What’s The Best Way To Prevent A Tick Bite
Ticks can’t fly or jump. But they live in shrubs and bushes and can grab onto you when you pass by. To avoid getting bitten:
- Wear pants and socks in areas with lots of trees and when you touch fallen leaves.
- Wear a tick repellent on your skin and clothing that has DEET, lemon oil, or eucalyptus.
- For even more protection, use the chemical permethrin on clothing and camping gear.
- Shower within 2 hours after coming inside. Look for ticks on your skin, and wash ticks out of your hair.
- Put your clothing and any exposed gear into a hot dryer to kill whatever pests might be on them.
How do you know if you’ve been bitten?
Since ticks are so small, you’ve got to have pretty good eyes to see them.
If you have a small, red bump on your skin that looks like a mosquito bite, it could be a tick bite. If it goes away in a few days, itâs not a problem. Remember, a tick bite doesnât necessarily mean you have Lyme disease.
If you notice a rash in the shape of a bull’s-eye, you might have a tick bite. Talk to your doctor about treatment.
If you have an allergic reaction to ticks, you’ll notice a bite right away.
Fact #: There Is No Place In The Country That A Dog Cant Contract Lyme Disease
An important aspect that is often misunderstood is the pervasiveness of ticks. There is a very high density of Lyme disease cases reported in the Northeast and Great Lakes area, but there are cases across the entire country. So important fact number one is that there is no place in the country that a dog cant contract Lyme disease.
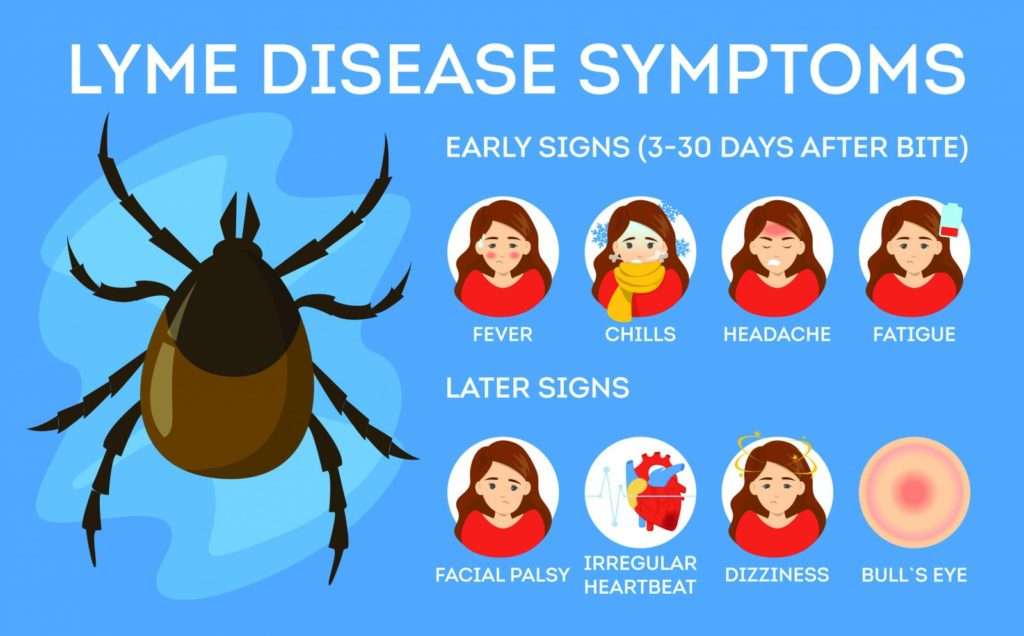
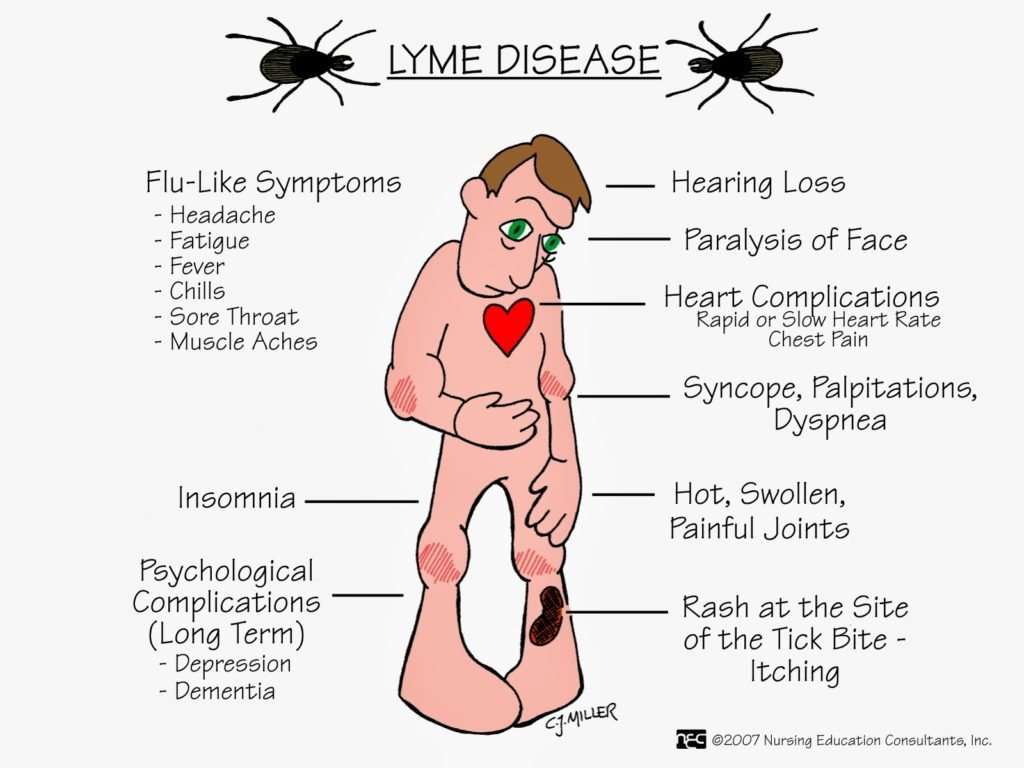
What Are Complications Of Lyme Disease
Lyme disease can be complicated by permanent damage to joints, the heart, the brain, and the nervous system. There is recent research that demonstrates an increased risk for autoimmune forms of arthritis, including
Medically Reviewed on 12/22/2021N Engl J MedPrimer on the Rheumatic DiseasesN Engl J MedAmerican Academy of Family Physicians
Don’t Miss: Where Did Lyme Disease Come From
Uncovering The Chimeritope Protein
Finding a single natural protein that would provide protection by targeting the bacteria in the tick as well as in individuals was quite a challenge, he says. We came to the conclusion that nature wasnt going to hand it to us, and that we had to get more creative than that.
Marconis work has centered on generating novel proteins called chimeritopes where, instead of using a single B. burgdorferi protein antigen to create a vaccine, the immunologically relevant pieces of several different proteins are joined together to create a new protein called a chimeritope.
This new type of protein stimulates antibodies that can recognize multiple targets on the surface of the Lyme disease causing bacteria, he says. It provides broader protection to against all variants of the Lyme disease spirochetes worldwide.
Thats what weve been striving for, and Im confident weve achieved that, he says.
Vaccine development is an intensive and expensive process. The work is funded in large part by a $2.54 million grant from the National Institutes of Health, with additional backing by the Steven & Alexandra Cohen Foundation, the Christian Family Foundation, and VCU. The VCU funding through the School of Medicine is supported by the university reinvesting royalties from the canine vaccine.
What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.
Recommended Reading: Apartments For Rent In East Lyme Ct
What Blacklegged Ticks Look Like
Blacklegged ticks are small and hard to see. They attach themselves to humans and animals and feed on their blood. They can range in size depending on how long they have been feeding.
You can find out if its a blacklegged tick by:
- calling your local public health unit or checking their website
- submitting a photo of the tick to etick.ca
Adult female blacklegged tick at various stages of feeding. Photo: Government of Canada
Essential Facts About Lyme Disease
Ticks are most active from April to September, which means spring and summer are the prime times for infection.
Every year, state health departments in the United States report about 30,000 cases of Lyme disease to the Centers for Disease Control and Prevention . But the CDC says the true number of cases in the United States could be 10 times higher.
Lyme disease is an infectious disease transmitted to humans from tick bites. Ticks infected with the bacteria Borrelia burgdorferi cause the disease and are most active from April to September, which means spring and summer are the prime times for infection. But with the right steps and regular tick checks, you can prevent Lyme disease. It’s also good to know that most cases can be treated and cured.
Here are 10 things you should know about this tick-borne disease.
Also Check: My Dog Tested Positive For Lyme
Essential Oils For Lyme Disease
It is believed that many essential oils have antimicrobial activities, and some people with persistent Lyme disease symptoms have turned to essential oils to help reduce symptoms of the disease.
Researchers tested 34 essential oils against B. burgdorferi in the lab and found cinnamon bark, clove bud, citronella, wintergreen, and oregano show strong activity against the bacterium that causes Lyme disease, even more effectively than daptomycin, the gold standard antibiotic many people with Lyme disease are prescribed.
These results indicate that essential oils show promise as treatments for persistent Lyme disease, but clinical trials are needed in order to show their effectiveness in humans.
When used properly, most essential oils are safe and free of adverse side effects. However, it is important to use them carefully. They can irritate the skin if not properly diluted, and some should not be taken internally.
Purchase high-quality essential oils that go through testing to ensure the product is safe to use. Follow the usage and dilution instructions on the label carefully. Talk with your healthcare professional before using essential oils to avoid drug interactions with any medications you are taking.
Key Points To Remember
- Most Lyme disease tests are designed to detect antibodies made by the body in response to infection.
- Antibodies can take several weeks to develop, so patients may test negative if infected only recently.
- Antibodies normally persist in the blood for months or even years after the infection is gone therefore, the test cannot be used to determine cure.
- Infection with other diseases, including some tickborne diseases, or some viral, bacterial, or autoimmune diseases, can result in false positive test results.
- Some tests give results for two types of antibody, IgM and IgG. Positive IgM results should be disregarded if the patient has been ill for more than 30 days.
Recommended Reading: Lyme Disease Specialist Long Island New York
Ongoing Symptoms Of Lyme Disease
A few people who are diagnosed and treated for Lyme disease continue to have symptoms, like tiredness, aches and loss of energy, that can last for years.
These symptoms are often compared to fibromyalgia and chronic fatigue syndrome.
It’s not clear why this happens to some people and not others. This means there’s also no agreed treatment.
Speak to a doctor if your symptoms come back, or do not improve, after treatment with antibiotics.
The doctor may be able to offer you further support if needed, such as:
- referral for a care needs assessment
- telling your employer, school or higher education institution that you require a gradual return to activities
- communicating with children and families’ social care
Page last reviewed: 05 July 2021 Next review due: 05 July 2024
What Causes Lyme Disease
Lyme disease is caused by bacteria. In the United States, this is usually a bacterium called Borrelia burgdorferi. It spreads to humans through the bite of an infected tick. The ticks that spread it are blacklegged ticks . They are usually found in the:
- Northeast
- Upper Midwest
- Pacific coast, especially northern California
These ticks can attach to any part your body. But they are often found in hard-to-see areas such as your groin, armpits, and scalp. Usually the tick must be attached to you for 36 to 48 hours or more to spread the bacterium to you.
Recommended Reading: What Does Lyme Disease Do To You
What Do You Do If There’s A Tick Under Your Skin
Use a pair of fine-tipped tweezers to remove it as soon as possible. Pull upward with steady pressure. If parts of the tick are still in your skin, try to get those with the tweezers, too. After everything is out, clean the bite area with rubbing alcohol or soap and water.
You probably wonât get infected if you remove the tick within 36 to 48 hours.
How do you throw away a tick?
Put it in soapy water or alcohol, stick it to a piece of tape, or flush it down the toilet.
Fact #: Ticks Are Most Likely To Be Found In Wooded Areas & Tall Grass

The areas that tick contact is most likely to be made are wooded areas and tall grass. Ticks feed by questing which means they hang out on a tall piece of grass and wait for the right signal then jump on the animal to feed. When they are done they simply fall off where they are and move on.
It is common for recommendations to be made to avoid tick areas, but if you are an outdoors person that shares that time with a canine companion then that is impossible.
Also Check: Homes For Sale Old Lyme Ct
How To Remove A Tick
Removing a tick is the same for humans and animals. Its important you do not crush or damage the tick because it could cause Lyme bacteria to pass from the tick into your bloodstream.
How to remove a tick.
Achy Stiff Or Swollen Joints
Joint pain and stiffness, often intermittent, are early Lyme symptoms. Your joints may be inflamed, warm to the touch, painful, and swollen. You may have stiffness and limited range of motion in some joints .
Pain may move around. Sometimes your knees may hurt, whereas other times its your neck or your heels. You may also have bursitis . Bursae are the thin cushions between bone and surrounding tissue.
The pain may be severe, and it may be transitory. More than one joint may be affected. Most often the large joints are involved .
People often attribute joint problems to age, genetics, or sports. Lyme should be added to that list, as these statistics indicate:
- One study estimates that 80 percent of people with untreated Lyme have muscle and joint symptoms .
- Fifty percent of people with untreated Lyme have intermittent episodes of arthritis .
- Two-thirds of people have their first episode of joint pain within six months of the infection .
- Use of anti-inflammatory drugs may mask the actual number of people with joint swelling .
Summary:
Joint pain that comes and goes, or moves from joint to joint, could be a sign of Lyme.
You May Like: Can I Test Myself For Lyme Disease
Differential Gene Expression Tick Transmission And Back Again
Because animals syringe-inoculated with in vitro-cultivated organisms develop manifestations indistinguishable from animals inoculated with ticks , the arthropod phases of the bacterial life cycle might be considered irrelevant to pathogenesis. However, in the real world, Lyme disease spirochetes are transmitted by ticks and, therefore, the tick-mammal interface must be regarded as the starting point for the infectious process . Indeed, there is now overwhelming evidence that spirochetes in feeding ticks undergo complex alterations in their transcriptional and protein profiles that are not reproduced by in vitro culture conditions . Collectively, these changes enable the spirochete to adapt physiologically to the feeding midgut environment , while, at the same time, preparing it for challenges looming during the mammalian phase . They also promote binding to the bacterial surface of serum proteins that exploit mammalian proteolytic systems to facilitate dissemination from tick to mammal and protect against complement-mediated lysis . The obligatory time course for this programmatic sequence explains why spirochetes are infrequently transmitted to mice or humans when ticks are attached for less than 48 h. It is critical for physicians to be aware of this time frame because it establishes the window of opportunity for antimicrobial prophylaxis and can be used to provide re-assurance to individuals who removed recently attached ticks that their risk of infection is low.
How Do I Know If I Have A Tick Bite
Many people who develop the disease do not remember seeing ticks or being bitten. Tick bites commonly occur from May to September in North America, although blacklegged ticks can be active most of the year. Ticks sometimes move around on the body but they usually attach themselves to the skin and stay in one place. Before feeding, ticks look like small, brown scabs or freckles. After feeding, ticks may swell considerably, and could be as big as a raisin or a small grape.
Follow the link for more information about blacklegged ticks from the Government of Canada.
Don’t Miss: At Home Lyme Disease Test
Chronic Lyme Disease And Post
Almost 30 years ago, clinicians began to report that some Lyme disease patients have persistent nonspecific symptoms after receiving an adequate course of therapy . In its 2006 guidelines, the Infectious Diseases Society of America created a working definition for this entity, now called post-treatment Lyme disease syndrome or PTLDS: clinical symptoms persisting at least six months after treatment for Lyme disease in persons who lack objective evidence of treatment failure, reinfection, or relapse . PTLDS differs from CLD in one particularly important respect patients with PTLDS have unequivocal documentation for appropriately treated Lyme disease. PTLDS occurs in only a small percentage of treated patients. As noted by Lantos in an excellent review , only 222 of 5846 patients screened to participate in clinical trials for PTLDS had credible evidence for past Lyme disease, while less than 10% of patients in ten prospective studies of EM and early disseminated Lyme disease described persistent symptoms such as myalgias or fatigue 9 or more months following treatment. Fortunately, multiple longitudinal studies in the U.S. and Europe report that functional impairment by PTLDS diminishes over time .
How Is Lyme Disease Diagnosed
Your doctor will diagnose you based on your symptoms and whether youâve been exposed to a tick. They might also run a blood test. In the first few weeks of infection, the test may be negative because antibodies take a few weeks to show up.
Hopefully soon, there will be tests that can diagnose Lyme disease in the first few weeks after youâre exposed. The earlier you get treated, the less likely itâll get worse.
Also Check: Jobs Near Old Lyme Ct
What Are The Complications Of Lyme Disease
Lyme disease affects people differently. Relapse and incomplete treatment responses happen. Relapse and incomplete treatment responses happen. Complications of untreated early-stage disease include:
-
Joint disease
-
Frequent hospitalizations to manage the disease
Some of these complications result in chronic, debilitating conditions.
Some people may develop post-Lyme disease syndrome . A condition also known as chronic Lyme disease includes PLDS, but also other syndromes. Usually, these are characterized by persistent musculoskeletal and peripheral nerve pain, fatigue, and memory impairment.
What Should You Do If You Find A Tick
-
Don’t touch the tick with your bare hand.
-
Use a pair of tweezers to remove the tick. Grab the tick firmly by its mouth or head as close to your skin as possible.
-
Pull up slowly and steadily without twisting until it lets go. Don’t squeeze the tick, and don’t use petroleum jelly, solvents, knives, or a lit match to kill the tick.
-
Save the tick. Place it in a plastic container or bag so it can be tested for disease, if needed.
-
Wash the bite area well with soap and water and put an antiseptic lotion or cream on the site.
Don’t Miss: Does Lyme Disease Cause Headaches
Biological Explanations For Chronic Lyme Disease
Several arguments have been made to support the biological plausibility of CLD and to justify its treatment with lengthy courses of antibiotics. One is that B burgdorferilocalizes intracellularly in the infected host, and that the antibiotics typically chosen to treat it do not penetrate cells effectively. Aside from the fact that B burgdorferi predominantly occupies the extracellular matrix, the antibiotics currently recommended to treat Lyme disease are well-established to treat a variety of intracellular infections. For example, doxycycline and azithromycin are first-line drugs for the treatment of Mycoplasma, Chlamydia, and Legionella, and doxycycline is the drug of choice for Rickettsia and related species. Ceftriaxone is effective against Salmonella and Neisseria, both of which are predominantly intracellular amoxicillin is effective against Listeria.
Another commonly voiced argument is that B burgdorferi assumes a round morphology, variously described as cyst forms,spheroplasts,L-forms, and round bodies. These variants are said to be resistant to antibiotic treatment and require alternative antibiotics and dosing strategies. On close review of the literature there is little evidence that these variants arise in vivo in humans, let alone that they are associated with CLD-like symptom complexes or that they require treatment.