Symptoms Of Lyme Disease
Many people with early symptoms of Lyme disease develop a circular rash around the tick bite. The rash:
- usually develops around 3 to 30 days after you’ve been bitten
- is often described as looking like a bull’s-eye on a dart board
- will be red and the edges may feel slightly raised
- may get bigger over several days or weeks
- is typically around 15 cm across, but it can be much larger or smaller
Some people may develop several rashes in different parts of their body.
Around 1 in 3 people with Lyme disease won’t develop a rash.
Lyme Disease In Dogs And Other Pets
Household pets can get Lyme disease, too. Typical symptoms in animals include swollen joints and lameness, fever, and loss of appetite. Experts in the FDAs Center for Veterinary Medicine say that dogs with Lyme disease occasionally develop serious kidney disease that can be fatal.
There are ways you can reduce your pets risk for tick bites and Lyme disease. Regularly checking pets for all types of ticks, for instance, reduces the risk of infection for both pet and owner. Avoid allowing your dog to roam in tick-infested areas.
Topical, oral and/or collar products are also very important in preventing Lyme disease in dogs.
There are two basic types of Lyme disease vaccines available for dogs. Talk to your veterinarian to see if vaccination is appropriate for your dog. There is no vaccination for cats, which do not seem susceptible to Lyme disease.
Pearls And Other Issues
Based on the geographic distribution of the shared vector Ixodes scapularis, co-infections with Lyme disease and human granulocytic anaplasmosis and/or babesiosis can occur. Co-infected patients may be more severely ill at presentation, have a persistent fever longer than 48 hours after initiating antibiotic therapy for Lyme disease, or present with anemia, leukopenia, and/or thrombocytopenia. When co-infection is suspected or confirmed, treatment with an appropriate antimicrobial regimen for each infection is necessary for resolution of illness.
Read Also: Best Lyme Clinic In The World
Early Signs And Symptoms
What Are The Symptoms Of Lyme Disease
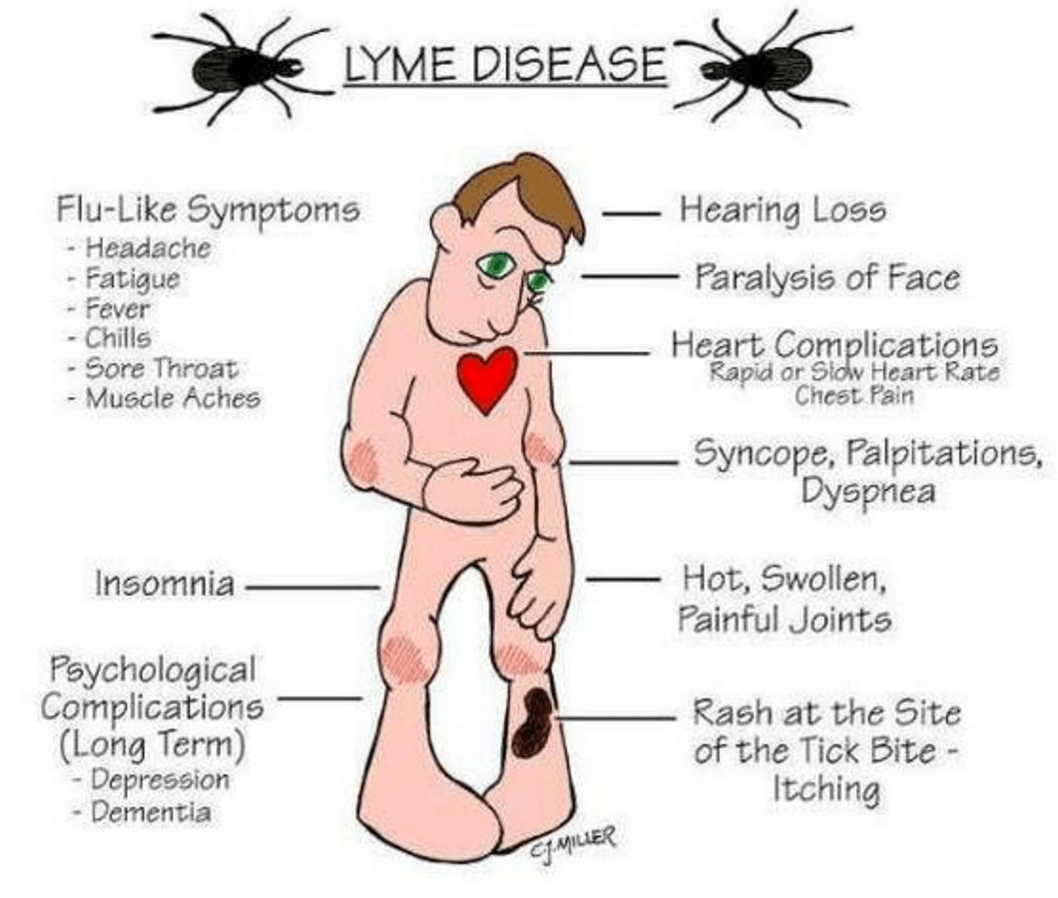
The list of possible symptoms is long, and symptoms can affect every part of the body. The following are the most common symptoms of Lyme disease. But symptoms are slightly different for each person.
The primary symptom is a red rash that:
-
Can appear several days after infection, or not at all
-
Can last up to several weeks
-
Can be very small or grow very large , and may resemble a “bulls-eye”
-
Can mimic such skin problems as hives, eczema, sunburn, poison ivy, and flea bites
-
Can itch or feel hot, or may not be felt at all
-
Can disappear and return several weeks later
Several days or weeks after a bite from an infected tick, you may have flu-like symptoms such as the following:
Weeks to months after the bite, the following symptoms may develop:
-
Neurological symptoms, including inflammation of the nervous system and weakness and paralysis of the facial muscles
-
Heart problems, including inflammation of the heart and problems with heart rate
-
Eye problems, including inflammation
Months to a few years after a bite, the following symptoms may include:
-
Inflammation of the joints
-
Neurological symptoms including numbness in the extremities, tingling and pain, and difficulties with speech, memory, and concentration
Some people may develop post-Lyme disease syndrome . A condition also known as chronic Lyme disease includes PLDS, but also other syndromes. Usually, these are characterized by persistent musculoskeletal and peripheral nerve pain, fatigue, and memory impairment.
Don’t Miss: What Happens If Lyme Disease Goes Untreated For Years
Can My Animal Get Infected Despite Being Vaccinated
Yes. Some animals have been infected despite vaccination. The most common reasons are low or short-lasting vaccine antibodies in the individual animal. It is advisable to monitor the vaccine response annually to ensure the animal develops sufficient antibodies in response to vaccination. Vaccine antibodies can be quantified with the Lyme Multiplex assay as early as two weeks following vaccination or anytime afterwards.
When Should I Go See My Doctor
Anyone who has been bitten by a black-legged deer tick is at risk for Lyme disease. The highest risk groups include those living in or visiting endemic areas, especially people who spend significant time outdoors such as gardeners, hikers, or outdoor workers.
Patients should seek advice from their doctor if they have a suspicious round expanding red skin lesion, and/or show signs of summer-flu, particularly during Lyme disease season, which is highest-risk late spring through July/August. If those circumstances apply or symptoms persist it is very important to go to a physician.
For the west coast and other more temperate regions Lyme disease can be a year-round concern.
In the later disseminated stages, Lyme disease can be a much more insidious and complex illness. An individual should seek medical care if experiencing symptoms such as prolonged fevers, unexplained fatigue, painful joints, new or unusual headache, or heart or neurologic symptoms. If unexplained viral-like symptoms last for more than 1-2 weeks, please seek the advice of a physician.
Recommended Reading: How Do I Know If My Lyme Disease Is Cured
What You Need To Know About Lyme Disease
-
Lyme disease is an infection caused by the spiral-shaped bacteria Borrelia burgdorferi, which is most commonly transmitted by a tick bite.
-
There are over 300,000 estimated new cases of Lyme disease in the United States each year.
-
The symptoms of Lyme disease depend on the how long the infection has been present in the body. The first sign of Lyme disease is often an expanding round or oval red “bullseye” rash.
-
If left untreated, people may develop neurological symptoms and heart problems, and have an approximately 60 percent chance of developing Lyme arthritis.
Does Lyme Disease Treatment With Antibiotics Affect Antibody Levels
Antibiotic treatment affects the pathogen . It does not directly influence antibody titers. However, if the treatment is successful and bacteria are removed from the host, the B-cells are not further triggered to produce new antibodies. As a consequence antibodies levels decrease after treatment. Thus, antibody levels are indicators of treatment success .
Don’t Miss: Images Of Ticks That Carry Lyme Disease
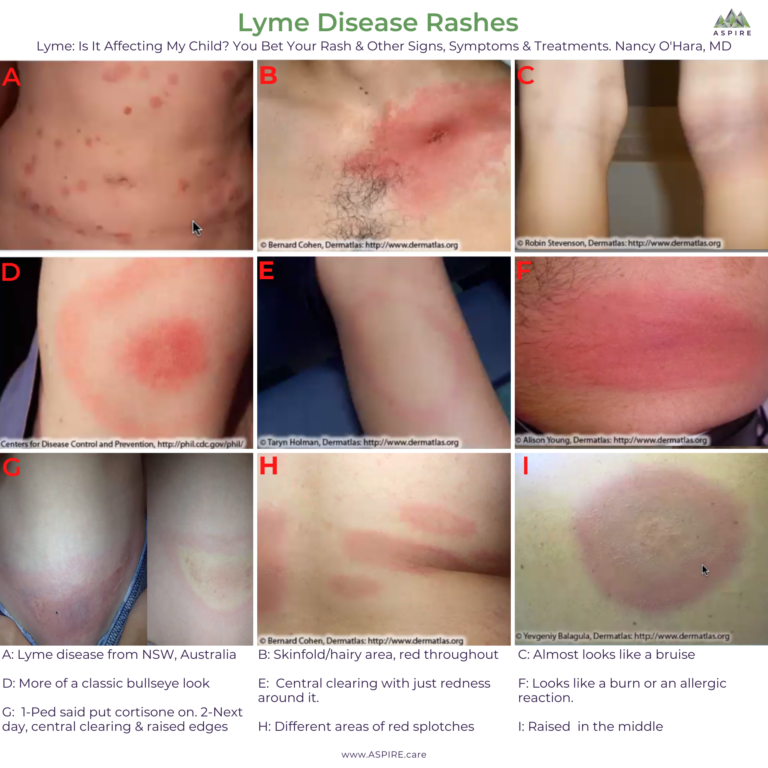
Lyme Disease Rashes And Look
Circular, expanding rash with target-like appearance.
Expanding rash with central crust
Expanding lesion with central crust on chest.
Expanding erythema migrans
Photo Credit: Reprinted from Bhate C, Schwartz RA. Lyme disease: Part I. Advances and perspectivesexternal icon. J Am Acad Dermatol 2011 64:619-36, with permission from Elsevier.
Description:Early, expanding erythema migrans with nodule.
Multiple rashes, disseminated infection
Early disseminated Lyme disease multiple lesions with dusky centers.
Red, oval plaque
Red, expanding oval-shaped plaque on trunk.
Expanding rash with central clearing
Circular, expanding rash with central clearing.
Bluish hued rash, no central clearing
Bluish hued without central clearing.
Expanding lesion, no central clearing
Expanding lesion without central clearing on back of knee.
Red-blue lesion with central clearing
Red-blue lesion with some central clearing on back of knee.
Insect bite hyper-sensitivity
Large itchy rash caused by an allergic reaction to an insect bite.
Fixed drug reaction
Description:A skin condition that occurs up to two weeks after a person takes a medication. The skin condition reappears at the same location every time a person takes that particular medication.
Ringworm
Description:Ringworm is a common skin infection that is caused by a fungus. Its called ringworm because it can cause a ring-shaped rash that is usually red and itchy with raised edges.
Pityriasis rosea rash
Granuloma annulare rash
Lyme Disease: A Pet Owner’s Guide
Lyme disease is an illness that affects both animals and humans what is known as a zoonotic disease and is the most commonly reported vector-borne illness in the United States, according to the U.S. Centers for Disease Control and Prevention . Transmitted through tick bites, the disease can be difficult to detect and can cause serious and recurring health problems. Therefore, it is best to prevent infection by taking appropriate measures to prevent tick bites and, for dogs, possibly vaccinating against the disease.
The bacterium that causes Lyme disease a worm-like, spiral-shaped bacterium called Borrelia burgdorferi is carried and transmitted primarily by the tiny black-legged tick known as the deer tick. Deer ticks are found in forests or grassy, wooded, marshy areas near rivers, lakes or oceans. People or animals may be bitten by deer ticks during outdoor activities such as hiking or camping, or even while spending time in their back yards.
Named after numerous cases were identified in Lyme, Conn., in 1975, the disease has since been reported in humans and animals across the United States and around the world. Within the U.S., it appears primarily in specific areas including the southern New England states eastern Mid-Atlantic states the upper Midwest, particularly Wisconsin and Minnesota and on the West Coast, particularly northern California. The CDC maintains a map detailing confirmed cases of Lyme disease throughout the years.
Don’t Miss: Tick And Lyme Disease Prevention
Drexel Lyme Disease Diagnostic Gets A Boost From Us Department Of Health And Human Services
Nearly half a million people become infected with Lyme disease in the United States each year a number expected to grow as climate change expands the range of the ticks that carry it. But despite its status as the countrys most common vector-borne disease, there is still no reliable way to detect the infection in its early stages when treatment is most effective.
A team of researchers from Drexel University has proposed a way to detect the bacterial infection by looking for a unique indicator that occurs before the immune system is able to launch a specific response. The groups method recently received a boost from a U.S. Department of Health and Human Services and the Steve & Alexandra Cohen Foundation initiative to finally find an effective test for the disease.
The challenge of detecting Lyme disease lies in the evasiveness of the Borrelia burgdorferi bacteria, which quickly moves into surrounding tissue once it enters the bloodstream, becoming virtually undetectable. Even the best tests are missing the early stages of infection about half the time, which means doctors are usually left to make a diagnosis based on symptoms and without confirmatory test results.
This altered response, while deleterious to the immune system, is key to the teams approach to early detection of Lyme disease.
Cdc Supports The Development Of New Tests

New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, they must be cleared by the Food and Drug Administration . For more details, see: Recommendations for Test Performance and Interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease.
Don’t Miss: How To Confirm Lyme Disease
Stage : Late Disseminated Lyme Disease
Timing: Months to years after a tick bite
The infection can spread to the joints or contribute to altered brain function, a condition known as encephalopathy.
Common symptoms of late disseminated Lyme disease include:
-
Arthritis with joint pain, warmth, and swelling that may be constant or come and go. Lyme disease-related arthritis typically occurs in one joint, usually the knee or another large joint, though it can also occur in more than one joint.
-
Concentration issues, brain fog, and memory issues
-
Nerve pain that feels like tingling, numbness, burning, or stabbing in the hands and feet
-
Anxiety, depression, mood swings, and other neuropsychiatric issues
-
Sleep disturbances such as difficulty falling or staying asleep, need for extended sleep, or unrefreshing sleep.
You may also experience a worsening of earlier Lyme disease symptoms.
In some people, Lyme disease can cause debilitating fatigue and sleep disturbances . Lyme disease-related arthritis typically occurs in a large joint like the knee .
Who Gets Lyme Disease And At What Time Of Year
Lyme disease is transmitted via the bite of infected ticks, which attach to any part of the body, but often to moist or hairy areas such as the groin, armpits, and scalp.
While everyone is susceptible to tick bites, campers, hikers, and people who work in gardens and other leafy outdoor venues are at the greatest risk of tick bites. As many a suburban gardener can attest, with the expansion of the suburbs and a push to conserve wooded areas, deer and mice populations are thriving, too, providing ample blood meals for ticks. For lyme disease to be transmitted, a tick needs to feed on the host for 24-48 hours.
In the majority of cases, tick bites are reported in the summer months when ticks are most active and people spend more time outdoors. But this can extend into the warmer months of early autumn, too, or even late winter if temperatures are unusually high. Similarly, a mild winter can allow ticks, much like other insects, to thrive and emerge earlier than usual.
Recommended Reading: How To Tell You Have Lyme Disease
Is There Already A Lyme Disease Vaccine
The FDA previously approved a Lyme disease vaccine called Lymerix in 1998. Manufactured by SmithKline Beecham , Lymerix reduced new infections in adults by nearly 80%, according to the journal Epidemiology and Infection.
But some patients testified that they later developed arthritis. Even though an FDA investigation failed to show a link, media reports about the claims led to declining use and dwindling sales at the time.
Lymerix was pulled from the market in 2002, after just three years.
Who Gets Lyme Disease
Lyme disease can affect people of any age. People who spend time outdoors in activities such as camping, hiking, golfing, or working or playing in grassy and wooded environments are at increased risk of exposure. The chances of being bitten by a deer tick are greater during times of the year when ticks are most active. Ticks can be active any time the temperature is above 45° F. Young deer ticks, called nymphs, are active from mid-May to mid-August and are about the size of poppy seeds. Adult ticks are most active from March to mid-May and from mid-August to November and are about the size of sesame seeds. Both nymphs and adults can spread Lyme disease. Infected deer ticks can be found throughout New York State.
Don’t Miss: What Are Some Treatments For Lyme Disease
Who’s At Risk Of Lyme Disease
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.
Lyme Disease Has Affected Celebrities Such As Avril Lavigne Kelly Osbourne And Shania Twain Among Others
If you happen to encounter the wrong tick, a walk in the woods can turn into a lingering battle with Lyme disease. Early signs and symptoms of Lyme disease, the result of a tick bite, include a bulls-eye shaped rash and flu-like symptoms that can be very mild and may even go unnoticed. And in at least a quarter of Lyme disease patients, the telltale rash does not develop, according to the National Institute of Allergy and Infectious Diseases .
Most cases can be treated successfully with antibiotics, but if Lyme disease is not detected early, it can cause serious and debilitating symptoms such as nerve pain, severe headaches, arthritis, and cognitive problems. As the NIAID notes, fatigue, pain, and aching joints and muscles can persist in some patients even after treatment, which is known as post-treatment Lyme disease syndrome. The symptoms and complications of Lyme disease especially when it comes to what has been called chronic Lyme, though experts are wary of that term are complex and not well-defined. But of course people should seek a medical evaluation if they are feeling unwell, and Lyme disease should be investigated if there has been a history of a tick bite.
Read Also: Ultrasound Therapy For Lyme Disease
Lyme Disease Test And Treatment
If you think you may have Lyme disease, contact your physician right away.
Your doctor may do a test for Lyme disease. The FDA regulates diagnostic tests to ensure that they are safe and effective. Its important to know that blood tests that check for antibodies to the bacterium that causes Lyme disease are not useful if done soon after a tick bite. It typically takes 2 to 5 weeks after a tick bite for initial antibodies to develop.
For this reason, your doctor may recommend treatment with antibiotics before the diagnostic tests are complete. According to the CDC, patients treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely.
How Will My Doctor Test Me For Lyme Disease
The CDC recommends two-step testing, sometimes referred to as a two-tiered test, for Lyme disease. You will need to go to a lab to have blood drawn. It takes a few days to get results.
If the first test comes back positive or unclear, the lab will do the second blood test. If the first test comes back negative, the CDC does not recommend the second test. However, according to the CDC the second test must be positive for you to be diagnosed with Lyme disease.
The first test: ELISA
This blood test is for antibodies against the Lyme disease bacteria. Because it can take some time for your body to produce antibodies, this test isnt always accurate soon after a person is infected.
The second test: Western Blot or a second ELISA
There are two options for the second test. One is called a Western blot, which looks at how your antibodies react to specific parts of the Lyme disease bacteria. The Western blot test has been part of the two-step testing system since 1994 and is more commonly used.
The other option is to do a second ELISA test, which measures antibodies to a specific protein found on Lyme disease bacteria. Because these tests are newer, not all doctors have experience with them and not all labs have access to them.
These tests can be run on the blood sample used for the first test. You should not need to go back to the lab.
A possible drawback of the two-step testing system
Which second test is best: ELISA or Western blot?
Read Also: Lyme Old Lyme High School