Borrelia Burgdorferi Infectious Cycle
The infectious cycle of B burgdorferi involves colonization, infection of Ixodes ticks, and then transmission to broad a range of mammalian hosts, including humans. Variation in environmental and host conditions promotes different gene expression and changes in the composition of the membrane proteins of the spirochete. This adaptation is a critical step in the pathogenesis and transmission of Lyme disease.
The Ixodes tick progresses through four stages of development: egg, larva, nymph, and adult . Only larvae, nymphs, and adult female ticks require blood meals, and only ticks in the nymphal and adult stages can transmit B burgdorferi.
The life cycle of Ixodes ticks spans 2 years . The adult lays eggs in the spring, and the larvae emerge in the summer. The larvae feed once, in late summer, on any of a wide variety of small animals . The following spring, the larvae emerge as nymphs. Nymphs feed once, in the spring and summer. The white-footed mouse is the preferred feeding source of nymphs, but other animals apparently suffice. Nymphs molt into adults the following fall and feed once on a larger animal, with the white-tailed deer being the preferred host.
Ticks carry B burgdorferi organisms in their midgut. The bacteria are introduced into the skin by a bite from an infected tick, and disease is transmitted to humans as the spirochete is translocated from the gut to the salivary glands and then to the person at the site of the bite.
How Is Lyme Disease Diagnosed
A healthcare provider will diagnose Lyme disease based on symptoms, physical findings and whether or not you’ve been in an area populated by infected ticks.
Many people dont remember or know that theyve been bitten by a tick. This is because the tick is tiny, and its bite is usually painless.
Your provider will confirm the diagnosis using a blood test. If your first blood test is negative for Lyme disease, you won’t need another test. If the first test is positive or equivocal, your provider will conduct the test again. You have to have two positive results to be diagnosed with Lyme disease.
What Are Signs And Symptoms Of The Third Stage Of Lyme Disease
Late stage Lyme disease can result when treatment is unsuccessful or started too late due to unrecognized symptoms or misdiagnosis. The late disseminated stage occurs months or years after initial infection and can have a major impact on a patients health and quality of life. Late Lyme arthritis is a third stage Lyme disease manifestation that involves fluid accumulation and pain in joints, particularly in the knee joints. Late neurologic disease is a 3rd stage condition that can also be debilitating and difficult to diagnose. Late disseminated Lyme disease symptoms include a variety of symptoms that are often neurologic in origin including: numbness in extremities, mental fogginess and concentration problems, and difficulty following conversations or processing information.
Also Check: Antibiotic Treatment For Lyme Disease
Antibiotics For Lyme Disease Treatment
Antibiotics for Lyme disease include:
-
Thinking and memory problems
After antibiotic treatment for Lyme disease, up to 10% of patients develop post-treatment Lyme disease syndrome . PTLDS can persist for many months. Signs and symptoms of PTLDS are similar to early-stage Lyme disease and include fatigue and joint and muscle aches and pains. Patients also report difficulty sleeping, memory problems, and headache.
Some people use the term chronic Lyme disease to describe a condition marked by symptoms like Lyme disease, such as fatigue, pain, memory problems, and arthritis. However, in many of these cases, lab tests for current or past Lyme disease are negative. For this reason, Lyme disease experts support no longer using the term chronic Lyme disease.
Diagnosis Of The Disease
New-onset Lyme disease is usually diagnosed based on symptoms, the presence of erythema migrans and possible exposure to infected ticks.
In addition, a blood test known as the two-step process is recommended.
The US CDC describes this testing process in its guidelines: Recommendations for Performing and Interpreting the Test from the Second National Conference on Serological Diagnosis of Lyme Disease.
Specifically, the two phases include:
- Stage 1: the EIA test or, less commonly, the immunofluorescence assay is performed.
- Stage 2: if the EIA or IFA are positive or inconclusive, the second test performed is an immunoblot test, also known as a Western blot. If the symptoms are new onset , the IgM Western blot is performed.
If symptoms have been present for more than 30 days, a positive or inconclusive EIA or IFA test is followed by the Western Blot IgG test.
Recommended Reading: Doxycycline For Lyme Disease In Dogs
What Are The Complications Of Lyme Disease
Lyme disease affects people differently. Relapse and incomplete treatment responses happen. Relapse and incomplete treatment responses happen. Complications of untreated early-stage disease include:
-
Frequent hospitalizations to manage the disease
Some of these complications result in chronic, debilitating conditions.
Some people may develop post-Lyme disease syndrome . A condition also known as chronic Lyme disease includes PLDS, but also other syndromes. Usually, these are characterized by persistent musculoskeletal and peripheral nerve pain, fatigue, and memory impairment.
Treatment Of Lyme Disease
Early diagnosis and proper antibiotic treatment of Lyme disease is important and can help prevent late Lyme disease. The following treatment regimens reflect CDCs interpretation of the most current data for four important manifestations of Lyme disease. These regimens are consistent with guidanceexternal icon published by the by the Infectious Disease Society of America, American Academy of Neurology, and American College of Rheumatology.
Some patients report persistent symptoms of pain, fatigue, or difficulty thinking even after treatment for Lyme disease. The state of the science relating to persistent symptoms associated with Lyme disease is limited, emerging, and unsettled.
Additional researchexternal icon is needed to better understand how to treat, manage, and support people with persistent symptoms associated with Lyme disease. In light of these research gaps, recommendations for treatment of persistent symptoms in people previously treated for Lyme disease are not provided here.
If you are interested in information on chronic Lyme diseaseexternal icon, see NIHs website.
Links with this icon indicate that you are leaving the CDC website.
CDC.gov Privacy Settings
We take your privacy seriously. You can review and change the way we collect information below.
Don’t Miss: Can A Vet Test A Tick For Lyme Disease
Early Disseminated Lyme Disease
If left untreated, the infection can spread through the bloodstream and lymphatic vessels within weeks to months where it may affect the joints, nervous system, heart, or other organs. Symptoms of early disseminated Lyme disease include:
- Multiple bull’s eye rashes on various parts of the body.
- Weakness or paralysis in the muscles of the face
- Stiff and painful neck, which may be a sign of Lyme meningitis
- Heart problems symptoms include light-headedness, heart palpitations, shortness of breath, chest pain, or fainting
What Are The Signs And Symptoms Of Lyme Disease
Early symptoms usually appear within 3 to 30 days after the bite of an infected tick. In 60-80 percent of cases, a circular bull’s eye rash about two inches in diameter, called erythema migrans, appears and expands around or near the site of the tick bite. Sometimes, multiple rash sites appear. One or more of the following symptoms usually mark the early stage of Lyme disease: chills and fever, headache, fatigue, stiff neck, muscle and/or joint pain, and swollen glands. If Lyme disease is unrecognized or untreated in the early stage, more severe symptoms may occur. As the disease progresses, severe fatigue, a stiff aching neck, and tingling or numbness in the arms and legs, or facial paralysis can occur. The most severe symptoms of Lyme disease may not appear until weeks, months or years after the tick bite. These can include severe headaches, painful arthritis, swelling of the joints, and heart and central nervous system problems.
Also Check: What Size Ticks Carry Lyme Disease
Unexplained Pain And Other Sensations
Some people with Lyme may have sharp rib and chest pains that send them to the emergency room, suspecting a heart problem 00090-7/abstract%20″ rel=”nofollow”> 27).
When no problem is found, after the usual testing, the ER diagnosis is noted as an unidentified musculoskeletal cause.
You can also have strange sensations like skin tingling or crawling, or numbness or itchiness 00090-7/abstract%20″ rel=”nofollow”> 27).
Other symptoms have to do with cranial nerves.
- Ear-ringing . Tinnitus can be a nuisance, especially at bedtime when it seems to get louder as youre trying to fall asleep. About 10 percent of people with Lyme experience this (
- Hearing loss. One study reported that 15 percent of Lyme patients experienced loss of hearing .
- Jaw pain or toothaches that are not related to actual tooth decay or infection.
Summary:
How To Avoid Tick Bites
To reduce the chance of being bitten:
- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin products containing DEET are best
- stay on clear paths whenever possible
- wear light-coloured clothing so ticks are easier to see and brush off
Don’t Miss: How Many Types Of Lyme Disease Are There
Lyme Disease Is An Infection Caused By The Spirochete Bacterium Borrelia Burgdorferi Which Is Transmitted To People And Animals Through The Bite Of An Infected Deer Tick Known As A Black
According to the Centres for Disease Control and Prevention , Lyme disease is the most common arthropod-borne illness in the United States.
Bacteria introduced by the tick bite travel through the bloodstream and settle in various tissues and organs.
Over time, it can cause significant symptoms.
The American Lyme Disease Foundation describes Lyme disease as a multisystem inflammatory disease that affects the skin in its early, localised phase and spreads to the joints, nervous system and, to a lesser extent, other organ systems in its later, disseminated phases.
Protecting Property From Tick Infestation

To decrease the tick population around your yard:
- Clear the yard regularly by raking leaves, trimming bushes, pruning low-lying branches, mowing lawn.
- Create a 3-foot wide barrier around the perimeter of your lawn with wood chips, gravel, or mulch.
- Place cardboard tubes stuffed with permethrin-treated cotton in places where mice can find them. These tubes are available in hardware stores. Mice collect the cotton for lining their nests the pesticide on the cotton kills any immature ticks that feed on the mice. For best results, do several tube applications from early to late summer.
- Erect fences or use repellants or deer-resistant plants to keep deer away.
- Consider spraying once a year a small amount of tick-killing insecticide such as permethrin or bifenthrin around the perimeter of your yard. To avoid health and environmental risks, consult a licensed professional experienced with tick control.
Also Check: How Many Ticks Carry Lyme Disease
What Are The Stages Of Lyme Infection
There are three stages:
- Early localized Lyme: Flu-like symptoms like fever, chills, headache, swollen lymph nodes, sore throat, and a rash that looks like a bull’s-eye or is round and red and at least 2 inches long
- Early disseminated Lyme: Flu-like symptoms like pain, weakness, or numbness in your arms and legs, changes in your vision, heart palpitations and chest pain, a rash , and a type of facial paralysis known as Bellâs palsy
- Late disseminated Lyme: This can happen weeks, months, or years after the tick bite. Symptoms might include arthritis, severe fatigue and headaches, dizziness, trouble sleeping, and confusion.
About 10% of people treated for Lyme infection donât shake the disease. They may go on to have three core symptoms: joint or muscle pain, fatigue, and short-term memory loss or confusion. This is called post-treatment Lyme disease syndrome. It can be hard to diagnose because it has the same symptoms as other diseases. Plus, there isn’t a blood test to confirm it.
Experts arenât sure why Lyme symptoms donât always go away. One theory is that your body keeps fighting the infection even after the bacteria are gone, like an autoimmune disorder.
When Should I Go See My Doctor
Anyone who has been bitten by a black-legged deer tick is at risk for Lyme disease. The highest risk groups include those living in or visiting endemic areas, especially people who spend significant time outdoors such as gardeners, hikers, or outdoor workers.
Patients should seek advice from their doctor if they have a suspicious round expanding red skin lesion, and/or show signs of summer-flu, particularly during Lyme disease season, which is highest-risk late spring through July/August. If those circumstances apply or symptoms persist it is very important to go to a physician.
For the west coast and other more temperate regions Lyme disease can be a year-round concern.
In the later disseminated stages, Lyme disease can be a much more insidious and complex illness. An individual should seek medical care if experiencing symptoms such as prolonged fevers, unexplained fatigue, painful joints, new or unusual headache, or heart or neurologic symptoms. If unexplained viral-like symptoms last for more than 1-2 weeks, please seek the advice of a physician.
Don’t Miss: Hey Google What Is Lyme Disease
What Is The Outlook With Treatment
Oral or intravenous antibiotics treat Lyme disease. Early treatment should clear up the infection and prevent the spread of bacteria.
In later stages, when the bacteria has spread and caused symptoms, antibiotics can still help reduce symptoms. However, they may remain for years or never fully resolve.
Resources For Maine Residents
Public Law, Chapter 340, LD 597, 126th Maine State Legislature: An Act to Inform Persons of the Options for the Treatment of Lyme Disease
- Acknowledges difficulty in diagnosing and treating Lyme disease
- Information on risks of long term antibiotic therapy
Public Law, Chapter 235, LD 422, 127th Maine State Legislature: An Act to Improve Access to Treatments for Lyme Disease
- Allows licensed physicians to prescribe long-term antibiotic therapy to eliminate infection or to control a patients symptoms
Don’t Miss: Does Lyme Disease Cause Arthritis
What Should You Do If You Find A Tick
-
Don’t touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Don’t squeeze the tick, and don’t use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
Chronic Lyme: What Happens When Lyme Goes Untreated
The Lyme community typically uses the term chronic Lyme disease to describe a range of physical, cognitive, and emotional symptoms that crop up after getting Lyme disease and persist for months to years after infection.
The risk of chronic Lyme increases the longer a Lyme infection goes untreated or undertreated. In other words, patients are more likely to recover fully if their Lyme infection is detected and treated as early as possible after the discovery of a tick bite. This stage is usually marked by symptoms such as fevers, chills, muscle aches, and sometimes rashes.
When left untreated or undertreated, however, Lyme disease can spread throughout the body and affect:
- The central nervous system
- Muscles and joints
As Lymedisease.org points out, these symptoms can evolve, disappear, and reappear at different times.
Don’t Miss: Could I Have Lyme Disease And Not Know It
Lyme Disease Rashes And Look
Circular, expanding rash with target-like appearance.
Expanding rash with central crust
Expanding lesion with central crust on chest.
Expanding erythema migrans
Photo Credit: Reprinted from Bhate C, Schwartz RA. Lyme disease: Part I. Advances and perspectivesexternal icon. J Am Acad Dermatol 2011 64:619-36, with permission from Elsevier.
Description:Early, expanding erythema migrans with nodule.
Multiple rashes, disseminated infection
Early disseminated Lyme disease multiple lesions with dusky centers.
Red, oval plaque
Red, expanding oval-shaped plaque on trunk.
Expanding rash with central clearing
Circular, expanding rash with central clearing.
Bluish hued rash, no central clearing
Bluish hued without central clearing.
Expanding lesion, no central clearing
Expanding lesion without central clearing on back of knee.
Red-blue lesion with central clearing
Red-blue lesion with some central clearing on back of knee.
Insect bite hyper-sensitivity
Large itchy rash caused by an allergic reaction to an insect bite.
Fixed drug reaction
Description:A skin condition that occurs up to two weeks after a person takes a medication. The skin condition reappears at the same location every time a person takes that particular medication.
Ringworm
Description:Ringworm is a common skin infection that is caused by a fungus. Its called ringworm because it can cause a ring-shaped rash that is usually red and itchy with raised edges.
Pityriasis rosea rash
Granuloma annulare rash
Chronic Lyme Disease Vs Ptlds
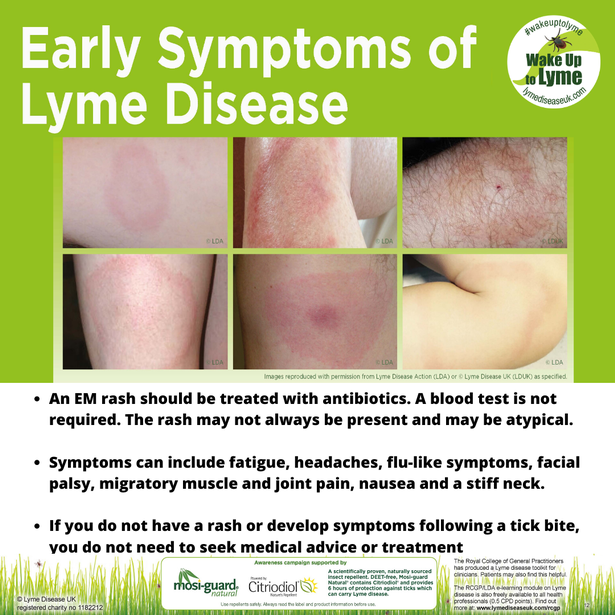
The terms chronic Lyme disease and Post-Treatment Lyme Disease Syndrome are sometimes used interchangeably. However, PTLDS is slightly more restrictive, referring to patients who have received treatment for Lyme disease but go on to experience Lyme disease symptoms. It does not include those who received a misdiagnosis or delayed diagnosis and have developed chronic symptoms of Lyme disease before receiving any kind of treatment.
The CDC defines PTLDS as generalized and/or recurring pain, fatigue, and cognitive difficulties that last for more than 6 months after treatment. These mirror symptoms associated with chronic Lyme disease, with or without treatment.
Also Check: Best Supplements For Lyme Brain
Who’s At Risk Of Lyme Disease
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.