What Are The Risk Factors For Post Treatment Lyme Disease
Risk factors for Post Treatment Lyme Disease include:
- Delay in diagnosis
- Increased severity of initial illness
- Presence of neurologic symptoms
Increased severity of initial illness, the presence of neurologic symptoms, and initial misdiagnosis increase the risk of Post Treatment Lyme Disease. PTLD is especially common in people that have had neurologic involvement. The rates of Post Treatment Lyme Disease after neurologic involvement may be as high as 20% or even higher. Other risk factors being investigated are genetic predispositions and immunologic variables.
In addition to Borrelia burgdorferi, the bacteria that causes Lyme disease, there are several other tick-borne co-infections that may also contribute to more prolonged and complicated illness.
If My Animal Is Positive On The Assay Should He/she Be Treated For Lyme Disease
If your animal is displaying clinical signs of Lyme disease and is positive on the Lyme Multiplex assay, it is advisable to discuss treatment options with your veterinarian. If your animal appears healthy, discuss the risks and benefits of treatment and develop a monitoring plan with your veterinarian.
How Lyme Disease Can Affect The Entire Body
Holtorf Medical Group
Lyme disease can affect any organ or system within the body, including the immune system, brain, nervous system, heart, and gut. Most cases of Lyme disease in the U.S. are caused by a corkscrew-shaped spirochete called Borrelia burgdorferi. This organism has a unique way of evading the human immune system starting as early as when the tick bite occurs and has learned to survive in the human body even when aggressive treatment attacks are mounted against it.
You May Like: How Do You Treat Lyme Disease In Humans
Symptoms Of Lyme Disease
The first sign of a tick bite is usually a small red lump similar to a mosquito bite where the tick has attached to the skin. While not every tick carries the Lyme disease bacteria, common early symptoms of infection include:
- Flu-like ailments including fever, headache, fatigue, swollen lymph nodes, and muscle or joint aches.
- According to the CDC, 70-80% of infected people experience an Erythema migrans rash. Typically appearing a week after being bitten, the rash expands gradually and may be warm to the touch.
While these early symptoms occur in the first 30 days of infection, later-stage symptoms can be quite severe. Sometimes occurring months after being infected, these symptoms include:
- Additional rashes
The Mayo Clinic also advises less common symptoms such as:
- Liver inflammation
- Inflammation in the membranes of the brain
- Eye inflammation
The Chance Of Getting Lyme Disease
Not all ticks in England carry the bacteria that causes Lyme disease.
But it’s still important to be aware of ticks and to safely remove them as soon as possible, just in case.
Ticks that may cause Lyme disease are found all over the UK, but high-risk places include grassy and wooded areas in southern and northern England and the Scottish Highlands.
SINCLAIR STAMMERS/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/263611/view
Ticks are tiny spider-like creatures that live in woods, areas with long grass, and sometimes in urban parks and gardens. They’re found all over the UK.
Ticks do not jump or fly. They attach to the skin of animals or humans that brush past them.
Once a tick bites into the skin, it feeds on blood for a few days before dropping off.
Also Check: Can You Get Rid Of Lyme Disease In Humans
The Cdc Reveals The Truth About Lyme Disease
Content updated from previous publish date.
Lyme disease is a bacterial infection caused by the bite of an infected black-legged tick, also known as a deer tick. Lyme disease is primarily known for causing a rash and flu-like symptoms, but according to the CDC, it can persist in some people and lead to what is called Post-Treatment Lyme Disease Syndrome .
Lyme disease is associated with numerous co-infections that can mimic or contribute to virtually any medical, neurological, or psychiatric condition, which is why Lyme has been called the great imitator. Lyme has been vastly underdiagnosed in the U.S., in part to inadequate testing methods, but also because of a general lack of acknowledgment within the medical community that chronic Lyme or PTLDS are real.
In the medical community, Lyme remains misunderstood at best and dismissed at worse. How can doctors treat an illness if they dont believe it exists? They cant, which is why far too many people have been suffering from Lyme brain for far too long.
At Amen Clinics, hundreds of patients struggling with resistant complex symptoms have tested positive for Lyme disease and gotten significantly better when it was treated.
Symptoms Of Post Treatment Lyme Disease
- Include severe fatigue, musculoskeletal pain, & cognitive problems
- Can significantly impact patients health and quality of life
- Can be debilitating and prolonged
Our research indicates the chronic symptom burden related to PTLD is significant. Although often invisible to others, the negative impact on quality of life and daily functioning is substantial for PTLD sufferers.
The chronic symptom burden related to Lyme disease is considerable, as shown on the left side of the graph above, and statistically significantly greater than the aches and pains of daily living experienced by the control group, on the right.
Also Check: How Do You Test For Lyme Disease In Dogs
Wipe It Out In The Wild
Any effort to snuff out Lyme disease has to start with its eight-legged bloodsucking hosts. Until you get rid of it in the environment, youve got to keep investing in prevention in humans, Hu said. Whereas if you wipe it out in the wild, its one and done, right? Eradicating Lyme in the ecosystem, however, is easier said than done. While the bacteria that cause the disease live in ticks, the ticks dont pass it down to their offspring directlyinstead, they feed on a vertebrate host, such as a white-footed mouse, and pass the pathogen to it. When another tick feeds on that same host, it too picks up the bacterium.
Many of the efforts by Hu and other scientists have been focused on breaking that chain. One promising technique Hu developed, for example, was to vaccinate mice by leaving out vaccine-infused food for them. The oral vaccine contained a virus that would express a Borrelia antigen that would make the mice immune to Lyme. The idea was to feed it to mice in the wild, and have fewer infected mice, which would translate into fewer infected ticks, and fewer human cases, Telford said. While the scientists insist the technique is safe, however, its been held up by the U.S. Department of Agriculture, which is leery about releasing a virus in a world beset by a pandemic. We got stuck in regulatory purgatory, Hu said. No one wants to put a live virus out in the wild right now.
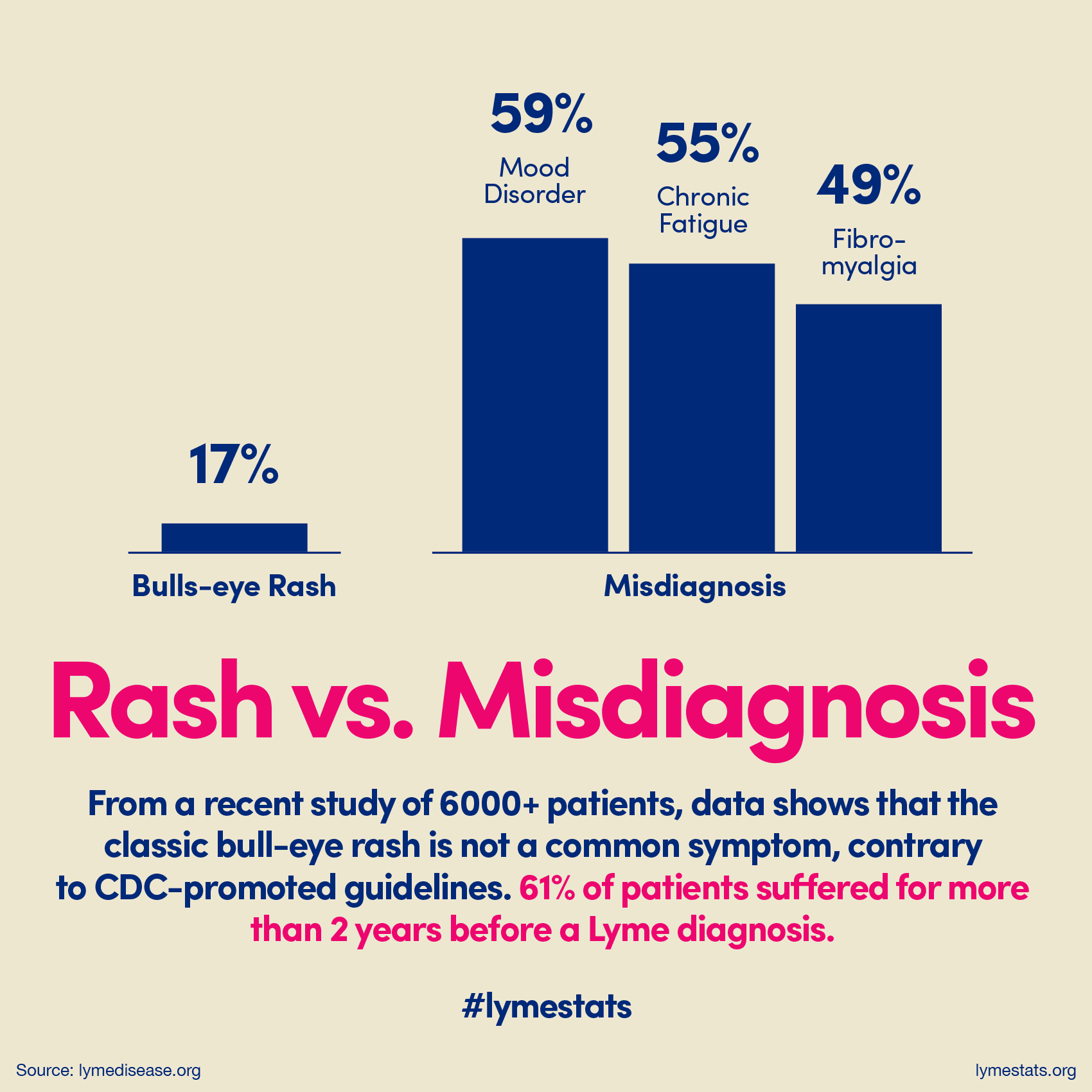
Lyme Disease: Misdiagnosis And Delayed Treatment
People who are diagnosed with Lyme disease within the first few weeks of being infected are fortunate because the appropriate antibiotics have a much better chance of working when used early. Unfortunately, Lyme disease is often missed and the infection is allowed to take hold, disrupting the immune system and causing a cascade of inflammatory responses.
Even when Lyme is suspected and a blood test is ordered, the common Western Blot test often results in false negatives. In addition, traditional medical practice rarely tests for Lymes co-infection antibodies, even though they may even be more common than Lyme itself!
Its not uncommon for someone with Lyme disease to get multiple negative test results before receiving a proper diagnosis. This leaves thousands of undiagnosed patients feeling sick and confused and spending months, years, or even decades wandering around from doctor to doctor trying to find out what is wrong with them. This means that some people with Lyme encounter financial ruin before finding a treatment that works.
Recommended Reading: Lyme Ct Real Estate For Sale
How Can Lyme Disease Last For Years
Category: Health Published: October 9, 2015
If treated, Lyme disease does not last for years. However, for some people, the after-effects of the disease can linger for months and sometimes even years. Alternative medicine providers call this condition “Chronic Lyme disease,” but this title is simply wrong. For a person who has been infected with Lyme disease and then treated, the bacteria that causes Lyme disease is measurably no longer present in his body, even though he may still feel some symptoms. The correct title for this condition is therefore “Post-treatment Lyme Disease Syndrome.”
Lyme disease is an infection caused by a bacteria known as Borrelia burgdorferi. This bacteria is delivered to humans through tick bites. From the bite site, the bacteria can enter the bloodstream and spread throughout the body. Usually, but not always, an infectious tick bite causes a characteristic red rash at the site of the bite. Other symptoms include fever, muscle soreness, headache, fatigue, and dizziness. In a few cases, symptoms can also include mood swings, memory loss, and sleep disturbance. If left untreated for too long, Lyme disease can lead to nerve damage, thereby causing shooting pain, numbness, and even paralysis.
The CDC states,
Can You Get Symptoms Of Lyme Disease Years Later
If Lyme disease is not diagnosed and treated early, the spirochetes can spread and may go into hiding in different parts of the body. Weeks, months or even years later, patients may develop problems with the brain and nervous system, muscles and joints, heart and circulation, digestion, reproductive system, and skin.
Read Also: Inns In Old Lyme Ct
For Animals That Have Not Been Vaccinated Can Osp A Values Be Positive How Should This Be Interpreted
Antibodies to OspA have previously been interpreted as markers for vaccination. Non-vaccinated animals usually have low values for antibodies to OspA, while vaccinated animals develop these antibodies. OspA antibodies have been shown to protect from infection with B. burgdorferi.
However, there is accumulating evidence that antibodies to OspA can occur without vaccination. First, residual OspA is present on the bacterial surface at the time of transmission to an animal. This causes a low and transient OspA antibody response early after infection. Second, antibodies to OspA have also been associated with treatment-resistant Lyme arthritis and with development of autoimmunity in human patients. Similarly, OspA antibodies in non-vaccinated dogs or horses can be considered as markers of chronicity and disease severity.
Which Antibodies Does The Vaccine From Merial Induce

It is a recombinant vaccine based on Osp A. Vaccinated animals should develop high antibody levels to OspA and maintain negative antibody levels to the remaining two antigens. Infected/non-infected animals can be identified based on OspC and OspF antibody values. Detection of the early Lyme infection stage is possible after using this vaccine.
You May Like: What Is Chronic Neurological Lyme Disease
Why Are Antibiotics The First Line Of Treatment For Lyme Disease
The use of antibiotics is critical for treating Lyme disease. Without antibiotic treatment, the Lyme disease causing bacteria can evade the host immune system, disseminate through the blood stream, and persist in the body. Antibiotics go into the bacteria preferentially and either stop the multiplication of the bacteria or disrupt the cell wall of the bacteria and kill the bacteria . By stopping the growth or killing the bacteria the human host immune response is given a leg up to eradicate the residual infection. Without antibiotics, the infection in Lyme disease can evade the host immune system and more readily persist.
What Does The Lyme Multiplex Assay Measure
The Lyme Multiplex assay quantifies antibodies directed against specific proteins on the surface of B. burgdorferi at three different stages of the bacterial life cycle. This antibody profile can indicate whether an animal has been recently infected or is chronically infected with B. burgdorferi. It can also be used to monitor protective antibodies after vaccination.
Recommended Reading: Vacation Rentals Old Lyme Ct
How Much On Average Does It Cost To Treat Lyme Disease In Dogs
The cost of Lyme disease treatment in dogs can vary by a number of factors, including where you live. From there, Dr. Muller says, The costs often depend on the treatment duration. A four-week antibiotic course might cost around $800, plus the cost of the diagnostic blood tests may approximately be an additional $80 to $200 depending on the type of tests, in addition to the vet consultation fees. Add in the cost of your dogs prescription medications, and that can be costly for many pet parents. Having pet insurance can help cover these crucial veterinary expenses in a big way. That said, while Pumpkin Pet Insurance covers tick infections and tick-borne diseases like Lyme, not all pet insurance providers will. In addition to discussing your treatment options with your veterinarian, make sure to check with your insurance provider to see what conditions are covered.
Also Check: How Long Lyme Disease Last
Lyme Disease: Resolving The Lyme Wars
- By , Contributor
Its finally getting warm here in New England, and most of us have plans to enjoy the beautiful weather. And thats why the Centers for Disease Control and Prevention recently released a report raising awareness about how to prevent the tickborne infections that typically occur during this time of the year. Lyme disease is probably the most well-known, and the one for which diagnosis and treatment are most controversial.
Read Also: How To Get Diagnosed With Lyme Disease
How Is Lyme Disease Diagnosed
A healthcare provider will diagnose Lyme disease based on symptoms, physical findings and whether or not you’ve been in an area populated by infected ticks.
Many people dont remember or know that theyve been bitten by a tick. This is because the tick is tiny, and its bite is usually painless.
Your provider will confirm the diagnosis using a blood test. If your first blood test is negative for Lyme disease, you won’t need another test. If the first test is positive or equivocal, your provider will conduct the test again. You have to have two positive results to be diagnosed with Lyme disease.
Can My Dog Recover From Lyme Disease
If you are able to detect the disease early, symptoms should disappear within the first 3 days of your pup’s treatment.
However, while treatment is usually very effective at eliminating signs of Lyme disease, dogs with Lyme disease can remain positive for the rest of their lives. If your dog tests positive for Lyme disease but is not showing any symptoms, your vet may not recommend treatment.
Most dogs infected with Lyme disease will eventually develop arthritis.
However, potentially serious kidney issues can result from a dog carrying Lyme disease. It is easy for these problems to go unnoticed until it is too late. If your vet identified that your dogs kidneys have been affected by Lyme disease, they will be able to monitor and treat the condition before more serious problems arise.
Read Also: What Is Lyme Vaccine For Dogs
How Do I Remove A Tick From My Dog
Check your pet immediately after it has been in a tick-infected area. The deer tick is a small tick and only about pinhead size in juvenile stage, but is a little more obvious in the adult phase and after feeding. If you find a tick moving on your pet, the tick has not fed. Remove the tick promptly and place it in rubbing alcohol or crush it between two solid surfaces. If you find a tick attached to your pet, grasp the tick with fine tweezers or your finger nails near the dog’s skin and firmly pull it straight out. There are also tools available called Tick Twister® or Tick Key® which can be useful. However, take care to use them cautiously as twisting or jerking the tick may cause the mouth parts to break off and remain in the skin. See your veterinarian if you are unsure or unable to remove the tick from your dog.
Make sure you protect your fingers from exposure by using a tissue or a disposable glove.You may need another person to help restrain your dog. Removing the tick quickly is important since the disease does not appear to be transmitted until the tick has fed for approximately 12 hours. If you crush the tick, do not get the tick’s contents, including blood, on your skin.
Note: The bacterium that causes Lyme disease can pass through a wound or cut in your skin.
Woman Will Forever Live With Chronic Lyme Disease
Its like living with a fake illness, said Denise Nichols.
ROCKFORD, Ill. – A Boone County Occupational Therapist who helps people with chronic illnesses find herself as the patient fighting a potentially debilitating disease.
Every Four of July, Denise Nichols marks another year since being diagnosed with Lyme Disease. It is spread from mouse to tick and through the bite of a tick into the humans blood stream. There are two different types of Lymes: Lyme arthritis and Lyme neuroborreliosis.
Nichols lives with Lyme neuroborreliosis, attacking both her brain and spinal cord. Symptoms can range from as small as flu symptoms to as aggressive as arthritis, meningitis, and facial nerve inflammation.
Acute disseminated Lyme, so they were thinking I had about it two to four weeks before they caught it. My legs started shaking at work and so by the time I got home it had looked like I had Parkinsons. I was shaking like this, said Nichols.
Nichols said she visited many doctors, being told it was just anxiety and I needed to believe in myself like they believed in me, calling the whole experience humiliating. Before landing on the one doctor that would change it all. Making her feel not-so-crazy for knowing something was actually wrong.
I would start going deaf in my left ear, or I would get numbness down the middle of my palette. Severe pain with swallowing is what did it, like it was a knife shooting down my throat, said Nichols.
Most Read
Don’t Miss: Can Stage 2 Lyme Disease Be Cured