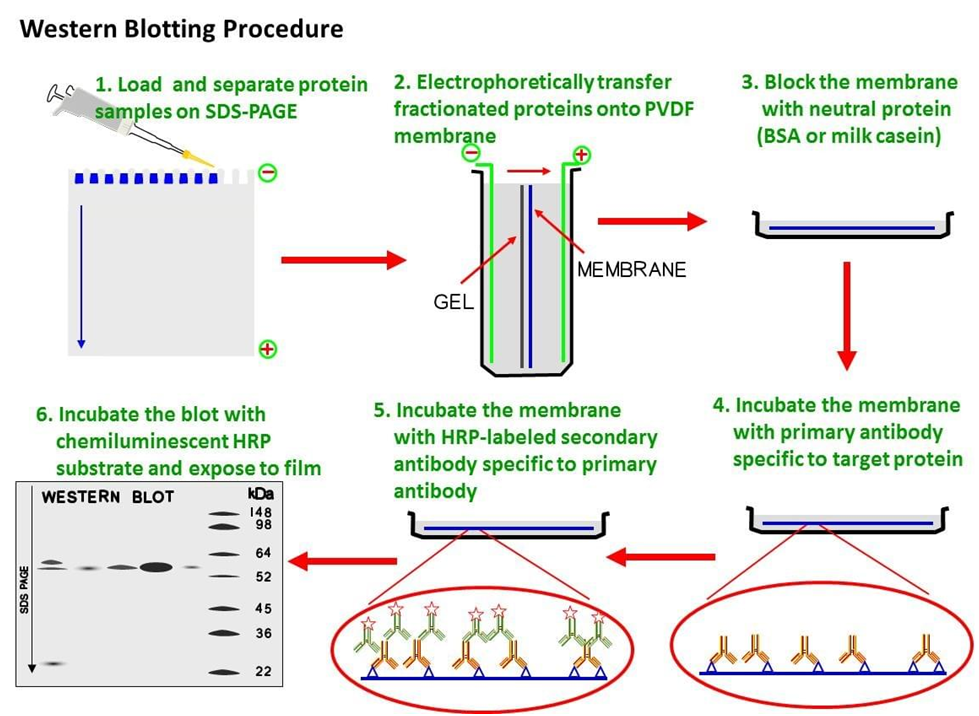
What Is The Western Blot Test
The Western blot test is also known as a protein immunoblot test or immunoblotting. It was invented in 1979 to identify ribosomal RNA binding proteins.
If you get a positive result for Lyme disease or HIV after taking an enzyme-linked immunosorbent assay test, your doctor may recommend a Western blot test to you.
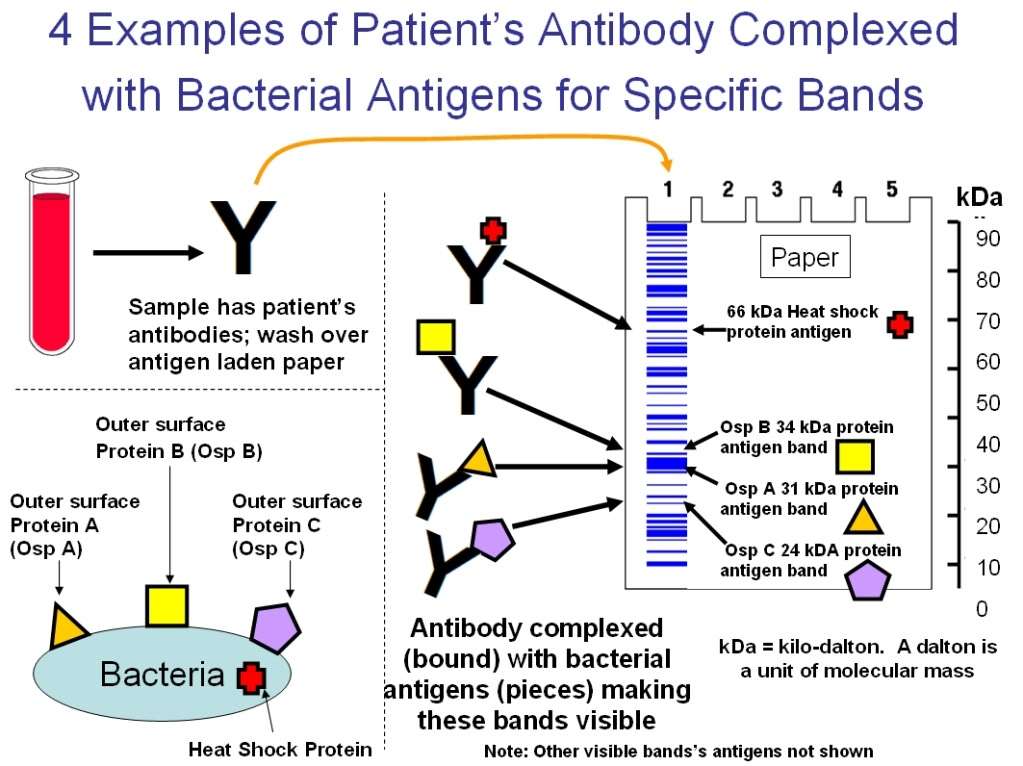
The Western blot test looks for the antibodies against an infection, not the infection itself. If you develop a viral, fungal, or bacterial infection, your body will produce proteins called antigens in response. Antigens stimulate your immune system to push out antibodies in an effort to fight the disease.
The Western blot uses a procedure called gel electrophoresis to identify and separate proteins by molecular weight and length. The proteins are placed onto blotting paper thats made from a material such as nitrocellulose.
An enzyme is added to the paper. If it causes a change in color, antibodies to a specific infection have been detected.
Since it can take several weeks or months before antibodies are found in blood, the Western blot test may not always be reliable.
The Diagnostic Accuracy Of Tests Compared To Clinical Diagnosis
Two-tier serological test vs. clinical diagnosis
Thirteen studies evaluated the two-tier serological test protocol for diagnosis of LD at different stages of disease and after antibiotic therapy. provides the meta-analytic summaries demonstrating low sensitivity, 46.3% , for early LD patients and increasing sensitivity with stage 2, 89.7% , and stage 3, 99.4%H LD. There was relatively high specificity across control groups. Most false positives within the control groups were patients with diseases known to produce antibodies that cross-react in serological tests for B. burgdorferi. Nine studies presented results for two-tier serological testing where at least one of the tests was not FDA licensed , . Heterogeneity analysis of sensitivity and specificity on the impact of using non-commercial tests was not significant. At the early stage of LD the two-tier testing method was good for ruling in LD if the patient tested positive, but had very poor predictive value for ruling out LD, which is why it is recommended to retest after 30 days . However, for convalescent patients treated at stage 1 LD sensitivity remained low even after 30 days.
Read Also: Symptoms Of Lyme Disease In Adults
The Test Isnt Designed To Detect The Exact Disease
A number of Lyme disease lab tests are designed to identify only a few species of the Borrelia bacteria that can cause Lyme disease. In the United States, for example, many tests are only designed to detect Borrelia burgdorferi, leaving out many other species that are less common yet still known to cause the disease in humans, including the recently discovered B. mayonii.
In fact, a recent internal study showed exactly how easily tests could miss infections from species other than B. burgdorferi. IGeneX researchers tested 43 samples all positive on IGeneX Lyme ImmunoBlot tests using the more limited Western blots prepared from the following species of Borrelia:
- burgdorferi B31
- spielmanii
- valensiana
When only a B. burgdorferi B31 Western Blot was performed, only 14 of the 43 Lyme ImmunoBlot-positive samples were Western-Blot-positive. In other words, the B. burgdoferi Western Blot missed 29 of the 43 infections. However, when all eight Western Blots were performed, the remaining twenty-nine samples were detected.
This inability of many lab tests to cast a wide enough net of detection could result in false-negative results for patients infected with different strains of disease-causing Borrelia.