What Are The Treatment Options For Lyme Disease Can It Be Treated Naturally
While numerous beneficial and natural treatments for Lyme exist, it is recommended that patients also complete a round of antibiotics as prescribed by their doctors. Treatment can come in different forms oral, intravenous, and intramuscular and which form to use depends on the stage of the disease.
How Are Dogs Tested For Lyme Disease
Diagnosis is made by a combination of history, physical signs, and diagnostics. For dogs, the two blood tests for diagnosing Lyme disease are called the C6 Test and Quant C6 test. Veterinarians perform both.
The C6 test detects antibodies against a protein called C6. Presence of the antibodies suggests an active Lyme infection. The C6 antibodies can be detected three to five weeks after an infected tick bites a dog and may be found in the bloodstream even before the dog shows signs of illness.
The next step is to do a Quant C6 test. This, along with urinalysis will help determine if antibiotic treatment is necessary.
What Is The History Of Lyme Disease
Interestingly, the disease only became apparent in 1975 when mothers of a group of children who lived near each other in Lyme, Conn., made researchers aware that their children had all been diagnosed with joint pain from rheumatoid arthritis. This unusual grouping of illnesses that appeared “rheumatoid” eventually led researchers to the identification of the bacterial cause of the children’s condition, which was then named “Lyme disease” in 1982.
The only vector for Lyme disease in the U.S. is the black-legged tick, or deer tick, known as Ixodes scapularis. These ticks are carriers of the Lyme disease spirochete in their stomachs Ixodes ticks may also transmit the Powassan virus. The ticks are vectors that can transmit the bacterium to humans with a tick bite. The number of cases of tick-borne illness in an area depends on the number of ticks present and how often the ticks are infected with the bacteria. In certain areas of New York, where Lyme disease is common, over half of the ticks are infected. Lyme disease has been reported most often in the northeastern United States, but it has been reported in all 50 states, as well as China, Europe, Japan, Australia, and parts of the former Soviet Union. In the United States, it is primarily contracted in the Northeast in the states from Maine to Maryland, in the Midwest in Minnesota and Wisconsin, and in the West in Oregon and Northern California. What those children actually had was Lyme arthritis.
You May Like: Ozone Therapy For Chronic Lyme
Where Blacklegged Ticks Live
We continue to track where infected and uninfected blacklegged ticks are being found.
Public Health Ontarios Lyme disease page has a map that shows areas in Ontario where they estimate you are more likely to find blacklegged ticks.
Blacklegged ticks are spreading to new areas of the province because of climate change. They can also spread by traveling on birds and deer. While the probability is low, it is possible to find an infected tick almost anywhere in Ontario.
Ticks are most active in spring and summer, but can be found at any time of the year when the temperature is above freezing.
Why Canadians Are Getting Tested For Lyme Disease In The Usa
In Canada, physicians familiar with Lyme disease are faced with a challenge, because the diagnostic tests in Canada are not fully effective yet. They can diagnose from symptoms, however, doctors take a risk when they begin treatment without a formal Lyme disease diagnosis.Unfortunately, waiting for a formal diagnosis can be a long and frustrating procedure, and as with Rachel, tests sometimes lead to a false negative. And the longer a patient waits for treatment, the longer recovery will eventually take.
Also Check: When To Treat Lyme Disease
Lyme Disease Symptoms To Watch For According To Doctors
Knowing the symptoms to look for can help diagnose Lyme disease early on, when it’s easily treatable.
Fever or fatigue, with or without a rash, can be a symptom of many thingsand Lyme disease is just one possibility. To diagnose Lyme, doctors say they have to consider symptoms and circumstances. If youve been hanging out in wooded or grassy areas, especially in certain regions of the country during the spring, summer, or even autumn months, it might make sense to entertain the possibility that you were bitten by a tick. And whats the most commonly reported tick-borne illness in America? Its Lyme disease, by far.
But Timothy P. Flanagan, MD, associate professor of medicine in the infectious diseases division at Brown Universitys Alpert Medical School, says it would be a mistake to latch on to a Lyme diagnosis without ruling out other possible causes, including other infections transmitted by ticks. You could have a different tick-borne infection entirely, such as anaplasmosis or babesiosis, or you could have Lyme with one or more co-infections. Thats because the same ticks that transmit Borrelia can carry other disease-causing microbes, too.
Its super important that we think of all the tick-borne diseasesnot just Lyme, Dr. Flanagan tells Health. Babesia, a parasite that causes babesiosis, is treated differently than Borrelia, for example.
Achy Stiff Or Swollen Joints
Joint pain and stiffness, often intermittent, are early Lyme symptoms. Your joints may be inflamed, warm to the touch, painful, and swollen. You may have stiffness and limited range of motion in some joints .
Pain may move around. Sometimes your knees may hurt, whereas other times its your neck or your heels. You may also have bursitis . Bursae are the thin cushions between bone and surrounding tissue.
The pain may be severe, and it may be transitory. More than one joint may be affected. Most often the large joints are involved .
People often attribute joint problems to age, genetics, or sports. Lyme should be added to that list, as these statistics indicate:
- One study estimates that 80 percent of people with untreated Lyme have muscle and joint symptoms .
- Fifty percent of people with untreated Lyme have intermittent episodes of arthritis .
- Two-thirds of people have their first episode of joint pain within six months of the infection .
- Use of anti-inflammatory drugs may mask the actual number of people with joint swelling .
Summary:
Joint pain that comes and goes, or moves from joint to joint, could be a sign of Lyme.
Also Check: Can Lyme Disease Be Cured In Dogs
Do All Ticks Transmit Lyme Disease
No. In the northeastern and north-central U.S., the black-legged tick carries Lyme disease. In the Pacific coastal U.S., the western black-legged tick spreads the disease.
Other major tick species in the U.S., like the lone star tick and the dog tick, do NOT transmit the Lyme disease bacterium. But beware: All 50 states have reported Lyme disease, as well as Canada, Europe, Asia, Australia, and South America.
Magnesium Deficiency In Lyme Patients
For years, Canadians with Lyme disease have been using Natural Calm magnesium as part of their treatment. We often hear from Natural Calm customers who tell us how magnesium helps. In fact, weve been approached by Lyme support groups who openly advocate for Natural Calm.
But why does magnesium help relieve symptoms of Lyme disease?
Research on the relationship between magnesium and Lyme disease is still in early phases. However, authorities in natural medicine believe magnesium can mitigate certain symptoms associated with Lyme disease.
Lyme patients have magnesium deficiencies for a number of different reasons. Lyme bacteria require magnesium to complete their life cycle, drawing magnesium from the patients stores. Magnesium must be replaced daily, so patients are wise to supplement.
In cases of Chronic Lyme disease, the body is under excessive stress for prolonged periods of time and magnesium levels drop, meaning that they need to be replenished as much as possible.
As Dr. Rawls explains in his book, Unlocking Lyme, Borrelia microbes prefer collagen-rich tissues, such as joints, brain, muscle eyes, and skin. Most symptoms associated with chronic Borrelia infection originate in these areas. The microbes are also fond of myelin, a fatty substance that forms a sheath around nerves. Inflammatory symptoms of Lyme disease are most pronounced in areas of the body rich in collagen and myelin.
Also Check: What Medication Is Used For Lyme Disease
The Recovery Prognosis For Canadians With Lyme Disease
Given the dissatisfactory Lyme care in Canada, many patients go months or even years without a diagnosis, though once they are diagnosed and given the appropriate medication, recovery can happen as fast as several weeks after the antibiotics.
Patients experience recoveries across a spectrum, depending on how fast they obtained treatment after being infected, and how their bodies responded to antibiotics. For up to 20% of Lyme patients, subdued symptoms last up to six months after antibiotic treatment.
The majority of Lyme patients do make a full recovery. The only exception is in chronic cases, when patients have gone long periods of time without treatment or diagnosis. Some chronic Lyme disease patients experience permanent or long lasting joint pain and damage to their nervous systems, but even then, it is expected that symptoms become more manageable with time.
Signs Of Lyme Disease That Appear On Your Skin
Signs of Lyme disease
If you see a rash or another sign of Lyme disease on your skin, see your primary doctor right away. When caught early and treated, Lyme disease can be cured with antibiotics and most people recover fully.
Lyme disease is caused by a bite from a black-legged tick. If you are bitten by this tick and develop Lyme disease, you may see a bulls-eye rash. Its a common sign of Lyme disease, but its not the only sign.
Lyme disease occurs in stages. Heres what you may see on your skin during each stage.
Read Also: Deer Ticks Carry Lyme Disease
Stage : Quickly Expanding Rash
After being bitten by a black-legged tick, a quickly growing rash can appear. This is the earliest stage of Lyme disease, known as stage 1.
Most people who develop a rash, get it within days or weeks of being bitten by a tick.
Where you see the rash: If you develop a rash, it appears near the tick bit you. For most people, that means the back, groin, armpit, or a lower leg. However, a tick can bite you anywhere.
What the rash can look like: You may see a spot or bump on the skin, which is the bite mark. Around or near the bite mark, a rash develops. Some people see the bulls-eye rash . You can also have one of the other rashes shown here.
Early rash caused by Lyme disease
Notice the bite mark in the center of this early rash, which will expand quickly.
Bull’s-eye rash on woman’s upper arm
This is another early sign of Lyme disease.
Lyme disease rash with lighter color on the outside
This rash has expanded, but you can still see the bite mark in the center.
Rash from Lyme disease has begun to clear
As the rash begins to clear, the redness fades.
If you develop a rash during this stage, you may notice that it:
-
Feels smooth and warm to the touch
-
Causes a burning sensation
-
Itches or feels painful
-
Has an outer edge that feels scaly or crusty
When the rash and symptoms begin: According to the Centers for Disease Control and Prevention , the rash begins 3 to 30 days after the tick bites you.
About 50% of people who have Lyme disease develop flu-like symptoms , which include:
What Is Lyme Disease

Lyme disease is a bacterial tick-borne illness transmitted from the bite of an infected black-legged or deer tick. Ticks dont naturally have the infection. They acquire it by feeding on an infected host animal. It is delivered to humans when ticks attach to the skin and through their bite, transfer a spirochete bacterium called Borrelia burgdorferi.1,2 Tick populations are concentrated in certain geographic areas. There is a higher concentration on the East and West coasts, and parts of the Midwestern US, although ticks can be found across the U.S.
Recommended Reading: How To Use Essential Oils To Treat Lyme Disease
Rachels Lyme Disease Story
Rachel Aide has spent close to 3 years living with Lyme disease, learning about it, and recently, recovering from it.
Like many Lyme patients, Rachel didnt experience the bullseye rash, making it hard to pinpoint where and when exactly her infection took place, however, she suspects she was infected in Saint Andrews by-the-Sea, NB, in 2016, while taking a walk in tall grasses.
Most likely, Rachel was bitten while the tick was in its nymph stage, when the tick is very small and harder to see. When small ticks go unnoticed, they often have enough time to transmit the Lyme disease bacterium before being noticed and removed.
Rachel like so many others didnt suspect Lyme disease because she didnt remember having a rash or being bitten.
Signs And Symptoms Of Lyme Disease
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
Overview
Lyme disease is an underreported, under-researched, and often debilitating disease transmitted by spirochete bacteria. The spiral-shaped bacteria, Borrelia burgdorferi, are transmitted by blacklegged deer ticks. Lymes wide range of symptoms mimic those of many other ailments, making it difficult to diagnose .
The blacklegged ticks can also transmit other disease-causing bacteria, viruses, and parasites. These are known as coinfections . These ticks that transmit Lyme are increasing their geographical spread. As of 2016, they were found in about half the counties in 43 of 50 states in the United States .
Lyme is the fifth most reported of notifiable diseases in the United States, with an estimated 329,000 new cases found annually . Some studies estimate that there are as many as 1 million cases of Lyme in the United States every year .
Most people with Lyme who are treated right away with three weeks of antibiotics have a good prognosis.
But if youre not treated for weeks, months, or even years after infection, Lyme becomes more difficult to treat. Within days of the bite, the bacteria can move to your central nervous system, muscles and joints, eyes, and heart .
Here is a list of 13 common signs and symptoms of Lyme disease.
Recommended Reading: What Type Of Doctors Treat Lyme Disease
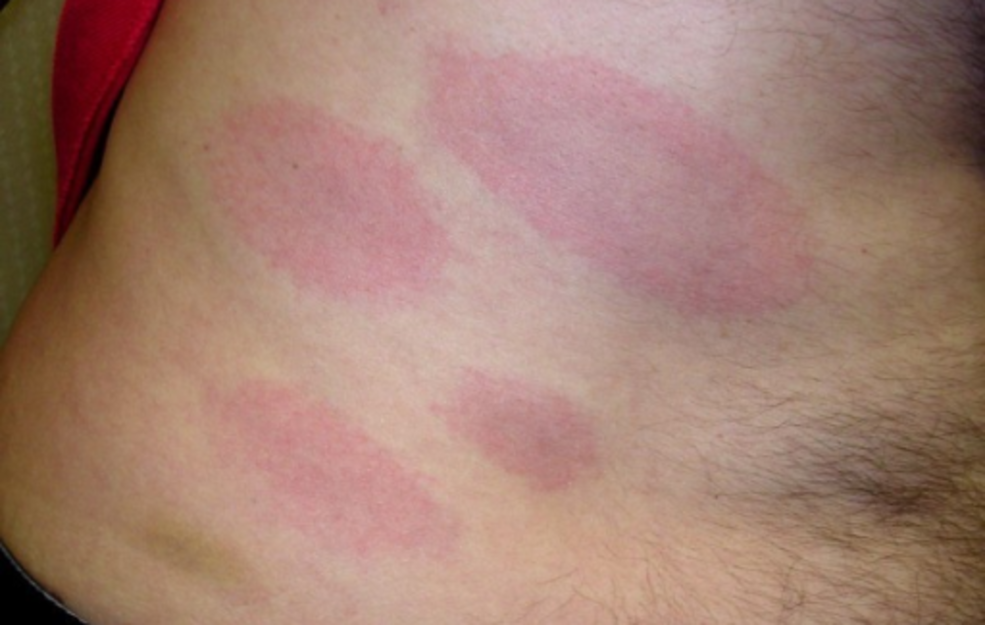
Atypical Lyme Rashes And Less
In some cases, the Lyme disease rash doesnt look like a bulls eye at all. It can be blistered , cause a bluish swelling , be uniform in color instead of banded, be oval or triangular in shape, or just look like a large red area . You can see a picture of atypical Lyme disease on a black man here.
There are also many instances of Lyme rashes which are considered to be bulls-eye shaped, but dont have the white band inside. The message? Dont expect a Lyme rash to look like a perfect bulls eye. If you suspect Lyme, contact your doctor!
Chronic Lyme Disease Symptoms
If Lyme disease is not diagnosed and treated early, it may become late-stage or chronic. This may also occur when early treatment is inadequate. While some symptoms of chronic or late stage Lyme disease are similar to those of early Lyme, as the graphic below shows, there are important differences.
Lyme disease may spread to any part of the body and affect any body system. Typically, it affects more than one body system. In our survey, which drew over 5,000 responses, patients with chronic Lyme disease reported an average of three severe or very severe symptoms, with 74% reporting at least one symptom as severe or very severe.
An extensive list of symptoms of chronic Lyme disease was developed by Dr. Joseph Burrascano, a pioneer in treating chronic Lyme disease.
Read Also: Do All Deer Ticks Have Lyme Disease
Differences In Treatment Goals
Options for MS treatment vary and are designed to manage symptoms and prevent relapse. Use of prescription medications, corticosteroids, and plasma exchange help keep the disease in check. Physical therapy, muscle relaxants, and other drugs are used to reduce fatigue, depression, sexual and bladder problems, and other miscellaneous symptoms. MS is a chronic, generally progressive, lifelong condition that can range mild to severe, whereas Lyme disease can be treated and usually cured.
Antibiotics: The First Line Of Lyme Disease Treatment
Right after her diagnosis, Rachel began oral antibiotic treatment using Doxycycline, and taking probiotics to maintain balance of her intestinal bacteria. Antibiotics are the only proven way to kill off the bacteria that cause Lyme disease.
Previously, it was common practice for doctors to prescribe just one round of antibiotics, regardless of the stage of the disease, however it is now believed that such a prescription would not be effective in treating more chronic cases. This is especially true considering cases which have been left untreated for longer periods of time and need long term treatment plans.
Doxycycline, Rachels prescribed antibiotic, had certain unpleasant side effects including extreme nausea. The nausea made her feel as though her symptoms were worsening, when in fact, the opposite was the case.
The bacteria release toxins as they die, resulting in what are called Herxheimer reactions. Lyme patients experience Herxheimer reactions as seemingly worsening symptoms or pain as the bacteria are being killed.
Since the bacteria dont die at fixed intervals, the more intense symptoms are very sporadic.
Rachel mitigated the nausea by taking antibiotics on a full stomach and with anti-nausea medications.
Ultimately, it was doxycycline that eliminated the infection, but throughout the recovery process, it was the treatment with the most severe side effects. Rachel spent 8 months on Doxycycline and subsequently took other antibiotics.
Read Also: Arizona Lyme Disease Treatment Center
Other Canine Diseases Carried By Ticks
Ticks can also carry several other less common but serious bacterial diseases affecting dogs, including anaplasmosis and babesiosis.
Anaplasmosis can involve symptoms similar to those for Lyme disease. Babesiosis can present with a wide range of symptoms, from sudden and severe shock, high fever, and dark urine to a slowly progressing infection with more subtle clinical signs. Diagnosis of both diseases includes blood tests similar to those used to check for Lyme disease.
Sometimes, dogs and people can become sick with co-infection of multiple tick-borne diseases, where more than one type of disease-causing bacteria is transmitted through a tick bite. This situation can make diagnosis and treatment even more challenging and difficult.