Lyme Disease Frequently Asked Questions
If you have not done so already, remove the tick with fine-tipped tweezers.
The chances that you might get Lyme disease from a single tick bite depend on the type of tick, where you acquired it, and how long it was attached to you. Many types of ticks bite people in the U.S., but only blacklegged ticks transmit the bacteria that cause Lyme disease. Furthermore, only blacklegged ticks in thehighly endemic areas of the northeastern and north central U.S. are commonly infected. Finally, blacklegged ticks need to be attached for at least 24 hours before they can transmit Lyme disease. This is why its so important to remove them promptly and to check your body daily for ticks if you live in an endemic area.
If you develop illness within a few weeks of a tick bite, see your health care provider right away. Common symptoms of Lyme disease include a rash, fever, body aches, facial paralysis, and arthritis. Ticks can also transmit other diseases, so its important to be alert for any illness that follows a tick bite.
References:
Moody KD, Barthold SW, 1991. Relative infectivity of Borrelia burgdorferi in Lewis rats by various routes of inoculation.Am J Trop Med Hyg 44: 135-9.
There are no reports of Lyme disease being spread to infants through breast milk. If you are diagnosed with Lyme disease and are also breastfeeding, make sure that your doctor knows this so that he or she can prescribe an antibiotic thats safe for use when breastfeeding.
Do You Have Lyme Disease What You Need To Know About Covid
Founder, Medical Director, Flatiron Functional Medicine
Its early 2020 and chances are, if you pick up a newspaper or flip on the news, youre going to be bombarded with coronavirus updates. And if youre living with Lyme disease and its devastating effects, you are likely concerned about how to best protect yourself during this difficult time.
Lyme disease and the co-infections that often accompany it, can weaken your immune system and make you more susceptible to catching contagious illnesses like the coronavirus. But the good news is, you have control over how you react and can take some powerful steps to defend yourself against this emerging virus.
Lets take a look at exactly how you can best protect yourself from coronavirus while living with Lyme disease.
Why Do People Get Chronic Lyme Disease
Lyme Disease has eluded doctors for many years. Those who are bitten by the infectious deer tick usually do not realize they have been bitten and do not show the telltale sign of the bullseye rash anywhere on there skin. In fact, only 1 in 5 Lyme sufferers ever exhibit such a symptom, yet it is often the only clear-cut sign that doctors can solely identify as being representative of Lyme. If and when a person is diagnosed with Lyme, mainstream medical practitioners will usually treat him or her with a two-to-three week course of antibiotics. Considering Lyme disease is a bacterial infection, the antibiotic treatment seems practical and in some cases, will rid the person of Lyme completely.
However, if the disease has gone untreated, the likelihood that one short course of antibiotics will kill the bacteria entirely is unlikely. Although symptoms may disappear for a short while, the remaining bacteria will eventually flourish once more and many who have been treated will relapse back into full-blown, chronic Lyme.
In an even more unfortunate circumstance, some Lyme sufferers are diagnosed far too late into their infection. With such vague and overlapping symptoms, Lyme is often misdiagnosed or mistreated, leaving the patient with chronic pain that only seem to worsen with time. Although the disease is fairly common, doctors frequently dismiss Lyme in lieu of other medical problems including depression, chronic fatigue, andin the most extreme caseshypochondria.
Recommended Reading: Best Essential Oils For Lyme Disease
Early Detection Is Key
Avoiding a Lyme disease misdiagnosis and possible complications depends on timely, accurate testing. Lyme disease should not be discounted in patients presenting with autoimmune disease-like symptoms, even if the patient doesnt remember a tick bite or rash. Even if the patient has a history of or genetic predisposition to autoimmune disorders, the presence of such a disorder doesnt rule out Lyme disease.
But diagnosing Lyme disease requires more specific, sensitive testing than is typically recommended by the CDC, especially at later stages of the disease. Learn why IGeneX tick-borne disease tests are different.
What Is The Most Accurate Test For Lyme Disease
Although there are at-home kits for Lyme disease, a blood test is still the most accurate way to diagnose this health condition as it is performed by experts in the field. Here are two blood tests you can order online or book in labs near you.
This test often uses Western blot or immunoblot to identify antibodies produced when the causative bacteria infect the tissues. These antibodies are released by immune cells, specifically against Lyme diseases pathogen . During the immunoblot, the antibodies are isolated from the blood sample and matched accordingly.
You can order an antibody test online and choose from an immunoblot blood test or Ab with reflex to blot blood test.
The ELISA test follows the same principle as that of the immunoblot test. It also detects antibodies associated with Borrelia burgdorferi. However, because the test can produce false negative and positive results, it is typically taken together with the Western blot for further verification. When choosing the most accurate test, consider the most efficient option and the symptoms you experience. Your doctor may recommend taking both tests to identify the causative agent. Likewise, getting both ELISA and western blot blood tests increases the accuracy of Lyme disease diagnosis by 99.9%.
Read Also: Old Lyme Waterfront Homes For Sale
Can You Get Lyme Disease Twice
You can be reinfected with Lyme disease if a carrier tick bites you for the second time. You may notice the same symptoms, especially the rash that looks like a bullseye .
On the other hand, Lyme disease flare-ups, or the tendency to experience the same symptoms even without getting exposed to deer ticks, indicates chronic Lyme disease.
Genomic Insights From Borreliaceae Lineages
Between 1982 and 2010, the B. burgdorferi species complex, known as B. burgdorferi sensu lato, steadily expanded from 1 to 18 species as isolates from tick vectors, their hosts, and patient samples were characterized . A subset of these species are associated with human disease. B. burgdorferi sensu stricto in the USA, as well as B. afzelii and B. garinii in Eurasia are the most common agents of LD in the Northern hemisphere. Cases of LD in Europe are also caused by Bb and B. bavariensis , but are less common. B. spielmanii , B. bisettiae , and B. lusitaniae have been identified in human specimens but their clinical importance is less clear. B. valaisiana has been identified in human specimens , but others have recently provided compelling reasons why existing evidence does not support it being considered a human pathogen . Additional species have been identified in tick vectors or their hosts, but not in patient samples.
Recommended Reading: Lyme Disease Specialist In Virginia
Autoimmune Disease And Lyme Disease
The incidence of PTLDS has increased over the years, and patients who have undergone antibiotic treatments are coming forward with symptoms they thought had disappeared long ago. Research has revealed that even long-term antibiotic treatment can leave some of the Lyme bacteria unscathed. When the bacteria is not completely eradicated, superficial symptoms can cascade into more serious, neurological conditions.
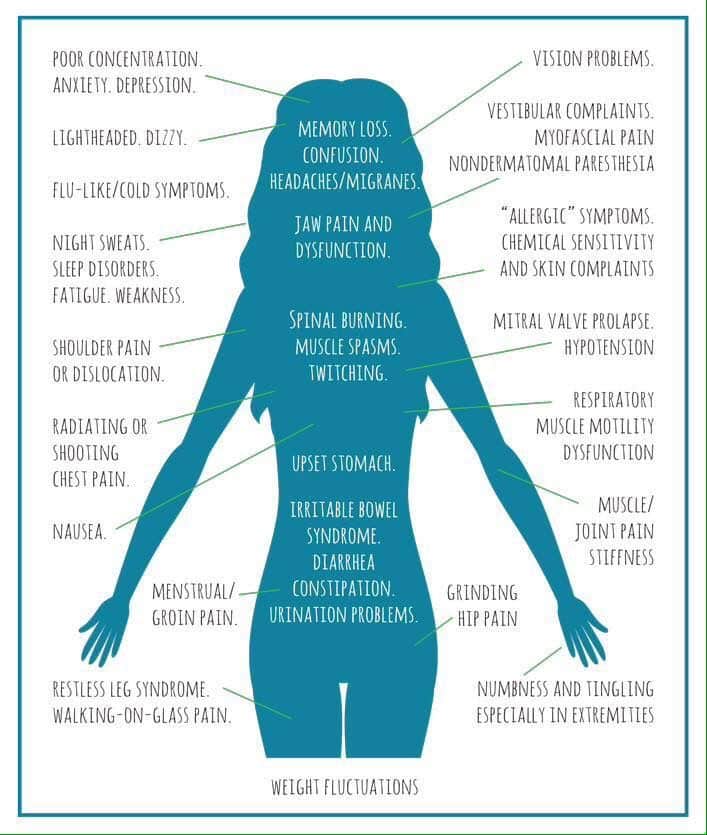
It is not surprising that chronic Lyme patients might also be afflicted with autoimmune diseases like multiple sclerosis or rheumatoid arthritis. What starts off as a disease bearing physical symptoms like sore joints and chest pain can transform into a chronic illness bearing symptoms of cognitive dysfunction, memory problems, chronic fatigue, and mood disorders.
Medical specialists believe the autoimmune response that triggers the aforementioned symptoms is a result of the residual damage that occurs during the initial infection. The outer coat of the Lyme bacteria is similar to tissue found in our nervous system, and it is believed that the immune system reacts to this leftover tissue, attacking it and mistakenly attacking neuronal tissue as well. Thus, the bacterial tissue that was not eliminated via antibiotics confuses the immune system. The onset of chronic symptoms thereafter are misattributed to other autoimmune diseases, and likewise, the autoimmune diseases may be a direct result of the Lyme infection itself.
It Starts With An Unusual Bacterium
Lyme disease can affect any organ or system within the body, including the brain, nervous system, muscles, joints, and heart. Most cases of Lyme disease in the U.S. are caused by a corkscrew-shaped spirochete called Borrelia burgdorferi. This organism has a unique way of evading the human immune system starting as early as when the tick bite occurs and has learned to survive in the human body even when aggressive treatment attacks are mounted against it.
You May Like: Lyme Disease Levels In Dogs
A New Study Has Shown That The Bacteria That Causes Lyme Disease Alters The Immune System Causing It To Attack The Healthy Cells In The Human Body
The bacteria that causes Lyme disease Borrelia burgdorferi has been shown to stop communication between dendritic cells and T-cells, which normally signals for a response against foreign invaders.
The study, carried out by researchers at the Johns Hopkins Lyme Disease Clinical Research Center, has demonstrated that the bacteria alters dendritic cells, which normally present proteins from pathogens such as bacteria and viruses, known as antigens, to immune system T-cells, which then signals an immune response against any viruses or infections.
The study has been published in Frontiers in Medicine.
Does Lyme Disease Affect Your Immune System Long Term
The bacteria initially trigger a strong immune response in an infected animal, but findings from this study indicate that the bacteria soon cause structural abnormalities in germinal centers sites in lymph nodes and other lymph tissues that are key to producing a long-term protective immune response.
Also Check: Lyme Disease Rash Early Stage
Who Is Most At Risk Of Contracting The Coronavirus
While anyone can potentially catch the coronavirus even if theyre young and healthy the primary concern is the extent to which coronavirus may affect you. The people most susceptible to serious and life-threatening reactions to COVID-19 are individuals that:3
- Have respiratory diseases
- Those above 65 years of age
- Are immune-compromised
- Have other underlying serious health conditions
Having an underlying infection like Lyme disease as well as the co-infections that usually come along with it, puts you at an increased risk when it comes to coronavirus. So, especially important to take precautions to protect yourself.
Support Your Immune System
When your immune system is in overdrive, it needs all the support it can get to keep running. Fortunately, there are some things you can do to give your immune system a boost so it can better fight off infection. Heres what I suggest:
- Load up on antioxidants: Loading up on anti-inflammatory foods is one way to get antioxidants. But I also recommend taking a daily dose of concentrated antioxidants with supplements like Liposomal Glutathione and Buffered C Powder.
- Take immune bolstering supplements: Your immune system relies on certain compounds to function properly. For example, it needs N-Acetyl Cysteine to make antioxidants and vitamin D to modulate immune function. Taking these supplements daily gives your immune system the tools it needs to run effectively.
- Support your gut: The health of your digestive tract is closely tied to the health of your immune system. One of the best ways to keep your gut happy is to maintain the right balance of beneficial bacteria by taking a daily probiotic. In addition, Gut Immune powder has been shown to passively bind pathogens in the gut.
- Assist your body in eliminating pathogens: Certain nutrients and botanical extracts like those found in Virastat or Immune Booster can enhance your immune systems ability to fight viruses.
Giving your immune system a boost will also help you feel more energized and healthy.
Read Also: Chances Of Lyme Disease After Tick Bite
Who’s At Risk Of Lyme Disease
The risk of getting Lyme disease is higher:
- for people who spend time in woodland or moorland areas
- from March to October because more people take part in outdoor activities
It’s thought only a small proportion of ticks carry the bacteria that cause Lyme disease. Being bitten doesn’t mean you’ll definitely be infected. However, it’s important to be aware of the risk and speak to a GP if you start to feel unwell.
Lyme Disease And Coronavirus An Increased Risk
Being infected with Lyme disease and a potential cocktail of other tick-borne infections spells trouble for your immune system in the sequence:
- Borrelia Burdorferi can actually disable certain aspects of your immune system. This suppression of your immune system allows the bacteria to hideout in your body
- While certain aspects of your immune system may be disabled, it doesnt entirely shut it off. Your body still launches attack after attack in an attempt to eliminate both Lyme disease and any other co-infectious microorganisms, if present.
- This low-level chronic inflammation taxes your immune system, leaving it with less and less resources to direct at any new threats
- This exhaustion of your immune system can eventually cause your immune system to malfunction entirely leading to autoimmunity where your body mistakenly begins attacking itself.8
This sequence of events means your immune system is not functioning on all cylinders. So if youre exposed to a potentially dangerous virus like the coronavirus your body is less prepared to fight it off.
Also Check: At Home Treatment For Lyme Disease
Is There Treatment For Renal Damage Caused By Lyme Disease
As mentioned above, the only treatment available for Lyme disease is antibiotics. Following this, lingering symptoms need to be treated separately and specifically for their severity. If kidney disease does develop because of Lyme disease infection, it will need to be treated separately but in conjunction with other symptoms and chronic ailments.
To control the symptoms and slow further damage to the kidneys, doctors may prescribe medications for:
- High blood pressure
- A low-protein diet
These medications all play a critical role in the restoration of the renal system, but each one will be specific to a patients needs and their level of kidney damage. In the worst cases, kidney disease can progress to a dangerous level. This is called end-stage kidney disease. In this case, treatment will come in the form of dialysis or a kidney transplant. These more serious treatments are done only in the worst cases to avoid complete kidney failure.
Image by on Pixabay: Can Lyme disease cause urinary retention? Yes, and it could lead to serious kidney disease if left untreated.
How To Manage Inflammation In Lyme Disease
Infection with Borrelia burgdorferi, the bacterial cause of Lyme disease, and co-infections causes the immune system to launch a profound inflammatory response. While antibiotic treatments, such as doxycycline and cefuroxime, can destroy B. burgdorferi, these drugs do little to mitigate the inflammatory response launched in response to these microbes. Left untreated, Lyme-induced inflammation damages cells, tissues, and organs, inducing widespread bodily dysfunction.
While the CDC offers recommendations for Lyme disease treatment from the antimicrobial perspective, it makes no recommendations as to how affected individuals should manage the inflammatory side effects of the illness. Functional medicine, on the other hand, offers a unique set of tools for managing Lyme-associated inflammation, including nutrition changes, lifestyle changes, and natural anti-inflammatory compounds. These holistic interventions can significantly improve Lyme disease inflammation, creating a strong foundation for healing.
Recommended Reading: How Do You Find Out If You Have Lyme Disease
Medically Approved By Dr Edward Salko Md
Dr. Edward Salko is the board-certified physician who reviews lab tests provided by PERSONALABS. He earned his Bachelor of Science in chemistry and pre-med from the University of Florida in Gainesville and his Doctor of Osteopathy Medicine in 1980 from Kansas City University School of Medicine.
Dr. Salkos career has specialized in family and emergency medicine. His passion is to provide clients with the tools they need in the most convenient way possible to allow them to take charge of their own healthcare. He has held a variety of positions in Kansas, Florida and Washington. Currently, in addition to his duties as Medical Director for Personalabs, he is a practicing emergency physician in Kennewick, Washington.
Does Having Lyme Disease Weaken Your Immune System
A new study has shown that the bacteria that causes Lyme disease alters the immune system, causing it to attack the healthy cells in the human body.
Does Lyme stay in your system forever?
If treated, Lyme disease does not last for years. However, for some people, the after-effects of the disease can linger for months and sometimes even years.
Does Lyme disease leave lasting effects?
In a study of 61 people treated for the bacteria that causes Lyme disease, Johns Hopkins researchers conclude that fatigue, pain, insomnia and depression do indeed persist over long periods of time for some people, despite largely normal physical exams and clinical laboratory testing.
What are the long term side effects of Lyme disease?
Chronic symptoms of Lyme are a much longer list and may include vertigo, ringing in the ears, short-term memory loss, light and sound sensitivity, mood swings, anxiety, depression, heart palpitations, and serious cardiac problems.
Don’t Miss: Single Dose Lyme Vaccine For Dogs
Lyme Disease And The Autoimmune Connection
Each year, more than 30,000 new cases of Lyme disease are reported to the Centers for Disease Control and Prevention , although the true prevalence is likely to be closer to 476,000 and its on the rise. While not classified as an autoimmune disease, research indicates that Lyme disease may trigger an autoimmune response and/or its symptoms may mimic an autoimmune disease.
Lyme disease is caused by the bacteria Borrelia burgdorferi and Borrelia mayonii, transmitted through the bite of an infected blacklegged tick. Left untreated, Lyme disease can cause chronic joint inflammation , typically in the knee but also occurring in the shoulders, ankles, elbows, and wrists neurological symptoms, such as facial palsy and neuropathy cognitive defects, such as impaired memory heart palpitations and irregular heartbeat and nerve pain. Lyme disease usually responds well to antibiotics, and prompt treatment can help avoid these escalating effects on the body.
As Meghan described, the first signs of Lyme disease are often flu-like symptoms, such as fever, chills, headache, fatigue, muscle, joint pain, and swollen lymph nodes. In 70-80% of infected people, a rash in the pattern of a target or bulls-eye will appear. This rash, known as erythema migrans, can spread over a large part of the body over several days. While this rash is one of the hallmarks of Lyme disease, not everyone who has been infected will develop it.
Post-Treatment Lyme Disease Syndrome and Autoimmune Diseases